Respiratory System Case Studies: Case study level 1 – Asthma-Community
Learning outcomes.
Level 1 case study: You will be able to:
- describe the risk factors
- describe the disease
- describe the pharmacology of the drug
- outline the formulations available, including drug molecule, excipients, etc. for the medicines
- summarise basic social pharmacy issues (e.g. opening containers, large labels).
An 18-year-old man, VB, presents with a history of recurrent episodes of wheeze after walking 200 meters. VB has recently started to go to a gym and his episodes of wheeze have worsened. He goes to see his GP. He can talk in sentences but his respiratory rate is increased. His peak flow is 420 L/min which is 80% of predicted result. A diagnosis of mild asthma is made. He is started on salbutamol metered dose inhaler (MDI) two puffs when required and beclomethasone (Qvar) 50 micrograms twice daily.
1. What is asthma? 2. What are the risk factors for developing asthma? What risk factors does the patient have? 3a. What is the pharmacology of beta2-agonists and inhaled corticosteroids? 3b. What are the side-effects of beta2-agonists? 4. What formulations of salbutamol and inhaled corticosteroids are available and what are the advantages and disadvantages? 5. Describe how to use an MDI. 6. What are the social implications of this man’s asthma?
1. What is asthma? Asthma is a chronic inflammatory disease affecting the airways. Symptoms are cough, wheeze, a feeling of tightness in the chest and shortness of breath. Asthma is characterized by:
- airway obstruction (bronchoconstriction), which is usually reversible either spontaneously or with therapeutic intervention,
- airway hyperresponsiveness to a range of stimuli,
- inflammation of the respiratory bronchioles due to eosinophils.
T lymphocytes and mast cells are involved in the production of mucus, edema, smooth muscle hypertrophy and this can lead to mucus production and epithelial damage. If asthma is chronic it can lead to inflammation associated with irreversible bronchoconstriction.
Asthma can be classified as either extrinsic or intrinsic.
- Extrinsic – there is a known external stimulus. This is usually in patients that are atopic and show reactions to allergens. This is common in childhood asthma
- Intrinsic – there is a causative agent identified. This usually starts in middle life, but there may be some evidence of allergy in younger life.
Patient VB may have had mild asthma as a child and this has now been exacerbated by the increased incidence of wheeze.
2. What are the risk factors for developing asthma? What risk factors does the patient have? The risk factors for developing asthma are as follows:
- Atopy in a patient, which refers to a group of disorders which include asthma, eczema and hay fever.
- Positive family history.
- Circulating antibodies and developing IgE class against common environmental factors.
- Genetic and environmental factors influencing levels of IgE.
- Occupational hazards (e.g. exposure to reactive chemicals such as isocyanates or IgE-related, such as allergens from animals, flour and grain).
- Non-steroidal anti-inflammatory drugs (NSAIDs) (e.g. aspirin), which can precipitate an attack in 5% of people with asthma.
- Beta-blockers. There is some evidence that beta-adrenergic blocking drugs such as propranolol can cause bronchoconstriction in some patients. Some selectivity with beta2-adrenergic drugs can minimise this effect but caution should be exercised.
- Atmospheric pollutants (e.g. cigarette smoke, car pollutants, dust).
- Cold air and exercise. People with asthma should ensure they are using effective medication since the latter can precipitate hyperresponsiveness of the airway.
This patient has limited risk factors, however, recurrent episodes of wheeze and exposure to cold and exercise may have precipitated the attack.
3a. What is the pharmacology of beta2-agonists and inhaled corticosteroids? Beta 2 -adrenergic agonists are available as short- and long-acting agents. These drugs have limited gastric absorption and are only effective when inhaled, following which they exert a local effect in the lungs. Beta2-adrenergic agents cause bronchodilation by increasing the levels of cyclic adenosine monophosphate (cAMP) following stimulation of the beta2-receptors in smooth muscle. They act throughout the respiratory tract. Short-acting beta2-adrenergic agents are the drugs of choice for the acute management of asthma. Longer-acting beta2 adrenergic agonists are used in patients with moderate to severe asthma in combination with corticosteroids.
Corticosteroids are anti-inflammatory drugs and are available in a range of formulations. These drugs are used in the management of short- and long-term control of asthma. A wide range of formulations and types of corticosteroids varying in potency are available. Inhaled corticosteroids are minimally absorbed and have a local effect. However, depending on the dose and potency of the inhaled corticosteroid, inhaled forms can produce systemic side-effects. Oral prednisolone is rapidly absorbed and is metabolized by the liver. Some corticosteroids may be administered intravenously.
Corticosteroids have a complex mechanism of action. They can affect the production of cytokines, leukotrienes, and prostaglandins. This affects the production of eosinophils and release of other markers of the inflammatory response. Corticosteroids can affect other areas of the body and hence have a range of side-effects.
3b. What are the side-effects of beta2-agonists?
Adverse effects include:
paradoxical bronchospasm tachycardia palpitations tremor headache blushing dry mouth hypertension arrhythmia low potassium levels.
4. What formulations of salbutamol and inhaled corticosteroids are available and what are the advantages and disadvantages?
Salbutamol is available as tablets, inhalers, nebulizer solution and intravenous injection. In the management of asthma at step 1 and 2 the inhaled formulation is the best option since it targets the drug and minimizes side-effects. Oral tablets of salbutamol are rarely used and there is limited evidence of their effectiveness.
Patients who have difficulty in coordination with inhalers can use a spacer device. These remove the need for coordination between actuation of a pressurised metered dose inhaler and inhalation. The spacer device reduces the velocity of the aerosol and subsequent impaction on the oropharynx. In addition, the device allows more time for evaporation of the propellant so that a larger proportion of the particles can be inhaled and deposited in the lungs. The size of the spacer is important, the larger spacers with a one-way valve (Nebuhaler, Volumatic) being most effective. Spacer devices are particularly useful for patients with poor inhalation technique, for children, for patients requiring higher doses, for nocturnal asthma, and for patients who have poor coordination.
Nebulised and intravenous salbutamol is required for more severe and acute status asthmaticus.
Corticosteroids
Corticosteroids are available in tablet, inhaled and intravenous dosage forms. Inhaled corticosteroids allow the control of asthma with minimal systemic absorption and thus reduce the risks associated with corticosteroids such as osteoporosis and adrenal suppression. These risks are greatly increased when taking systemic corticosteroids. Oral tablets and intravenous steroids are used in more severe and acute status asthmaticus.
5. Describe how to use an MDI. Patient education is vital for the management of asthma. Patients should be guided in their use of the asthma inhaler. It is important that you then observe the patient’s use. Instructions given to the patient are as follows:
- Sit in a comfortable, upright position.
- Remove the cap of the inhaler.
- Shake the inhaler.
- Breathe out and then put the mouthpiece into your mouth and take a deep inhalation, simultaneously pressing the inhaler.
- Hold your breath, then exhale slowly.
- Wipe the mouthpiece and replace the lid.
- The inhaler should be stored in a cool dry place.
- The essential counseling points should be taken from the inhaler package insert
- If you are to take two puffs, wait half a minute before repeating the steps above.
6. What are the social implications of this man’s asthma?
VP is entering adult life and will need to be aware of the importance of effective asthma management. He has to be mature enough to take responsibility for his asthma management and must not feel inhibited by having to carry inhalers with him. He needs to ensure prophylactic cover with beta2-agonists when undergoing strenuous exercise. He needs to be counseled on issues of sex education and the regular use of his inhalers. There is limited evidence of genetic malformation from his medicines, but the patient needs to be aware that when he considers a family, his child may be prone to asthma due to the genetic predisposition.
General references
- Joint Formulary Committee (2008) British National Formulary 55. London: British Medical Association and Royal Pharmaceutical Society of Great Britain, March.
- Soraya Dhillon, MBE, BPharm (Hons), PhD, FRPharmS
- Andrzej Kostrzewski, BSc, MSc, MMedEd, PhD, FHEA, MRPharmS
- Asthma-community
- Case study for pharmacist
- Pharmacy case study
- Respiratory system

You might be interested in
Liver disease case studies: Case study level 1 – Alcoholic cirrhosis; alcohol withdrawal
Cardiovascular case studies: case study level mb – myocardial infarction.
Pharmacy Case Studies for Pharmacists & Medical Sciences Students
Leave a reply cancel reply.
Your email address will not be published.
{{#message}}{{{message}}}{{/message}}{{^message}}Your submission failed. The server responded with {{status_text}} (code {{status_code}}). Please contact the developer of this form processor to improve this message. Learn More {{/message}}
{{#message}}{{{message}}}{{/message}}{{^message}}It appears your submission was successful. Even though the server responded OK, it is possible the submission was not processed. Please contact the developer of this form processor to improve this message. Learn More {{/message}}
Submitting…
This site uses Akismet to reduce spam. Learn how your comment data is processed .
Cardiovascular Case Studies : Case study level 2 – Hypertension
Cardiovascular case studies : case study level 1 – angina.
Thank you for visiting nature.com. You are using a browser version with limited support for CSS. To obtain the best experience, we recommend you use a more up to date browser (or turn off compatibility mode in Internet Explorer). In the meantime, to ensure continued support, we are displaying the site without styles and JavaScript.
- View all journals
- Explore content
- About the journal
- Publish with us
- Sign up for alerts
- Perspective
- Open access
- Published: 16 October 2014
A woman with asthma: a whole systems approach to supporting self-management
- Hilary Pinnock 1 ,
- Elisabeth Ehrlich 1 ,
- Gaylor Hoskins 2 &
- Ron Tomlins 3
npj Primary Care Respiratory Medicine volume 24 , Article number: 14063 ( 2014 ) Cite this article
16k Accesses
2 Citations
6 Altmetric
Metrics details
- Health care
A 35-year-old lady attends for review of her asthma following an acute exacerbation. There is an extensive evidence base for supported self-management for people living with asthma, and international and national guidelines emphasise the importance of providing a written asthma action plan. Effective implementation of this recommendation for the lady in this case study is considered from the perspective of a patient, healthcare professional, and the organisation. The patient emphasises the importance of developing a partnership based on honesty and trust, the need for adherence to monitoring and regular treatment, and involvement of family support. The professional considers the provision of asthma self-management in the context of a structured review, with a focus on a self-management discussion which elicits the patient’s goals and preferences. The organisation has a crucial role in promoting, enabling and providing resources to support professionals to provide self-management. The patient’s asthma control was assessed and management optimised in two structured reviews. Her goal was to avoid disruption to her work and her personalised action plan focused on achieving that goal.
Similar content being viewed by others
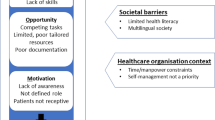
Barriers to implementing asthma self-management in Malaysian primary care: qualitative study exploring the perspectives of healthcare professionals

The self-management abilities test (SMAT): a tool to identify the self-management abilities of adults with bronchiectasis
Improving primary care management of asthma: do we know what really works?
A 35-year-old sales representative attends the practice for an asthma review. Her medical record notes that she has had asthma since childhood, and although for many months of the year her asthma is well controlled (when she often reduces or stops her inhaled steroids), she experiences one or two exacerbations a year requiring oral steroids. These are usually triggered by a viral upper respiratory infection, though last summer when the pollen count was particularly high she became tight chested and wheezy for a couple of weeks.
Her regular prescription is for fluticasone 100 mcg twice a day, and salbutamol as required. She has a young family and a busy lifestyle so does not often manage to find time to attend the asthma clinic. A few weeks previously, an asthma attack had interfered with some important work-related travel, and she has attended the clinic on this occasion to ask about how this can be managed better in the future. There is no record of her having been given an asthma action plan.
What do we know about asthma self-management? The academic perspective
Supported self-management reduces asthma morbidity.
The lady in this case study is struggling to maintain control of her asthma within the context of her busy professional and domestic life. The recent unfortunate experience which triggered this consultation offers a rare opportunity to engage with her and discuss how she can manage her asthma better. It behoves the clinician whom she is seeing (regardless of whether this is in a dedicated asthma clinic or an appointment in a routine general practice surgery) to grasp the opportunity and discuss self-management and provide her with a (written) personalised asthma action plan (PAAP).
The healthcare professional advising the lady is likely to be aware that international and national guidelines emphasise the importance of supporting self-management. 1 – 4 There is an extensive evidence base for asthma self-management: a recent synthesis identified 22 systematic reviews summarising data from 260 randomised controlled trials encompassing a broad range of demographic, clinical and healthcare contexts, which concluded that asthma self-management reduces emergency use of healthcare resources, including emergency department visits, hospital admissions and unscheduled consultations and improves markers of asthma control, including reduced symptoms and days off work, and improves quality of life. 1 , 2 , 5 – 12 Health economic analysis suggests that it is not only clinically effective, but also a cost-effective intervention. 13
Personalised asthma action plans
Key features of effective self-management approaches are:
Self-management education should be reinforced by provision of a (written) PAAP which reminds patients of their regular treatment, how to monitor and recognise that control is deteriorating and the action they should take. 14 – 16 As an adult, our patient can choose whether she wishes to monitor her control with symptoms or by recording peak flows (or a combination of both). 6 , 8 , 9 , 14 Symptom-based monitoring is generally better in children. 15 , 16
Plans should have between two and three action points including emergency doses of reliever medication; increasing low dose (or recommencing) inhaled steroids; or starting a course of oral steroids according to severity of the exacerbation. 14
Personalisation of the action plan is crucial. Focussing specifically on what actions she could take to prevent a repetition of the recent attack is likely to engage her interest. Not all patients will wish to start oral steroids without advice from a healthcare professional, though with her busy lifestyle and travel our patient is likely to be keen to have an emergency supply of prednisolone. Mobile technology has the potential to support self-management, 17 , 18 though a recent systematic review concluded that none of the currently available smart phone ‘apps’ were fit for purpose. 19
Identification and avoidance of her triggers is important. As pollen seems to be a trigger, management of allergic rhinitis needs to be discussed (and included in her action plan): she may benefit from regular use of a nasal steroid spray during the season. 20
Self-management as recommended by guidelines, 1 , 2 focuses narrowly on adherence to medication/monitoring and the early recognition/remediation of exacerbations, summarised in (written) PAAPs. Patients, however, may want to discuss how to reduce the impact of asthma on their life more generally, 21 including non-pharmacological approaches.
Supported self-management
The impact is greater if self-management education is delivered within a comprehensive programme of accessible, proactive asthma care, 22 and needs to be supported by ongoing regular review. 6 With her busy lifestyle, our patient may be reluctant to attend follow-up appointments, and once her asthma is controlled it may be possible to make convenient arrangements for professional review perhaps by telephone, 23 , 24 or e-mail. Flexible access to professional advice (e.g., utilising diverse modes of consultation) is an important component of supporting self-management. 25
The challenge of implementation
Implementation of self-management, however, remains poor in routine clinical practice. A recent Asthma UK web-survey estimated that only 24% of people with asthma in the UK currently have a PAAP, 26 with similar figures from Sweden 27 and Australia. 28 The general practitioner may feel that they do not have time to discuss self-management in a routine surgery appointment, or may not have a supply of paper-based PAAPs readily available. 29 However, as our patient rarely finds time to attend the practice, inviting her to make an appointment for a future clinic is likely to be unsuccessful and the opportunity to provide the help she needs will be missed.
The solution will need a whole systems approach
A systematic meta-review of implementing supported self-management in long-term conditions (including asthma) concluded that effective implementation was multifaceted and multidisciplinary; engaging patients, training and motivating professionals within the context of an organisation which actively supported self-management. 5 This whole systems approach considers that although patient education, professional training and organisational support are all essential components of successful support, they are rarely effective in isolation. 30 A systematic review of interventions that promote provision/use of PAAPs highlighted the importance of organisational systems (e.g., sending blank PAAPs with recall reminders). 31 A patient offers her perspective ( Box 1 ), a healthcare professional considers the clinical challenge, and the challenges are discussed from an organisational perspective.
Box 1: What self-management help should this lady expect from her general practitioner or asthma nurse? The patient’s perspective
The first priority is that the patient is reassured that her condition can be managed successfully both in the short and the long term. A good working relationship with the health professional is essential to achieve this outcome. Developing trust between patient and healthcare professional is more likely to lead to the patient following the PAAP on a long-term basis.
A review of all medication and possible alternative treatments should be discussed. The patient needs to understand why any changes are being made and when she can expect to see improvements in her condition. Be honest, as sometimes it will be necessary to adjust dosages before benefits are experienced. Be positive. ‘There are a number of things we can do to try to reduce the impact of asthma on your daily life’. ‘Preventer treatment can protect against the effect of pollen in the hay fever season’. If possible, the same healthcare professional should see the patient at all follow-up appointments as this builds trust and a feeling of working together to achieve the aim of better self-management.
Is the healthcare professional sure that the patient knows how to take her medication and that it is taken at the same time each day? The patient needs to understand the benefit of such a routine. Medication taken regularly at the same time each day is part of any self-management regime. If the patient is unused to taking medication at the same time each day then keeping a record on paper or with an electronic device could help. Possibly the patient could be encouraged to set up a system of reminders by text or smartphone.
Some people find having a peak flow meter useful. Knowing one's usual reading means that any fall can act as an early warning to put the PAAP into action. Patients need to be proactive here and take responsibility.
Ongoing support is essential for this patient to ensure that she takes her medication appropriately. Someone needs to be available to answer questions and provide encouragement. This could be a doctor or a nurse or a pharmacist. Again, this is an example of the partnership needed to achieve good asthma control.
It would also be useful at a future appointment to discuss the patient’s lifestyle and work with her to reduce her stress. Feeling better would allow her to take simple steps such as taking exercise. It would also be helpful if all members of her family understood how to help her. Even young children can do this.
From personal experience some people know how beneficial it is to feel they are in a partnership with their local practice and pharmacy. Being proactive produces dividends in asthma control.
What are the clinical challenges for the healthcare professional in providing self-management support?
Due to the variable nature of asthma, a long-standing history may mean that the frequency and severity of symptoms, as well as what triggers them, may have changed over time. 32 Exacerbations requiring oral steroids, interrupting periods of ‘stability’, indicate the need for re-assessment of the patient’s clinical as well as educational needs. The patient’s perception of stability may be at odds with the clinical definition 1 , 33 —a check on the number of short-acting bronchodilator inhalers the patient has used over a specific period of time is a good indication of control. 34 Assessment of asthma control should be carried out using objective tools such as the Asthma Control Test or the Royal College of Physicians three questions. 35 , 36 However, it is important to remember that these assessment tools are not an end in themselves but should be a springboard for further discussion on the nature and pattern of symptoms. Balancing work with family can often make it difficult to find the time to attend a review of asthma particularly when the patient feels well. The practice should consider utilising other means of communication to maintain contact with patients, encouraging them to come in when a problem is highlighted. 37 , 38 Asthma guidelines advocate a structured approach to ensure the patient is reviewed regularly and recommend a detailed assessment to enable development of an appropriate patient-centred (self)management strategy. 1 – 4
Although self-management plans have been shown to be successful for reducing the impact of asthma, 21 , 39 the complexity of managing such a fluctuating disease on a day-to-day basis is challenging. During an asthma review, there is an opportunity to work with the patient to try to identify what triggers their symptoms and any actions that may help improve or maintain control. 38 An integral part of personalised self-management education is the written PAAP, which gives the patient the knowledge to respond to the changes in symptoms and ensures they maintain control of their asthma within predetermined parameters. 9 , 40 The PAAP should include details on how to monitor asthma, recognise symptoms, how to alter medication and what to do if the symptoms do not improve. The plan should include details on the treatment to be taken when asthma is well controlled, and how to adjust it when the symptoms are mild, moderate or severe. These action plans need to be developed between the doctor, nurse or asthma educator and the patient during the review and should be frequently reviewed and updated in partnership (see Box 1). Patient preference as well as clinical features such as whether she under- or over-perceives her symptoms should be taken into account when deciding whether the action plan is peak flow or symptom-driven. Our patient has a lot to gain from having an action plan. She has poorly controlled asthma and her lifestyle means that she will probably see different doctors (depending who is available) when she needs help. Being empowered to self-manage could make a big difference to her asthma control and the impact it has on her life.
The practice should have protocols in place, underpinned by specific training to support asthma self-management. As well as ensuring that healthcare professionals have appropriate skills, this should include training for reception staff so that they know what action to take if a patient telephones to say they are having an asthma attack.
However, focusing solely on symptom management strategies (actions) to follow in the presence of deteriorating symptoms fails to incorporate the patients’ wider views of asthma, its management within the context of her/his life, and their personal asthma management strategies. 41 This may result in a failure to use plans to maximise their health potential. 21 , 42 A self-management strategy leading to improved outcomes requires a high level of patient self-efficacy, 43 a meaningful partnership between the patient and the supporting health professional, 42 , 44 and a focused self-management discussion. 14
Central to both the effectiveness and personalisation of action plans, 43 , 45 in particular the likelihood that the plan will lead to changes in patients’ day-to-day self-management behaviours, 45 is the identification of goals. Goals are more likely to be achieved when they are specific, important to patients, collaboratively set and there is a belief that these can be achieved. Success depends on motivation 44 , 46 to engage in a specific behaviour to achieve a valued outcome (goal) and the ability to translate the behavioural intention into action. 47 Action and coping planning increases the likelihood that patient behaviour will actually change. 44 , 46 , 47 Our patient has a goal: she wants to avoid having her work disrupted by her asthma. Her personalised action plan needs to explicitly focus on achieving that goal.
As providers of self-management support, health professionals must work with patients to identify goals (valued outcomes) that are important to patients, that may be achievable and with which they can engage. The identification of specific, personalised goals and associated feasible behaviours is a prerequisite for the creation of asthma self-management plans. Divergent perceptions of asthma and how to manage it, and a mismatch between what patients want/need from these plans and what is provided by professionals are barriers to success. 41 , 42
What are the challenges for the healthcare organisation in providing self-management support?
A number of studies have demonstrated the challenges for primary care physicians in providing ongoing support for people with asthma. 31 , 48 , 49 In some countries, nurses and other allied health professionals have been trained as asthma educators and monitor people with stable asthma. These resources are not always available. In addition, some primary care services are delivered in constrained systems where only a few minutes are available to the practitioner in a consultation, or where only a limited range of asthma medicines are available or affordable. 50
There is recognition that the delivery of quality care depends on the competence of the doctor (and supporting health professionals), the relationship between the care providers and care recipients, and the quality of the environment in which care is delivered. 51 This includes societal expectations, health literacy and financial drivers.
In 2001, the Australian Government adopted a programme developed by the General Practitioner Asthma Group of the National Asthma Council Australia that provided a structured approach to the implementation of asthma management guidelines in a primary care setting. 52 Patients with moderate-to-severe asthma were eligible to participate. The 3+ visit plan required confirmation of asthma diagnosis, spirometry if appropriate, assessment of trigger factors, consideration of medication and patient self-management education including provision of a written PAAP. These elements, including regular medical review, were delivered over three visits. Evaluation demonstrated that the programme was beneficial but that it was difficult to complete the third visit in the programme. 53 – 55 Accordingly, the programme, renamed the Asthma Cycle of Care, was modified to incorporate two visits. 56 Financial incentives are provided to practices for each patient who receives this service each year.
Concurrently, other programmes were implemented which support practice-based care. Since 2002, the National Asthma Council has provided best-practice asthma and respiratory management education to health professionals, 57 and this programme will be continuing to 2017. The general practitioner and allied health professional trainers travel the country to provide asthma and COPD updates to groups of doctors, nurses and community pharmacists. A number of online modules are also provided. The PACE (Physician Asthma Care Education) programme developed by Noreen Clark has also been adapted to the Australian healthcare system. 58 In addition, a pharmacy-based intervention has been trialled and implemented. 59
To support these programmes, the National Asthma Council ( www.nationalasthma.org.au ) has developed resources for use in practices. A strong emphasis has been on the availability of a range of PAAPs (including plans for using adjustable maintenance dosing with ICS/LABA combination inhalers), plans for indigenous Australians, paediatric plans and plans translated into nine languages. PAAPs embedded in practice computer systems are readily available in consultations, and there are easily accessible online paediatric PAAPs ( http://digitalmedia.sahealth.sa.gov.au/public/asthma/ ). A software package, developed in the UK, can be downloaded and used to generate a pictorial PAAP within the consultation. 60
One of the strongest drivers towards the provision of written asthma action plans in Australia has been the Asthma Friendly Schools programme. 61 , 62 Established with Australian Government funding and the co-operation of Education Departments of each state, the Asthma Friendly Schools programme engages schools to address and satisfy a set of criteria that establishes an asthma-friendly environment. As part of accreditation, the school requires that each child with asthma should have a written PAAP prepared by their doctor to assist (trained) staff in managing a child with asthma at school.
The case study continues...
The initial presentation some weeks ago was during an exacerbation of asthma, which may not be the best time to educate a patient. It is, however, a splendid time to build on their motivation to feel better. She agreed to return after her asthma had settled to look more closely at her asthma control, and an appointment was made for a routine review.
At this follow-up consultation, the patient’s diagnosis was reviewed and confirmed and her trigger factors discussed. For this lady, respiratory tract infections are the usual trigger but allergic factors during times of high pollen count may also be relevant. Assessment of her nasal airway suggested that she would benefit from better control of allergic rhinitis. Other factors were discussed, as many patients are unaware that changes in air temperature, exercise and pets can also trigger asthma exacerbations. In addition, use of the Asthma Control Test was useful as an objective assessment of control as well as helping her realise what her life could be like! Many people with long-term asthma live their life within the constraints of their illness, accepting that is all that they can do.
After assessing the level of asthma control, a discussion about management options—trigger avoidance, exercise and medicines—led to the development of a written PAAP. Asthma can affect the whole family, and ways were explored that could help her family understand why it is important that she finds time in the busy domestic schedules to take her regular medication. Family and friends can also help by understanding what triggers her asthma so that they can avoid exposing her to perfumes, pollens or pets that risk triggering her symptoms. Information from the national patient organisation was provided to reinforce the messages.
The patient agreed to return in a couple of weeks, and a recall reminder was set up. At the second consultation, the level of control since the last visit will be explored including repeat spirometry, if appropriate. Further education about the pathophysiology of asthma and how to recognise early warning signs of loss of control can be given. Device use will be reassessed and the PAAP reviewed. Our patient’s goal is to avoid disruption to her work and her PAAP will focus on achieving that goal. Finally, agreement will be reached with the patient about future routine reviews, which, now that she has a written PAAP, could be scheduled by telephone if all is well, or face-to-face if a change in her clinical condition necessitates a more comprehensive review.
Global Initiative for Asthma. Global Strategy for Asthma Management and Prevention, 2012. Available from: http://www.ginasthma.org (accessed July 2013).
British Thoracic Society/Scottish Intercollegiate Guideline Network British Guideline on the Management of Asthma. Thorax 2008; 63 (Suppl 4 iv1–121, updated version available from: http://www.sign.ac.uk (accessed January 2014).
Article Google Scholar
National Asthma Council Australia. Australian Asthma Handbook. Available from: http://www.nationalasthma.org.au/handbook (accessed May 2014).
National Asthma Education and Prevention Program (NAEPP) Coordinating Committee. Expert Panel Report 3 (EPR3): Guidelines for the Diagnosis and Management of Asthma. Available from: https://www.nhlbi.nih.gov/guidelines/asthma/asthgdln.htm (accessed May 2014).
Taylor SJC, Pinnock H, Epiphaniou E, Pearce G, Parke H . A rapid synthesis of the evidence on interventions supporting self-management for people with long-term conditions. (PRISMS Practical Systematic Review of Self-Management Support for long-term conditions). Health Serv Deliv Res (in press).
Gibson PG, Powell H, Wilson A, Abramson MJ, Haywood P, Bauman A et al. Self-management education and regular practitioner review for adults with asthma. Cochrane Database Syst Rev 2002: (Issue 3) Art No. CD001117.
Tapp S, Lasserson TJ, Rowe BH . Education interventions for adults who attend the emergency room for acute asthma. Cochrane Database Syst Rev 2007: (Issue 3) Art No. CD003000.
Powell H, Gibson PG . Options for self-management education for adults with asthma. Cochrane Database Syst Rev 2002: (Issue 3) Art No: CD004107.
Toelle B, Ram FSF . Written individualised management plans for asthma in children and adults. Cochrane Database Syst Rev 2004: (Issue 1) Art No. CD002171.
Lefevre F, Piper M, Weiss K, Mark D, Clark N, Aronson N . Do written action plans improve patient outcomes in asthma? An evidence-based analysis. J Fam Pract 2002; 51 : 842–848.
PubMed Google Scholar
Boyd M, Lasserson TJ, McKean MC, Gibson PG, Ducharme FM, Haby M . Interventions for educating children who are at risk of asthma-related emergency department attendance. Cochrane Database Syst Rev 2009: (Issue 2) Art No.CD001290.
Bravata DM, Gienger AL, Holty JE, Sundaram V, Khazeni N, Wise PH et al. Quality improvement strategies for children with asthma: a systematic review. Arch Pediatr Adolesc Med 2009; 163 : 572–581.
Bower P, Murray E, Kennedy A, Newman S, Richardson G, Rogers A . Self-management support interventions to reduce health care utilisation without compromising outcomes: a rapid synthesis of the evidence. Available from: http://www.nets.nihr.ac.uk/projects/hsdr/11101406 (accessed April 2014).
Gibson PG, Powell H . Written action plans for asthma: an evidence-based review of the key components. Thorax 2004; 59 : 94–99.
Article CAS Google Scholar
Bhogal SK, Zemek RL, Ducharme F . Written action plans for asthma in children. Cochrane Database Syst Rev 2006: (Issue 3) Art No. CD005306.
Zemek RL, Bhogal SK, Ducharme FM . Systematic review of randomized controlled trials examining written action plans in children: what is the plan?. Arch Pediatr Adolesc Med 2008; 162 : 157–163.
Pinnock H, Slack R, Pagliari C, Price D, Sheikh A . Understanding the potential role of mobile phone based monitoring on asthma self-management: qualitative study. Clin Exp Allergy 2007; 37 : 794–802.
de Jongh T, Gurol-Urganci I, Vodopivec-Jamsek V, Car J, Atun R . Mobile phone messaging for facilitating self-management of long-term illnesses. Cochrane Database Syst Rev 2012: (Issue 12) Art No. CD007459.
Huckvale K, Car M, Morrison C, Car J . Apps for asthma self-management: a systematic assessment of content and tools. BMC Med 2012; 10 : 144.
Allergic Rhinitis and its Impact on Asthma. Management of Allergic Rhinitis and its Impact on Asthma: Pocket Guide. ARIA 2008. Available from: http://www.whiar.org (accessed May 2014).
Ring N, Jepson R, Hoskins G, Wilson C, Pinnock H, Sheikh A et al. Understanding what helps or hinders asthma action plan use: a systematic review and synthesis of the qualitative literature. Patient Educ Couns 2011; 85 : e131–e143.
Moullec G, Gour-Provencal G, Bacon SL, Campbell TS, Lavoie KL . Efficacy of interventions to improve adherence to inhaled corticosteroids in adult asthmatics: Impact of using components of the chronic care model. Respir Med 2012; 106 : 1211–1225.
Pinnock H, Bawden R, Proctor S, Wolfe S, Scullion J, Price D et al. Accessibility, acceptability and effectiveness of telephone reviews for asthma in primary care: randomised controlled trial. BMJ 2003; 326 : 477–479.
Pinnock H, Adlem L, Gaskin S, Harris J, Snellgrove C, Sheikh A . Accessibility, clinical effectiveness and practice costs of providing a telephone option for routine asthma reviews: phase IV controlled implementation study. Br J Gen Pract 2007; 57 : 714–722.
PubMed PubMed Central Google Scholar
Kielmann T, Huby G, Powell A, Sheikh A, Price D, Williams S et al. From support to boundary: a qualitative study of the border between self care and professional care. Patient Educ Couns 2010; 79 : 55–61.
Asthma UK . Compare your care report. Asthma UK, 2013. Available from: http://www.asthma.org.uk (accessed January 2014).
Stallberg B, Lisspers K, Hasselgren M, Janson C, Johansson G, Svardsudd K . Asthma control in primary care in Sweden: a comparison between 2001 and 2005. Prim Care Respir J 2009; 18 : 279–286.
Reddel H, Peters M, Everett P, Flood P, Sawyer S . Ownership of written asthma action plans in a large Australian survey. Eur Respir J 2013; 42 . Abstract 2011.
Wiener-Ogilvie S, Pinnock H, Huby G, Sheikh A, Partridge MR, Gillies J . Do practices comply with key recommendations of the British Asthma Guideline? If not, why not? Prim Care Respir J 2007; 16 : 369–377.
Kennedy A, Rogers A, Bower P . Support for self care for patients with chronic disease. BMJ 2007; 335 : 968–970.
Ring N, Malcolm C, Wyke S, Macgillivray S, Dixon D, Hoskins G et al. Promoting the Use of Personal Asthma Action Plans: A Systematic Review. Prim Care Respir J 2007; 16 : 271–283.
Taylor DR, Bateman ED, Boulet LP, Boushey HA, Busse WW, Casale TB et al. A new perspective on concepts of asthma severity and control. Eur Respir J 2008; 32 : 545–554.
Horne R . Compliance, adherence, and concordance: implications for asthma treatment. Chest 2006; 130 (suppl): 65S–72S.
Reddel HK, Taylor DR, Bateman ED, Boulet L-P, Boushey HA, Busse WW et al. An official American Thoracic Society/European Respiratory Society statement: asthma control and exacerbations standardizing endpoints for clinical asthma trials and clinical practice. Am J Respir Crit Care Med 2009; 180 : 59–99.
Thomas M, Kay S, Pike J, Rosenzweig JR, Hillyer EV, Price D . The Asthma Control Test (ACT) as a predictor of GINA guideline-defined asthma control: analysis of a multinational cross-sectional survey. Prim Care Respir J 2009; 18 : 41–49.
Hoskins G, Williams B, Jackson C, Norman P, Donnan P . Assessing asthma control in UK primary care: use of routinely collected prospective observational consultation data to determine appropriateness of a variety of control assessment models. BMC Fam Pract 2011; 12 : 105.
Pinnock H, Fletcher M, Holmes S, Keeley D, Leyshon J, Price D et al. Setting the standard for routine asthma consultations: a discussion of the aims, process and outcomes of reviewing people with asthma in primary care. Prim Care Respir J 2010; 19 : 75–83.
McKinstry B, Hammersley V, Burton C, Pinnock H, Elton RA, Dowell J et al. The quality, safety and content of telephone and face-to-face consultations: a comparative study. Qual Saf Health Care 2010; 19 : 298–303.
Gordon C, Galloway T . Review of Findings on Chronic Disease Self-Management Program (CDSMP) Outcomes: Physical, Emotional & Health-Related Quality of Life, Healthcare Utilization and Costs . Centers for Disease Control and Prevention and National Council on Aging: Atlanta, GA, USA, 2008.
Beasley R, Crane J . Reducing asthma mortality with the self-management plan system of care. Am J Respir Crit Care Med 2001; 163 : 3–4.
Ring N, Jepson R, Pinnock H, Wilson C, Hoskins G, Sheikh A et al. Encouraging the promotion and use of asthma action plans: a cross study synthesis of qualitative and quantitative evidence. Trials 2012; 13 : 21.
Jones A, Pill R, Adams S . Qualitative study of views of health professionals and patients on guided self-management plans for asthma. BMJ 2000; 321 : 1507–1510.
Bandura A . Self-efficacy: toward a unifying theory of behavioural change. Psychol Rev 1977; 84 : 191–215.
Gollwitzer PM, Sheeran P . Implementation intentions and goal achievement: a meta-analysis of effects and processes. Adv Exp Soc Psychol 2006; 38 : 69–119.
Google Scholar
Hardeman W, Johnston M, Johnston DW, Bonetti D, Wareham NJ, Kinmonth AL . Application of the theory of planned behaviour change interventions: a systematic review. Psychol Health 2002; 17 : 123–158.
Schwarzer R . Modeling health behavior change: how to predict and modify the adoption and maintenance of health behaviors. Appl Psychol 2008; 57 : 1–29.
Sniehotta F . Towards a theory of intentional behaviour change: plans, planning, and self-regulation. Br J Health Psychol 2009; 14 : 261–273.
Okelo SO, Butz AM, Sharma R, Diette GB, Pitts SI, King TM et al. Interventions to modify health care provider adherence to asthma guidelines: a systematic review. Pediatrics 2013; 132 : 517–534.
Grol R, Grimshaw RJ . From best evidence to best practice: effective implementation of change in patients care. Lancet 2003; 362 : 1225–1230.
Jusef L, Hsieh C-T, Abad L, Chaiyote W, Chin WS, Choi Y-J et al. Primary care challenges in treating paediatric asthma in the Asia-Pacific region. Prim Care Respir J 2013; 22 : 360–362.
Donabedian A . Evaluating the quality of medical care. Milbank Q 2005; 83 : 691–729.
Fardy HJ . Moving towards organized care of chronic disease. The 3+ visit plan. Aust Fam Physician 2001; 30 : 121–125.
CAS PubMed Google Scholar
Glasgow NJ, Ponsonby AL, Yates R, Beilby J, Dugdale P . Proactive asthma care in childhood: general practice based randomised controlled trial. BMJ 2003; 327 : 659.
Douglass JA, Goemann DP, Abramson MJ . Asthma 3+ visit plan: a qualitative evaluation. Intern Med J 2005; 35 : 457–462.
Beilby J, Holton C . Chronic disease management in Australia; evidence and policy mismatch, with asthma as an example. Chronic Illn 2005; 1 : 73–80.
The Department of Health. Asthma Cycle of Care. Accessed on 14 May 2014 at http://www.health.gov.au/internet/main/publishing.nsf/Content/asthma-cycle .
National Asthma Council Australia. Asthma and Respiratory Education Program. Accessed on 14 May 2014 at http://www.nationalasthma.org.au/health-professionals/education-training/asthma-respiratory-education-program .
Patel MR, Shah S, Cabana MD, Sawyer SM, Toelle B, Mellis C et al. Translation of an evidence-based asthma intervention: Physician Asthma Care Education (PACE) in the United States and Australia. Prim Care Respir J 2013; 22 : 29–34.
Armour C, Bosnic-Anticevich S, Brilliant M, Burton D, Emmerton L, Krass I et al. Pharmacy Asthma Care Program (PACP) improves outcomes for patients in the community. Thorax 2007; 62 : 496–502.
Roberts NJ, Mohamed Z, Wong PS, Johnson M, Loh LC, Partridge MR . The development and comprehensibility of a pictorial asthma action plan. Patient Educ Couns 2009; 74 : 12–18.
Henry RL, Gibson PG, Vimpani GV, Francis JL, Hazell J . Randomised controlled trial of a teacher-led asthma education program. Pediatr Pulmonol 2004; 38 : 434–442.
National Asthma Council Australia. Asthma Friendly Schools program. Accessed on 14 May 2014 at http://www.asthmaaustralia.org.au/Asthma-Friendly-Schools.aspx .
Download references
Author information
Authors and affiliations.
Asthma UK Centre for Applied Research, Centre for Population Health Sciences, The University of Edinburgh, Edinburgh, UK,
Hilary Pinnock & Elisabeth Ehrlich
NMAHP-RU, University of Stirling, Stirling, UK,
Gaylor Hoskins
Discipline of General Practice, University of Sydney, Sydney, NSW, Australia
Ron Tomlins
You can also search for this author in PubMed Google Scholar
Corresponding author
Correspondence to Hilary Pinnock .
Ethics declarations
Competing interests.
The authors declare no conflict of interest.
Rights and permissions
This work is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike 4.0 International License. The images or other third party material in this article are included in the article's Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-sa/4.0/
Reprints and permissions
About this article
Cite this article.
Pinnock, H., Ehrlich, E., Hoskins, G. et al. A woman with asthma: a whole systems approach to supporting self-management. npj Prim Care Resp Med 24 , 14063 (2014). https://doi.org/10.1038/npjpcrm.2014.63
Download citation
Received : 23 June 2014
Revised : 15 July 2014
Accepted : 15 July 2014
Published : 16 October 2014
DOI : https://doi.org/10.1038/npjpcrm.2014.63
Share this article
Anyone you share the following link with will be able to read this content:
Sorry, a shareable link is not currently available for this article.
Provided by the Springer Nature SharedIt content-sharing initiative
Quick links
- Explore articles by subject
- Guide to authors
- Editorial policies
Sign up for the Nature Briefing newsletter — what matters in science, free to your inbox daily.
We have a new app!
Take the Access library with you wherever you go—easy access to books, videos, images, podcasts, personalized features, and more.
Download the Access App here: iOS and Android . Learn more here!
- Remote Access
- Save figures into PowerPoint
- Download tables as PDFs

