5 moving, beautiful essays about death and dying
by Sarah Kliff

It is never easy to contemplate the end-of-life, whether its own our experience or that of a loved one.
This has made a recent swath of beautiful essays a surprise. In different publications over the past few weeks, I've stumbled upon writers who were contemplating final days. These are, no doubt, hard stories to read. I had to take breaks as I read about Paul Kalanithi's experience facing metastatic lung cancer while parenting a toddler, and was devastated as I followed Liz Lopatto's contemplations on how to give her ailing cat the best death possible. But I also learned so much from reading these essays, too, about what it means to have a good death versus a difficult endfrom those forced to grapple with the issue. These are four stories that have stood out to me recently, alongside one essay from a few years ago that sticks with me today.

My Own Life | Oliver Sacks

As recently as last month, popular author and neurologist Oliver Sacks was in great health, even swimming a mile every day. Then, everything changed: the 81-year-old was diagnosed with terminal liver cancer. In a beautiful op-ed , published in late February in the New York Times, he describes his state of mind and how he'll face his final moments. What I liked about this essay is how Sacks describes how his world view shifts as he sees his time on earth getting shorter, and how he thinks about the value of his time.
Before I go | Paul Kalanithi

Kalanthi began noticing symptoms — "weight loss, fevers, night sweats, unremitting back pain, cough" — during his sixth year of residency as a neurologist at Stanford. A CT scan revealed metastatic lung cancer. Kalanthi writes about his daughter, Cady and how he "probably won't live long enough for her to have a memory of me." Much of his essay focuses on an interesting discussion of time, how it's become a double-edged sword. Each day, he sees his daughter grow older, a joy. But every day is also one that brings him closer to his likely death from cancer.
As I lay dying | Laurie Becklund

Becklund's essay was published posthumonously after her death on February 8 of this year. One of the unique issues she grapples with is how to discuss her terminal diagnosis with others and the challenge of not becoming defined by a disease. "Who would ever sign another book contract with a dying woman?" she writes. "Or remember Laurie Becklund, valedictorian, Fulbright scholar, former Times staff writer who exposed the Salvadoran death squads and helped The Times win a Pulitzer Prize for coverage of the 1992 L.A. riots? More important, and more honest, who would ever again look at me just as Laurie?"
Everything I know about a good death I learned from my cat | Liz Lopatto

Dorothy Parker was Lopatto's cat, a stray adopted from a local vet. And Dorothy Parker, known mostly as Dottie, died peacefullywhen she passed away earlier this month. Lopatto's essay is, in part, about what she learned about end-of-life care for humans from her cat. But perhaps more than that, it's also about the limitations of how much her experience caring for a pet can transfer to caring for another person.
Yes, Lopatto's essay is about a cat rather than a human being. No, it does not make it any easier to read. She describes in searing detail about the experience of caring for another being at the end of life. "Dottie used to weigh almost 20 pounds; she now weighs six," Lopatto writes. "My vet is right about Dottie being close to death, that it’s probably a matter of weeks rather than months."
Letting Go | Atul Gawande

"Letting Go" is a beautiful, difficult true story of death. You know from the very first sentence — "Sara Thomas Monopoli was pregnant with her first child when her doctors learned that she was going to die" — that it is going to be tragic. This story has long been one of my favorite pieces of health care journalism because it grapples so starkly with the difficult realities of end-of-life care.
In the story, Monopoli is diagnosed with stage four lung cancer, a surprise for a non-smoking young woman. It's a devastating death sentence: doctors know that lung cancer that advanced is terminal. Gawande knew this too — Monpoli was his patient. But actually discussing this fact with a young patient with a newborn baby seemed impossible.
"Having any sort of discussion where you begin to say, 'look you probably only have a few months to live. How do we make the best of that time without giving up on the options that you have?' That was a conversation I wasn't ready to have," Gawande recounts of the case in a new Frontline documentary .
What's tragic about Monopoli's case was, of course, her death at an early age, in her 30s. But the tragedy that Gawande hones in on — the type of tragedy we talk about much less — is how terribly Monopoli's last days played out.
Most Popular
Stop setting your thermostat at 72, web3 is the future, or a scam, or both, what do we do about alice munro now, is kamala harris a better candidate now than she was four years ago, take a mental break with the newest vox crossword, today, explained.
Understand the world with a daily explainer plus the most compelling stories of the day.
More in Politics

What the world can learn from Indian liberalism

The arguments for Biden 2024 keep getting worse

Is it undemocratic to replace Biden on the ticket?

France’s elections showed a polarized country

The real lesson for America in the French and British elections

Why I quit Spotify

Heat is deadly. Why does our culture push us to ignore it?

What American cities could do right now to save us from this unbearable heat

Why are so many female pop stars flopping?

How do you know it’s time to retire?