- Download Chapter PDF
Disclaimer: These citations have been automatically generated based on the information we have and it may not be 100% accurate. Please consult the latest official manual style if you have any questions regarding the format accuracy.
Download citation file:
- Search Book
Jump to a Section
Pathophysiology, epidemiology, risk factors, clinical presentation.
- DESIRED OUTCOMES
- TREATMENT: GENERAL APPROACH
- TREATMENT: NONPHARMACOLOGIC THERAPY
- TREATMENT: PHARMACOLOGIC THERAPY
- ADDITIONAL RESOURCES
- Full Chapter
- Supplementary Content
Source : Sorkness CA, Blake KV. Asthma. In: DiPiro JT, Talbert RL, Yee GC, Matzke GR, Wells BG, Posey LM, eds. Pharmacotherapy: A Pathophysiologic Approach . 10th ed. New York, NY: McGraw-Hill; 2017. http://accesspharmacy.mhmedical.com/content.aspx?bookid=1861§ionid=146058008 . Accessed April 13, 2017.
Chronic inflammatory disorder of airways that causes recurrent episodes of wheezing, breathlessness, chest tightness, and coughing.
Genetic factors.
Environmental exposures (see Risk Factors)
Major characteristics:
Airflow obstruction (related to bronchospasm, edema, and hypersecretion)
Bronchial hyperresponsiveness (BHR)
Airway inflammation.
Inhaled allergen causes activation of B lymphocytes, mast cells, and macrophages, which release proinflammatory mediators such as histamine and eicosanoids that induce contraction of airway smooth muscle, mucus secretion, vasodilation, exudation, and edema with reduced mucus clearance.
Activation of eosinophils, T lymphocytes, basophils, neutrophils, and macrophages cause further release of inflammatory mediators such as leukotrienes, interleukins, histamine, platelet-activating factor (PAF), and chemotactic factors.
Affects 25.7 million persons in the United States.
Most common chronic childhood disease, affecting approximately 7 million children.
Accounts for 1.6% of ambulatory care visits (10.6 million physician office visits and 1.2 million hospital outpatient visits).
Resulted in 479,000 hospitalizations and 2.1 million emergency department (ED) visits in 2009.
Accounts for >14.4 million missed school days per year.
Genetic predisposition.
Socioeconomic status.
Family size.
Exposure to secondhand tobacco smoke in infancy and in utero.
Allergen exposure.
Ambient air pollution.
Urbanization.
Respiratory syncytial virus (RSV) and rhinovirus infection.
Decreased exposure to common childhood infectious agents.
SIGNS AND SYMPTOMS
Chronic asthma.
Symptoms: Episodic dyspnea with wheezing, chest tightness, and coughing that may occur spontaneously, with exercise, or after exposure to known allergens.
Signs: Expiratory wheezing; dry, hacking cough; atopy (eg, allergic rhinitis, eczema)
Can vary in frequency from intermittent to chronic daily symptoms.
Severity determined by lung function, symptoms, nighttime awakenings, and interference with normal activity.
Acute severe asthma.
Symptoms: Anxiousness with acute distress and complaints of severe dyspnea, shortness of breath, and chest tightness unresponsive to usual measures.
Signs: Expiratory and inspiratory wheezing; dry, hacking cough; tachypnea; tachycardia; pallor or cyanosis; hyperinflated chest with intercostal and supraclavicular retractions.
MEANS OF CONFIRMATION AND DIAGNOSIS
History of recurrent episodes of coughing, wheezing, chest tightness, or shortness of breath and confirmatory spirometry.
May be family history of allergy or asthma, or patient symptoms of allergic rhinitis.
History of exercise or cold air precipitating symptoms during specific allergen seasons.
History of previous asthma exacerbations (eg, hospitalizations, intubations) and complicating illnesses (eg, cardiac disease, diabetes).
Get Free Access Through Your Institution
Pop-up div successfully displayed.
This div only appears when the trigger link is hovered over. Otherwise it is hidden from view.
Please Wait
- Join our Mailing List
Working locally in primary care and collaborating globally to improve respiratory health
Clinical case study - asthma, clinical case study - asthma, resource information.
- Disease management
Clinical Case Studies with Answers
This section includes clinical case studies* with answers for the theoretical practice of Doctor of Pharmacy ( Pharm.D ) students. Also, it is equally useful for Pharm.D PB students. These Pharm.D case studies are regularly discussed in the telegram group . You can join there and participate in active case discussions. Case studies help you revise your Pharmacotherapy syllabus and increase knowledge of disease in an innovative way apart from practical knowledge.
You can access these clinical case studies with answers with no charge, which are contributed by various seniors from Doctor of Pharmacy stream only. In some cases practical references are also taken from certified & specialized practitioner from the respective field along with standard treatment guidelines.
*Clinical Case Studies included here are collected from various sources and are only for study purpose while maintaining the privacy of patients.
1. Pharm.D Case Studies for second year and Pharm.D PB first year
A) cardiovascular system case studies with answers: .
- Hypertension : Case Study 1 and Case Study 2
- Congestive Heart Failure : Case Study 3 and Case Study 4
- Angina Pectoris : Case study 5 and Case Study 6
- Myocardial Infarction : Case Study 7 and Case Study 8
- Hyperlipidaemias : Case Study 9 and Case Study 10
- Electrophysiology of heart and Arrhythmia : Case Study 11 and Case Study 12
b) Respiratory System Case Studies with answers:
- Asthma: Case Study 13 and Case Study 14
- COPD : Case Study 15 and Case Study 16
c) Endocrine System Case Studies with answers:
- Diabetes: Case Study 17 and Case Study – 18
- Hypothyroidism : Case Study -19 and Case Study -20
- Other Thyroid Disorders : Case Study -21 and Case Study -22
- Oral Contraceptive Use : Case Study- 23 and Case Study- 24
- Hormone Replacement Therapy: Case Study- 25 and Case Study- 26
- Osteoporosis: Case Study – 27 and Case Study – 28
d) Opthalmology Case Studies with answers:
- Glaucoma: Case Study – 29 and Case Study – 30
- Conjunctivitis: Case Study – 3 1 and Case Study – 32
e) General prescribing guidelines, Small Case Study with answers:
- Pediatrics : Case Study – 33
Case Studies for Doctor of Pharmacy students :
Case study-1 (hypertension with cardiovascular comorbidities).
JR is a 58-year-old man with a medical history of elevated low-density lipoprotein levels and well-controlled chronic stable angina (experiencing <1 angina attack per month) secondary to coronary artery disease (CAD). He presents to his primary care physician for a follow-up appointment after his blood pressure (BP) was found to be 165/94 mm Hg at his annual physical exam. At today’s visit, JR’s BP is found to be 166/93 mm Hg, resulting in a diagnosis of hypertension. JR is currently on Atorvastatin 40 mg daily and Metoprolol Tartrate 100 mg twice daily. And he reports no adverse effects from either medication. He has no other medical history of note, and his resting heart rate is 65 to 70 beats per minute.
Questions :
- What is the target goal for BP in this patient?
- What are the main classes of anti-hypertensives that can be used in this case ?
- Prepare a therapeutic regimen for this patient.
For Case Study-1 Answer, Click here.
Case Study-2 (Hypertension with Type-2 Diabetes Mellitus)
Mr. MK a 55-year-old man, having history of hypertension and type-2 diabetes mellitus for past 10 years with non-compliance to medication and poor diet control referred to the clinic for further management of poorly controlled diabetes and hypertension.
Socio-demographics:
Age :55 Sex : Male BMI : 35kg/m² Weight : 98 kg Occupation : Salesman
Family History :
Mother : Diabetic ( on dialysis). Father : Stroke ( residual left hemiparesis).
Subjective and Objective Evidence :
- Minimal bilateral leg edema.
- Bilateral proliferative retinopathy. Vitals – Blood Pressure : 160/90 mm/Hg Pulse rate. : 88 /min
Investigation results :
A1c : 9.2% FBS. : 11.8 mmol/L Serum creatinine : 1.2 mg/dl eGFR : 88 ml/min/1.73m² 24 hr urinary protein : 200mg/24 hr. ECG : Left Ventricular Hypertrophy.
Past medication :
Metformin 1000 mg BD Gliclazide 160 mg BD Amlodipine 10 mg OD
- What might be reasons for his poorly controlled diabetes and hypertension?
- What would be the A1c and BP target?
- How would you manage both HTN and T2DM ?
- Is there any Drug interaction, that should be taken in consider?
- What are the major patient counselling points?
For Case Study-2 Answer, Click here
For more Pharm.D Case studies. Click here.
Case Study-3 ( Congestive Cardiac Failure)
Mrs. JE a 70-year-old woman, was admitted to the medical unit with complaints of increasing dyspnea on exertion.
Subjective data:
- Had a severe MI at 58 years of age
- Has experienced increasing dyspnea on exertion during the last 2 years
- Recently had a respiratory tract infection, frequently cough and edema in legs 2 weeks ago
- Shortness of breathe while having average walking
- Has to sleep with head elevated on 3 pillows
- Does not always remember to take medication
Objective Evidence :
- In respiratory distress, use of accessory muscles.
- Heart murmur.
- Moist cracle in both lungs.
- Cyanotic lips and extremeties.
- Skin cool and diaphoretic. Vitals – Blood Pressure : 130/80 mm/Hg Pulse rate. : 70 /min Respiratory rate : 36 / min
Chest X-Ray : Cardiomegaly with right and left ventricular hypertrophy, fluid in lower lung fields.
Current Medication/ Collaborative Care
Digoxin 0.25 mg PO qd Furosemide 40 mg IV bid Potassium 40 mEq PO bid Enalapril 5 mg PO qd Sodium diet 2 gm Oxygen 6 L/min
- What is the significance of the findings of the chest X- Ray?
- Are there any collaborative problems that has been not considered?
- Is Mrs. JE provided with appropriate drug regimen? Justify.
For Case Study-3 Answer, Click here .
For more Pharm.D Case studies. Click here.
Case Study-4 ( Case of Congestive Heart Failure in Pediatrics patient)
A 6 weeks old female presented to the emergency room with the chief complaints of lethargy, poor feeding, and respiratory distress. Her parents reported that she sweats a lot on her forehead when feeding. Her parents have also noted her to be increasingly lethargic, with tachypnea, and retractions.
- She is the product of a G3P2, full term, uncomplicated pregnancy. Delivery was unremarkable except for meconium stained fluid. Her pediatric follow-up has been poor.
- Developed a febrile illness with cough, rhinorrhea, and emesis prior 2 weeks
- Subsequently developed progressive respiratory distress.
Objective Evidence:
- Acyanotic, Lethargic, tachypneic, mildly cachectic
- Mild to moderate subcoastal & intercoastal Retractions
Heart rate : 160 / min
Respiratory rate : 72 / min
Temp. : 98.24 ᵒF
HEENT exam : unremarkable
- Neck is supple without lymphadenopathy.
- Skin is clear with no rashes or other significant skin lesions.
- Lungs have scattered crackles with slightly decreased aeration in the left lower lobe.
- Precordium is mildly active.
- Heart is of regular rate and rhythm, with a Grade II/VI holosystolic murmur at the mid lower left sternal border with radiation to the cardiac apex.
- S1 is normal and the S2 is prominent. An S4 gallop is noted at the cardiac apex. There are no rubs or valve clicks.
- Her abdomen is soft, non-distended, and non-tender.
- The liver edge is palpable 3 to 4 cm below the right costal margin. Bowel sounds are hypoactive.
- Capillary refill is 4 to 5 seconds (delayed).
- Chest x-ray: Moderate cardiomegaly with a moderate degree of pulmonary edema. No pleural effusions.
- 12 lead ECG: Sinus tachycardia, normal PR and QTc intervals, and a left axis deviation. Voltage evidence of biventricular hypertrophy is present. No significant Q-waves or ST segment changes are noted.
A large peri-membranous ventricular septal defect with non-restrictive left to right shunting. All cardiac chambers are dilated. Left ventricular contractility is at the lower range of normal. There is no pericardial effusion.
- Suggest the best therapeutic regimen to control/overcome the current situation.
- Should she be referred for surgical correction of Ventricular Septal Defect after the drug regimen has been started?
Go to Case Study-4 Answers | Other Case Studies
Case Study-5 ( Case of Angina Pectoris)
A 62-year-old male smoker with Type-2 Diabetes Mellitus and Hypertension presents with a 4-month history of exertional chest pain.
Physical examination shows a blood pressure of 152/90 mm Hg, but is otherwise unremarkable.
The ECG is normal, and laboratory tests show a fasting blood glucose value of 110 mg/dL, glycosylated hemoglobin 6.0%, creatinine 1.1 mg/dL, total cholesterol 160, LDL 120, HDL 38, and triglycerides 147 mg/dL.
He exercises for 8 minutes, experiences chest pain, and is found to have a 2-mm ST-segment depression in the inferolateral leads at the end of exercise.
The patient is diagnosed with chronic stable angina .
- What is the treatment goal and strategy for this case?
- Suggest the best follow-up for this case.
- What are the conditions which worsens the symptoms of angina (in general)?
Case Study-6 (Case of Angina Pectoris)
A Mr SW is a 48-year-old man going through a stressful time at work, who for the past 6 months, has been increasingly short of breath while walking to the bus. He has put this down to his ‘unhealthy ‘ lifestyle. Although he has cut down from two packets to one packet of cigarettes a week, reduced his alcohol intake from about 40 units to 25 units a week and is trying to lose weight (currently 1.8 m tall, weighing 100 kg). He sometimes finds himself short of breath with mild chest tightness, especially when he is running late. He has a strong family history of cardiovascular disease with his father having a stroke in his early 50s and his older brother having had a CABG (coronary artery bypass graft) 2 years ago. Both have encouraged Mr. SW to see his general physician due to his worsening symptoms.
Mr. SW was seen by a physician 2 years ago who prescribed aspirin 75 mg daily, atenolol 50 mg daily and a GTN spray to be used if he experiences chest pain. Since this time, he has stopped taking the aspirin, because he feels that he does not need it and he has stopped the atenolol for more than a year because he was feeling tired and read that it can cause impotence. He has used the GTN once but, after experiencing a headache and facial flushing, he has not used it since and he does not carry it with him.
After his current physician visit, he is prescribed with:
Aspirin 75 mg daily
Simvastatin 40 mg at night
Amlodipine 5 mg daily
GTN spray when required
- What information and counselling points would you include?
- How is stable angina managed?
- What options are there, if Mr. SW experiences further symptoms despite the use of amlodipine?
Go For Case Study-6 Answer | Go back to Case Studies | Go to Home
Case Study-7 (Myocardial Infarction)
A 50 year-old male ( Height -154 cm , weight – 70 kg ) who was auto driver visited to the clinic with chief complaints of chest pain. The patient was apparently alright till 3 h back, when he suddenly felt a vague chest pain present at the center of the chest. Pain was located in the substernal location and was radiating to the right side of the shoulder. The quality of the pain was dull aching, which was increasing in severity rapidly over few hours. Chest pain was aggravated by exertion. Pain was not relieved even during rest. There was profuse sweating associated with the chest pain, and also a sense of doom or impending death. There were mild dyspnea and palpitation associated with the chest pain. There was no history of pedal edema, abdominal distension and facial puffiness, loss of appetite/fullness, right hypochondriac pain, or increased neck pulsations. Chest pain was diffuse in nature and not localized. There is no relation of the chest pain to food intake. There were no associated vomiting and hematemesis. There was no history of trauma and no history of any psychological disorders in the past. Review of other systems was normal.
Past Medical History:
The patient is not a known diabetic, or hypertensive. He has had no similar history in the past.
Past Medication History:
The patient is not on any medications. There was no history of any intake of any cardiotoxic drugs (cancer chemotherapy or prolonged steroids).
Personal History:
The patient takes mixed diet and smokes 1 packet cigarette/day for last 15 years. There was no alleged history of any alcohol or illicit drug abuse.
Pulse rate : 120/min with regular rhythm
Blood pressure : Left hand – 138/94 mm Hg
Left leg -. 144/90 mm Hg.
Lab Findings:
Hb : 15 g/dL
WBC : 10,000 u/mcL
Creatinine clearance : 90 ml/min
ECG Finding :
There is ST elevation >2 mm in v2–v6, and >1 mm ST-elevation in lead 1 and aVL with some minimal reciprocal changes seen in lead 3 suggestive of anterior wall + lateral wall MI due to complete left anterior descending (LAD) occlusion. Likely in the proximal LAD.
Diagnosis : Acute Myocardial infarction
Treatment :
T. Aspirin 75 mg OD
T. Ticagrelor 90 mg BD (after initial loading dose of 180 mg)
T. Atorvastatin 80 mg OD HS
T. Metoprolol 50 mg OD
T. Ramipril 2.5 mg BD
T. Lasix + Spironolactone (20/50) mg OD
1. What is the latest definition of STEMI?
2. What are the classical ECG criteria for diagnosing STEMI ?
3. What are the different types of MI ?
4. Justify the treatment given to this patient.
5. Determine the duration of DAPT In this patient ?
For Case Study-7 Answers | Go to Guidelines | Go to other Case Studies
Case Study-8 (Myocardial Infarction)
Mr TR, a 54-year-old man, presented to his general physician with sudden-onset epigastric pain that started the previous night and ‘felt like trapped wind’ . This radiated through his back, up to his neck and into both shoulders/arms. He was extremely flatulent.
The patient was referred for coronary angiogram/percutaneous coronary intervention (PCI), which was carried out on site the same day. It showed the presence of a thrombus in the OM (obtuse marginal coronary artery). The distal LAD (distal left anterior descending coronary artery) and the RCA (right coronary artery) were 80% and 60- 70% stenosed, respectively.
Echocardiogram: normal LV function.
Diagnosis: NSTEMI
Two drug- eluting stents were inserted into the OM. The following drugs were prescribed post-PCI:
- Aspirin 75 mg daily
- Clopidogrel 75 mg daily
- Bisoprolol 2.5 mg daily
- Ramipril 1.25 mg at night
- Atorvastatin 40 mg at night
- Lansoprazole 30 mg daily
Mr TR was discharged after 3 days, after an uneventful outpatient stay, with the drugs listed above and a GTN spray to be used sublingually. Arrangements were made for an exercise tolerance test (ETT) in 6 weeks to determine whether further PCI was indicated, and for Mr TR to enter the local cardiac rehabilitation programme.
- Is the diagnosis & treatment given to Mr TR justified? Explain.
- Is there a need of counselling?
Go for Case Study-8 Answers | Explore more Case Studies | Go to Guidelines
Case Study-9 (Hyperlipidemia)
A 62-year-old male is referred for management of elevated cholesterol. He has history of obesity, hypertension, and hyperlipidemia. He had a non–ST-segment elevation myocardial infarction (NSTEMI) one year ago with drug-eluting stent placement in his right coronary artery. His current medications include aspirin 81 mg daily, lisinopril 20 mg daily, and metoprolol XL 50 mg daily. His physical exam is notable for a body mass index (BMI) of 32 kg/m 2 but is otherwise unremarkable. His blood pressure is 135/85 mm Hg.
A recent lipid panel shows the following:
- Total Cholesterol: 226 mg/dL
- Triglycerides: 154 mg/dL
- High-Density Lipoprotein Cholesterol (HDL-C): 39 mg/dL
- Low-Density Lipoprotein Cholesterol (LDL-C): 190 mg/dL
- He has a normal creatinine and normal liver enzymes. His TSH and vitamin D levels are within normal limits.
- What would be the target goal for LDL-C in this patient?
- What is the drug of choice in this patient to treat LDL-C?
- What would be the treatment plan, if the patient’s LDL-C goal is not reached even after initiation of statin therapy?
- What would be choice of drug in this patient, if he is intolerant to statin therapy?
Go for Case Study-9 Answers | Explore more Case Studies | Refer Guidelines
Case Study-10 ( Hyperlipidemias)
Four months ago, a 46-year-old man was admitted to hospital with acute chest pain. A subendocardial inferior MI was diagnosed and he was treated with thrombolytics and aspirin. After discharge, he complained of angina, and coronary angiography was performed. This showed severe triple-vessel disease not suitable for stenting, and coronary artery bypass grafting was performed. He is attending a cardiac rehabilitation clinic and he has had no further angina since his surgery.
Family History:
He has a strong family history of ischaemic heart disease, with his father and two paternal uncles having died of myocardial infarctions in their 50s; his 50-year-old brother has angina. He is married with two children.
Social History:
He smokes 25 cigarettes per day and drinks at least 40 units of alcohol per week.
Medication History:
He is taking atenolol and aspirin.
Examination :
He is slightly overweight (85 kg; body mass index ) 28). He has tar-stained nails. He has bilateral corneal arcus, xanthelasmata around his eyes and xanthomata on his Achilles tendons. He has a well-healed midline sternotomy scar. His pulse is 64/min regular, blood pressure 150/84 mmHg. He has no palpable pedal pulses. His respiratory, gastrointestinal and neurological systems are normal.
Lab Investigation:

Urinalysis : no abnormality detected.
- What is the metabolic abnormality present?
- Discuss the Patient counselling for this case?
Go to Case Study-10 Answers | Explore more Case Studies | Refer Guidelines
Case Study-11 ( Arrthymias )
(Arrhythmia) A 2 month-old male who presents to the emergency room with a chief complaint of fever, lethargy, and poor feeding for the past 36 hours. His parents began noticing increasing lethargy and tiring with feeding and increased work of breathing for about 12 hours prior to presentation.
He is the product of a G2P1, full term, uncomplicated pregnancy and spontaneous vaginal delivery. Nursery course was uneventful.
Vital Sign: Temp: 99.32 ᵒF,
Heart Rate: 240 per min,
Respiratory Rate: 72 per min,
BP: 87/64mmHg, oxygen saturation 98% in room air.
He is well developed, well nourished, but pale, lethargic and tachypneic, with mild subcostal retractions. HEENT exam is normal . Neck is supple without adenopathy.
Lungs have good aeration with fine crackles and mild retractions. His heart is tachycardic with a regular rhythm. No murmur, rub, or valve clicks are heard. His abdomen is soft, non-distended, non-tender, and without masses. His liver is 2 to 3 cm below right costal margin. His feet and hands are cool.
His peripheral pulses are 1+ to 2+ (out of 4+) throughout. Capillary refill time is 3 to 4 seconds. He has no rashes or other significant lesions.
Chest x-ray shows mild cardiomegaly and mild pulmonary edema. A 12 lead electrocardiogram shows a narrow complex tachycardia (rate of 240 bpm) with no visible P-waves (rhythm strip below).
The patient is felt to be in supraventricular tachycardia and mild congestive heart failure.
A peripheral IV is started and he is given a rapid IV bolus dose of adenosine. The patient immediately becomes briefly bradycardic followed by resumption of a normal sinus rhythm at a rate of 140 beats per minute. He is admitted for overnight observation and initiation of an anti-arrhythmic medication.
A 12-lead electrocardiogram (ECG) following conversion shows no evidence of a delta-wave, so he is started on digoxin .
- What medicine used to treat Supraventricular tachycardia is contraindicated specifically in Wolff-Parkinson-White syndrome?
- What would be the possible differential diagnosis?
Go For Case Study-11 Answers | Explore More Case study | Go to Guidelines
Case Study-12 ( Atrial Fibrillation )
A 67-year-old man presents to the emergency department with palpitations and dyspnea which began approximately 4 hours ago. He has a history of hypertension, diabetes, and gastroesophageal reflux disease, and LVH. On further questioning, he reports drinking 1 cup of coffee daily and 1-2 beers on the weekends.
He denies binge drinking and the use of herbal or alternative medications. He quit smoking 10 years ago. His urine drug screen is negative. His body mass index is 36 and he admits to snoring and daytime sleepiness. He is at high risk for obstructive sleep apnea (OSA). His current medications include lisinopril, metformin, and omeprazole. He has no history of congestive heart failure, stroke, or transient ischemic attack (TIA).
He appears to be in mild respiratory distress.
Blood pressure is 88/60 mmHg, pulse rate is 140 bpm, respiratory rate is 24/min, and temperature is normal. Oxygen saturation is 90% on 40% oxygen by face mask. Cardiac exam reveals tachycardia with an irregularly irregular tachycardic rhythm. There are crackles in the lower lung fields.
Electrocardiogram demonstrates atrial fibrillation (AF) with rapid ventricular rate.
- What would be the most appropriate initial management in this patient?
- Calculate the risk of thromboembolism and risk of bleeding in this patient?
Go for Case Study-12 Answers | Explore more Case Study | Go to G uidelines
Case Study-13 ( Case study of Asthma )
A 29-year-old man with mild persistent asthma presented to an outpatient office for a follow-up visit. He was originally referred 6 months ago by his primary care provider after having an asthma exacerbation which required treatment in an emergency room.
At his initial visit, he reported wheeze and cough 4 days a week and nocturnal symptoms three times a month. Spirometry revealed forced vital capacity (FVC) 85% predicted, forced expiratory volume in 1 second (FEV 1 ) 75% predicted, FEV 1 /FVC 65%, and an increase in FEV 1 of 220 ml or 14% following an inhaled short-acting bronchodilator. He was placed on a low-dose inhaled corticosteroid twice a day and a short-acting inhaled beta-agonist as needed.
He returned 4 weeks later improved, but with continued daytime symptoms 2 days a week. He also had symptoms of rhinitis; therefore he was referred to an allergist for evaluation. Skin testing was positive for trees, ragweed, dust mites, and cats, and he was prescribed a nasal steroid spray and nonsedating oral antihistamine. He presents today and reports no asthma exacerbations since his last visit.
Furthermore, during the past 4 weeks, he has not been awakened by his asthma, experienced morning breathing symptoms, missed work, had any limitations in activities due to asthma, or required the use of rescue albuterol. He currently denies shortness of breath or wheezing. He performs aerobic exercise 4 days a week for 45 minutes per session without symptoms, provided he premedicates with a short-acting inhaled beta-agonist. His review of symptoms is otherwise unremarkable.
His current medications include low-dose inhaled corticosteroid, 1 puff twice a day; steroid nasal spray, 2 puffs each nostril daily; a nonsedating antihistamine, 1 tablet daily; and inhaled beta-agonist, 2 puffs as needed.
His past medical history is significant for intermittent asthma diagnosed at age 13 and frequent “colds.” He has never required hospitalization for an asthma exacerbation. He works as a hospital microbiologist and does not smoke, drink alcohol, or use illicit drugs. He recently moved to a pet-free apartment complex and instituted dust mite protective barriers for his bedding. His family history is noncontributory.
Physical Exam
On physical exam, he is an age-appropriate man in no acute distress. His height and weight are proportionate and resting oxygen saturation as measured by a pulse (SpO 2 ) is 98% on room air. A Head and neck exam revealed mild erythema of the nasal mucosa. A heart exam revealed normal heart tones, no murmurs, gallops or rubs, and the lungs were clear to auscultation. Extremities were free of oedema, cyanosis, or clubbing.
Lab: In the office, spirometry is completely normal. He states he feels great and inquires about stopping his inhalers, particularly his inhaled steroid.
1. Based on current evidence, which of the following would be the most appropriate recommendation regarding his asthma medication regimen?
A. Maintain current medication regimen; no adjustment is indicated.
B. Discontinue the inhaled corticosteroid; maintain on an Inhaled beta-agonist as needed.
C. Decrease the inhaled corticosteroid to 1 puff daily.
D. Discontinue the inhaled corticosteroid; start a leukotriene modifier at bedtime.
E. Discontinue the inhaled corticosteroid; start low-dose inhaled corticosteroid/long-acting beta-agonist, 1 inhalation at bedtime.
2. Which of the following should be done routinely with each follow-up visit?
A. Methacholine challenge testing
B. Sputum for eosinophils
C. In-office peak flow recordings
D. Review of proper inhaler technique and adherence
E. Measurement of exhaled nitric oxide (NO)
3. What findings would suggest that the patient requires a step-up in asthma medication?
A. Two or more nighttime awakenings per month due to Asthma.
B. Two or more interruptions in daytime activities per month due to asthma .
C. Peak flow readings 85% of personal best
D. Short-acting beta-agonist for rescue once a week
E. Short-acting beta-agonist 4 days/week prior to exercise
4. The patient was provided with an asthma action plan to follow at home. Which component of the asthma action plan is considered the most critical element for improving asthma outcomes?
A. A list of the patient’s controller and rescue medications
B. A list of symptoms indicative of worsening asthma
C. Medication changes based on personal-best peak flow readings
D. Instructions describing when, how, and how long to increase medications when symptomatic
E. Medication changes based on symptoms
5. How often is spirometry testing recommended if the previous readings are normal and the patient’s asthma is well controlled?
A. Every 1 to 2 years
B. Only if asthma controller medications are changed
C. Only if symptomatic
D. Every 4 to 6 months
E. Every follow-up visit

Explore more Case Studies | Go to Case Study-13 Answers | Guidelines
Case Study-14 ( Case Study - II of Asthma )
A 14-year-old girl with a history of asthma requiring daily inhaled corticosteroid therapy and allergies to house dust, mites, cats, grasses, and ragweed presents to the emergency department in mid-September, reporting a recent “cold” complicated by worsening shortness of breath and audible inspiratory and expiratory wheezing.
She appears frightened and refuses to lie down but is not cyanotic.
Her pulse is 120 bpm, and respirations are 32/min.
Her mother states that she has used her albuterol inhaler several times a day for the past 3 days and twice during the previous night. She took an additional two puffs on her way to the emergency department, but her mother states that “the inhaler didn’t seem to be helping so I told her not to take any more.
1. What emergency measures are indicated?
2. How should her long-term management be altered?
Case Study-14 Answer | More Case Studies | Guidelines
Case Study-15 ( Chronic Obstructive Pulmonary Disease : COPD Case Study)
Mrs. Glenda is a 60-year-old and has recently retires from her job working for a firm that manufactures fabrics. She is a thin lady who appears older than her stated age. Glenda visits her GP as she beginning to get short of breath while climbing the stairs and is struggling to walk to the end of her road. She explains to the GP that for the past six months she has become increasingly short of breath while carrying out daily activities.
Glenda takes no regular medications and has no history of drug allergies .
She says she has not had any acute changes in her breathing, but she does have a chronic cough that produces around one or two tablespoons of clear sputum daily. Her cough has not changed recently, and the colour and volume of her sputum have also remained unaltered. She says she is not suffering from chest pains or wheezing and has not been coughing up blood.
She has smoked at least ten cigarettes a day since she was 20 but has recently cut down to five a day because of her shortness of breath. In the last few years, she has had at least two chest infections each year requiring treatment with antibiotics.
The GP suspects COPD and conducts spirometry testing, the results of which are:
| FEV1 | 1.2 L |
| FEV1 predicted | 2.2 L |
| FEV1 % | 55% |
| FVC | 1.79 L |
| FEV1/FVC | 0.67 |
1. What clinical features and risk factors of COPD does glenda exhibit? What grade of severity does glenda’s COPD fall into?
2. What initial treatment would you recommend for glenda?
3. Glenda continues to report that her breathlessness is getting worse. Her medical research council dyspnea score is now four and in the last few days she has been producing more sputum than usual. Her sputum has turned a yellow green colour. What does these changes indicate & what treatment would you recommend?
Explore more Case Studies | Guidelines | Case Answers of this COPD Case Study-15
Case Study-16 ( Case of COPD with comorbidity )
A 63-year-old woman, 67 kg, is admitted to hospital with chest pain, shortness of breath and sweating. She is seen in casualty and treated using a salbutamol nebuliser. She looks obese. She has been a life-long smoker who stopped one day ago.
Her previous medical history includes chronic obstructive pulmonary disease (COPD) for 10 years, the last admission to hospital was two weeks ago; ischaemic heart disease since 1995, myocardial infarction 4 years ago; osteoporosis diagnosed 3 years ago; hypertension diagnosed 9 years ago; and pulmonary embolism two months ago.
On examination:
Blood pressure 105/90 mmHg
Heart rate 90 bpm
Respiratory rate 20 breaths per minute.
Arterial blood gases on admission:
pH 7.388 on 35% O2
PCO2 9.67 kPa
PO2 6.5 kPa.
Oxygen saturation: SpO2 89%. Lungs were hyperinflated, no wheeze, few right base crepitations.
Laboratory tests at admission :
WCC 16.5 × 109/L (4–11 × 109/L)
Na+ 140 mmol/L (135–145 mmol/L)
K+ 4.4 mmol/L (3.5–5 mmol/L)
Creatinine 75 micromol/L (59–104 micromol/L)
Urea 7.8 mmol/L (1.7–8.3 mmol/L)
Hb 11.6 g/dL (13–17 g/dL)
Medication on admission:
Prednisolone 10 mg o.d.
Fluticasone inhaler 500 micrograms b.d.
Aspirin 75 mg o.d.
Bumetanide 1 mg o.d.
Combivent nebs 2 q.d.s.
Enalapril 5 mg o.d.
Uniphyllin Continus 200 mg bd
Senna 2 tablets nocte
Warfarin 5 mg o.d.
Zopiclone 7.5 mg nocte
Diclofenac 50 mg p.r.n.
Oxygen (O2) 2 L nasal specs.
1. How the sign, symptoms & pathophysiology of COPD, relates to the patient?
2. Comment on the current drug therapy and describe the role of O2 in this patient.
3. What are the social issues in treating this patient at home?
Case Study-16 Answer | Explore more Case Studies | Guidelines
Case Study-17 ( Type-1 Diabetes in Pregnancy )
Mrs Jaya is a 36-year-old married lady who has type 1 diabetes. She undertook a home pregnancy test because she was feeling particularly nauseated in the mornings and her period was late. The test was positive confirming that she was pregnant.
However, at 8 weeks, she experienced vaginal bleeding and abdominal pain . She attended the Accident & Emergency department, where a miscarriage was confirmed.
Upon questioning, it was discovered that she had been taking folic acid 400 μcg daily for the previous 6 months but had not received any pre-conception diabetes care.
Her most recent HbA1c was 7.3% (56 mmol/mol). Her regular medications are ramipril 10 mg daily , simvastatin 40 mg daily , insulin glargine at night and insulin aspart three times daily with meals.
- Why should women of childbearing age be offered advice about pregnancy?
- Was she taking appropriate dietary supplements prior to conception?
- What advice should she be given with respect to her regular medication?
Go to Case Study-17 Answers
Case Study-18 (Type-2 Diabetes)
Case scenario:.
Mk a 68-yr-old woman who has previously diagnosed with type 2 diabetes 15 years ago came to the clinic for her regular follow-up. she reports paraesthesia’s in her feet at night but her sleep was not disturbed by these symptoms. She checked her blood sugars at home two to four times each day and found them to range from 100-250 mg/dl.
She reported compliance with her medications that included lisinopril 20 mg OD, hydrochlorothiazide 25 mg OD, diltiazem 180 mg OD, glargine insulin 0.4 units/kg , atorvastatin 40 mg , and aspirin 81 mg OD.
Past medical history & medication history :
- Type 2 diabetes, hyperlipidaemia and hypertension diagnosed at the age of 47. For these conditions she was treated with metformin, atorvastatin, and hydrochlorothiazide and maintained Hb A1c below 7.0 %, LDL below 100 mg/dl, and blood pressure below 135/80 mmHg for many years.
- At the age 59, she was noted to have an increase in her urine albumin to 54 mg/g of creatinine and lisinopril was added to her regimen.
- Three years later at the age 62, her serum creatinine increased to 1.56 mg/dl, and her GFR was estimated to be 36 ml/min. Her Hb A1c increased to 7.2% and she began to experience paraesthesia’s in her feet. The metformin was discontinued, and she was started on glargine insulin.
- At age 63, she developed proliferative retinopathy in her right eye and underwent laser photocoagulation. Bilateral macular edema developed at age 65.
Examination – Present visit:
- BMI – 38.2 kg/m² (height – 151 cm, weight – 87 kg)
- Blood pressure – 142/90 mmHg
- Heart rate – 68 bpm
- Retinal exam – significant for panretinal photocoagulation changes with scattered dot haemorrhages and macular edema in both eyes.
- Heart, lung and abdominal exams were unremarkable.
- Extremities – Pulses in her feet were reduced, but her feet were warm and without ulcers. She was unable to detect a Semmes Weinstein 5.07 monofilament on the soles of her feet.
Lab parameters:
- Hb A1c : 7.9%.
- Serum creatinine : 2.45 mg/dl.
- GFR : 20 ml/min.
- Calcium : 9.8 mg/dl. Phosphorus : 4.6 mg/dl.
- PTH : 75 pg/ml
- Total cholesterol : 188 mg/dl,
- Triglycerides :82 mg/dl,
- High-density lipoprotein cholesterol :42 mg/dl,
- LDL cholesterol : 131 mg/dl
- Hb : 10.8 g/dl.
- Prepare pharmaceutical care plan for this case study.
Go to Case Study-18 Answers
Case Study-19 (Thyroid Disorder)
A 55-year-old man presents to his general practitioner, complaining of lack of energy. He has become increasingly tired over the past 18 months. He works as a solicitor and describes episodes where he has fallen asleep in his office.
He is unable to stay awake after 9:30 pm, and sleeps through until 7:30 am. He finds it difficult to concentrate at work, and has stopped playing his weekly game of tennis. He had an episode of depression 10 years ago related to the break-up of his first marriage. He has no current personal problems. He has had no other major illnesses.
His brother developed type 1 diabetes mellitus at the age of 13. On direct questioning, he has noticed that he has become more constipated but denies any abdominal pain or rectal bleeding. He has put on 8kg in weight over the past year.
Examination:
On examination he is overweight. His facial skin is dry and scaly. His pulse is 56/min, regular and blood pressure 146/88 mmHg. Examination of his cardiovascular, respiratory and abdominal systems is unremarkable. Neurological examination was not performed.
Haemoglobin 10.3 g/dL 13.3–17.7 g/dL
Mean corpuscular volume (MCV) 92 fL 80–99 fL
White cell count 4.3 x 10⁹/L 3.9–10.6 x 10⁹/L
Platelets 154 x 10⁹/L 150–440 x 10⁹/L
Sodium 140 mmol/L 135–145 mmol/L
Potassium 4.4 mmol/L 3.5–5.0 mmol/L
Urea 6.4 mmol/L 2.5–6.7 mmol
Creatinine 125 μmol/L 70–120 μmol/L
Glucose 4.7 mmol/L 4.0–6.0 mmol/L
Calcium 2.48 mmol/L 2.12–2.65 mmol/L
Phosphate 1.20 mmol/L 0.8–1.45 mmol/L
Cholesterol 6.4 mmol/L 3.9–6.0 mmol/L
Triglycerides 1.4 mmol/L 0.55–1.90 mmol/L
Urinalysis: nothing abnormal detected (NAD)
- What is the likely diagnosis? Main differential diagnosis?
- How would you further manage this patient?
Go to Case Study-19 Answers
Case Study-20 (Thyroid Disorder)
A 40-year-old woman (51kg) presents with complaints of left side chest pain since 4 months that last for 1-2 hours and radiates to back, increase on exertion; associated with palpitation, perspiration. Headache since 1 month in occipital region that lasts 30-40 min. Generalised weakness, easy fatigue, facial swelling, peri-orbital swelling, bilateral lower limb swelling.
Past medication history :
Blood transfusion 2 times 4 months back.
Temp : Afebrile Pulse: 86 beats/min
BP: 130/84mmHg (pattern for hypotension seen for 2 days)
Lab details:
Hb 10.1 g% 13-17g%
WBC 4600 cumm 4000-11,000 cumm
PCV 31.3% 36-47%
MCV 85.2fL 82-92fL
MCH 27.6pg 27-31pg
MCHC 32.3% 32-36%
Platelet 1.55 lac/cumm 1.5-4.5 lakh/cumm
RBC 3.67 millions/ μ L 4.4-5.9 millions/ μ L
RDW 17.7% 13-15 %
Pus & epithelial cells 1-2/hpf
Reticulocyte count 0.5% 0.5-2.5%
Na 135 mmol/L 135-145mmol/L
K 4.2mmol/L 3.5-5.5mmol/L
Cl 100mmol/L 98-110mmol/L
Creatinine 0.8mg% 0.6-1.3 mg%
Glucose : RBS 103mg% 70-140mg%
RBC Smear : Mild anisocytosis
Stool Test ( Occult Blood) : Positive
TSH >100 miu/ml >15miu/ml
Total T4 0.10 ng /dL 0.82- 2ng/dL
Free T4 0.10ng /dL 0.9- 2.3 ng/dL
ECG : normal sinus rhythm , poor P-wave progression
LVEF: 60%; Grade 1 diastolic function; mild MR; mild TR; mild PAH; Concentric LVH
Local part
Findings: Left lobe P/O — hyperplastic nodule
Both lobe P/O – inflammatory etiology thyroiditis
Inj pantoprazole 40mg 12hrly
Infusion 0.45% NS 500ml + 2 ampoule Optineuron at 60cc/hr
Tab Fdson MP Forte 0-1-0
Tab febac XT 1-0-1
Tab Thyronorm 25mg 1-0-0
- What is the likely diagnosis in this case? And are lab finding clinically justified?
- What are the Pharmacist Intervention points in this case?
- Patient counselling regarding drug & disease?
- Write the Generic Names of above advised drugs.
Go to Case Study-20 Answers
Case Study-21 (Thyroid Disorder)
A 34-year-old pregnant woman came to the emergency department with complaints of fetal movements not felt since 1 day ago.
At present the patient is the third pregnant at the age of 23-24 weeks, so far the regular control to the midwife and specialist doctors.
The patient has never experienced bleeding or trauma before. A history of previous labour was normal with a healthy baby. The patient has been suffering from Grave’s disease for the past 10 years and has not been treated for one year.
During pregnancy, the patient feels palpitations and tightness during activity. The patient also complaint about weight loss and fatigue.
The patient’s general condition appeared weak with a blood pressure of 197/87 mmHg and pulse 148 times per minute regular.
The exophthalmos and the thyroid gland feel soft in the neck without pain.
Laboratory tests results:
An increase in FT4 levels of 75.62 pmol / L and low TSHs levels of 0.005 µIU / mL. Wayne index with a value of 23 or found signs of toxicity and the Burch Wartofsky scale with a value of 45 or impending thyroid storm.
Q1 . What is the likely diagnosis ?
The patient was taken to the endocrine section and given methimazole 30 mg twice daily, propranolol 30 mg twice daily, and Lugol 5 drops per 6 hours .
The termination of pregnancy is carried out by vaginal delivery and administration of oxytocin postpartum.
The patient complained of shortness of breath and anxiety after two hours postpartum.
Patient was consulted in the Cardiology division with pulmonary oedema and advised giving diuretics and vasodilators .
Patient was given nitroglycerin at a dose of 5 meq per hour and furosemide 30 mg per hour intravenously to improve the condition of pulmonary oedema.
Close monitoring is carried out on the patient for several days until the patient’s condition is stable.
Q2. Was the Treatment given to the patient justified according to clinical condition?
Q3. Widely used anti-thyroid drugs in pregnant women with hyperthyroidism?
Patient is planned to go home for outpatient care after monitoring side effects and postpartum complications. Hemodynamic condition is stable with blood pressure 110/70 mmHg and pulse 92 times per minute. Patient was given anti-thyroid therapy and beta-blockers on discharge. During treatment at home, patient is advised to monitor thyroid function to the clinic every once a month.
Q4. What should be the Patient Counselling points ?
Go to Case Study-21 Answers
Case Study- 22 (Thyroid Disorder)
A 55-year-old woman presents with complaints of pus discharge per vagina since 8-9 months. Decreased urine output. Palpitation 3-4 months. Shortness of breath 4-6 months
Past medical history :
Hysterectomy 10-12 years ago
Social History :
“ Chulha ” user
Temp : Afebrile Pulse: 140 beats/min
BP: 126/80mmHg
Provisional Diagnosis :
Atrial Fibrillation w/ hemorrhoids w/ hyperthyroidism w/ perianal fissure.
Hb 13.2 g% 13-17g%
WBC 8100 cumm 4000-11,000 cumm
Platelet 2.11 lac/cumm 1.5-4.5 lakh/cumm
Pus cell 5-6
Epithelial cells 1-2/hpf
Na 142 mmol/L 135-145mmol/L
K 3.8mmol/L(3 rd day: 2.9) 3.5-5.5mmol/L
Cl 106mmol/L 98-110mmol/L
Creatinine 0.6mg% 0.6-1.3 mg%
Urea 24
Mg 2.1
Ca 8.6
Protein 6.1 g % 6.0-8.0 g %
Albumin 3.4g% 2.7-5.0 g %
Globulin 2.7 g% 2.5-4.0 g %
SGOT 59
SGPT 27
Bilirubin 1.6
TSH 0.01 0.39-5.0
Free T3 7.01 2.1-3.8
Free T4 4.28ng /dL 0.9- 2.3 ng/dL
CRP <10 0-6.0
ECG : Flat T- wave (V5) atrial fibrillation.
ECO : Mild MR; Mild TR; LVEF: 60%
Inj Dilzem 12.5mg stat w/ 10ml NS
Tab Dilzem 30mg 1-1-1
Inj Lasix 20mg 1-0-0
Inj PAN 40mg 24 hrly
Tab Metro 400mg 1-1-1
Syp Duphalac 2tsp 0-0-1
Tab Ciplox T2 500/600 1-0-1
Tab Neomercazole 10mg 1-1-1
Tab Propanolol 10mg 1-0-1
Syp Potklor 15ml 1-1-1
Metrogyl ointment 1-1-1-1
Inj NS + KCl 1 amp 12hrly
- Are there any drug-drug interactions?
- Is the dosing of medication for hyperthyroidism, according to standard treatment guidelines?
- What should be Patient counselling in this case, regarding drug & disease?
Go to Case Study-22 Answers
Case Study-23 (OB/GYN: Oral Contraceptive Use)
An 18-year-old female presents with an absence of periods for 6 months. This has occurred twice before in the past but on both occasions menstruation returned so she was not too concerned. Her periods started at the age of 12 years and were initially regular.
She has no medical history of note and denies any medication. She is currently in her first year at university. She sometimes follows inconsistent diet plan. However, She runs most days and reports a ‘healthy ‘ diet avoiding carbohydrate foods and meat. She is the oldest of three siblings and her parents separated when she was 12 years. She has minimal contact with her father and lives mainly with her mother who she says she gets on well with. She has had a boyfriend in the past but has veered away from any sexual relationships.
The woman is tall and thin with a body mass index (BMI) of 15.5 kg/m².
There is evidence of fine downy hair growth on her arms.
Heart rate is 86/min and blood pressure 100/65 mmHg.
Abdominal examination reveals no scars or masses, and genital examination is not performed.
INVESTIGATIONS:
Follicle-stimulating hormone 1.0 IU/L Day 2-5
Luteinizing hormone 0.8 IU/L Day 2-5
0.5-14.5 IU/L
Oestradiol 52 pmol/L 70-600 pmoI/L
Prolactin 630 mu/L 90-520 mu/L
Testosterone 1.6 nmol/L 0.8-3.1 nmol/L
Diagnosis : Hypogonadotrophic hypogonadism
- What should be the further investigation ?
- How, this patient would be managed ?
- What Patient counselling points should be included in this case?
Go to Case Study-23 Answers
Case Study-24 (OB/GYN: Oral Contraceptive Use)
A 19-year-old female was referred by her general practitioner with increased hair. She first noticed the problem when she was about 16 years old and it has progressively worsened such that she now feels very self-conscious. It also affects her forming relationships.
The hair growth is noticed mainly on her arms, thighs and abdomen. Hair has developed on the upper lip more recently. She has tried shaving but this seems to make the problem worse. She feels depilation creams are ineffective. Waxing is helpful but very expensive and she has bleached her upper-lip hair.
Her GP has not prescribed any medication in the past.
There is no significant previous medical history of note. Her periods started at the age of 13 years and she bleeds every 30-35 days. The periods are not painful or heavy and there is no intermenstrual bleeding or discharge. She has never been sexually active.
Examination
On examination she has an increased body mass index (BMI) of 29 kg/m². The blood pressure is 118/70 mmHg. There is excessive hair growth on the lower arms, legs and thighs and in the midline of the abdomen below the umbilicus. There is a small amount of growth on the upper lip too.
The abdomen is soft and no masses are palpable. Pelvic examination is not indicated.
INVESTIGATIONS
Follicle-stimulating hormone (FSH) 7 IU/L Day 2-5
1-11 IU/L
Luteinizing hormone (LH) 12 IU/L Day 2-5
0.5-14.5 IU/L
Prolactin 780 mu/L 90-520 mu/L
Testosterone 3.2 nmol/L 0.8-3.1 nmol/L
Thyroid-stimulating hormone 4.9mu/L 0.5-5.7 mu/L
Free thyroxine 14.7pmol/L 10-40pmol/L
Provisional Diagnosis : Polycystic ovarian syndrome(PCOS)
Clinical features: Hirsutism , acne, increased BMI and slight menstrual irregularity
Go to Case Study-24 Answers
Case Study-25 (Hormone Replacement Therapy)
History of present illness :.
A 51-year-old newly postmenopausal woman suffering from intense hot flashes and night sweats, as well as anxiety, insomnia, and stress, presents to the hospital.
The doctor presents a breakdown of the patient’s self-reported symptoms before going into the details of her test results – where she highlights the biochemical factors that explain both her symptoms and her observed results.
Symptoms she rated as severe , included, depression, anxiety, and sleep disturbances , moderate symptoms included hot flashes, night sweats, foggy thinking, vaginal dryness, and mood swings. In addition, she had multiple symptoms that she rated as mild in severity.
The Patient had already tried multiple supplements in an attempt to address her own symptoms – these included elements like magnesium, calcium, selenium, zinc, and copper, as well as L-theanine and Rhodiola, vitamin D, fish oil, and some probiotics.
Investigation:
Saliva Hormone Test Results:
Name Lab value Normal range
Estrogen hormone 0.3 0.9-3.1 pg/ml
Progesterone hormone 5 12-100 pg/ml
DHEA 1 2-23 ng/ml
Testosterone 90 16-55 pg/ml
|
Serotonin metabolite 5-HIAA DOPAC
|
Neurotransmitter Test revealed:
LOW levels of:
Nor Epinephrine
- What should be the further investigation for this patient ?
- Give the provisional diagnosis for this case.
Go to Case Study-25 Answers
Case Study-26 (Hormone Replacement Therapy)
A 25 year-old woman with menarche at 13 years and menstrual periods until about 1 year ago.
Complains of hot flushes, skin and vaginal dryness, weakness , poor sleep and scanty and infrequent menstrual periods of a year duration.
She visits her gynecologist, who obtains plasma levels of follicle-stimulating hormone and luteinizing hormone, both of which are moderately elevated.
She is diagnosed with premature ovarian failure, and estrogen and progesterone replacement therapy is recommended.
A dual energy absorptiometry scan (DEXA) reveals bone density t-score f <2.5 SD, ie., Frank osteoporosis.
- How should the ovarian hormones she lacks be replaced?
- What extra measures should she take for her osteoporosis while receiving treatment?
Go to Case Study-26 Answers
Case Study-27 (Osteoporosis)
History of present illness:.
A 73-year- old woman presenting for a physical examination who looks and feels healthy and well.
Medication history:
Takes a multivitamin daily plus a calcium tablet
History of low-trauma Colles’ fracture (11 years ago)
Physical Examination:
Weight: 55 kg (121 lbs.)
Height: 157 cm (5’2”)
Body Mass Index (BMI): 22.3 kg/m2
*Changes in height and weight can be signs of vertebral fractures
INVESTIGATION:
BMD : Value
Spine -3.6;
Hip -2.0
Provisional Diagnosis : Osteoporosis with moderate risk of fracture
- What all investigations are needed for the further management?
- How this patient would be managed ?
- How will you do the Patient counselling in this case?
- Mention the indications for BMD testing.
Case Study-28 (Osteoporosis)
A 64-year-old retired firefighter Retired nine years ago; now doing contract carpentry Presents for physical examination, complaining his back has been “worse than usual” the past three weeks.
On no medications
Prior smoker (45 pack/year history)
Quit smoking one year ago
Height: 180 cm (5’11”)
Patient recalls being 185.5 cm (6’1”)
Weight: 80 kg (up 5 kg from one year ago)
Body mass index (BMI): 24.7 kg/m2
*Other indicators of vertebral fracture in physical examination: Rib-pelvis distance and occiput-wall distance
INVESTIGATION:
Screening for osteoporosis with dual energy X-ray absorptiometry (DXA) is T-score -1.9 at femoral neck
Lateral thoraco-lumbar spine X-ray is ordered to rule out vertebral compression deformities
*The radiologist makes note of two vertebrae being wedge shaped and just meeting the criteria for vertebral compression fracture
- What is the significance of T- Score?
Go to Case Study – 28 Answers
Case Study-29 (Glaucoma)
The patient, a 61 year-old female retired school teacher, has not had an eye exam in 10 years. She reports no problems with driving, watching TV, computer or reading. She uses over-the-counter readers for close work. She admits to mild eye burning feeling after reading for long periods of time or in the afternoons. She denies any flashes, floaters, pain, redness or double vision.
Past Ocular History:
Presbyopia. No prior eye surgeries, hx of eye trauma, amblyopia or strabismus.
Ocular Medications:
Hypertension
Surgical History:
Cesarean delivery x 1
Past Family Ocular History:
Cataract surgery in her mother and father. Negative for macular degeneration, glaucoma or blindness.
Never smoked
Medications :
Hydrochlorothiazide
Allergies :
Denies any recent illness or any new CNS, heart, lungs, GI, skin or joint symptoms.
Ocular Exam:
Visual Acuity (cc):
IOP (tonoapplantation):
OD: 21 mmHg
OS: 23 mmHg
Equal, round and reactive to light, no APD
Extraocular Movements:
Full OU, no nystagmus
Confrontational Visual Fields:
Full to finger counting OU
Normal, both sides
Lids and Lashes: Normal OU
Conjunctiva/Sclera: Normal OU
Cornea: Clear OU; no krukenberg spindle or embryotoxon
Anterior Chamber: Deep and quiet OU
Iris: Normal, no neovascularization or atrophy
Lens: 1+ nuclear sclerotic cataracts OU
Anterior Vitreous: Clear OU
Dilated Fundus Examination:
OD: Clear view, CDR 0.7 with sharp optic disc margins (no obvious rim thinning or disc hemorrhage); flat macula with normal foveal light reflex; normal vessels and peripheral retina.
OS: Clear view, CDR 0.8 with sharp optic disc margins (no obvious rim thinning or disc hemorrhage); flat macula with normal foveal light reflex; normal vessels and peripheral retina
Gonioscopy: Open angles with minimal pigmentation in the trabecular meshwork, no synechiae OU
Automated visual field test: superior arcuate defect in both eyes
Pachymetry: 560 OD; 551 OS (within normal range)
- What findings are needed for the diagnosis of POAG?
- Explain the result of the above mentioned investigations of the ocular exam?
- Enlist the Patient counselling points in this case?
Go to Case Study – 29 Answers
Case Study-30 (Galucoma)
The patient is a 51 year-old stay-at-home mother who presented to the ED with severe R brow, R cheek and R eye pain/pressure that started 2-3 hrs prior. She also noticed blurry vision from that eye and rainbow-colored halos around lights around the same time.
Accompanying symptoms include acute nausea. She has vomited twice since feeling eye pain. Denies prior episodes. Denies flashes, floaters or diplopia. There is mild redness in the R eye.
Hx myopia OU No prior eye surgeries, trauma, amblyopia or strabismus
Degenerative disc disease – lower back
Father: chronic angle-closure glaucoma. No FHx of macular degeneration or other blinding diseases.
30 pack/year smoking history Drinks alcohol on occasion No illicit drug use
Medications:
Multivitamins Vicodin prn (uses few days/month for back pain)
Denies recent illnesses, new medications, CNS, lungs, GI, skin, joint problems except for above.
Ocular Exam
Visual Acuity (cc): OD: 20/70 OS: 20/20 IOP (tonoapplantation): OD: 62 mmHg OS: 11 mmHg Pupils: OD: pupil mid dilated, sluggish to respond to light. OS: pupil round and reactive to light No obvious APD Extraocular Movements: Full OU No nystagmus Confrontational Visual Fields: Full to finger counting OU External: Normal, both sides
Lids and Lashes: Normal OU Conjunctiva/Sclera: Mild diffused injected conjunctiva OD, Normal OS Cornea: Hazy cornea OD, Normal OS Anterior Chamber: Shallow anterior chamber 360 OD – hazy view, Deep and quiet OS Iris: Mid dilated iris OD, Normal OS Lens: Trace nuclear sclerosis OU Anterior Vitreous: Clear OU
OD: Dilation not performed, examination through undilated pupil showed hazy view, CDR 0.5 with sharp optic disc margins; flat macula OS: Dilation not performed, examination through undilated pupil showed clear media, CDR 0.4 with sharp optic disc margins; flat macula
Gonioscopy: Performed with Abraham 4 mirrored lens, shallow angle and no view of the angle structures 360 degrees OD, shallow angle with view of the trabecular meshwork 360 degrees OS without synechiae, mild pigmentation 360 degrees OS
1. What is the Diagnosis in this case? 2. What is the mechanism of angle closure in an episode of acute angle closure glaucoma resulting from a pupillary block? 3. Mention in brief the surgical options for the disease?
Go to Case Study – 30 Answers
Case Study - 31 (Conjunctivitis)
The patient is an 31 year-old male who reports a 4-day history of irritation and itching, first in the L eye followed by the R eye one day later. Both eyes have also had a mild yellow discharge and mattering of the eyelids making it difficult to open the eyes in the morning. There is minimal eye redness but no foreign body sensation, flashes, floaters, decreased vision or diplopia. Not using any drops. No environmental exposures to the eyes.
No history of eye trauma, surgery, amblyopia or strabismus. No history of contact lens use.
Born at term without complications
No history of glaucoma, macular degeneration or other blinding diseases
No smokers at home
Exposure to the common cold (neighbor friend). No history of environmental allergies, recent cold, CNS, heart, lung, GI, skin or joint problems.
OD: 17 mmHg
OS: 14 mmHg
Equal, round and reactive OU, no APD
Normal-appearing orbital structures; no redness or swelling either eye
Lids and Lashes: Crusted dry flaky material on eyelashes OU, no follicles in inferior or superior fornix OU. No foreign body in fornices OU
Conjunctiva/Sclera Mild conjunctival injection OU, no chemosis
Cornea Clear OU, no infiltrates
Anterior Chamber Deep and quiet OU
Iris Normal OU
Lens Normal OU
Anterior Vitreous Clear OU
Dilated Fundus Examination :
OD Clear view, CDR 0.2 with sharp optic disc margins, flat macula with normal foveal light reflex, normal vessels and peripheral retina
OS Clear view, CDR 0.2 with sharp optic disc margins, flat macula with normal foveal light reflex, normal vessels and peripheral retina
No preauricular or submandibular lymph node enlargement
- What are the patient counselling points in these case?
- What is not a typical exam finding of conjunctivitis?
Go to Case Study-31 Answers
Case Study - 32 (Conjunctivitis)
History: A 35 year old female presented with complaints of sticky eyelids, watery and green ocular discharge, redness, soreness and slightly blurred vision in both eyes.
The symptoms started 2 weeks ago; the right eye was affected first.
Initially prescribed with Chloramphenicol (0.5%), no improvement was reported.
Chloramphenicol was replaced with Tobramycin, improvement was noticed only on 1 st day.
· Ocular swab taken for PCR and was advised to stop tobramycin.
Again, on the visit, she reported that the left eye now felt worse and noticed an increase in green discharge, however a decrease in redness since the drop discontinuation.
Past medical history : A metal foreign body removal from the right eye – 10years ago.
She had flu, 3 weeks ago but is in good health now (was not atopic and she was not taking any medications.)
Vision: OD : 6/6 OS : 6/5
Slit lamp examination:
OD: Mild conjunctival injection. Mild follicular change of the inferior palpebral conjunctiva. No corneal surface involvement. No anterior chamber inflammation.
OS: 360 degree conjunctival injection grade 3. Multiple white nodules at the limbus. Mild follicular change of the inferior palpebral conjunctiva. No anterior chamber inflammation.
Other Investigation:
PCR test : negative for Adenovirus, Varicella-Zoster virus, Herpes Simplex virus and Chlamydia trachomatis.
Provisional Diagnosis: Bacterial Conjunctivitis
For left eye:
Instill one drop of ofloxacin q2h
* reduce the dosage to “qid” the next day if the condition improves.
For right eye:
Ofloxacin qid
Revisit after 1 week.
- What are the possible differential diagnosis in this case?
- What is the role of Ofloxacin in this Patient’s case?
- Why Tobramycin wasn’t readvised after the PCR result, is there any evidence suggestive for the change?
Go to Case Study -32 Answers
Case Study - 33 ( Pediatrics)
Leanne is a 6-year-old girl whose teachers have suggested that her parents take to her GP. They have noticed that she seems to have problems listening and to be daydreaming a lot in class. The GP asks whether her parents have also seen her daydream. Her mother has, but has not thought much about it. However, more recently, it seems to have been happening more frequently. On direct questioning by the GP, Leanne’s mother thinks that these daydreams or ‘trances’ as she calls them sometimes occur when Leanne is in the middle of doing or saying something, and they interrupt her activity. Leanne’s birth and early medical history, including her development, have been normal. There was a history of epilepsy on her father’s side of the family. Her younger brother and older sister are well.
1.What should Leanne’s GP consider as a possible diagnosis?
2. What further investigations should the paediatrician or paediatric neurologist Request, and what considerations should be taken into account?
3. What should the discussion around medication include, and what medications may be Prescribed?
Go to Case Study- 33 Answers

Answers for Case Studies for Pharm.D / PharmD students:
Case study-1 answers.
- According to AHA guidelines the target BP goal for hypertensive patients with CAD is <130/80 mmHg.
- Beta blockers, ACE inhibitors, ARB’s, thiazide diuretics, and calcium channel blockers (CCB). ( Beta – blocker , first line agent to treat HTN in patients with Angina).
Explanation : stepwise Go to CASE STUDY 1
Step 1: In HTN patients with angina as comorbidity Beta blockers are the first line agents. Here metoprolol ( beta- blocker is already prescribed). Check whether target BP goal is achieved or not. Here target BP goal is not achieved in this patient (noted as 166/93 mmHg on his today’s visit to clinic). Follow step-2 if target Bp goal is not achieved. Step-2 : Prescribe the maximum dose of metoprolol (100 mg twice daily). In this case already maximum dose is prescribed. Follow step 3 if target BP goal is not achieved. Step-3 : Add another anti-hypertensive agent from ACEI’s / ARB’s / Thiazide diuretics/ CCB’s to the Beta -blocker. Note : Here the patient is tolerant to METOPROLOL , however if the patient is intolerant to METOPROLOL ,Consider ACEi/ARB as first line agent and add CCB/thiazide as adjuvant.
Go to CASE STUDY 1
Case Study-2 Answers
Poor diet control, non-compliance to medication and obesity were considered to be the main reasons for poorly controlled hypertension and diabetes in Mr. MK
- HbA1C target value should be less than 6.5%
- Target value for BP should be 130/80 mm Hg.
- Achieving these targets found to be beneficial in decreasing the Cardiovascular morbidities and prevention or delay of CKD progression.
3.Ans) FOR HTN: Go to Case Study 2.
For diabetic patients whose blood pressure levels are ≥160/100 start with two anti-hypertensive agents. Diabetic and hypertensive Patients with albuminuria consider ACEI /ARB as first line agent and add adjunctive drug from classes calcium channel blockers or Diuretic. Eg : Telmisartan (ARB) + Furosemide (diuretic)
FOR DIABETES: Metformin is the preferred initial pharmacologic agent for the treatment of type 2 diabetes. Once initiated, metformin should be continued as long as it is tolerated and not contraindicated; If the A1c levels are not achieved within the target levels, consider other class of agents to metformin. LIRAGLUTIDE (GLP1 AGONISTS) has the benefit of decreasing both the HBA1c values as well as body weight. So replacing GLICLAZIDE with LIRAGLUTIDE increases the effectiveness of treatment. Rx : Metformin + LIRAGLUTIDE .
4. Ans) DRUG INTERACTION:
AMLODIPINE+METFORMIN – Amlodipine decreases effect of Metformin by pharmacodynamic antagonism. Management – Monitor closely after withdrawal of Amlodipine whether the blood sugar levels are decreased or any hypoglycemic condition is observed.
5.Ans) Patient counselling:
- Counsel the patient regarding importance of medication adherence.
- Suggest to maintain regular exercise or at least do walking for 1 hour as it will be more beneficial for the weight loss.
- Follow DASH diet to control HTN and reduce cardiovascular comorbidities.
- Reduce intake of saturated fat and trans-fat; increase of dietary n-3 fatty acids, viscous fiber, and plant stanols/sterols.
- Counsel the patient for regular checkup of A1c levels at least four times yearly.
Considerations: Go to Case Study 2.
- LIRAGLUTIDE -1.2MG SC as GLP 1 agonists mainly decrease the HbA1c value (~0.8% -1.6%)and it also decreases body weight to (1-3kgs). Monitor closely while using liraglutide as it is contraindicated in medullary thyroid carcinoma and Monitor the calcitonin levels .
- Metformin is contraindicated in patients with an eGFR ,30 mL/min/1.73 m2;
- eGFR should be monitored while taking metformin;
- The benefits and risks of continuing treatment should be reassessed when eGFR falls ,45 mL/min/1.73 m2;
- Metformin should not be initiated for patients with an eGFR ,45 mL/min/1.73 m2; and
- Metformin should be temporarily discontinued at the time of or before iodinated contrast imaging procedures in patients with eGFR 30 60 mL/min/1.73m2
Within these constraints, metformin should be considered the first-line treatment for all patients with type 2 diabetes, including those with CKD.
- If cost of medication was the reason for non-compliance replace Liraglutide with insulin therapy basal insulin with lowest acquisition cost. If replaced with insulin there must be strict diet control and exercise that helps the patient to loose weight.
- If Furosemide was given as an adjunctive drug advice the patient to observe closely for hypoglycemia, if needed switch to other anti-hypertensive agent.
Go to Case Study 2. | For more CASE STUDIES .
Case Study-5 Answers
1. what is the treatment goal and strategy for this case.
Ans : Goals of therapy of CSA are :
- Amelioration of anginal symptoms and improved angina-free exertion capability
- Prevention or reduction of subsequent acute MI, UA, or ISD and there by increasing quality of life.
1. Vasodilating – Beta-blockers as initial therapy:
Vaso-dilating beta blockers like Carvedilol and nebivolol can be used as first line agents, as they don’t have negative metabolic effects as compared to non-vasodilating beta-blockers like metoprolol.
Usually non-vasodilating beta-blockers like metoprolol, propranolol etc., have high risk for new onset diabetes or masking of hypoglycemia.
{ Usually beta-blockers are preferred as initial therapy in the absence of any contraindications or chances for severe side effects.
In case of contraindications to beta blockers → use long acting calcium channel blockers as initial therapy. }
2. Lipid lowering agents :
Lipid lowering agents like atorvastatin can be used as prophylactic therapy to prevent or minimizing risk of CAD.
3. Anti-platelet agents :
Adding Aspirin to the treatment shows a good evidence of Preventing MI and Death and Reducing Symptoms.
2. Suggest the best follow-up for this case.
Ans: Monitoring of Symptoms and Antianginal Therapy:
During the first year of therapy, evaluations every 4 to 6 months are recommended. After the first year of therapy, annual evaluations are recommended if the patient is stable and reliable enough to call or make an appointment when anginal symptoms become worse or other symptoms occur.
- Has the patient decreased the level of physical activity since the last visit?
- Have the patient’s anginal symptoms increased in frequency and become more severe since the last visit? If the symptoms have worsened or the patient has decreased physical activity to avoid precipitating angina, then he or she should be evaluated and treated according to either the unstable angina or chronic stable angina guidelines, as appropriate.
- How well is the patient tolerating therapy?
- How successful has the patient been in reducing modifiable risk factors and improving knowledge about ischemic heart disease?
- Has the patient developed any new comorbid illnesses or has the severity or treatment of known comorbid illnesses worsened the patient’s angina.
3.What are the conditions which worsens the symptoms of angina (in general)?
- Tobacco use,
- high blood pressure,
- high cholesterol,
Go to Case 5 | Explore more Case Studies | Go to guidelines
Case Study-6 Answers
1 . what information and counselling points would you include.
Ans: Mr SW has already been taking steps to address his unhealthy lifestyle and reduce his cardiovascular risk.
- Furthermore, he can be counselled for risk factors for cardiovascular disease that are commonly distinguished as modifiable and non-modifiable. Modifiable risk factors are those that can be controlled, treated or modified. These include smoking, diet (especially cholesterol and lipids), weight and obesity, physical exercise, blood sugar levels and hypertension .
Non-modifiable risk factors are those that cannot be changed, such as age, gender, ethnicity and family history.
- However, Mr SW should be counselled about how primary and secondary prevention helps in delaying the progression of disease by early detection of any further onset of disease .
- He should be given proper information about the side effects (like muscle spasm, headache, flushing, breathlessness on physical work) & use, storage of medications; and how the benefits of treatment are much more as compared to side effects. So that, Mr SW will understand the rational use of medication and develop better medication adherence.
- Also, if Mr SW founds any side effects that he is concerned about ( like impotence in previous ), rather quitting the drug by himself, consult his physician for the same. Drugs can be changed/further treatment option will be suggested based on the situation, the physician finds.
2. How is stable Angina managed ? Go to CASE STUDY-6
Ans: Managing stable Angina:
Treatments can be divided into those that reduce the risk of future cardiovascular events, thereby reducing mortality ( secondary prevention ) and those that prevent symptoms ( which can be further subdivided into short- and long-term relief ).
For Secondary Prevention:
Aspirin 75 mg daily (reduction in non-fatal MI & vascular events)
Simvastatin 40 mg daily (starting dose)
- Alternative / lower dose can be used if contraindication / interactions found.
- If total cholesterol <4 mmol/L or LDL <2 mmol/L not achieved at initial dose, titration of simvastatin or alternative should be used.
For Short-Acting relief:
GTN sublingually (rapid onset of action: within 1-5 min) Go to CASE STUDY-6
- Minimizes the discomfort
- Choice of dosage form should be discussed with patient
- Pt should be counselled for side effects, use & storage
- Can cause difficulties in Pt with significant arthritis or reduced hand dexterity
For Long-Acting symptom control:
- 1 st line treatment should be with either beta-blocker or CCBs.
- If symptoms are not controlled, the next step is to swap or add the other (usually avoiding the combination of beta – blocker & verapamil ).
- Long-acting nitrate
- Response to treatment should be reviewed 2-4 weeks after starting or changing drug treatment. Go to CASE STUDY-6
3. What options are there, if Mr. SW experiences further symptoms despite the use of amlodipine?
Ans : If further symptoms are experienced, i.e., symptoms not adequately
controlled with medication, the relative merits and risks of coronary artery bypass grafts (CABG) versus percutaneous coronary intervention to alleviate symptoms should be discussed. A multidisciplinary discussion should take place when the coronary artery disease is more complex.
REFERENCES:
1. European Society of Cardiology (2006). Guidelines on the management of stable Angina Pectoris.
2. national institute for health and clinical excellence (2011). management of stable angina. clinical guideline 126. london.
Go to CASE STUDY-6
Explore more Case Study | Guidelines | Home
Case Study-7 Answers
Ans. the fourth universal definition of mi (udmi) was released in 2018. according to the udmi, mi is defined as myocardial injury in the clinical setting of myocardial ischemia. there are two components:.
- Myocardial injury which is defined as raise of troponins above the 99th percentile
- Clinical Setting of myocardial ischemia-symptoms and signs of myocardial ischemia, ECG changes with new ischemic changes or pathological Q waves, imaging evidence like loss of viability, regional wall motion abnormality (RWMA), thrombus in angiography, evidence of thrombus in autopsy, sudden cardiac death.
2. What are the classical ECG criteria for diagnosing STEMI ? Go to Case Study-7
Ans. There should be two contiguous leads with ST elevation (measured at J point).
>2.5 mm for men <40 years
>2 mm for men >40 years in leads V2, V3
>1.5 mm for women.
And/or >1 mm in other leads in absence of LVH, LBBB.
For posterior MI, in leads v7–v9, 0.5 mm is itself enough to diagnose posterior wall MI in inferior MI.

3. What are the different types of MI ? Go to Case Study-7
Ans. UDMI classifies MI in five types:
a) Type 1 MI due to thrombosis of an atherosclerotic plaque
b) Type 2 MI due to myocardial oxygen supply demand imbalance in the context of another acute illness.
c) Type 3 MI presenting as sudden death
d) Type 4 post-percutaneous coronary intervention (PCI)
e) Type 5 postcoronary artery bypass grafting.
4. Justify the treatment given to this patient. Go to Case Study-7
- Aspirin – ISIS 2 was the landmark trial in 1988 after which aspirin was considered as mainstay in ACS patients
- DAPT – benefit of DAPT in ACS setting and post-PCI setting were shown in CURE and PCI CURE trials, where they used Clopidogrel as the p2y12 inhibitor of choice. There was a significant reduction in composite primary endpoint of cardiovascular (CVS) mortality, non-fatal MI and stroke (9.3vs. 11.4%) with number needed to treat (NNT=48)
Ticagrelor was compared to clopidogrel in PLATO trial. Addition of ticagrelor to aspirin was able to further reduce composite primary endpoint of cardiovascular mortality, non-fatal MI, and stroke from 11.7% to 9.8% (P < 0.001) with an insignificant increase in major bleeding (11.6% vs. 11.2%)
- In this case BMI of the patient was found to be 29.2 which is overweight. This puts patient at high risk for increased LDL, Cardiovascular comorbidities etc.
Statins have a huge body of evidence both for early initiation and intensive treatment strategy mainly from meta-analysis data by cholesterol treatment trialist. Most of the trials utilized atorvastatin in the STEMI setting. With high intensity statin defined as the atorvastatin 40-80 mg with an ability to decrease LDL cholesterol by >50
- Beta blockers found to have robust benefit in people with MI and post MI reduced LVEF.
- ACE inhibitor trials are the SAVE, AIRE and TRACE trials which demonstrated mortality benefit of starting ACE inhibitors within first 24 h. AIRE trial used the drug ramipril.
# Discontinue Lasix + Spironolactone :
Early initiation of Lasix and Spironolactone was not was not found to beneficial in Acute Myocardial infarction. ( As MI is one of the main cause for reduced ejection fraction or systolic heart failure consider using Mineralocorticoid receptor antagonists when reduced ejection fraction is less than 40% ).
(These can be used if the patient is having post-MI heart failure or LV dysfunction or Ejection fraction < 40% or diabetic with symptoms of heart failure.)
5. Determine the duration of DAPT In this patient ? Go to Case Study-7
Ans. In this case patient has had an acute coronary event (STEMI). He is a 56-year-old male, with only smoking as risk factor. He does not have any features of high bleeding risk. He is a candidate with a Low Bleeding risk with a moderate ischemic risk. PRECISE DAPT SCORE in this patient is <25. Hence, strategy for DAPT duration will be till 12 months with Aspirin 75 mg dose and ticagrelor 90 mg BD dose. Reassess the patient at the end of 12 months , with DAPT score. If the patient is found to have high ischemic risk features, prefer continuing the patient on ticagrelor 60 mg BD till 3 years’ duration if cost is not an issue for greater benefit .
( Refer : high bleeding risk criteria and Precise DAPT scoring)
Go to Case Study-7
Explore more Clinical Case Studies | Guidelines | Home
Case Study-8 Answers
1. is the diagnosis & treatment given to mr tr justified explain. case 8 .
Ans: The diagnosis and treatment given to patient is appropriate .
Justification:
Diagnosis : The most likely diagnosis was confirmed by angiogram, which identified thrombosis and stenosis in the coronary arteries obtuse marginal, LAD& RCA, requiring deployment of drug-eluting stents. Also, Echocardiogram shows normal LV function.
Treatment :
- Drug eluting stents(DES) – for stenosed coronary artery to restore blood flow.
- Dual antiplatelet therapy (Aspirin+Clopidogrel) – required as DES is inserted, until re-endothelisation occurs. However, treatment courses of 2 nd antiplatelet agent(clopidogrel) should be kept to a minimum(1-3 months or 1 year)
- Beta blocker & ACEI started with minimum required dose which is required.
- High-intensity statins are recommended after an acute coronary syndrome.
- GTN helps in venodilatation and arterial dilatation & reduction of cardiac ischaemia.
***Major and intermediate drugs interactions are there. However, drugs dosage is already maintained minimum as recommended , if used together .
2. Is there a need of counselling? Case 8
Ans: Approx. 50% or more cardiovascular patients do not take their medications as intended. Poor adherence can lead to increase in recurrence, hospitalization, mortality. So, counselling is required to increase positive adherence.
Pt should be informed of drugs effects and side effects and the benefits of medication adherence.
Also, he should be counselled for lifestyle modification.
The patient should be encouraged to report any adverse effects from the drugs.
**He may have to take Aspirin lifelong to prevent secondary cardiovascular events.
Case 8 | Clinical Case Studies | Guidelines | Home
Case Study-9 Answers
- As the patient is at High risk with known CVD, the target goal for LDL-C would be < 70 mg/dl.
- High-intensity statins (Atorvastatin 40-80 mg , Rosuvastatin 20 – 40 mg ) would be choice of treatment in this patient.
- If on maximal statin & LDL-C ≥70 mg/dL (≥1.8 mmol/L), add ezetimibe.
- Using non-statin therapy like niacin would be helpful in the patients who are intolerant to statins. (prior to withdrawing statin therapy check whether the patient is having true intolerance to statin or not).
References :
- https://www.acc.org/~/media/Non-Clinical/Files-PDFs-Excel-MS-Word-etc/Guidelines/2018/Guidelines-Made-Simple-Tool-2018-Cholesterol.pdf
- https://www.lipid.org/sites/default/files/6-_lipid_u-_guidelines-_jones.pdf
Case 9 | Clinical Case Studies | Guidelines | Home
Case Study-10 Answers
1. what is the metabolic abnormality present case 10.
Ans: The obvious abnormal investigation is a very high serum cholesterol with high
LDL and low HDL levels. He has many clinical features to go with the high cholesterol and premature vascular disease. The patient has familial hypercholesterolaemia . He has presented with premature coronary artery disease. His absent pedal pulses suggest peripheral vascular disease.
** The metabolic defect is a result of a reduced number of high-affinity cell-surface LDL receptors. This leads to increased LDL levels. Increased uptake of LDL by macrophage scavenger receptors leads to increased oxidized LDL, which is particularly atherogenic. Triglyceride and VLDL levels are normal or mildly elevated. HDL levels are low. The other major causes of hypercholesterolaemia are familial combined hyperlipidaemia and polygenic hypercholesterolaemia. Familial combined hyperlipidaemia differs from familial hypercholesterolaemia by patients having raised triglycerides. Patients with polygenic hypercholesterolaemia have a similar lipid profile to familial hypercholesterolaemia but they do not develop xanthomata.
2. Discuss the Patient counselling for this case? Case 10
Ans: The patient is at extremely high risk for further vascular events and especially
occlusion of his coronary artery bypass grafts. His risk depends on the combination of his risk factors, and all of these need attentions.
He should be counselled about following points:
- To stop smoking,
- Reduce his alcohol intake
- Take more exercise and
- Eat a strict low-cholesterol diet.
- He should be suggested that diet alone will not control this level of cholesterol. So, a proper adherence with the pharmacological treatment with a statin or combined treatment for this level of hyperlipidaemia, is needed.
- Importance of periodic lab check-ups.
- His children should have their lipid profile measured so that they can be treated to prevent premature coronary artery disease.
Case 10 | Clinical Case Studies | Guidelines | Home
Case Study-11 Answers
1. what would be the possible differential diagnosis case 11 .
Ans: The differential diagnosis of a pediatric patient who presents with a narrow complex tachycardia includes atrioventricular reentrant tachycardia (AVRT ), AV nodal reentrant tachycardia ( AVNRT ), sinus tachycardia , atrial flutter , atrial fibrillation , junctional ectopic tachycardia , atrial ectopic tachycardia , and multifocal atrial tachycardia/chaotic atrial tachycardia .
Provisional Diagnosis: SVT ( supraventricular tachycardia)
2. What is the treatment goal and strategy for this case? Case 11
Ans: Treatment goals include:
- Reducing the symptoms and stabilizing the patient,
- Terminating the SVT and
- Stablishing a mechanism to prevent any cardiac emergency condition.
Treatment Strategy:
If the patient is clinically stable , vagal maneuvers may be initially attempted to convert the tachycardia. Such vagal maneuvers may include bearing down (as though having a bowel movement (i.e., Valsalva maneuver)), blowing in a straw or inducing the diving reflex using an ice bag to the face for infants. Other vagal maneuvers such as eyeball pressure and unilateral carotid massage are harmful and should not be performed.
If the patient appears clinically unstable , urgent electrical cardioversion is indicated using 0.5-1 J/kg. If an intravenous line is already in place (antecubital preferred over a hand vein), an IV bolus of 0.1-0.2 mg/kg adenosine may be given prior to cardioversion. Adenosine causes a transient AV block and sinus bradycardia, thus interrupting the reentrant circuit involving the AV node and accessory pathway. It must be remembered that this medication is metabolized by the red blood cells and has a very short half-life (approximately 5 seconds), therefore it should be administered via bolus injection followed by an immediate bolus of saline (rapid push and flush). A 12-lead ECG should be obtained before and after conversion, if possible, and a rhythm strip should be continuously run during attempted conversion. External pacing equipment should be available since some patients go into sinus arrest following administration of adenosine .
If adenosine initially fails to convert the SVT , but the patient is hemodynamically stable, they may be started on a medication such as propranolol, digoxin or verapamil (digoxin should be avoided in WPW, verapamil should be avoided in infants) followed by a repeat dose of adenosine.
3. What medicine used to treat Supraventricular tachycardia(SVT) is contraindicated specifically in Wolff-Parkinson-White syndrome(WPW)? Case 11
Ans: Digoxin .
** In the setting of WPW, digoxin can facilitate impulse conduction via accessory pathway and increase risk for ventricular arrhythmias (i.e., ventricular fibrillation).
Case 11 | Clinical case Studies | Guidelines | Home
Case Study-12 Answers
1. acute management of af with hemodynamic instability case 12.
Given his presentation of AF with hypotension and pulmonary edema, considering AF with hemodynamic instability, sinus rhythm must be rapidly restored by synchronised electrical cardioversion. After achieving normal sinus rhythm, consider anti-coagulation as the patient is at risk for thromboembolism. Anticoagulation must be initiated and should be continued for at least 4 weeks.
(The decision to continue anticoagulation beyond the initial 4 weeks is based on the long-term risk for thromboembolism associated with nonvalvular AF. This risk is estimated by determining his CHA 2 DS 2 -VASc score, which is calculated by assigning points for congestive heart failure (1 point), hypertension (1 point), age (1 point for 65-74 years and 2 points for >75), diabetes (1 point), stroke, TIA, or thromboembolism (2 points), vascular disease defined as history of myocardial infarction, peripheral vascular disease, or aortic atherosclerosis (1 point), and female gender (1 point) )
2. CHA 2 DS 2 -VASc score (estimating risk of stroke & thromboembolism): 3 points Case 12
Stroke risk was 3.2% per year in >90000 patients ( the Swedish atrial fibrillation cohort study) and 4.6%risk of stroke/TIA/systemic embolism.
HAS-BLED score ( for estimating major bleeding risk) : 2 points
Risk was 4.1% in one validation study (Lip 2011) and 1.88 bleeds per 100 patient-years in another validation study (Pisters 2010).Anticoagulation can be considered, however patient does have moderate risk for major bleeding (~2/100 patient-years).
Case 12 | Clinical Case Studies | Guidelines | Home
Case Study-13 Answers
1. based on current evidence, which of the following would be the most appropriate recommendation regarding his asthma medication regimen case study-13.
A. Maintain current medication regimen; no adjustment is indicated
B. Discontinue the inhaled corticosteroid; maintain on an inhaled beta-agonist as needed
C. Decrease the inhaled corticosteroid to 1 puff daily
D. Discontinue the inhaled corticosteroid; start a leukotriene modifier at bedtime
E. Discontinue the inhaled corticosteroid; start low-dose inhaled corticosteroid/long-acting beta-agonist, 1 inhalation at bedtime
ANS: correct answer = option E
EXPLANATION : The goal of asthma therapy is to minimize risk and maintain asthma control with the least amount of medication (1). In patients with mild persistent asthma, recent studies have demonstrated several options for “step-down therapy.” The American Lung Association Asthma Clinical Research Centers network study found that patients who stepped down from twice daily low-dose fluticasone to once daily combination therapy with fluticasone/salmeterol had equivalent asthma control scores, FEV 1 , and frequency of exacerbations compared with continued therapy with twice daily fluticasone (2). Once-daily montelukast demonstrated a slightly higher treatment failure compared with either of the regimens containing inhaled steroids. Despite the slight increase in treatment failure with montelukast, each of the treatment groups had equivalent symptom-free days and rates of clinically significant asthma exacerbations. Thus, while either regimen would be appropriate, stepping down to once-daily combination therapy with fluticasone/salmeterol appears to be more beneficial.
Recent studies also suggest that those with mild persistent asthma taking inhaled corticosteroids in combination with either a long-acting beta-agonist or a short-acting beta-agonist when symptomatic, had no increase in adverse outcomes compared with those taking scheduled daily inhaled doses. Boushey et al. (3) compared patients with mild persistent asthma using twice-daily budesonide versus twice-daily zafirlukast verses placebo. All three groups used budesonide as-needed following a symptom-based action plan. The study found that in comparison with patients on a daily controller (budesonide or zafikulast), participants using only as-needed budesonide had no significant difference in morning peak expiratory flow, postbronchodilator FEV 1 , quality of life, or frequency of asthma exacerbations. Results of this study raise the possibility of treating mild persistent asthmatics with as-needed inhaled corticosteroids. More recently, Papi et al. (4) found as-needed use of an inhaler containing both beclomethasone and albuterol for symptom relief was associated with fewer exacerbations and higher morning peak flow readings than using an inhaler with albuterol alone. The morning peak flow readings in the as-needed combination beclomethasone/albuterol group was equivalent to those taking scheduled daily doses of beclomethasone alone, or scheduled daily doses of beclomethasone/albuterol combined. The combination of an inhaled steroid and a short-acting beta-agonist in a single inhaler is not currently available in the United States.
In the mild persistent asthmatic there is now strong evidence to support multiple treatment approaches which provide good asthma control. Matching the drug regimen with the patient’s preferences, lifestyle, comorbidities, and financial limitations will help ensure drug adherence and maintain asthma control.
2. Which of the following should be done routinely with each follow-up visit? Case Study-13
ANS: correct answer = option D
EXPLANATION: Assessing inhaler technique at each office visit allows the provider an opportunity to assess compliance, reinforce proper use, and identify motor or physical limitations affecting technique (8).
When studied, only approximately 25% of patients are able to properly demonstrate use of a meter dose inhaler when asked. The remaining 75% improved with specific instruction and practice which reinforces the need to incorporate proper inhaler use during the office visit (9,10). The use of a spacer significantly improves accuracy and dose delivery, particularly in patients with poor coordination skills (9,10).
Assessing patient adherence is best approached with a non-judgmental attitude. Adherence to inhaled corticosteroids is estimated at < 50% (11). Causes of nonadherence are multifactorial but may be improved by providing asthma education, encouraging self management through use of an asthma action plan, and facilitating open communication (11). Financial barriers often transcend all other efforts to improve adherence and must be taken into account when prescribing asthma therapy (11).
Methacholine challenge testing is useful to demonstrate airway hyperresponsiveness in those with normal spirometry and a suspicion of asthma, but is not recommended as a serial procedure. Biomarkers for inflammation such as eosinophils or nitric oxide are being investigated in clinical trials but currently have no indication in routine asthma care (1). Peak flow monitoring is useful for long-term home assessment of asthma control and medication response, but is not indicated for regular office assessment or diagnostic purposes (1).
3. What findings would suggest that the patient requires a step-up in asthma medication? Case Study-13
A. Two or more night time awakenings per month due to Asthma.
B. Two or more interruptions in daytime activities per month due to asthma
ANS: correct answer = option A
EXPLANATION: Inadequate asthma control and a need for step-up therapy is based on two or more daytime symptoms per week, two or more nighttime symptoms per month, interference with activities of daily living, use of short-acting beta-agonist > 2 days/week (excluding use for prevention of exercise-induced bronchospasm),or peak flow or FEV 1 <80% predicted/personal best (1).
Asthma symptoms should be assessed at each office visit to determine asthma control. Validated self-assessment tools such as the Asthma Control Test (ACT), Asthma Therapy Assessment Questionnaire (ATAQ), or Asthma Control Questionnaire (ACQ) can facilitate consistent measurement and documentation of asthma symptoms during office visits (1, 8). All asthmatics are at risk for a severe asthma attack regardless of their asthma classification; therefore, providers are encouraged to teach patients to recognize symptoms of inadequate asthma control and provide them with specific instructions for adjusting their medications or seeking medical care (1)
4. The patient was provided with an asthma action plan to follow at home. Which component of the asthma action plan is considered the most critical element for improving asthma outcomes? Case Study-13
ANS: correct answer = option D
EXPLANATION : All of the elements are important components of an asthma action plan. However, Gibson and Powell (5) found a 40% reduction in hospital admissions and a 20% reduction in emergency room visits when the plan contained personalized instructions regarding the medications to add, criteria for adding the medication, duration of use, and when to seek medical help when patients are symptomatic. An asthma action plan serves as a patient guide for early recognition and treatment of an exacerbation. Treatment guidelines may be based on symptoms, peak flow readings, or both. When peak flow readings are used, personal-best readings were consistently associated with improved health outcomes compared with percentage-predicted readings (5).
5. How often is spirometry testing recommended if the previous readings are normal and the patient’s asthma is well controlled? Case Study-13
EXPLANATION: Spirometry is a simple test that can be performed in-office and can be used to assist the provider in determining the degree of airway obstruction (1, 6). There are no widely accepted data correlating frequency of spirometry with clinical outcomes in asthmatics, thus one must rely on expert opinion and individual patient needs. Spirometry is recommended during the initial evaluation after treatment is initiated and the patient’s symptoms have stabilized during periods of progressive or prolonged loss of asthma control and at least every 1-2 years (1).
When spirometry is used to diagnose or confirm asthma, testing must include pre- and post-bronchodilator readings (1). A change in FEV 1 of >200 ml and ≥ 12% from the baseline measure following the administration of a short-acting bronchodilator is indicative of significant airway reversibility which has been shown to correlate with airway inflammation (7).
The Expert Panel (1) classifies asthma severity by FEV 1 , FEV 1 /FVC, short-acting beta-agonist use, or frequency of asthma symptoms. Parameters are measured at baseline with asthma severity determined by the worse parameter, e.g., daily symptoms with normal FEV 1 is classified as moderate persistent asthma. Correct identification of asthma severity guides the provider in choosing the appropriate type and amount of therapy
REFERENCES :
- Expert Panel Report 3 (EPR 3). Guidelines for the Diagnosis and Management of Asthma. Bethesda, Md: National Institutes of Health; 2007. NIH Publication No. 08-4051.
- The American Lung Association Asthma Clinical Research Centers. Randomized comparison of strategies for reducing treatment in mild persistent asthma. N Engl J Med 2007;356:2027-2039.
- Boushey HA, Sorkness CA, King TS, et al. Daily versus as-needed corticosteroids for mild persistent asthma. N Engl J Med 2005;352:1519-1528.
- Papi A, Giorgio GW, Maestrelli P, et al. Rescue use of beclomethasone and albuterol in a single inhaler for mild asthma. N Engl J Med 2007;356:2040-2052.
- Gibson PG, Powell H. Written action plans for asthma: an evidence-based review of the key components. Thorax 2007;59:94-99.
- Miller MR, Hankinson J, Brusasco V, et al. Series ATS/ERS Task Force: Standardization of lung function testing. Eur Respir J 2005;26:319-338.
- Pellegrino R, Viegi G, Brusasco V, et al. Interpretative strategies for lung function tests. N Engl J Med 2005;26:948-968.
- Global Initiative for Asthma. Pocket guide for asthma management and prevention. Bethesda, Md: National Institutes of Health; 2006.
- Giraud V, Roche N. Misuse of corticosteroid metered-dose inhaler is associated with decreased asthma stability. Eur Respir J 2002;19(2):246-251.
- Johnson DH, Robart P. Inhaler technique of outpatients in the home. Respir Care 2000;45(10):1182-1187.
- Elliott RA. Poor adherence to anti-inflammatory medication in asthma reasons, challenges, and strategies for improved disease management. Dis Manage Health Outcomes 2006;14(4):223-233.Top of Form
Case Study-14 Answers
1. what emergency measures are indicated case study- 14.
Ans: In this case patient demonstrates the destabilizing effects of a respiratory infection on asthma, and her mother’s comments demonstrate the common (and dangerous) phobia about overuse of bronchodilator or steroid inhalers. The patient has signs of imminent respiratory failure, including her refusal to lie down, her fear and her tachycardia, which cannot be attributed to her minimal treatment with albuterol.
#Critically important immediate steps are
- to administer high flow oxygen and to start albuterol by nebulisation.
- Adding ipratropium to the nebulized solution is recommended.
- A corticosteroid (0.5 – 1.0 mg/kg of methylprednisolone) should be administered intravenously.
#Alert the intensive care unit, because a patient with severe bronchospasm who tires can slip into respiratory failure quickly, and intubation can be difficult.
2. How should her long-term management be altered? Case Study- 14
Ans: Presuming this patient recovers, she needs adjustments to her therapy before discharge. The strongest predictor of severe attacks of asthma is their occurrence in the past. Thus, this patient therapy needs to be stepped up to a higher level, like a high dose inhaled corticosteroid in combination with a long acting beta agonist. Both the patient and her parents need instructions on the importance of regular adherence to therapy, with reassurance that it can be stepped down to a lower dose of inhaled corticosteroid( although still in combination with long acting beta agonist) once her condition stabilizes.
They also need instruction on an action plan for managing severe symptoms. This can be as simple as advising that if the patient has a severe, frightening attack, she can take up to four puffs of albuterol every 15 minutes, but if the first treatment doesn’t bring significant relief, she should take next four puffs while on her way to an emergency department or urgent care clinic.
She should also be given a prescription for prednisone, with instructions to take 40-60 mg orally for severe attacks, but not to wait for it to take effect if she remains severely short of breath even after albuterol inhalations.
# Asthma is a chronic disease, and a good care requires close follow up and creation of a provider-patient partnership for optimal management. If she has had several previous exacerbations, she should be a candidate considered for monoclonal anti-IgE antibody therapy with omalizumab, which effectively reduces the rate of asthma exacerbations _ even those associated with viral respiratory infection.
Reference : Text book Bertram G. katzung Basic and clinical pharmacology 14 th edition page number 365.
Go to Case Study- 14
For more Case Studies | Guidelines
All subject, PharmD books in pdf free download
Case Study-15 Answers
1. what clinical features and risk factors of copd does glenda exhibit what grade of severity does glenda’s copd fall into case study -15.
Ans: Glenda presents with a clinical scenario suggestive of COPD based on her age, smoking history, weight, frequent chest infections and gradual worsening of respiratory symptoms – breathlessness on exertion, a reduction in exercise tolerance, chronic cough and regular sputum production. Working in a fabric factory is also one of the identified occupational risk factors for COPD. Glenda is considered to have moderate COPD based on her spirometry results and breathlessness score.
(refer NICE classification of severity of airflow obstruction)
2. What initial treatment would you recommend for glenda? Case Study -15
Ans: Start a short acting beta agonist such as salbutamol or a short acting muscarinic antagonist, such as ipratropium bromide, to alleviate symptoms as required. Short acting bronchodilators should be used as needed; their onset of action ranges from approximately five minutes (beta2 agonists) to 30 minutes (muscarinic antagonists) and effects lasts for between 3 and 6 hours.
Refer: NICE clinical guideline for COPD
3. Glenda continues to report that her breathlessness is getting worse. Her medical research council dyspnea score is now four and in the last few days she has been producing more sputum than usual. Her sputum has turned a yellow green colour. What does these changes indicate & what treatment would you recommend? Case Study -15
Ans: Glenda’s symptoms suggest that she is experiencing exacerbations of COPD. She must be prescribed an antibiotic for 5 days at a therapeutic dose with Oral prednisolone 30 mg every morning for 7-14 days.
(Systemic corticosteroids are beneficial in the management of exacerbations of COPD. They shorten recovery time and improving lung function (FEV10 and hypoxemia (PaO2). Antibiotics should be used to treat exacerbations of COPD associated with a history of more purulent sputum. Initial empirical treatment should be amoxicillin, doxycycline or clarithromycin depending on a local resistance pattern.
Go to Case Study -15
Explore more Case Studies | Guidelines
Case Study-16 Answers
1. how the sign, symptoms & pathophysiology of copd, relates to the patient case study-16.
Ans: Clinical signs and symptoms of COPD, the pathophysiology and how this relates to the patient.
| Airflow obstruction, due to airway and parenchymal damage as a result of chronic inflammation that is progressive, not fully reversible. | Shortness of breath | |
| Due to increased hydrogen ion concentrations and possible increased metabolic rate stimulating the respiratory centre. | RR 20 per min | |
| Airway narrowing, mucosal damage, oedema of airway and increased sputum production increases the ventilation/ perfusion mismatch. | PCO2 9.672 kPa | |
| The duration of expiration is insufficient to allow the lungs to deflate (due to airway resistance or increased breathing rate). | Lungs hyperinflated |
2. Comment on the current drug therapy and describe the role of O2 in this patient. Case Study-16
| 10 mg od | Need to review the duration and need. Will need bisphosphonate for bone protection as osteoporotic | |
| 500 micrograms BD | Check which device? Accuhaler or Diskhaler. Patient not taking a long acting beta agonist, so why is she on an inhaled corticosteroid? | |
| 75 mg od | NICE guidelines post MI | |
| 1 mg od | Loop diuretic, why? BP is low, what evidence of heart failure is there? | |
| 2 qds | Salbutamol 2.5 mg, ipratropium 500 micrograms in 2.5 mls. Is there a need for regular short acting beta2-agonist? Change to long acting. Why use nebulisers? | |
| 5 mg od | Low dose for heart failure, or is it for high BP, but patient has a low BP!!! On admission. So it should be changed to other antihypertensives. | |
| 200 mg bd | Theophylline normally used after a trial of short and long-acting bronchodilators. Needs plasma levels monitored. Increased risk of low potassium when given with prednisolone and bumetanide. | |
| 2 tablets nocte | Review the patient’s intake and need for laxatives. | |
| 5 mg od | INR will need to be checked, 3–6 months duration. Care with drug interactions, anticoagulant effect may be affected by prednisolone, and aspirin. Patients Hb is already at the lower end of normal. | |
| 7.5 mg nocte | Normally only used for 4 weeks, as a hypnotic. | |
| 50 mg prn | Need to change to different pain control as high risk of bleeding when on warfarin and aspirin. Must not be taken as required. | |
| 2 L nasal specs | Nasal specs: difficult to predict the amount of oxygen inspired Need to investigate LTOT for home use. |
Role of oxygen:
As this patient has a PaO2 of less than 7.3 kPa and oxygen saturation of arterial blood of less than 90%, she is eligible for Long-Term Oxygen Therapy (LTOT). She will need to use oxygen at least 15 hours a day and needs to be counselled on the importance of smoking cessation. Ambulatory and short-burst oxygen therapy should also be considered, as per NICE guidelines (NICE, 2004).
3. What are the social issues in treating this patient at home? Case Study-16
Ans: Patients may be anxious and refuse such support. The cultural and social setting of the patient needs to be taken into account. As patients lose their mobility and increase dependence on others for help with day-to-day living, anxiety increases. Patients can become hesitant to seek help because of the perception that their condition was self-inflicted. Poor populations tend to have a higher risk of developing COPD, other factors include poor nutrition, crowding, exposure to pollutants, poor access to healthcare and early respiratory infections. Some evidence suggests women are more susceptible to COPD development than men. A multidisciplinary team should be involved in the support of the patient at home. Additional use can be made of nebulisers, compressors, oxygen, visiting respiratory nurses and increased social service input. The patient remains under care of the hospital but the GP is made aware of the extra support. Health status is better in home-treated patients. COPD is linked with other co-morbid conditions. Patients are more likely to have ischaemic heart disease, pneumonia and diabetes, making treatment more complicated and requiring a holistic approach to care.
This patient demonstrates five co-morbidities. These in turn impact on the medication load she has to cope with, so concordance is important.
Book: Pharmacy case studies by Rebekah Raymond
Go to Case Study-16
Explore more Case Studie s | Guidelines
PharmD 1st year, 2nd year, 3rd year, 4th year books pdf free download
Case Study-17 Answers
1. Why should women of childbearing age be offered advice about pregnancy? Case Study-17
Ans: Mrs Jaya or other women like her should have been offered preconception advice prior to becoming pregnant because glucose control needs to be optimal to reduce the risks of miscarriage, congenital malformation, stillbirth and neonatal death associated with diabetes in early pregnancy. Preconception advice should also include information for the patient on how diabetes affects pregnancy and how pregnancy affects diabetes, what dietary supplements to take and advice on diabetes-related medicines that are unsafe to take during pregnancy.
2. Was she taking appropriate dietary supplements prior to conception? Case Study-17
Ans: Mrs Jaya was taking the appropriate dietary supplement; however, the recommended dose for women with diabetes is 5 mg daily, rather than 400 μcg daily. The 5-mg strength tablets are available on prescription.
3. What advice should she be given with respect to her regular medication? Case Study-17
Ans: Mrs Jaya should have been advised to stop her ramipril and simvastatin since both have been associated with an increased risk of birth defects.
Case Study - 18 Answers
You can get Case -18th answers with explanation by this link.
Go back to Case Study-18
Case Study - 19 Answers
Answers : (CORRECTED)
1. What is the likely diagnosis? Main differential diagnosis? Case Study-19
Ans: Diagnosis: Hypothyroidism.
The differential diagnosis is extensive.
However, Main Differential Diagnosis : Depression and Hypothyroidism
** Fatigue is a very common symptom of both physical and mental illness. The differential diagnosis is extensive and includes cancer, depression, anaemia, renal failure and endocrine diseases. He has a past history of depression, but currently has no obvious triggers for a further episode of depression. He is not waking early in the morning or having difficulty getting to sleep, which are common biological symptoms of severe depression.
There are a number of clues in this case to the diagnosis of hypothyroidism . Insidious onset of fatigue, difficulty concentrating, increased somnolence, constipation and weight gain are features of hypothyroidism. As in this case there may be a family or past medical history of other autoimmune diseases such as type 1 diabetes mellitus, vitiligo or Addison’s disease. Hypothyroidism typically presents in the fifth or sixth decade, and is about five times more common in women than men. Obstructive sleep apnoea is associated with hypothyroidism and may contribute to daytime sleepiness and fatigue. On examination the facial appearances and bradycardia are consistent with the diagnosis
2. How would you further manage this patient? Case Study-19
Ans: For the management of the patient in this case, patient should be advised for Thyroid Function Test . Level of TSH, T ₃ , T ₄ will lead to decide the accurate therapy for him.
**However, a starting dose of levothyroxine 50-70 μ g/day will be sufficient. Clinical benefits begin in 3-5 days.
Response is measured clinically and biochemically by the return of TSH to the normal range.
*Elderly patients or those with coronary heart disease should be started cautiously on T4 because of the risk of precipitating myocardial ischaemia.
The most common cause of hypothyroidism is autoimmune thyroiditis and the patient should have thyroid autoantibodies assayed.
Patients should be advised to avoid or do heavy physical labor with caution (hypotonia may be there sometimes).
· No specific diets are required for hypothyroidism . WHO recommends a daily dietary iodine intake of 150 μ g for adults.
CORRECTION : Case Study-19
1. Starting Dose of Levothyroxine should be 1.6 – 1.8 mcg/kg/day of lean body mass.
2. If started with levothyroxine, then, soyabean, walnuts, dietary fiber, calcium fortified juices should be avoided, if possible. When levothyroxine is given during continuous enteral nutrition for more than 7 days, the tube should be interrupted for at least one hour before and one hour after the dose of levothyroxine.
Ref-2: Recommendations for the use of medications with continuous enteral nutrition , “ American journal of health-system pharmacy: AJHP: official journal of the American Society of Health-System Pharmacists ”
Case Study - 20 Answers
1. What is the likely diagnosis in this case? & Are the Lab finding s clinically justified? Case Study- 20
Ans: Diagnosis: Hypothyroidism with Anemia.
! Ix Hashimoto Thyroiditis .
Yes , the lab findings are clinically justified.
· High TSH & low levels of T4 suggestive of Hypothyroidism.
· Stool occult blood positive: Reason to justify blood loss, decrease in levels of RBC, Haemglobin.
· High RDW with normal MCV indication for anemia further evalualtion needed for iron/B12/FA deficiency/anemia of chronic disease.
· Decrease in reticulocyte:(borderline to decrease) indication for iron deficiency/anemia of chronic disease.
· USG: indicates Thyroditis further lab values needs for antibody testing(thyroxine peroxidase).
2. What are the Pharmacist Intervention points in this case? Case Study- 20
Ans: Overdose: According to TSH value, Tab Thyronorm 75 mcg should have been started instead of Tab Thyronorm 25mg on the basis of wt. of patient (1.6-1.8mcg/kg/day).
Inappropriate Dose: There is no electrolytic imbalance seen therefore, isotonic (0.90% NS) should have been administered.
Untreated Indication: No medication for headache has been prescribed (antipyretic SOS can be prescribed)
Drug- Drug Interaction: Moderate Interaction
( Pantoprazole : Iron supplements ), ( Levothyroxine: Pantoprazole ), [ Levothyroxin: Iron Supplements ( Theoritical )]
Drug-Food Interaction: Is seen with soyabean products
3. Patient counselling regarding drug & disease? Case Study- 20
Ans: Disease: It is a disorder in which under activity of Thyroid glands occur(in local language).
Signs & Symptoms : related to slow metabolism (functioning) of the body .
· Fatigueness, dry skin, constipation, feeling cold, slow heart rate, weight gain
*Avoid soyabean & its products; cruciferous vegetables.
· Don’t chew the tablet
· Don’t split the tablet
· Tightly place the cap of container after use
· In the case of missed dose, Don’t take double dose; If it is time for next dose, take the single dose only.
· Don’t take the dose immediately, when you recall anytime, after you missed the dose
· If case, vomiting occurs immediately after taking the dose, consume it after sometime. If another episode occurs, consult your physician. Don’t stop taking the medication [this further may lead to untreated condition, resulting in myxedema (emergency condition)]
ü The Improvement of symptoms may not be evident for several weeks after the starting of the therapy. So, she should be counselled for proper medication adherence.
Drugs Counselling Points:
· Take tab Thyronorm on an empty stomach (30min to 1 hour prior to breakfast) once daily.
· Take tab Thyronorm 4 hours apart from Pantoprazole and Febac XT, Fdson MP Forte.
· Take tab Fdson MP Forte once daily after lunch
· Take one tab Febac XT after breakfast and another after dinner.
· For Tab Fdson MP Forte & Febac XT, you may observe metallic taste in the mouth. Therefore, don’t stop taking the medication.
· Take Tab Pantoprazole once a day 1 hour before lunch.
4. Write the Generic Names of above advised drugs. Case Study- 20
Ans: Generic
Pantoprazole Pantoprazole
Optineuron Vit. B-Complex
Fdson MP Forte Folic Acid 5mg + Methylcobalamin
1500mcg + Pyridoxine 20mg
Febac XT Ferrous Ascorbat 100mg + Folic Acid
1.5mg + Zinc Sulphate 22.5 mg
Thyronorm Levothyroxine Sodium
Case Study - 21 Answers
Q1 . What is the likely diagnosis ? Case Study-21
Ans: Diagnosis : Grave disease in pregnancy with impending thyroid storm and
IUFD at 23-24 weeks gestation.
Q2. Was the Treatment given to the patient justified according to clinical condition? Case Study-21
Ans: The dosing and the regimen advised to the patient is according to the prescribed guidelines and in the limit according to the lab reports.
***Methimazole 30mg BD, recommended 60-80mg/day (impending
thyroid storm cond. )
*** Lugol solution can be given 5 drops 2 times a day, but should not be more than 1 week.
*** The combination of propranolol 40 mg every 6 hours with iodide usually results in clinical improvement within 2 to 7 days.
Q3. Widely used anti-thyroid drugs in pregnant women with hyperthyroidism? Case Study-21
Ans: Propylthiouracil (PTU) and methimazole
Q4. What should be the Patient Counselling points? Case Study-21
· Pt should be instructed to report any new symptoms occurring.
· She should be counselled about the necessity of medication adherence.
· Next optimal time to conceive is once a euthyroid state is reached, should consult the practitioner for the same.
· Pre- pregnancy counselling for all patients with hyperthyroidism or a history of hyperthyroidism is imperative and use of contraception until the disease is controlled.
· Prior to conception, ablative therapy (radioiodine or surgery) or medical therapy may be offered when the thyroid gland is overactive.
· May experience the previous symptoms of hyperthyroidism along with new symptoms, consult the practitioner
· Avoid caffeine; stress reduction therapy should be suggested to relieve the symptoms of anxiety, nervousness, poor conc. May occur due to the miscarriage.
· It is normal to women to experience some Vaginal bleeding (light, menstrual-like bleeding) for several weeks after an abortion.
· Some pain is normal after an abortion, as the uterus is contracting.
· In this case, she should be specially suggested of the recommended interval to next interval to next pregnancy is at least 6 months (checking the hyperthyroid condition)
· She should be counselled with care and one to one interactions and the family members should be counselled to maintain a better social environment for her.
ADDITIONAL BASIC POINTS TO CONSIDER IN COUNSELLING:
· If case, vomiting occurs immediately after taking the dose, consume it after sometime. If another episode occurs, consult your physician. Don’t stop taking the medication [this further may lead to untreated condition , resulting in myxedema (emergency condition)]
Case Study - 22 Answers
1. Are there any drug-drug interactions? Case Study – 22
Ans: Major:
Diltiazem + Propranolol :: Increases the toxicity of other by unspecified mechanism. Can increase the risk of bradycardia.
**In this case, alternative drugs also have the major/serious interaction (alternatively: closely monitor)
Moderate:
Propranolol + Furosemide :: Decreases serum potassium.
Propranolol + Diltiazem :: Both increase anti-hypertensive channel blocking.
** Monitor Closely *Minor interactions are also there.
2. Is the dosing of medication for hyperthyroidism, according to standard treatment guidelines? Case Study – 22
Ans: Dose of carbimazole in hyperthyroidism; depends on the
FT4 levels. If the levels are raised 2 times higher than the upper limit of normal values then the dose is : 10-20 mg. So, correct in this case.
Given in split doses as duration of action is less than 24 hours, Twice a day is acceptable.
If HR >90 BPM Beta adrenergic blocker are considered, Propranolol dose :10-40 mg 3-4 times / day
For atrial fibrillation: diltiazem IV 15-20 mg is considered.
Maintenance dose is: 5-10 mg Carbimazole
3. What should be Patient counselling in this case, regarding drug & disease? Case Study – 22
Ans: Drugs:
· If case, vomiting occurs immediately after taking the dose, consume it after sometime. If another episode occurs, consult your physician. Don’t stop taking the medication.
Disease:
Hyperthyroidism
· It is a disorder in which thyroid hormones level are increased. So, they may cause some alarming symptoms related to increase in the metabolism of the body such as wt loss, over active bowel movement, heat intolerance, tremors, palpitations, nervousness, fatigue , weakness.
· Patient should be advised to follow medication adherence, Otherwise may increase the risk of cardiovascular problems.
· Pt should be informed that improvement in the symptoms may be seen in 3-4 weeks.
· A sightly elevated liver function test are commonly seen in some hyperthyroidism pts.
· Patient should be informed of side effects of ATDs and the necessity of informing the physician promptly if they should develop pruritic rash, jaundice, acolic stools or dark urine, arthralgias, abdominal pain, nausea, fatigue, fever, or pharyngitis. Preferably, this information should be in writing.
· Before starting ATDs and at each subsequent visit, the patient should be alerted to stop the medication immediately and call their physician if there are symptoms suggestive of agranulocytosis or hepatic injury.
· Patient should be informed about the condition like, Sometimes, after apparently successful treatment, the condition may return, and further treatment may be needed.
Hemorrhoids/ Anal fissure
· May be advised to sit over Hot water bag/ tub/brick not more than 15 min.
Note: As much as one can tolerate
· Keep a check on your regular bowel movement, avoid any straining.
· Pt should be advised to Eat less, oily less spicy easily digested food items
Case Study -23 Answers
1. What should be the further investigation ? Case Study- 23
Ans: Females with primary ovarian insufficiency-related estrogen deficiency are
at risk of osteopenia, osteoporosis, and fracture, especially if hypoestrogenism occurs early in life and before accrual of peak bone mass. Therefore, Dual-energy X-ray absorptiometry has been recommended for the evaluation of bone mineral density in women diagnosed with primary ovarian insufficiency.
Flow-mediated brachial artery diameter for endothelial dysfunction as there are cardiovascular risks .
[** The woman has evidence of hypogonadotrophic hypogonadism- she has low oestradiol
levels associated with low gonadotrophin stimulation from the anterior pituitary. This
may be due to various pituitary or hypothalamic causes, but in this case clearly relates to
anorexia nervosa and possibly excessive exercise . The raised prolactin is consistent with
stress and does not need to be investigated further. At a BMI below 18 kg/m2, menstru-
ation tends to cease, returning once the BMI increases again.]
-Furthermore, CBC, Liver & renal function test should be
monitored.
-Cognition, Mood, and Psychosocial Functioning
-Vasomotor Symptoms and Quality of Life
-Also include USG abdomen if needed!
2. How, this patient would be managed ? Case Study- 23
Ans: The combined oral contraceptive pill should be prescribed, which will prevent osteoporosis and bring on periods. However, this anorexia and primary ovarian insufficiency condition can be refractory to treatment, albeit pharmacologically induced.
Recommended dose:
|
|
| |
|
|
|
|
| 1-2 mg micronized 17 beta-estradiol (oral) | 2.5mg medroxyprogesterone acetate daily (oral)
| 10mg medroxyprogesterone acetate daily (oral) for 12 days each month |
| 0.625-1.25 mg conjugated equine estrogen (oral) | 100mg micronized progesterone daily (oral) | 200mg micronized progesterone daily (oral) for 12 days each month |
* One of the estrogen options to be combined with one of the progestogen options.
Also, vitamin supplementation and calcium should be started (if evident)
3. What Patient counselling points should be included in this case? Case Study- 23
Ans: Following Counselling points will help in effective recovering:
· Encouraging the woman to eat a more normal diet and to avoid exercising is the ideal management.
· Explanation that her periods will return if she increases her BMI may possibly encourage her to put on weight.
· Proper counselling should also be given to her parents, to help in stress reduction.
· She should be advised to consult dietician & nutritionist also, to maintain regular food habits with minimal or moderate physical exercise.
· Combined oral contraceptive pills are to be taken daily at approximately the same time each day.
· Avoid taking them greater than 24 hours apart as this could affect efficacy.
· When you initiate the contraceptive pills you are not protected from pregnancy prevention in the first 7 days and an alternative method of birth control is recommended during this time period (not required in this case)
· If she, miss a tablet, just take the missed tablet as soon as she remembers and the next tablet at the usual time (taking 2 tablets in 1 day).
· If she, miss 2 tablets in a row in the first or second week, then, take 2 tablets the day she remembers and 2 tablets the next day, then resume 1 per day.
· The most common adverse effect of combined oral contraceptive pills is break through bleeding.
· She may feel of nausea, headaches, abdominal cramping, breast tenderness, and an increase in vaginal discharge or decreased libido.
· Nausea can be avoided by taking the medication at night before sleep.
Ref: 1. https://www.acog.org/en/Clinical/Clinical%20Guidance/Committee%20Opinion/Articles/2017/05/Hormone%20Therapy%20in%20Primary%20Ovarian%20Insufficiency
2. Oral contraceptive pills, NCBI, National Library of Medicine,USA
Case Study -24 Answers
1. What should be the further investigation ? Case Study – 24
Ans: Further recommended investigations are :
Lipid panel , 2 hr OGTT, questionnaire for Depression, USG Abdomen (transabdominal)
2. How, this patient would be managed ? Case Study – 24
Ans : For acne: First line: hormonal contraception, and topical cream (benzoyl
peroxide/ tretinoin/adapalene/ antibiotic cream like clindamycin.
** depending upon the staging nd grading of acne
Obesity: First line is Lifestyle Modifications
Insulin resistance: First line METFORMIN (Dose 1500-2250 mg twice daily )
Hirsutism: First line: Hormonal contraception with or without anti androgen therapy
Menstrual irregularities : Clomiphene 50-100mg / day
3. What Patient counselling points should be included in this case? Case Study – 24
· Encouraging the woman to eat a more normal diet and to avoid leg exercising is the ideal management.
· Explanation that how increased BMI can also affect the normal menstrual cycle.
· For Acne: Wash the face twice daily with medicated face wash and can spill water during day time.
· Adapalene is UV, light sensitive, to be used at night. And wash your face before stepping out. It should be instructed that cold temperatures or wind may also increase skin irritation during drug therapy.
· Benzoyl peroxide : May cause dry skin and peeling, so avoid using higher concentration. Should be advised to use a test dose for over-the-counter (OTC) products due to potential hypersensitivity reactions. Apply small amount to skin for 3 days and if no discomfort occurs, use product as directed.
· Clomiphene citrate: Drug may cause decreased visual acuity. Patient should be instructed to report visual symptoms, such as blurred vision. Advise patient to take drug exactly as ordered, as administration is timing-sensitive.
Case Study - 25 Answers
1. What should be the further investigation for this patient ? Case Study – 25
Ans : The following further investigation should be suggested for her:
i. Thyroid profile
ii. HbA1C test
iii. Diurnal epinephrine test
2. Give the provisional diagnosis for this case. Case Study – 25
Ans : Provisional Diagnosis: Menopausal syndrome
3. How, this patient would be managed ? Case Study – 25
Ans : Following management plan is recommended for the patient:
Estradiol low dose transdermal patch is to be started with min possible dose
of : 0.025 mg with size 5 cm ² patch. (Duration : 3 weeks of therapy + 1 week off)
An oral progestin is also added for only 10-14 days every month this will promote sleep.
( Dose : 10mg dydrogesterone OR Micronised progesterone capsule 100mg Frequency : at night 1 tab)
For glycine and glutamate: glutathione 20mg is recommended Or NAC(n-Acetyl cysteine) if needed
For PEA: vit B6 is advised daily, at lunch time.. 1tab, MVBC most preferably
4. What Patient counselling points should be included in this case? Case Study – 25
Ans: About disease:
- Give information to menopausal women and their family members (as appropriate) that includes:
- That a change in their menstrual cycle they may experience a variety of symptoms associated with menopause, including:
· Vasomotor symptoms (for example, hot flushes and sweats)
· Musculoskeletal symptoms (for example, joint and muscle pain)
· Effects on mood (for example, low mood)
· Urogenital symptoms (for example, vaginal dryness)
· Sexual difficulties (for example, low sexual desire)
· Benefits and risks of treatments for menopausal symptoms
· Long-term health implications of menopause
· Hormone replacement therapy (HRT) aids for Psychological symptoms , Consider HRT to alleviate low mood that arises as a result of the menopause
· Non-pharmaceutical, for example cognitive behavioral therapy (CBT), Consider CBT to alleviate low mood or anxiety that arise as a result of the menopause
About drugs: (general points)
Transdermal patch:
Application : It is to be applied to non hairy skin, below waist on upper quadrant of abdomen.
Replace the patch in every 3-4 days using a different site.
· Gradually reducing HRT may limit recurrence of symptoms in the short term
· Gradually reducing or immediately stopping HRT makes no difference to their symptoms in the longer term
**Long-term benefits and risks of hormone replacement therapy–
· Venous thromboembolism:The risk of venous thromboembolism (VTE) is increased by oral HRT compared with baseline population risk
· The risk of VTE associated with HRT is greater for oral than transdermal preparations
· Consider transdermal rather than oral HRT for menopausal women who are at increased risk of VTE, including those with a BMI over 30 kg/m ²
· Consider referring menopausal women at high risk of VTE (for example, those with a strong family history of VTE or a hereditary thrombophilia) to a haematologist for assessment before considering HRT
Lifestyle changes:
· She should be suggested to exercise regularly
· She can take cold water bath as required.
· She should be counselled to avoid stress and enjoy day to day activity.
· Advise her to deep her feet in mild-salted, tolerable cold water, to ease her in hot flashes.
· Consult your gynecologist and ask her about vaginal wash products to prevent dryness, if needed.
· isoflavones or black cohosh may relieve vasomotor symptoms advice to consume soy products, nuts raisins, legumes, sesame, peanuts, Meat, pork, chicken, egg , banana.
Note: Ensure that menopausal women and healthcare professionals involved in their care understand that there is no clear evidence for SSRIs or SNRIs to ease low mood in menopausal women who have not been diagnosed with depression. (NICE Guidelines)
1. Indian Menopause Society ( https://indianmenopausesociety.org/prescription-writing-module-for-hormone-therapy/ )
2. Essentials of medical Pharmacology, Tripathi.KD, 6 th edition.
3. https://www.acc.org/latest-in-cardiology/ten-points-to-remember/2020/02/10/12/13/hormone-therapy-for-postmenopausal-women
4. https://dailymed.nlm.nih.gov/dailymed/lookup.cfm?setid=c714974b-766f-42f2-a846-b0c1f5a60560
5. https://www.jmidlifehealth.org/article.asp?issn=0976-7800;year=2013;volume=4;issue=2;spage=77;epage=106;aulast=Meeta%2C
Case Study -26 Answers
1. How should the ovarian hormones she lacks be replaced? Case Study- 26
Ans: The patient should be advised to start daily transdermal estradiol (100
mcg/day) along with oral natural progesterone (200mg/day) for the last 12 days of each 28 day cycle. On this regimen, her symptoms should disappear and normal monthly uterine bleeding resume.
2. What extra measures should she take for her osteoporosis while receiving treatment? Case Study- 26
Ans: She should also be advised to get adequate exercise and increase her calcium
and vitamin D intake as treatment for her osteoporosis.
Clinical evidence:
Non-pharmacological approaches–
· A balanced diet, adequate calcium and vitamin D intake, weight-bearing exercise, maintaining a healthy body weight and cessation of smoking and moderation of alcohol intake are primary goals in reducing fracture risk.
· Calcium is essential for bone health, and there is evidence that calcium supplementation in older women reduces the risk of fracture.
· The recommended nutritional intake (RNI) for calcium is 1000mg/day, and for vitamin D 800 IU/day
**Higher calcium intake during growth and early adulthood is associated with higher peak bone mass.
**Based on recent concerns of a potential association between calcium supplement use and increased risk of myocardial infarction, calcium supplements should not be prescribed when dietary calcium intake is adequate (1000 – 1200 mg/day).
Case Study - 27 Answers
1. What all investigations are needed for the further management?
· Her 10-year risk of fracture FRAX is the risk assessment tools validated for use
· She has been taking multivitamin with calcium so
· Consider assessing serum 25-OH-D
· dual-energy X-ray absorptiometry (DXA) and repeat DXA every 1 to 2 years until findings are stable
· Additional tests for Clinical Identification of Vertebral Fracture :
2. How this patient would be managed ?
· Counsel patients to maintain adequate dietary intake
of calcium, to a total intake (including diet plus supplement, if needed) of 1,200 mg/day for women age ≥50 years
· Pharmacologic therapy is strongly recommended for Patients with osteopenia or low bone mass and a history Of fragility fracture of the hip or spine
· Pharmacologic therapy is strongly recommended for Patients with a T-score of −2.5 or lower in the spine, femoral neck, total hip, or 1/3 radius
Calcium: 1200mg/day is recommended so as per the patients need either 500mg twice daily OR 1000mg once daily is given with food items rich in calcium..
Vit D3: If serum25[OH]D deficiency is seen then according to individualize patient therapy is given as per this case: vit D3 5000IU / day for 8-12 weeks is recommended…. With the maintenance therapy of 1000-2000 IU/day
3. How will you do the Patient counselling in this case?
· Counsel patients to maintain adequate dietary intake of calcium rich products.
· Counsel patients to avoid or stop smoking.
· Counsel patients to maintain an active lifestyle, including weight-bearing, balance, and resistance exercises
· Provide counseling on reducing risk of falls, particularly among the elderly.
· Daily sun bath is advised.
· Consider referral for physical therapy, which may reduce discomfort, prevent falls, and improve quality of life.
· avoiding use of tobacco And excessive use of alcohol;
· This “bone healthy” lifestyle is Important for everyone, not only patients with osteopenia And osteoporosis.
· Weight-bearing exercise includes walking, jogging, Tai Chi, stair climbing, and dancing, among other activities.
· Muscle-strengthening exercise includes weight training and other resistive exercises.
· Before initiating an exercise program in an individual with osteoporosis, a clinician’s evaluation is recommended.
· Physical therapy plays an important role in the effort to mitigate sarcopenia and reduce risk of falls.
· Measures for Prevention of Falls
· Anchor rugs
· Minimize clutter
· Remove loose wires
· Use nonskid mats
· Install handrails in bathrooms, halls, and long stairways
· Light hallways, stairwells, and entrances
· Encourage patient to wear sturdy, low-heeled shoes
4. Mention the indications for BMD testing.
· All women 65 years of age or older
· All postmenopausal women
· With a history of fracture(s) without major trauma
· With osteopenia identified radiographically
· Starting or taking long-term systemic glucocorticoid therapy (≥3 months)
· Other perimenopausal or postmenopausal women with risk factors for Osteoporosis if willing to consider pharmacologic interventions
· Low body weight (<127 lb or body mass index <20 kg/m2)
· Long-term systemic glucocorticoid therapy (≥3 months)
· Family history of osteoporotic fracture
· Early menopause
· Current smoking
· Excessive consumption of alcohol
· Secondary osteoporosis
Case Study-28 Answers
1. what is the significance of t- score case study – 28.
• The T-score on your bone density report shows how much your bone mass differs from the bone mass of an average healthy adult.
• DEXA accomplishes with only one-tenth of the radiation exposure of a standard chest x-ray and is considered the gold standard for osteoporosis screening
• Standard X-rays may show weakened bones. But at the point when bone weakness can be seen on standard X-rays, it may be too far advanced to treat. Bone densitometry testing can find decreasing bone density and strength at a much earlier stage when treatment can be beneficial
• The World Health Organization has established the following classification system for bone density:
1. If your T-score is –1 or greater: your bone density is considered normal.
2. If your T-score is between –1 and –2.5: you have low bone density, known as osteopenia, but not osteoporosis.
3. If your T-score is –2.5 or less: you have osteoporosis, even if you haven’t yet broken a bone.
2. How this patient would be managed ? Case Study – 28
• A daily calcium intake of 1000 mg for men under 70 years is advised(only of dietary calcium is not sufficient enough). So 500 mg twice daily once on morning and other at night is ideal.
• Vit D starting from 800 IU/day (once daily OR 400 IU twice daily)
3. How will you do the Patient counselling in this case? Case Study – 28
• to not involve yourself in smoking again
• Quit drinking alcohol
• Regular exercise helps make your bones stronger. • physical activity is reviewed and prescribed by an exercise professional, such as a physiotherapist or exercise physiologist. This is because some activities like jumping, running and twisting can be hazardous to weaker bones, particularly if you have had a fracture. • Other forms of exercise such as strength training can actually benefit the bones
• Foods high in calcium include milk products, leafy green vegetables, sardines, salmon, tofu, and almonds.
• You can get enough vitamin D from being in direct sunlight for 10 to 15 minutes, two or three times weekly.
Falls prevention program –
• falls are responsible for the majority of hip and spine fractures in older people.
• A falls prevention program can provide strategies to help you prevent falls occurring
Measures for Prevention of Falls
• Anchor rugs
• Minimize clutter
• Remove loose wires
• Use nonskid mats
• Install handrails in bathrooms, halls, and long stairways
• Light hallways, stairwells, and entrances
Sources Of Calcium :
• Milk & milk products -cheese, yogurt, ice cream, buttermilk
• Turnip greens, Spinach, Kale, Radish, Okra( lady Finger),bottle gourd
• Dry Beans, such as rajma, chole, chana, lobia, other kidney beans, black-eyed peas, kidney beans, black beans
• Kamal gatta(makhana)
• Water chestnuts/cresnuts(singhada)
• Nuts like peanuts, groundnuts, walnuts, cashew nuts ,almonds , and fruit seeds.
• Seeds like melon seeds, watermelon seeds etc
• Fruits like Custard Apple, Guavas, Banana, Jackfruits, Figs, Oragnges & chiku
Sources of Vit D :
1. Sunlight
2. Food – fatty fish (examples are mackerel, salmon and tuna), egg yolks and liver.
Calcium: take the tablet with meals… and better at night…
Vit D: with meals.. Together with calcium supplements.
Case Study - 29 Answers
1. What findings are needed for the diagnosis of POAG? Case Study – 29
§ enlarged cup-to-disc ratio
§ Visual acuity loss
§ Family history of glaucoma
§ Race/ Ethnicity (African American)
2. Explain the result of the above mentioned investigations of the ocular exam? Case Study – 29
1. evidence of increased IOP ,
2. optic nerve head abnormality
3. open anterior chamber angle,
4. visual field deficits and no history to suggest a secondary glaucoma (glaucoma due to an identifiable cause.
· Visual field examination shows defects that are consistent with the state of the optic nerve.
· Measurements of the nerve fiber layer over the optic nerve can confirm an abnormally thin nerve.
3. How this patient would be managed ? Case Study – 29
Ans : **Damage is permanent to eyes—it cannot be reversed. But medicine and surgery help to stop further damage.
However, Latanoprost 0.005% eyedrops only once at bedtime
And, If further required,then,
Pilocarpine 1-4% eyedrops thrice a day OR
Brimonidine tartarate 0.2% twice daily OR
Dorzolamide 2% eyedrops 2-3 times a day can be advised.
**If patient is not controlled on 2 topical drugs, then consider alternative treatment options with either laser trabeculoplasty or glaucoma filtering surgery.
4. Enlist the Patient counselling points in this case? Case Study – 29
Patient should be counselled as-
Counselling regarding administration of drops
· It is extremely important to use your glaucoma eye drops exactly as your ophthalmologist tells you to. That includes taking every dose, every day.
· But remember, glaucoma eye drops won’t cure glaucoma or improve your vision. They prevent your vision from getting worse. If you don’t use them as prescribed, you could lose your vision.
How to put drops In eyes:
Follow these steps to put in your eye drops:
· Tilt your head back and look up
· With one hand, pull your lower eyelid down and away from your eyeball — this makes a “pocket” for the drops
· With the other hand, hold the eye drop bottle upside down with the tip just above the pocket
· Squeeze the prescribed number of eye drops into the pocket
· For at least 1 minute, close your eye and press your finger lightly on your tear duct (small hole in the inner corner of your eye) — this keeps the eye drop from draining into your nose
· to use more than 1 type of eye drop, like different drops for different eye conditions, wait at least 5 minutes between each type.
Follow these tips to protect your eyes from infection:
· Wash your hands with soap and water before you use eye drops
· Don’t touch the tip of the eye drop bottle with your hands
· Don’t let the tip of the eye drop bottle touch your eye or eyelid
Storage of drops:
· All eye drops have an expiration date, which refers to the shelf life of a drop which has not been opened.
· opened Eye Drops can lose potency and even become contaminated.
· Most eye drops are stored in a cool dry place and should not be used longer than one month after the bottle is opened, unless otherwise stated on the label.
· Pt should be advised to mention the date of opening of drops on the label itself.
General points:
· Do not drive or operate machinery if your glaucoma eye drops make you feel tired or drowsy.
· Blurry vision, stinging, and redness may improve with time. But if the side effects still bother you, call your ophthalmologist.
· Never suddenly quit taking your medicine unless your doctor tells you to.
Case Study -30 Answers
1. what is the diagnosis in this case case study – 30.
Ans • Suspected acute angle closure glaucoma R eye
• Narrow angle L eye
2. What is the mechanism of angle closure in an episode of acute angle closure glaucoma resulting from a pupillary block?
• The apposition of the pupil border against the lens obstructs aqueous humor flow through the pupil and creates a pressure gradient with increased pressure behind the iris. This moves the iris forward with subsequent apposition of the peripheral iris with the trabecular meshwork. • Decreased drainage by the trabecular meshwork causes increased pressure in the anterior chamber and pushes the iris against the lens. • A portion of vitreous humor moves anteriorly and around the lens, blocking the trabecular meshwork. • Increased aqueous humor drainage through the trabecular meshwork causes a decreased pressure in the anterior chamber, causing a pressure gradient that presses the iris forward and blocks the angle.
3. Mention in brief the surgical options for the disease? Case Study – 30
Ans: laser iridotomy Is recommended as the first line treatment for all patients Laser peripheral iridotomy/ Surgical iridectomy Preferably, a laser peripheral iridotomy (LPI) is done to alleviate pupillary block. It allows the aqueous to bypass the pupil, providing an alternative route for outflow from posterior to anterior chambers of the eye. Surgical iridectomy may rarely be needed in case of failures of laser iridotomy. Laser peripheral iridotomy: Technique: The role and limitations and possible complications of laser iridotomy are explained to the patient. To reduce the risk of post laser IOP spike and inflammation, apraclonidine 1% or brimonidine 0.15/ 0.2% can be used either before or after the procedure. Alternatively, oral/ topical carbonic anhydrase inhibitors or topical glycerine (in case of corneal epithelial edema secondary to raised IOP) can be used in selected patients. • It is preferable to reduce IOP to a safe level prior to the procedure. To reduce the risk of bleeding, selected patients on oral anticoagulants for systemic diseases should be counseled and may be asked to stop their anticoagulants for a few days prior to the procedure. • Usually iridotomy is recommended between 11-1 o’ clock beneath theeyelids avoiding the 12 o’ clock position. However, others prefer 3 and 9 o’ clock positions. • PI is avoided at lid margins to reduce symptoms of glare formed by tear meniscus. Successful penetration is seen with a gush of pigments in anterior chamber with a visible deepening of anterior chamber. A minimum opening of 150-200 microns is aimed to ensure patency. • Surgery is usually considered in case of failure of medical/ laser . • Management for IOP control or progression of glaucoma despite maximum medical Management. • Trabeculectomy alone or combined with cataract surgery.
Case Study - 31 Answers
Questions/Answers:
1. What are the patient counselling points in these case? Case Study-31
With one hand, pull your lower eyelid down and away from your eyeball — this makes a “pocket” for the drops
To use more than 1 type of eye drop, like different drops for different eye conditions, wait at least 5 minutes between each type.
Follow these tips to protect your eyes from infection :
· Opened Eye Drops can lose potency and even become contaminated.
· Wash your face 3-4 times per day with plain water
· Soak your eyes with cotton filled of water if having any discomfort , it will ease in your painful eyes.
· Don’t touch your eyes with bare hands
· If accidently touching the infected eye then wash hands .. OR least possibly don’t touch the eyes which is non infected.
· Avoid any extra strain on eyes with limited activity of gadgets
· Do not drive or operate machinery if your eye drops make you feel tired or drowsy.
2. What is not a typical exam finding of conjunctivitis? Case Study-31
· Eyelid erythema
· Red conjunctiva
· Subepithelial corneal infiltrates
· Anterior chamber cell
· Mucous in the canthus
Case Study - 32 Answers
1. what are the possible differential diagnosis in this case case study – 32.
Ans: Differential Diagnosis • Viral Conjunctivitis • Hyperacute Bacterial Conjunctivitis • Chlamydial Conjunctivitis • Allergic Conjunctivitis • Superficial Keratitis • Blepharitis • Episcleritis • Scleritis • Acute Angle-closure Glaucoma • Acute Anterior Uveitis
2. What is the role of Ofloxacin in this Patient’s case?
Ans: Ofloxacin was prescribed to replace tobramycin due to suspecting toxic reaction to Tobramycin. Patient was asked to instil one drop of ofloxacin into the left Eye q2h on the day, to reduce the dosage to qid the next day if the condition Improves, the right eye is to be treated with ofloxacin qid. A review appointment was Scheduled in one week time.
3. Why Tobramycin wasn’t readvised after the PCR result, is there any evidence suggestive for the change?
Case study – 32.
Ans: 1. the patient had an adverse Reaction to the aminoglycoside, this was evident when she noted that the Discontinuation of tobramycin had reduced ocular hyperaemia, but resulted an Increase in ocular discharge. 2. PCR was performed to rule possible viral and Chlamydia infection. This was deemed necessary as her condition was unresponsive To prescribed therapy. 3. The ophthalmologist had a strong suspicion that the condition Was caused by a gram-negative bacteria due to the nature of ocular discharge, Therefore prescribed ofloxacin as it has a relatively strong antibacterial activity Against gram-negative organisms.
Case Study - 33 Answers
1.What should Leanne’s GP consider as a possible diagnosis? Case Study- 33
Ans: Following points should be considered for the diagnostic purpose-
· Take a detailed history from Leanne and her parents and explore the ‘trances’ because they have experienced and witnessed them. This should determine whether an epileptic seizure is likely to have occurred.
· Diagnosis should not be based on the presence or absence of single features.
· Consider a history of absence seizures. Leanne is the right age
and gender for this relatively common childhood epilepsy syndrome.
· The frequent occurrence of the daydreams and the fact that they interrupt her activities are suspicious features of childhood-onset absence epilepsy.
· The positive family history is supportive but not diagnostic of this epilepsy syndrome. Childhood-onset absence epilepsy is classified as an idiopathic (presumed genetic) generalised epilepsy.
· Confirm the diagnosis in the surgery. Children with typical absence seizures will often experience one of their absences during hyperventilation (over-breathing). However, hyperventilation usually has to be performed well and for at least 3 minutes to induce an absence.
· Refer Leanne to a general paediatrician with an interest in epilepsy or a paediatric neurologist to establish the diagnosis.
Ans: First, information should be given to Leanne and her parents about the reasons For further tests, and they should be carried out in a child-centred environment.
· An electroencephalogram (EEG) should be arranged and Leanne should have This test soon after it has been requested. Because the paediatrician or Paediatric neurologist suspects that her seizures are epileptic in origin, the EEG Should be performed to support a diagnosis of epilepsy.
· It should not be used in Isolation to make a diagnosis of epilepsy.
· The healthcare professionals carrying Out the EEG should encourage Leanne to hyperventilate, because this is one of The provocation techniques always undertaken during an EEG.
· The EEG is abnormal, as in the vast majority of children with childhood-onset Absence epilepsy. It ‘captures’ an absence seizure, particularly during Hyperventilation.
3. What should the discussion around medication include, and what medications may be Prescribed? Case Study- 33
· The discussion on anti-epileptic medication should include the different . Medications that are available, and specifically ethosuximide, sodium valproate And lamotrigine, the evidence base for using these medications.
· Their Common and potentially unwanted side effects. Discussion should also include The likely outcome or prognosis of the epilepsy and specifically that it will go into Spontaneous remission (that is, it will ‘go away’).
· The family should also be Referred to a paediatric epilepsy nurse who can provide information and Guidance on lifestyle and other non-medical issues.
· Ethosuximide or sodium valproate should be offered as a first-line treatment.
Case Study: Management of a Middle-Aged Patient with Multiple Comorbidities
—a 52-year-old woman reports a 2-week history of dyspnea and wheezing, and presents with mild respiratory distress with audible wheezing. what should next steps be to provide optimal care.
By Shawn E. Kuhmann, PhD Reviewed by Joe G. Zein, MD
Societies are now caring for a higher number of older individuals with multiple chronic diseases, including asthma. 1 In addition to age-related comorbidities, older asthma patients are at a particular risk for severe asthma due to lower lung function compared with younger adults with asthma. 2 Consistent with this, cluster analyses based on the National Heart, Lung, and Blood Institute (NHLBI)-Severe Asthma Research Program (SARP) cohort identified a unique phenotype of older asthmatics with severe symptoms and reduced lung function. 3 Similarly, older asthmatics have been observed to have increased asthma treatment failures and to respond less well to inhaled corticosteroids (ICS). 4

Case presentation and patient history
Dr. L is a 52-year-old college professor with no significant medical history except for obesity (body mass index of 36). She reports occasional heartburn, which is self-medicated with over-the-counter antacids.
She presented in June to the emergency room (ED) reporting a 2-week history of dyspnea and wheezing. Upon arrival, she was in mild respiratory distress with audible wheezing. Yet, she was able to speak in full sentences and had a room air oxygen saturation of 92%. The physical exam was significant for tachycardia (heart rate of 110 bpm), tachypnea, and bilateral inspiratory and expiratory wheezing. There was no accessory muscle use. The peak expiratory flow (PEF) rate was only 250 L/min.
In the ED, she received nebulized albuterol and a corticosteroid injection. Albuterol resulted in significant improvement in her symptoms and resolution of the respiratory distress. She was discharged home with a 5-day prednisone taper and referred to the asthma center for further management.
In the asthma clinic, she continued to have mild expiratory wheezing. Upon additional questioning, she reported that she entered menopause about a year prior and was recently started on hormone replacement therapy (HRT) by her primary care physician for hot flashes and vaginal dryness. Since then, she started noticing more respiratory symptoms occurring mostly at night, which she linked to menopause. Similarly, she noticed more heartburn symptoms.
She did not report any previous history of childhood asthma, but her 17-year-old daughter is being treated with inhaled fluticasone and oral contraceptives for severe premenstrual asthma. She did not report having any food or environmental allergies or any pets at home. She also did not report any significant occupational or smoking history.
An office spirometry revealed a baseline forced expiratory volume in 1 second (FEV1) of 1.8 L (61%), which improved to 2.76 L (94%) after bronchodilator use. The percent FEV1 change was 53%, meeting the American Thoracic Society criteria for positive bronchodilator response. The measured exhaled nitric oxide was 16 ppb.
Dr. L is a middle-aged obese nonatopic woman with a lung function test showing airway obstruction and a positive bronchodilator response. Such clinical characteristics suggest late-onset asthma, and meet "cluster 3" phenotypic criteria according to the NHLBI-SARP cluster phenotypes, which include: 3
- Moderate reductions in FEV1
- Mostly older obese women
- Increased medication requirements, including high-dose ICS
- Frequent oral corticosteroid use
- High healthcare utilization
It is likely that her asthma was triggered or exacerbated by HRT and gastroesophageal reflux disease (GERD).
Treatment options
According to Global Initiative for Asthma (GINA) guidelines , initial therapy includes low-dose ICS and an as-needed short-acting beta2-agonist (SABA) such as albuterol. 5
Dr. L was advised that while high-dose ICS can place asthma patients at risk for osteopenia and cataracts, both asthma therapies are relatively safe. 5 She was also advised that a spacer is recommended with hydrofluoroalkane inhalers and that she needs to rinse her mouth after each ICS use. 5 She received asthma education and was provided an asthma action plan to help her manage her asthma. A follow-up appointment is set for 4 weeks in order to assess the efficacy of the treatment regimen and the need for stepping up therapy (ie, adding a long-acting beta2-agonist [LABA] to the ICS). 5
Additionally, GERD therapy is recommended to control heartburn and reflux symptoms, and she was advised to stop and avoid HRT. 5 A weight reduction plan is put into place; advice is given about the management of exercise-induced bronchoconstriction. 5
Treatment outcome
Dr. L returns 4 weeks later to the chest clinic for follow-up. She reports partial improvement in her dyspnea and exercise intolerance. However, she continues to report cough, wheezing, and dyspnea on exertion more than twice a week requiring rescue albuterol. She has been compliant with therapy and has been using her inhalers with a spacer routinely. She also reports losing 3 lb since her last visit and says that her heartburn has been controlled with therapy. Her peak flow measurement improved from an average of 250 to 350 L/min. A repeated office spirometry demonstrated a baseline percent predicted FEV1 of 72%. Since her asthma was not fully controlled, a LABA was added to her treatment regimen. She was advised to continue measuring peak flow and to return in 1 to 3 months to assess asthma control and response to therapy.
Although there are a wide variety of asthma phenotypes, treatment is uniformly applied to all patients in a stepped-care approach. 5-8 However, the morbidities and costs associated with the overtreatment and/or undertreatment of this common disease provide a rationale for precision medicine, particularly for older asthmatics (age 30 and older), who comprise a heterogeneous group of patients.
Aging and menopause Older asthmatics tend to have multiple comorbidities, such as GERD, rhinosinusitis, and obstructive sleep apnea, which may contribute to more severe asthma. 5 In addition, data suggest that older asthma patients have a greater risk of treatment failure, particularly for ICS, compared with younger adult patients; this finding was observed in a recent study based on data from ten Asthma Clinical Research Network trials. 4
Importantly, lung aging occurs over the course of life. 2 In a cross-sectional study of patients enrolled in NHLBI-SARP, the risk of severe asthma increased by 7% each year until age 45. 2 Asthma was more likely to be severe in older adult patients (older than age 45 versus age 18-45) independent of asthma duration or age-related comorbidities. 2 After age 45, the risk of severe asthma continued to increase with age in men but not women. 2 These data, along with other reports, suggest that asthma may improve with menopausal transition, when sex hormones wane. 9,10
Overview of comorbidities and factors affecting asthma relevant to this case
HRT Postmenopausal HRT may be disadvantageous and worsen asthma severity in menopausal women. 11 HRT was also shown to be associated with an increased risk of asthma diagnoses in postmenopausal women in the prospective Nurses' Health Study and in the prospective French E3N study ; there was also an increased prevalence of asthma in perimenopausal women using HRT in the population-based, cross-sectional Respiratory Health in Northern Europe study . 9,12,13 This finding regarding HRT emphasizes the importance of reviewing the medications asthma patients take.
GERD The most common digestive system disorder in the United States, GERD affects nearly one third of Americans and has been reported in 40% to 80% of asthma patients. 14 GERD may cause bronchoconstriction through microaspiration into airways or through effects on the vagus nerve. 14 Asthma may also favor the development of GERD. 14 A meta-analysis on the effects of proton pump inhibitor (PPI) therapy on asthma in adults found that PPI therapy yielded a small but significant improvement in morning PEF rate, with a larger benefit in morning PEF rate in patients with GERD than in those without. 14 However, other objective and subjective outcomes were not significantly altered by PPI treatment. 14 The authors concluded that the benefit from GERD treatment is unlikely to be clinically significant and there is not enough evidence to support the use of PPIs to treat asthma in adults. 14
Obesity Asthma is more severe in obese compared with nonoverweight patients. 15 In the National Asthma Survey , obese respondents more often reported symptoms all of the time, missed more work days, and were more likely to use SABA and ICS treatments. 15 When classified according to the GINA guidelines, obese respondents were also more likely to use controller medications, less likely to be in remission, and more likely to have persistent and/or severe persistent asthma. 15
Asthma is also more difficult to control in obesity. 16,17 In a post-hoc study of four placebo-controlled trials , the effect of an ICS on the number of asthma control days decreased with increasing body mass index. 17 Similarly, in another pooled analysis , fewer obese individuals achieved asthma control with an ICS + LABA or an ICS alone compared with nonobese patients. 16
Importantly, the Global Initiative for Asthma guidelines recommend including a weight reduction program in the treatment of obese patients with asthma. 5 A randomized trial studying the effects of weight loss by dietary intervention, exercise intervention, or both on clinical asthma outcomes in overweight and obese men and women found that a 5% to 10% weight loss improved measures of lung function, asthma control, and quality of life. 18 Weight loss greater than 10% further improved lung function, but not asthma control or quality of life. 18
The treatment of older asthma patients may be complicated by the presence of comorbidities, such as GERD and obesity, and by the use of HRT in postmenopausal women. Addressing all of these factors in a personalized, precision medicine approach is essential to providing optimal care to older asthma patients and ensuring the best outcomes.
Published: April 16, 2018
- 1. Centers for Disease Control and Prevention. The State of Aging and Health in America 2013.
- 2. Zein JG, Dweik RA, Comhair SA, et al; Severe Asthma Research Program. Asthma is more severe in older adults. PLoS One . 2015;10:e0133490.
- 3. Moore WC, Meyers DA, Wenzel SE, et al; National Heart, Lung, and Blood Institute's Severe Asthma Research Program. Identification of asthma phenotypes using cluster analysis in the Severe Asthma Research Program. Am J Respir Crit Care Med . 2010;18:315-323.
- 4. Dunn RM, Lehman E, Chinchilli VM, et al; NHLBI Asthma Clinical Research Network. Impact of age and sex on response to asthma therapy. Am J Respir Crit Care Med . 2015;192:551-558.
- 5. Global Initiative for Asthma. Pocket Guide for Asthma Management and Prevention, 2015.
- 6. Marozkina NV, Wang XQ, Stsiapura V, et al. Phenotype of asthmatics with increased airway S-nitrosoglutathione reductase activity. Eur Respir J . 2015;45:87-97.
- 7. Holguin F, Bleecker ER, Busse WW, et al. Obesity and asthma: an association modified by age of asthma onset. J Allergy Clin Immunol . 2011;127:1486-1493.e2.
- 8. Wenzel SE. Asthma: defining of the persistent adult phenotypes. Lancet . 2006;368:804-813.
- 9. Troisi RJ, Speizer FE, Willett WC, et al. Menopause, postmenopausal estrogen preparations, and the risk of adult-onset asthma. A prospective cohort study. Am J Respir Crit Care Med . 1995;152:1183-1188.
- 10. O'Connor KA, Ferrell RJ, Brindle E, et al. Total and unopposed estrogen exposure across stages of the transition to menopause. Cancer Epidemiol Biomarkers Prev . 2009;18:828-836.
- 11. Bønnelykke K, Raaschou-Nielsen O, Bisgaard H, et al. Postmenopausal hormone replacement therapy is associated with increased risk of asthma hospitalization. Eur Respir J . 2011;38(suppl 55):P4111.
- 12. Romieu I, Fabre A, Fournier A, et al. Postmenopausal hormone therapy and asthma onset in the E3N cohort. Thorax . 2010;65:292-297.
- 13. Gómez Real F, Svanes C, Björnsson EH, et al. Hormone replacement therapy, body mass index and asthma in perimenopausal women: a cross sectional survey. Thorax . 2006;61:34-40.
- 14. Chan WW, Chiou E, Obstein KL, et al. The efficacy of proton pump inhibitors for the treatment of asthma in adults: a meta-analysis. Arch Intern Med . 2011;171:620-629.
- 15. Taylor B, Mannino D, Brown C, et al. Body mass index and asthma severity in the National Asthma Survey. Thorax . 2008;63:14-20.
- 16. Boulet LP, Franssen E. Influence of obesity on response to fluticasone with or without salmeterol in moderate asthma. Respir Med . 2007;101:2240-2247.
- 17. Peters-Golden M, Swern A, Bird SS, et al. Influence of body mass index on the response to asthma controller agents. Eur Respir J . 2006;27:495-503.
- 18. Scott HA, Gibson PG, Garg ML, et al. Dietary restriction and exercise improve airway inflammation and clinical outcomes in overweight and obese asthma: a randomized trial. Clin Exp Allergy . 2013;43:36-49.
Treatable traits and future exacerbation risk in severe asthma, baker’s asthma, the long-term trajectory of mild asthma, age, gender, & systemic corticosteroid comorbidities, ask the expert: william busse, md, challenges the current definition of the atopic march, considering the curveballs in asthma treatment, do mucus plugs play a bigger role in chronic severe asthma than previously thought, an emerging subtype of copd is associated with early respiratory disease.

An official website of the United States government
The .gov means it’s official. Federal government websites often end in .gov or .mil. Before sharing sensitive information, make sure you’re on a federal government site.
The site is secure. The https:// ensures that you are connecting to the official website and that any information you provide is encrypted and transmitted securely.
- Publications
- Account settings
Preview improvements coming to the PMC website in October 2024. Learn More or Try it out now .
- Advanced Search
- Journal List
- Clin Case Rep
- v.11(2); 2023 Feb
Challenging case of severe acute asthma in a mechanically ventilated patient managed with sevoflurane
Satheesh munusamy.
1 Intensive Care Department, Hamad Medical Corporation, Doha Qatar
Seyedeh Saba Nabavi Monfared
2 Emergency and Trauma Pharmacy Department, Hamad Medical Corporation, Qatar University, Doha Qatar
Phool Iqbal
3 Internal Medicine Department, Metropolitan Hospital Center, New York New York, USA
Ahmed Lutfe Mohamad Abdussalam
4 Hamad General Hospital, Doha Qatar
5 Weill Cornell Medicine Qatar, Qatar
Associated Data
Acute severe bronchial asthma is a chronic inflammatory disease characterized by hyperresponsiveness of the airways leading to bronchoconstriction. We present a case of refractory life‐threatening bronchial asthma that was managed with sevoflurane gas along with the standard treatment and achieved stability and clinical improvement through its bronchodilator and anesthetic effect.
1. INTRODUCTION
Acute severe asthma is a life‐threatening emergency characterized by severe tachypnea, tachycardia, and type 1 respiratory failure. 1 According to the international standard guidelines, it is managed with bronchodilators, systemic steroids, and magnesium sulfate in emergency cases. 2 Here, we describe a case of a 38 years old male who presented with a severe asthmatic attack resistant to conventional therapy of bronchodilators and corticosteroids. Subsequently, the patient was started on noninvasive ventilator support; he could not tolerate it and was intubated. Later the patient had a good recovery after managing with an anesthetic inhalation agent sevoflurane and mechanical ventilator support by using an anesthesia machine. This case report highlights the potential management of severe acute asthma in the critical care unit with sevoflurane.
2. CASE PRESENTATION
A 38‐year‐old man with a background of bronchial asthma presented to the Emergency Department with a 2‐day history of progressive shortness of breath following cold exposure. He was on a regular metered‐dose inhaler of Salbutamol 100 μg, one puff Q6hrly at home. He mentioned having a mild cough and audible wheezes before admission but no associated fever, rhinorrhea, cough, or upper respiratory tract symptoms. He was compliant with his medications. The patient had a recent admission with a severe asthma attack treated with intravenous corticosteroids with Hydrocortisone 200 mg three times daily, nebulizer therapy Budesonide 500 μg BID, Salbutamol 2.5 mg Q8hrly, Ipratropium bromide 125 μg QID 2 days before this admission. He was discharged home with a salbutamol inhaler, one puff Q6H, and a Budesonide inhaler 500 μg two puff BID. On day two of discharge, the patient was readmitted with complaints of cough and audible wheezes. On clinical assessment, he was oriented but was unable to complete entire sentences. He was using accessory muscles for breathing. Vitally, he had tachypnea of 35 breaths/min, oxygen saturation of 99% on 10 L of the nonrebreather oxygen mask, tachycardia of 145 beats/min, and blood pressure of 145/91 mmHg, and an oral temperature of 37.3°C. His chest XR is shown in Figure 1A and was unremarkable for any pulmonary infiltrates, pneumothorax, pleural effusion, or pathology. Initial ECG was also unremarkable, as mentioned in Figure 2 . Initial arterial blood gas revealed respiratory acidosis, pH 7.314, PCO 2 72 mmHg, PO 2 132 mmHg and the bicarbonate level 32 mEq/L. Salbutamol 2.5 mg Q2hrly and Ipratropium bromide 125 μg Q2hrly nebs were given immediately.

(A) Before intubation and (B) after intubation

Unremarkable ECG
Nevertheless, the patient kept deteriorating clinically. He was given 4 g of magnesium sulfate along with a trial of noninvasive ventilation (NIV) with the settings of ST (spontaneous timed) mode, PS (pressure support) 12, PEEP (positive end‐expiratory pressure) 6, and FiO 2 40%. Arterial blood gases showed worsening respiratory acidosis—pH 7.130, PCO 2 83 mmHg, PO 2 111 mmHg, and HCO 3 30 mEq/L. Due to the increased work of breathing and drowsy state of the patient, he was intubated and started on mechanical ventilation with volume‐controlled mode, and settings of tidal volume 450 ml, respiratory rate of 14 breaths/min, PEEP of 5 cm·H 2 O, and FiO 2 of 60%. Chest XR postintubation is shown in Figure 1B . The flow volume scale was not touching the baseline due to severe bronchial constriction. The metered‐dose inhaler was started with bronchodilator therapy and steroids (Salbutamol 2.5 mg Q4hrly through the endotracheal tube). Auto‐PEEP showed 4 cm·H 2 O. Settings were altered as Inspiratory (I): Expiratory (E) ratio from 1:2.5 to 1:5. Secretions were cleared with closed inline suctioning regularly. Two days later, the patient did not show any improvement. Subsequently, it was decided by the ICU team to give bronchodilator therapy through an anesthetist agent, sevoflurane, in‐between 0.5% and 2% for 48 h. After starting inhaling sevoflurane patient, the peak pressure started to come down. Presevoflurane therapy and postsevoflurane therapy pressures are summarized in Table 1 . The arterial blood gas showed an improvement in ventilation. The comparison of ABG values is also mentioned in Table 2 . The patient gradually improved and was eventually extubated without any complications.
The comparison of ventilator status from pretherapy and post‐therapy treatment with sevoflurane
| Pressures | Pretherapy | Post‐therapy |
|---|---|---|
| Ppeak | 48 cm·H O | 30 cm·H O |
| Pplat | 22 cm·H O | 23 cm·H O |
| Stat. comp | 21.6 cm·H O | 26 cm·H O |
| Auto‐PEEP | 4 cm·H O | 0 |
Abbreviations: Ppeak, peak pressure; Pplat, plateau pressure; Stat. comp, static lung compliance.
The ABG values from pretherapy and postsevoflurane therapy treatment
| ABG | Pretherapy | Post‐therapy |
|---|---|---|
| pH | 7.314 | 7.443 |
| PCO | 72 mmHg | 38 mmHg |
| PO | 132 mmHg | 102 mmHg |
| HCO | 32 mEq/L | 25.9 mEq/L |
| Lactate | 0.40 | 0.40 |
Abbreviations: HCO 3 , bicarbonate; PCO 2 , partial pressure of carbon dioxide; pH, hydrogen ion; PO 2, partial pressure of oxygen.
3. DISCUSSION
Severe bronchial asthma can be life‐threatening if not timely managed. However, patient response varies even on a standard guideline treatment. Ng et al. 3 described acute asthma as a dangerous disease‐causing acute dyspnea leading to increase work of breathing. In the United States, 1.8‐million asthma attack cases visit the emergency department annually. Nearly 10 cases of death occur per day. 4 Most patients will recover with standard treatment. However, few cases reported resistant status‐asthmaticus, which responded only to sevoflurane and the standard treatment. 3 Our case describes the successful treatment of inhaled anesthesia gas in addition to standard treatment. Inhaled anesthesia gas (sevoflurane) has been shown to reduce Auto‐PEEP, bronchial constriction, and dynamic hyperinflation. 4 sevoflurane has a rapid bronchodilator effect and smooth muscle relaxant effect, easily ventilating the patient without asynchrony. sevoflurane is usually used in anesthesia to sedate the patient during a procedure; in selected cases, only using sevoflurane in critical care settings. 5 The main drawbacks of sevoflurane use are its high cost, monitoring, and scavenging of exhaled gas. With conservative anesthesia devices, the exhaled gas and sevoflurane can be filtered and reused. 2 Intravenous sedation could be reduced or discontinued during sevoflurane administration through ventilator support. 6 Soukup et al. evaluated the impact of sevoflurane during long‐term treatment of critical care unit patients, which showed high effectiveness on patient safety and reduced weaning time in comparison with standard conventional intravenous sedation concept. 7 Routine use of sevoflurane is easily feasible, effective, and safe, has a short awakening time, and has an adequate bronchodilator effect. 8 Current studies show that sevoflurane has significant bronchodilator properties and is an effective treatment option for severe acute asthma before rescue therapies. 9 The beneficial effect of sevoflurane in our case is supported by alveolar unit and distal airway dilation, which reduce distortion of the surrounding parenchyma and amount of alveolar collapse and finally reduce viscoelastic stress adaptation. sevoflurane has a rapid bronchodilator effect and muscle relaxant properties by reducing intracellular calcium in smooth muscle cells to ventilate the patient efficiently without asynchrony. 10 Despite the presence of nephrotoxic metabolites upon sevoflurane degradation, it can be considered a safe option in long‐term use and challenging intubation case scenarios. 11 , 12 This case aims to show there is an effect of sevoflurane for acute severe asthma cases treatment in addition to standard treatment.
4. CONCLUSION
Our objective is to highlight the potential of sevoflurane in the management of severe acute asthma refractory to standard management in mechanically ventilated patients. sevoflurane can be considered a lifesaving add‐on therapy to the standard treatment of severe asthma in resourceful countries. Considering endotracheal intubation should not be delayed in severe asthma to avoid fatal outcomes. Further meta‐analysis and studies are recommended to evaluate the long‐term efficacy and clinical applicability.
AUTHOR CONTRIBUTIONS
Satheesh Munusamy: Conceptualization; investigation; methodology; writing – original draft; writing – review and editing. Seyedeh Saba Nabavi Monfared: Writing – original draft; writing – review and editing. Phool Iqbal: Formal analysis; supervision; writing – original draft; writing – review and editing. Ahmed Lutfe Mohamad Abdussalam: Supervision; visualization.
FUNDING INFORMATION
This research has been funded by Qatar National Library.
CONFLICT OF INTEREST
The authors certify that they have no conflict of interest and no affiliations with or involvement in any organization or entity with any financial or nonfinancial interest in the subject matter or materials discussed in this manuscript.
ETHICAL APPROVAL
The study is conducted ethically in accordance with the World Medical Association Declaration of Helsinki.
Written informed consent was obtained from the patient to publish this report in accordance with the journal's patient consent policy.
ACKNOWLEDGMENT
Munusamy S, Monfared SSN, Iqbal P, Abdussalam ALM. Challenging case of severe acute asthma in a mechanically ventilated patient managed with sevoflurane . Clin Case Rep . 2023; 11 :e06571. doi: 10.1002/ccr3.6571 [ CrossRef ] [ Google Scholar ]
DATA AVAILABILITY STATEMENT

Pharmacy Quiz: Test Your Knowledge on Asthma
Ten quiz questions to assess your knowledge on common symptoms and treatments for asthma.
True or false: Asthma treatment options start with inhaled corticosteroids.

Empowering Women in Pharmacy as Leaders and Owners

Pharmacy Focus: World Psychedelics Day

Education on Screening for Type 1 Diabetes Can Facilitate Earlier Treatment

Pharmacy Focus: The Role of Pharmacists in Promoting Mental Health Care

Pharmacy Faces Potential Liability Exposure for Unsafe Premises

Educational Nutrition Programs Targeted at Communities Improve Diabetes Outcomes
2 Commerce Drive Cranbury, NJ 08512
609-716-7777

- Get new issue alerts Get alerts
- Submit a Manuscript
Secondary Logo
Journal logo.
Colleague's E-mail is Invalid
Your message has been successfully sent to your colleague.
Save my selection
Unilateral Sweating: A Case Study of Localized Unilateral Hyperhidrosis
Vaid, Zubin
Nanavati Max Super Speciality Hospital, LIC Colony, Suresh Colony, Vile Parle West, Mumbai, Maharashtra, India
Address for correspondence: Dr. Zubin Vaid, Nanavati Max Super Speciality Hospital, LIC Colony, Suresh Colony, Vile Parle West, Mumbai, Maharashtra – 400 056, India. E-mail: [email protected]
Localized unilateral hyperhidrosis (LUH) is a rare disorder with intense sweating in a specific area, often without common triggers. This study details a 32-year-old man with activity-induced unilateral sweating. Comprehensive tests ruled out serious conditions. This unique case adds to the limited reports of LUH in healthy individuals.
I NTRODUCTION
Sweating is a vital physiological process that helps regulate body temperature; cleanse the body of various toxins, excess nutrients, and waste; and aids in grip function by moistening the palms. However, excessive sweating, known as hyperhidrosis, can have adverse effects on an individual’s social and overall quality of life. [ 1 ] Hyperhidrosis can be classified into primary and secondary types. Primary hyperhidrosis is further divided into focal and generalized forms. Primary focal hyperhidrosis, which is the most common type, can affect specific parts of the body such as the palms, soles, armpits, and face. [ 2 ] In contrast, generalized hyperhidrosis involves increased sweating over the entire body and can also be primary or secondary, with causes such as infections, hyperthyroidism, endocrine and metabolic disturbances, neurological disorders, or drug effects. It is crucial to differentiate primary hyperhidrosis from secondary hyperhidrosis. [ 2 , 3 ]
While primary focal hyperhidrosis affects specific parts of the body, such as the palms, soles, armpits, and face and is relatively common, hyperhidrosis occurring unilaterally in localized areas on the body is rare and is referred to as localized unilateral hyperhidrosis (LUH). [ 4 , 5 ] LUH has been associated with organic disorders such as malignancies and neurological conditions, but it can also occur after trauma or without an apparent cause. [ 5 ]
C ASE P RESENTATION
The chief complaint of a 32-year-old male patient was unilateral excessive perspiration, which was significantly worsened during vigorous physical exertion. This condition was causing him significant discomfort and hindering his ability to exert himself without becoming excessively sweaty unilaterally. He was not on any medications.
During the clinical examination, it was noted that when the patient walked or engaged in physical exertion, sweating occurred only on one side of his upper body as he had aptly described. A photograph was taken after making the patient climb up and down a flight of stairs to demonstrate this phenomenon [ Figure 1 ]. The patient’s eye examination, with respect to pupils and light reflexes, was normal. No other abnormality was found on general or systemic examination.

In this patient’s evaluation, besides routine lab tests, electromyography with nerve conduction tests and an MRI of the brain with screening of the entire spine revealed no abnormalities. A CT scan of the chest also did not reveal any intrathoracic lesion.
D ISCUSSION
Unilateral localized hyperhidrosis typically affects the face and upper extremities in otherwise healthy individuals. Excessive sweating in this condition occurs in a distinct area, often triggered by heat, and sometimes exacerbated by emotional stress and gustatory stimulation. [ 6 , 7 ]
This type of hyperhidrosis has sometimes been associated with lesions involving various parts of the sympathetic nerve pathway, including conditions such as syringomyelia, intramedullary glioma, vertebral osteoma, head and spinal cord injuries, as well as structural lesions in the hypothalamus and spinal cord infarction. Sweating can occur spontaneously and may be of short duration in affected individuals. [ 8 , 9 ] There have been instances where unilateral hyperhidrosis was observed contralateral to acute cerebral infarction, possibly due to disruptions in the cortical pathway that inhibits contralateral sweating. Some experts suggest that paroxysmal unilateral hyperhidrosis could indicate a poor prognosis in stroke patients, particularly when the stroke affects both superficial and deep subcortical structures. [ 10-13 ] In addition, rare cases of unilateral hyperhidrosis have been reported as a secondary effect of bronchial carcinoma, suggesting possible neoplastic involvement of the ipsilateral sympathetic chain. In these unique cases, profuse sweating may occur even during sleep. [ 5 , 14 ]
Idiopathic unilateral localized hyperhidrosis, on the contrary, represents a complex and relatively uncommon condition that requires further research to fully understand its pathogenesis and possible mechanisms. [ 10-14 ] In this case, a 32-year-old male presented with LUH, primarily affecting one side of his upper body, particularly during strenuous physical activity. The clinical examination in this case revealed that sweating occurred exclusively on one side of the patient’s body, more so during physical exertion. This unilateral presentation is a hallmark of LUH. In cases of LUH, the affected area is typically sharply demarcated and relatively small, often no larger than 10 cm × 10 cm. [ 2 , 5 , 13 ] Our patient, however, had a large area involved, including the entire forehead, face, and right hemithorax. The area was sharply demarcated but large, which is a rarity.
LUH can easily be differentiated from primary essential hyperhidrosis, which typically presents symmetrically in areas such as palms, feet, and axillae. Secondary hyperhidrosis, caused by underlying medical conditions, should also be ruled out as it can be associated with various organic disorders, including malignancies, trauma, and neurological conditions. [ 5 , 8 , 9 , 10 , 13 , 14 ] LUH also needs to be differentiated from Harlequin syndrome, which is characterized by facial flushing (being a hallmark essential for diagnosis) along with unilateral sweating, and Ross syndrome, which is accompanied by areflexia and a tonic pupil besides hyperhidrosis. These features were distinctly absent in our patient. [ 15-17 ]
Comprehensive laboratory tests and imaging studies ruled out underlying malignancies and other abnormalities. Thus, as no cause was found, our patient fitted into the idiopathic category. While the exact cause of idiopathic LUH remains unclear, in some cases, hypertrophy of the glands on biopsy specimens has been reported, with sweat glands in other patients showing a normal histologic finding.
The therapeutic options included video-assisted thoracoscopic sympathectomy, iontophoresis, and local instillation of botulinum toxin type A. The last two treatments are free of side effects, but the resulting improvement is usually partial and transitory. Thoracic sympathectomy is the definitive treatment for localized hyperhidrosis but may have associated morbidity such as hyperpyrexia, especially when there is hypohidrosis on the other side. In this case, topical treatments such as aluminum chloride were recommended, similar to the management of essential hyperhidrosis. [ 18 , 19 ]
C ONCLUSION
Idiopathic LUH is a rare condition that requires a thorough evaluation to rule out underlying organic disorders and syndromes. Despite its rarity, LUH can significantly impact a patient’s quality of life, especially when it occurs unilaterally. Management options should be tailored to the individual patient’s needs and may include topical treatments and, in some cases, botulinum toxin therapy. Further research is needed to understand the underlying mechanisms and improve the management of this condition.
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent forms. In the form the patient(s) has/have given his/her/their consent for his/her/their images and other clinical information to be reported in the journal. The patients understand that their names and initials will not be published and due efforts will be made to conceal their identity, but anonymity cannot be guaranteed.
Financial support and sponsorship
Conflicts of interest.
There are no conflicts of interest.
R EFERENCES
Hyperhidrosis ; idiopathic hyperhidrosis ; localized unilateral hyperhidrosis ; sympathetic nerve pathway
- + Favorites
- View in Gallery
The browser you are using is no longer supported and for that reason you will not get the best experience when using our website.
You currently have JavaScript disabled in your web browser, please enable JavaScript to view our website as intended.
Lecturer clinches early career award for outstanding work in pharmacy
Dr Sion Scott, a lecturer in behavioural medicine and lead postgraduate tutor at the University of Leicester, is the winner of the 'Outstanding Pharmacy Early-Career Researcher Award' (OPERA) 2024.
The award, which is granted by the Royal Pharmaceutical Society (RPS) and The Pharmaceutical Journal, recognises early-career researchers from across pharmacy and the pharmaceutical sciences who demonstrate potential to achieve world-leading status.
An intervention he developed during his PhD is now being trialled as part of the ‘ Comprehensive Geriatrician-led Medication Review ’ (CHARMER) research project, which involves 22,000 patients in 24 hospitals across England, for which he is co-investigator and programme manager.
Dr Scott has also developed behaviour change interventions that are already influencing government policy and being adopted nationally, with recommendations from his deprescribing research embedded in the government’s response to the 2021 National Overprescribing Review .
His many achievements also include the co-development of the Medicine Acceptability Questionnaire (MAQ) , which is now being used in phase III studies by pharmaceutical companies to evaluate their new medicines.
In addition, he has also applied behavioural science to establish the determinants required for prescribers and patients to switch to liquid formulations of medicines used to treat Parkinson’s disease where swallowing difficulties are experienced. This research also identified opportunities to improve disease control through microdose changes, with Scott’s recommendations prompting industry to develop new microdosing devices.
The impact of Dr Scott's research extends beyond the UK. An implementation framework for deprescribing interventions in hospitals has been cited more than 60 times, with a group in Switzerland using it to design their own hospital deprescribing intervention and another in Australia adapting it for the primary care system. In 2022, he also helped convene the first international deprescribing conference in Kolding, Denmark, which drew attendees from across the globe and is scheduled to convene again later in 2024 in France.
He said: “I am delighted to have been recognised by my professional body, the RPS, for the contribution that my research is making to the advancement of the science of medicines and clinical pharmacy. The 2024 ‘OPERA’ prize recognises the importance of applying behavioural science to address medicines optimisation challenges and is a culmination of a portfolio of collaborative projects both here in the UK and internationally.”
Judging panel member Amira Guirguis, MPharm programme director at Swansea University Medical School and chair of the RPS Science and Research Committee, said: "We are thrilled to commend Sion Scott as the winner of OPERA. This prestigious award celebrates his remarkable contributions to the advancement of the science of medicines and clinical pharmacy.
“Sion's research has had a profound impact on the field of pharmacy, particularly through the development of recommendations for the NHS implementation strategy for an AI-powered medicines sourcing platform and contributions to the National Overprescribing Review. His work on deprescribing policy has been embedded in national and regional NHS responses, demonstrating the translational and applicable nature of his research.”
Professor David Wright, Head of the School of Healthcare at the University of Leicester, added: “I am absolutely delighted for Sion. Pharmacy is a very research focused profession and to win this award is incredibly impressive, although it is nothing less than Sion deserves. Since he joined academia he has gone from strength to strength. building an incredibly impressive CV over a very short period of time.”
- Awards and prizes
- Human health
Related stories
A global project to help those suffering from chronic lung disease could help millions, say experts, leicester professor receives king’s honour for services to healthcare, pioneering centre is making a difference one year after officially opening, vascular patients wanted to help shape future of research, uk first as new nhs study of digital ‘smart inhalers’ for children with asthma starts in leicester, university of leicester heart research receives £7 million funding boost.
As big pharma exits Nigeria, asthma patients face spiralling costs
The price of asthma inhalers has more than doubled amid scarcity and added costs after GSK exited the Nigerian market in 2023.

Ibadan, Nigeria — When Gloria Mofifoluwa’s friend informed her in March that the price of inhalers had risen in Nigeria, she did not think much about it.
The following week, when she went out in Ibadan city to replace her old Ventolin inhaler, the asthma sufferer was shocked to see that many pharmacies were out of stock and the only place it was available sold it for 7,500 naira ($5) – more than double the 2,800 naira ($1.86) she had paid months before.
Keep reading
Could therapy horses be the solution to britain’s prison crisis, how has the medical gender gap been affecting women’s health, immigration, economy, wars: key issues at the heart of uk general election, world leaders launch programme to boost vaccine production in africa.
This price jump – which followed the departure from Nigeria of a major health pharmaceutical – was a shock for the 24-year-old undergraduate student who earns a bit of money designing clothes. And the ripple effects were even worse.
Last month, while alone in her room at the university hostel and consumed by thoughts of her economic challenges, Mofifoluwa started hyperventilating and struggled to catch her breath.
Her roommate was away and there was no one to take her to hospital. All she had on her was an Aeroline inhaler, which she explained does not work as fast for her as the Ventolin she now struggles to get.
“I was just scared because not only was I alone in my room, I was also on my floor [and without the medicine I most needed],” she told Al Jazeera, adding that all she could do was pray until she fell asleep, hoping she would regain her strength by the time she woke up.

The pharmaceutical scarcity and rising prices causing stress for asthma sufferers like Mofifoluwa cap off a chain of events that began in May 2023, when Bola Tinubu was elected president.
During his inauguration ceremony, Tinubu announced the removal of a fuel subsidy , which resulted in an unprecedented increase in petrol prices. This also affected the cost of various goods and services and contributed to an inflation rate of above 27 percent. The cumulative economic effects have been harsh, especially for the vulnerable – including students and low-income earners.
The hardships worsened as the president’s monetary policies pushed the naira to an all-time low against the United States dollar, further leading to a downward trend as manufacturers struggled to meet production targets.
Amid the downturn – which included exchange rate volatility, declining revenues and a general worsening of the investment climate in Nigeria – a significant number of businesses including international pharmaceuticals exited the country.
Among those that left was British company GlaxoSmithKline (GSK), which ceased direct business in Nigeria in August 2023 and transitioned to a third-party distribution model. The company had operated in the Nigerian market since 1972.
“We believe the move to a third-party distribution model, a strategy we’ve successfully implemented in other markets, will enable more sustainable access to our medicines and vaccines for patients in Nigeria in line with our global strategy,” said GSK spokesperson Dan Smith.
However, Nigerian doctors and patients Al Jazeera spoke to said GSK’s departure has contributed to rising prices and increased the scarcity of some medicines. As a major supplier of inhalers – including the type Mofifoluwa depended on – the company’s exit has not been good news for asthma patients.
According to the World Health Organization (WHO), asthma cannot be cured but common treatments like the usage of inhalers which deliver medication to the lungs allow patients to live normal, active lives.
The global health body recommends that people with asthma get access to proper healthcare, but in developing countries like Nigeria, the situation is complicated. This has been worsened by the exit of companies like GSK.

While asthma inhalers were easily available and more affordable when the company was around, many now find the medication is out of reach. Despite there being alternative options, Nigeria relies largely on imported medicines, meaning high operational costs get added to the price tag for consumers.
For the average patient, an inhaler lasts about two months, depending on usage, which makes it a pricey regular cost in a country where the minimum monthly wage is 30,000 naira (about $20).
Like Mofifoluwa, 21-year-old Joseph Biyi also struggles with asthma. The library, archival and information science student was diagnosed in the middle of last year, and has since been confronted with the rising prices of inhalers.
The first time he bought a Ventolin inhaler, it sold at 3,500 naira ($2.30) but by his next visit to the pharmacy this year, the price had jumped to 7,500 naira ($5).
While Biyi has his parents to help him with money for inhalers, especially since the prices have skyrocketed, he said he now also forgoes some essential items, like groceries, to save the extra money for medicine, “just to avoid risk”.
High asthma rates
The Nigerian Thoracic Society says that, as of 2019, 15 million Nigerians were asthmatics while a nationwide study put the number at 13 million – one of the highest rates in Africa. With less than accurate data in Nigeria, because those in rural areas have limited access to quality healthcare or medical tracking, the number could be even higher.
On World Asthma Day in 2023 , the president of the Nigerian Society of Asthmatics, University College Hospital (UCH) Branch, Professor Olusoji Ige, said more than 10 million Nigerians have asthma and about three-quarters of them risked dying due to poor asthma control.
Mrs Tinubu, the Matron of the University of Ibadan’s Asthmatic Club who prefers to be identified only by her surname, said there are several factors responsible for asthma. However, she noted that the ill-equipped healthcare system worsens the condition over time.
Due to the poor state of the public healthcare system in Nigeria, after diagnosis, most people take charge of getting their medication themselves.

Meanwhile, in Ibadan, some enterprising young Nigerians have been trying to help fill the health gaps that exist.
Temitope Omosebi, a postgraduate psychology student, told Al Jazeera that after having an encounter with an asthma sufferer in 2023, he understood the full gravity of the condition and wanted to do something to help.
That’s when he launched the #AttackAgainstAsthma campaign at the University of Ibadan, to help at least some patients get access to interventions. The campaign helps provide various types of inhalers, including Sivobutamol, Aeroline, Ventolin and Fortide, to those who need them. Last year alone, 40 inhalers were distributed and this year, an additional 60 were disbursed for free; all were procured with funds from Omosebi himself.
“The campaign is important as it addresses self-care medication for asthmatic patients which has become highly costly in the recent time,” Omosebi said. “Our focus is specifically on varsity students – and on individuals in low socioeconomic communities hopefully soon – because of the known financial challenges among these groups of people.
“In Nigeria, the government isn’t doing anything it’s meant to do,” he added,
‘All inhalers are expensive’
Olabitan Odunola, a doctor and the lead at The Health City, a tech-enabled platform that focuses on preventive services and education, bemoaned the scarcity and cost of GSK products since the company exited the Nigerian market.
She said that especially for asthmatic patients who depended on GSK’s inhalers, the new circumstances are disturbing and even alternative medicines are out of reach for most patients.
“Across the board, all the inhalers are expensive,” Odunola said.
Patients have switched to alternatives like Longlife Pharmaceuticals which mostly sells Aeroline inhalers, to find relief. There are also other options like Symbicort inhalers, manufactured by AstraZeneca, and Fortide inhalers, distributed by Pakistani pharmaceutical company Getz Pharma. While all are recognised and available, they are also largely unaffordable.

Odunola said the limited access to these preventers could worsen healthcare outcomes for asthmatics. Since the condition is long-term, she also feared that it could lead to more deaths, especially in instances when someone has an asthmatic attack.
The poverty rate in Nigeria, according to the World Bank, was estimated at 38.9 percent in 2023, and considering the relatively high prices of inhalers, patients may even resort to unproven asthmatic treatments out of desperation, experts fear.
There is a correlation between limited access to quality healthcare services and the number of asthmatic patients in Nigeria, said Bello Wada, a physician and the current public health rirector of the State Ministry of Health in Kano.
“This leads to delayed diagnosis, inadequate treatment and poor management of asthma, exacerbating the condition and increasing the number of patients,” he said.
Wada also pointed out that GSK leaving Nigeria further puts those who have been diagnosed at a disadvantage, as inaccessibly priced inhalers could lead to increased morbidity and mortality rates.
Finding solutions
In January, the value of drugs imported into Nigeria was estimated at 900 billion naira ($606m), showing a high dependency on imported medicines.
In February, the federal government announced a $240m investment in the local manufacturing of pharmaceuticals, but while this is yet to materialise, Wada wants the government to do more to address the situation.
“They need to implement policies to make essential medicines more affordable, increase funding for healthcare infrastructure and personnel, develop programmes to improve access to quality healthcare services, especially for vulnerable populations, and also engage with international organisations to secure donations or discounted prices for essential medicines,” he stressed.

Nigeria’s Coordinating Minister of Health and Social Welfare, Professor Muhammad Pate, met with representatives and chief executive officers of pharmaceutical companies in Nigeria last year and said the government is concerned about the high cost of medicines and finding solutions to the crisis.
“The Federal Ministry of Health & Social Welfare, @Fmohnigeria, is working towards policy actions that may address the high prices of medicines especially for the most vulnerable Nigerians,” he said on the social platform X in November.
Until that happens, to help her asthma and manage costs, Mofifoluwa said she will continue to use Aeroline, which at 6,500 naira ($4.30) is slightly cheaper than Ventolin. Even though it does not work as well for her, she feels the lower price makes a difference and allows her supplies to last longer.
“I normally don’t use Aeroline because Ventolin works faster. I had to start buying because it’s less costly,” she told Al Jazeera. “But I still have to manage when I buy it and use it based on calculation [and only when necessary].
“During examinations period, I consume a lot because anxiety and stress are all over me,” she added.
Now, with the high cost of essential medicine she needs, school is not the only thing adding to her stress.
An official website of the United States government
The .gov means it’s official. Federal government websites often end in .gov or .mil. Before sharing sensitive information, make sure you’re on a federal government site.
The site is secure. The https:// ensures that you are connecting to the official website and that any information you provide is encrypted and transmitted securely.
- Publications
- Account settings
- My Bibliography
- Collections
- Citation manager
Save citation to file
Email citation, add to collections.
- Create a new collection
- Add to an existing collection
Add to My Bibliography
Your saved search, create a file for external citation management software, your rss feed.
- Search in PubMed
- Search in NLM Catalog
- Add to Search
Factors Associated with Chronic Obstructive Pulmonary Disease: A Hospital-Based Case-Control Study
Affiliations.
- 1 Department of Internal Medicine, Mbarara University of Science and Technology, Mbarara, Uganda.
- 2 Science Department, Phillips Academy, Andover, MA, USA.
- 3 Department of Public Health, Kabale University, Kabale, Uganda.
- 4 Division of Pulmonary and Critical Care Medicine, Massachusetts General Hospital, Boston, MA, USA.
- 5 Department of Environmental Health, Harvard T.H. Chan School of Public Health, Boston, MA, USA.
- PMID: 38022824
- PMCID: PMC10644879
- DOI: 10.2147/COPD.S426928
Purpose: Chronic obstructive pulmonary disease (COPD) is a leading cause of morbidity and mortality worldwide. In this paper, we determined risk factors for COPD among patients presenting to pulmonology and medical outpatients' clinics of Mbarara Regional Referral Hospital (MRRH).
Methods: In this case-control study, cases were patients with COPD confirmed by spirometry and controls were those with normal spirometry. The two groups were matched by age and gender.
Results: We enrolled 123 participants, of whom 41 were cases and 82 controls. A total of 51 women (41.5%) and 72 men (58.5%), of whom 25 were male cases (61%) and 47 were male controls (57%), were included. The results of our study suggest that the variables associated with the presence of COPD among participants attending MRRH were a history of having ever smoked and a prior history of atopy. This brings to our attention the fact that smoking remains a major risk factor for COPD in this setting, just as it is in developed countries.
Conclusion: Our study has shown that the factors associated with COPD are smoking and a history of atopy. Patients with a history of asthma and tuberculosis are also probably more likely to develop COPD than those without similar disease conditions.
Keywords: asthma; chronic bronchitis; emphysema; smoking.
© 2023 Twinamasiko et al.
PubMed Disclaimer
Conflict of interest statement
The authors declare that they have no competing interests.
Similar articles
- Chronic obstructive pulmonary disease with mild airflow limitation: current knowledge and proposal for future research - a consensus document from six scientific societies. Rossi A, Butorac-Petanjek B, Chilosi M, Cosío BG, Flezar M, Koulouris N, Marin J, Miculinic N, Polese G, Samaržija M, Skrgat S, Vassilakopoulos T, Vukić-Dugac A, Zakynthinos S, Miravitlles M. Rossi A, et al. Int J Chron Obstruct Pulmon Dis. 2017 Aug 29;12:2593-2610. doi: 10.2147/COPD.S132236. eCollection 2017. Int J Chron Obstruct Pulmon Dis. 2017. PMID: 28919728 Free PMC article. Review.
- The objective evaluation of obstructive pulmonary diseases with spirometry. Ozkaya S, Dirican A, Tuna T. Ozkaya S, et al. Int J Chron Obstruct Pulmon Dis. 2016 Aug 25;11:2009-15. doi: 10.2147/COPD.S113774. eCollection 2016. Int J Chron Obstruct Pulmon Dis. 2016. PMID: 27616884 Free PMC article.
- Prevalence of chronic obstructive pulmonary disease among adult male cigarettes smokers: a community-based study in Jordan. Al Omari M, Khassawneh BY, Khader Y, Dauod AS, Bergus G. Al Omari M, et al. Int J Chron Obstruct Pulmon Dis. 2014 Jul 17;9:753-8. doi: 10.2147/COPD.S62898. eCollection 2014. Int J Chron Obstruct Pulmon Dis. 2014. PMID: 25092972 Free PMC article.
- The prevalence of chronic obstructive pulmonary disease in Uppsala, Sweden--the Burden of Obstructive Lung Disease (BOLD) study: cross-sectional population-based study. Danielsson P, Ólafsdóttir IS, Benediktsdóttir B, Gíslason T, Janson C. Danielsson P, et al. Clin Respir J. 2012 Apr;6(2):120-7. doi: 10.1111/j.1752-699X.2011.00257.x. Epub 2011 Jul 6. Clin Respir J. 2012. PMID: 21651748
- Postoperative outcome after coronary artery bypass grafting in chronic obstructive pulmonary disease. Manganas H, Lacasse Y, Bourgeois S, Perron J, Dagenais F, Maltais F. Manganas H, et al. Can Respir J. 2007 Jan-Feb;14(1):19-24. doi: 10.1155/2007/378963. Can Respir J. 2007. PMID: 17315054 Free PMC article.
- Hogea SP, Tudorache E, Fildan AP, Fira-Mladinescu O, Marc M, Oancea C. Risk factors of chronic obstructive pulmonary disease exacerbations. Clin Respir J. 2020;14(3):183–197. PMID: 31814260. doi:10.1111/drj.13129 - DOI - PubMed
- Eisner MD, Anthonisen N, Coultas D, et al. An official American Thoracic Society public policy statement: Novel risk factors and the global burden of chronic obstructive pulmonary disease.Am J Respir Crit Care Med. 2010, 182(5):693–718. doi:10.1164/rccm.200811-1757ST - DOI - PubMed
- Richter DC, Joubert JR, Nell H, Schuurmans MM, Irusen EM. Diagnostic value of post-bronchodilator pulmonary function testing to distinguish between stable, moderate to severe COPD and asthma. Int J Chron Obstruct Pulmon Dis. 2008;3(4):693–699. doi:10.2147/copd.s948 - DOI - PMC - PubMed
- Labaki WW, Rosenberg SR. Chronic obstructive pulmonary disease. Ann Intern Med. 2020;173(3):ITC17–ITC32. PMID:32745458. doi:10.7326/AITC202008040 - DOI - PubMed
- Vogelmeier CF, Criner GJ, Martinez FJ, et al. Global strategy for the diagnosis, management, and prevention of chronic obstructive lung disease 2017 report. GOLD Executive Summary. Am J Respir Crit Care Med. 2017;195(5):557–582. PMID: 28128970. doi:10.1164/rccm.201701-0218PP - DOI - PubMed
- Search in MeSH
Related information
Grants and funding, linkout - more resources, full text sources.
- Dove Medical Press
- Europe PubMed Central
- PubMed Central
- Genetic Alliance
- MedlinePlus Health Information

- Citation Manager
NCBI Literature Resources
MeSH PMC Bookshelf Disclaimer
The PubMed wordmark and PubMed logo are registered trademarks of the U.S. Department of Health and Human Services (HHS). Unauthorized use of these marks is strictly prohibited.
- Alzheimer's disease & dementia
- Arthritis & Rheumatism
- Attention deficit disorders
- Autism spectrum disorders
- Biomedical technology
- Diseases, Conditions, Syndromes
- Endocrinology & Metabolism
- Gastroenterology
- Gerontology & Geriatrics
- Health informatics
- Inflammatory disorders
- Medical economics
- Medical research
- Medications
- Neuroscience
- Obstetrics & gynaecology
- Oncology & Cancer
- Ophthalmology
- Overweight & Obesity
- Parkinson's & Movement disorders
- Psychology & Psychiatry
- Radiology & Imaging
- Sleep disorders
- Sports medicine & Kinesiology
- Vaccination
- Breast cancer
- Cardiovascular disease
- Chronic obstructive pulmonary disease
- Colon cancer
- Coronary artery disease
- Heart attack
- Heart disease
- High blood pressure
- Kidney disease
- Lung cancer
- Multiple sclerosis
- Myocardial infarction
- Ovarian cancer
- Post traumatic stress disorder
- Rheumatoid arthritis
- Schizophrenia
- Skin cancer
- Type 2 diabetes
- Full List »
share this!
June 24, 2024
This article has been reviewed according to Science X's editorial process and policies . Editors have highlighted the following attributes while ensuring the content's credibility:
fact-checked
peer-reviewed publication
trusted source
New study finds medication abortion without ultrasound to be safe
by University of California, San Francisco

Researchers compared patients who received care remotely to those who got ultrasounds and found no differences in outcomes. Medication abortion patients who receive pills by mail without first getting an ultrasound do just as well as those who are examined and given the drugs in person, new research from UC San Francisco has found.
The study, which appears June 24 in JAMA , adds to evidence from UCSF's Advancing New Standards in Reproductive Health (ANSIRH) program that using telehealth for medication abortion is safe and effective.
Although the Supreme Court recently upheld the Food and Drug Administration (FDA) guidelines that permit remote prescribing and delivery of medication abortion, it was a narrow ruling based on the plaintiffs not having the standing to sue.
These guidelines have enabled the provision of medication abortion via telehealth, which has improved access to care in recent years. More legal challenges to medication abortion are expected in the wake of the narrow ruling.
After the high court ended the constitutional right to abortion in 2022, a growing number of states enacted restrictions; and medication abortion now accounts for about two-thirds of all abortions in the U.S. health care system.
"This study adds to a growing and robust body of evidence demonstrating the effectiveness and safety of medication abortion with telehealth and mailing medications," said Lauren J. Ralph, Ph.D., MPH, an associate professor of obstetrics, gynecology and reproductive sciences at UCSF and first author of the study.
"Patient history-based models of medication abortion care without ultrasound and via telehealth offer a safe, effective and urgently needed way to overcome logistical and geographic obstacles to accessing abortion today," she said.
Testing the 'no test' method
The researchers analyzed the experiences of 585 patients at clinics in Colorado, Illinois, Maryland, Minnesota, Virginia and Washington from May 2021 to March 2023, dividing them into three groups.
The first were evaluated for eligibility for medication abortion using telehealth. They underwent a patient history-based screening without ultrasound, also known as the "no-test" method, and received their medication by mail (288 patients). The second were assessed using the "no-test" method and received their medication in person (119 patients). And the third underwent an ultrasound and got their medication in person (238 patients).
All participants took the two-drug regimen of mifepristone, which blocks progesterone, a hormone that is needed to continue pregnancy, and misoprostol, which is used one to two days later to bring on contractions. The safety of mifepristone, the only drug approved by the Food and Drug Administration (FDA) specifically for medication abortion, has been at the center of the Supreme Court case.
The researchers found that 95% of the participants had a complete abortion without having to repeat the regimen, and the telehealth patients did as well as those who received in-person care. Serious adverse events were rare regardless of the group.
Medication abortion is approved for use in people up to 10 weeks (70 days) of pregnancy. And Ralph said patients can report enough information about their history to assess how far along they are in pregnancy without an ultrasound.
"These models of care that rely on no-test telehealth screening and mailing medications are as effective as in-person care with ultrasound and should be offered to all pregnant people," she said.
Research confirms that restrictions were not necessary
The recent Supreme Court case sought to roll back guidelines that have made the medication more widely available, including the FDA's removal in 2021 of a requirement that mifepristone be dispensed in person at a clinic or doctor's office.
In February, UCSF researchers showed that medication abortion can be delivered safely and effectively through telehealth . And in May, they published a study that found dispensing the pills through the mail works as well as requiring patients to pick them up in person.
"The science is clear that telehealth evaluation and pharmacy dispensing of abortion pills is safe and effective," said ANSIRH's director, Daniel Grossman, MD, a UCSF professor of obstetrics, gynecology and reproductive sciences and senior author of the latest study. "Any attempt to restrict it is not based on science."
Explore further
Feedback to editors

Chronic loneliness may increase stroke risk among older adults
46 minutes ago

Scientists can now detect antibiotics in fingerprints, aiding the fight against drug-resistant TB

Children born underweight found to be at increased risk of disease if they develop obesity

Wearable sweat monitor uses machine learning to protect workers from dehydration
4 hours ago

Signaling pathway in brain helps maintain balance in microglia, prevent cognitive deficit

New research points to possibility for testing to explore early-stage Alzheimer's disease
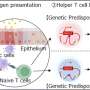
Study elucidates crucial role of G900 gene enhancers in asthma-associated inflammation
5 hours ago

Texas's 2021 abortion ban tied to rise in infant deaths
Study reveals same genes that can drive cancer also guide neural-circuit growth
7 hours ago

New evidence shows that higher oxygen concentrations may help prevent deaths of preterm babies
Related stories.

Sending abortion pills through the mail found to be timely and effective
May 13, 2024

Large study finds telehealth is as safe as a visit to the clinic for abortion pills
Feb 15, 2024

Use of abortion pill grows in US, despite threat of new restrictions
Mar 19, 2024

Abortion pill at the center of a US court battle
Dec 13, 2023

Telehealth makes timely abortions possible for many, research shows
Jan 31, 2024

FDA allows abortion pill to stay available by mail
Dec 17, 2021
Recommended for you
Fertility treatments could get a boost from stem cells

Trial offers hope for cheaper, more tolerable, ketamine treatment
9 hours ago

Q&A: How future medications could be personalized on a 3D printer
New approach accurately identifies medications most toxic to the liver
Common blood pressure drug may increase risk of bleeding
Jun 21, 2024
Let us know if there is a problem with our content
Use this form if you have come across a typo, inaccuracy or would like to send an edit request for the content on this page. For general inquiries, please use our contact form . For general feedback, use the public comments section below (please adhere to guidelines ).
Please select the most appropriate category to facilitate processing of your request
Thank you for taking time to provide your feedback to the editors.
Your feedback is important to us. However, we do not guarantee individual replies due to the high volume of messages.
E-mail the story
Your email address is used only to let the recipient know who sent the email. Neither your address nor the recipient's address will be used for any other purpose. The information you enter will appear in your e-mail message and is not retained by Medical Xpress in any form.
Newsletter sign up
Get weekly and/or daily updates delivered to your inbox. You can unsubscribe at any time and we'll never share your details to third parties.
More information Privacy policy
Donate and enjoy an ad-free experience
We keep our content available to everyone. Consider supporting Science X's mission by getting a premium account.
E-mail newsletter
Information
- Author Services
Initiatives
You are accessing a machine-readable page. In order to be human-readable, please install an RSS reader.
All articles published by MDPI are made immediately available worldwide under an open access license. No special permission is required to reuse all or part of the article published by MDPI, including figures and tables. For articles published under an open access Creative Common CC BY license, any part of the article may be reused without permission provided that the original article is clearly cited. For more information, please refer to https://www.mdpi.com/openaccess .
Feature papers represent the most advanced research with significant potential for high impact in the field. A Feature Paper should be a substantial original Article that involves several techniques or approaches, provides an outlook for future research directions and describes possible research applications.
Feature papers are submitted upon individual invitation or recommendation by the scientific editors and must receive positive feedback from the reviewers.
Editor’s Choice articles are based on recommendations by the scientific editors of MDPI journals from around the world. Editors select a small number of articles recently published in the journal that they believe will be particularly interesting to readers, or important in the respective research area. The aim is to provide a snapshot of some of the most exciting work published in the various research areas of the journal.
Original Submission Date Received: .
- Active Journals
- Find a Journal
- Proceedings Series
- For Authors
- For Reviewers
- For Editors
- For Librarians
- For Publishers
- For Societies
- For Conference Organizers
- Open Access Policy
- Institutional Open Access Program
- Special Issues Guidelines
- Editorial Process
- Research and Publication Ethics
- Article Processing Charges
- Testimonials
- Preprints.org
- SciProfiles
- Encyclopedia

Article Menu

- Subscribe SciFeed
- Recommended Articles
- Google Scholar
- on Google Scholar
- Table of Contents
Find support for a specific problem in the support section of our website.
Please let us know what you think of our products and services.
Visit our dedicated information section to learn more about MDPI.
JSmol Viewer
Spatial analysis of intra-urban air pollution disparities through an environmental justice lens: a case study of philadelphia, pa.

Share and Cite
Scolio, M.; Borha, C.; Kremer, P.; Shakya, K.M. Spatial Analysis of Intra-Urban Air Pollution Disparities through an Environmental Justice Lens: A Case Study of Philadelphia, PA. Atmosphere 2024 , 15 , 755. https://doi.org/10.3390/atmos15070755
Scolio M, Borha C, Kremer P, Shakya KM. Spatial Analysis of Intra-Urban Air Pollution Disparities through an Environmental Justice Lens: A Case Study of Philadelphia, PA. Atmosphere . 2024; 15(7):755. https://doi.org/10.3390/atmos15070755
Scolio, Madeline, Charlotte Borha, Peleg Kremer, and Kabindra M. Shakya. 2024. "Spatial Analysis of Intra-Urban Air Pollution Disparities through an Environmental Justice Lens: A Case Study of Philadelphia, PA" Atmosphere 15, no. 7: 755. https://doi.org/10.3390/atmos15070755
Article Metrics
Article access statistics, supplementary material.
ZIP-Document (ZIP, 423 KiB)
Further Information
Mdpi initiatives, follow mdpi.

Subscribe to receive issue release notifications and newsletters from MDPI journals

COMMENTS
Introduction. Asthma, one of the most common chronic diseases, poses a substantial socioeconomic burden on both patients and caregivers. 1 Asthma affects people of all ages, including children, with a considerable negative impact on both school and work performance. In 2017, an estimated 25.2 million people, including 6.2 million children, had asthma in the United States. 2 Furthermore ...
Pharmacy Times offers the latest news and insights for the pharmacy professional and solutions that impact the everyday practice of pharmacy. ... CASE TWO. Moderate Persistent Asthma. CC is a 17-year-old teenager previously diagnosed with intermittent asthma (infrequent symptoms, usually occurring twice weekly at most) who complains to his ...
Uncontrolled asthma has negative effects on clinical, humanistic, and economic outcomes.The Task Force on Community Preventative Services, a volunteer group of preventative and public health-care experts appointed by the director of the CDC, has recommended an educational and interventional approach to asthma care that has demonstrated an increase in symptom-free days and in cost avoidance.
Learning outcomes Level 1 case study: You will be able to: describe the risk factors describe the disease describe the pharmacology of the drug outline the formulations available, including drug molecule, excipients, etc. for the medicines summarise basic social pharmacy issues (e.g. opening containers, large labels). Scenario An 18-year-old man, VB, presents with a history of recurrent ...
CASE STUDY. A 14-year-old girl with a history of asthma requiring daily inhaled corticosteroid therapy and allergies to house dust mites, cats, grasses, and ragweed presents to the emergency department in mid-September, reporting a recent "cold" complicated by worsening shortness of breath and audible inspiratory and expiratory wheezing.
Pharmacists could be involved in the provision of community pharmacy-based asthma interventions that involve more than inhaler technique education. ... patients registered with the GP practice in the Northwest of England whose medical records were reviewed in a previous study (case note review of patients' medical records) 70 and consented to ...
Primary Care Respiratory Society. Charity Number 1098117 Company Number 4298947 VAT Registration Number 866 1543 09 Registered office Miria House, 1683b High Street, Knowle, B93 0LL Telephone +44 (0)1675 477600 Email [email protected] Website https://www.pcrs-uk.org.
Case-based questions related to asthma also regularly appeared on examinations throughout Pathophysiology and the Integrated Sequence. Within the Integrated Sequence block at South University, there was a built-in 3-hour weekly recitation that could be used for formal case study. During this recitation, students were broken into small groups of ...
In one study of pharmacy database medication refills of a combination of an inhaled corticosteroid and a long-acting beta-agonist in a single device, approximately 22% adherence over the course of ...
Supported self-management reduces asthma morbidity. The lady in this case study is struggling to maintain control of her asthma within the context of her busy professional and domestic life.
The majority of adverse effects occurred within 1 day of the procedure and resolved within 7 days. 6. In this study, bronchial thermoplasty was found to significantly improve quality of life, as ...
Chronic asthma. History of recurrent episodes of coughing, wheezing, chest tightness, or shortness of breath and confirmatory spirometry. May be family history of allergy or asthma, or patient symptoms of allergic rhinitis. History of exercise or cold air precipitating symptoms during specific allergen seasons. Acute severe asthma.
Clinical case study - asthma . 2019 . Clinical Case Study - Asthma. pdf. Clinical Case Study - Asthma. 6.34 MB. Resource information. Respiratory conditions. Asthma; Respiratory topics. Disease management; Diagnosis; Type of resource. Presentation . Author(s) Jaime Correia de Sousa Ioanna Tsiligianni Miguel Román Rodriguez
Pharmacy Times July 2017 Digestive Health. Volume 83. Issue 7. What should these pharmacists do? CASE 1. WB is a 57-year-old man who reports to the clinic complaining of frequent but intermittent cramping pain in his left leg induced by walking. His primary care physician performed a resting ankle-brachial index (ABI) test and found WB to have ...
Asthma is a chronic inflammatory airway disorder with acute exacerbations that currently affects approximately 14 million-15 million children and adults in the United States. Costs for asthma are staggering and nurse practitioners (NPs) are frequently presented with management decisions for the acute treatment and chronic management of this ...
c) Endocrine System Case Studies with answers: Diabetes: Case Study 17 and Case Study - 18. Hypothyroidism : Case Study -19 and Case Study -20. Other Thyroid Disorders : Case Study -21 and Case Study -22. Oral Contraceptive Use: Case Study- 23 and Case Study- 24. Hormone Replacement Therapy: Case Study- 25 and Case Study- 26.
Importantly, lung aging occurs over the course of life. 2 In a cross-sectional study of patients enrolled in NHLBI-SARP, the risk of severe asthma increased by 7% each year until age 45. 2 Asthma ...
Quick-Relief Medication for All Patients: SABA as needed for symptoms. Intensity of treatment depends on severity of symptoms: up to 3 treatments at 20-minute intervals as needed. Short course of systemic oral corticosteroids may be needed. Caution: Increasing of b-agonist or use >2x/week for symptoms control indicates.
Jane Doe #1. 49 year old female. History of heavy tobacco use and asthma. Patient has been feeling somewhat poorly over the last few weeks and her roommate reports that she has been using her nebulizers quite heavily -despite this, she also has continued to smoke quite heavily. The patient's roommate said that the patient was in her room and ...
1. INTRODUCTION. Acute severe asthma is a life‐threatening emergency characterized by severe tachypnea, tachycardia, and type 1 respiratory failure. 1 According to the international standard guidelines, it is managed with bronchodilators, systemic steroids, and magnesium sulfate in emergency cases. 2 Here, we describe a case of a 38 years old male who presented with a severe asthmatic attack ...
Asthma 2023 case studies. ... Course. case study for pharmacy (CPP 6101) 9 Documents. Students shared 9 documents in this course. University St. John's University. Academic year: 2023/2024. Uploaded by: Anonymous Student. This document has been uploaded by a student, just like you, who decided to remain anonymous.
Pharmacy Quiz: Test Your Knowledge on Asthma. October 27, 2021. Saro Arakelians, PharmD. Article. Ten quiz questions to assess your knowledge on common symptoms and treatments for asthma. True or false: Asthma treatment options start with inhaled corticosteroids. True. False.
This case study describes a 19-year-old university student named Miss GN who has had asthma since age 7. She was using her salbutamol inhaler frequently and was referred by her pharmacist to her doctor. Her doctor prescribed her an inhaled corticosteroid in addition to her rescue inhaler. However, she continued having symptoms and using her rescue inhaler frequently. The pharmacist then ...
Localized unilateral hyperhidrosis (LUH) is a rare disorder with intense sweating in a specific area, often without common triggers. This study details a 32-year-old man with activity-induced unilateral sweating. Comprehensive tests ruled out serious conditions. This unique case adds to the limited reports of LUH in healthy individuals.
"Sion's research has had a profound impact on the field of pharmacy, particularly through the development of recommendations for the NHS implementation strategy for an AI-powered medicines sourcing platform and contributions to the National Overprescribing Review. ... UK First as new NHS study of digital 'smart inhalers' for children with ...
Price of asthma inhalers has more than doubled amid scarcity and added costs after GSK exited Nigerian market in 2023. ... it sold at 3,500 naira ($2.30) but by his next visit to the pharmacy this ...
Patients with a history of asthma and tuberculosis are also probably more likely to develop COPD than those without similar disease conditions. ... Methods: In this case-control study, cases were patients with COPD confirmed by spirometry and controls were those with normal spirometry. The two groups were matched by age and gender.
The study, which appears June 24 in JAMA, adds to evidence from UCSF's Advancing New Standards in Reproductive Health (ANSIRH) program that using telehealth for medication abortion is safe and ...
Urban air pollution has been long understood as a critical threat to human health worldwide. Worsening urban air quality can cause increased rates of asthma, respiratory illnesses, and mortality. Air pollution is also an important environmental justice issue as it disproportionately burdens populations made vulnerable by their socioeconomic and health status. Using spatially continuous fine ...