Iran’s new president can only change the country so much

Presentations made painless
- Get Premium
115 Death Essay Topic Ideas & Examples
Inside This Article
Death is an inevitable part of life that has been contemplated and explored by humans throughout history. It is a subject that evokes a wide range of emotions and thoughts, from fear and sorrow to curiosity and acceptance. Writing an essay about death can be a profound and thought-provoking experience, allowing individuals to reflect on their own mortality and explore existential questions. To inspire your writing, here are 115 death essay topic ideas and examples.
- The concept of death in different cultures.
- The role of death in religious beliefs.
- The fear of death and its impact on human behavior.
- Death as a theme in literature and poetry.
- The portrayal of death in art and cinema.
- The psychology of grief and mourning.
- The stages of grief according to Elisabeth Kübler-Ross.
- How to cope with the loss of a loved one.
- The impact of death on family dynamics.
- The connection between death and existentialism.
- Near-death experiences and their implications.
- The debate between the existence of an afterlife and oblivion.
- The significance of death rituals and funeral customs.
- The ethics of euthanasia and assisted suicide.
- The right to die: exploring the concept of death with dignity.
- The role of death in philosophical thought.
- Death as a catalyst for personal growth and transformation.
- The impact of death anxiety on mental health.
- Exploring the concept of a "good death."
- The portrayal of death in popular culture.
- Death and the meaning of life.
- The portrayal of death in ancient mythology.
- Death and the concept of time.
- The impact of death on medical ethics.
- The portrayal of death in children's literature.
- The intersection of death and technology.
- Death and the fear of the unknown.
- The impact of death on social media and digital legacies.
- The acceptance of death: exploring different perspectives.
- The role of humor in coping with death.
- Death and the concept of justice.
- The impact of death on religious beliefs and practices.
- The influence of death on artistic expression.
- Death and the concept of free will.
- The portrayal of death in different historical periods.
- Death and the concept of fate.
- The impact of death on the concept of identity.
- Death and the concept of soul.
- Death and the concept of pain.
- The impact of death on medical advancements.
- Death and the concept of forgiveness.
- The portrayal of death in video games.
- Death and the concept of sacrifice.
- The impact of death on cultural traditions.
- Death and the concept of legacy.
- Death and the concept of beauty.
- The portrayal of death in religious texts.
- Death and the concept of morality.
- The impact of death on social structures.
- Death and the concept of justice in different societies.
- The portrayal of death in different artistic mediums.
- Death and the concept of love.
- The impact of death on the concept of time.
- Death and the concept of truth.
- The portrayal of death in different musical genres.
- Death and the concept of suffering.
- The impact of death on the concept of freedom.
- Death and the concept of redemption.
- The portrayal of death in different dance forms.
- Death and the concept of rebirth.
- The impact of death on the concept of beauty.
- Death and the concept of forgiveness in different cultures.
- The portrayal of death in different architectural styles.
- Death and the concept of fate in different societies.
- The impact of death on the concept of identity in different periods.
- Death and the concept of pain in different cultures.
- The portrayal of death in different fashion trends.
- Death and the concept of sacrifice in different religions.
- The impact of death on the concept of legacy in different civilizations.
- Death and the concept of beauty in different art forms.
- The portrayal of death in different culinary traditions.
- Death and the concept of justice in different historical eras.
- The impact of death on the concept of morality in different societies.
- Death and the concept of love in different cultures.
- The portrayal of death in different sports.
- Death and the concept of suffering in different religions.
- The impact of death on the concept of freedom in different periods.
- Death and the concept of redemption in different belief systems.
- The portrayal of death in different circus acts.
- Death and the concept of rebirth in different mythologies.
- The impact of death on the concept of beauty in different civilizations.
- Death and the concept of forgiveness in different cultural practices.
- The portrayal of death in different gardening styles.
- Death and the concept of fate in different belief systems.
- The impact of death on the concept of identity in different societies.
- Death and the concept of pain in different historical periods.
- The portrayal of death in different interior design trends.
- Death and the concept of sacrifice in different cultural practices.
- Death and the concept of beauty in different fashion trends.
- The portrayal of death in different music genres.
- The impact of death on the concept of morality in different periods.
- The portrayal of death in different film genres.
- The impact of death on the concept of freedom in different societies.
- The portrayal of death in different theater styles.
- The portrayal of death in different dance styles.
- The portrayal of death in different visual art forms.
- Death and the concept of beauty in different architectural styles.
- The portrayal of death in different literary genres.
Whether you choose to explore the philosophical, cultural, psychological, or artistic aspects of death, these essay topic ideas provide a wide range of possibilities to delve into this profound subject. Remember to approach the topic with sensitivity and respect, as death is a deeply personal and meaningful experience for many individuals.
Want to create a presentation now?
Instantly Create A Deck
Let PitchGrade do this for me
Hassle Free
We will create your text and designs for you. Sit back and relax while we do the work.
Explore More Content
- Privacy Policy
- Terms of Service
© 2023 Pitchgrade
- Death And Dying
8 Popular Essays About Death, Grief & the Afterlife
Updated 05/4/2022
Published 07/19/2021

Joe Oliveto, BA in English
Contributing writer

Cake values integrity and transparency. We follow a strict editorial process to provide you with the best content possible. We also may earn commission from purchases made through affiliate links. As an Amazon Associate, we earn from qualifying purchases. Learn more in our affiliate disclosure .
Death is a strange topic for many reasons, one of which is the simple fact that different people can have vastly different opinions about discussing it.
Jump ahead to these sections:
Essays or articles about the death of a loved one, essays or articles about dealing with grief, essays or articles about the afterlife or near-death experiences.
Some fear death so greatly they don’t want to talk about it at all. However, because death is a universal human experience, there are also those who believe firmly in addressing it directly. This may be more common now than ever before due to the rise of the death positive movement and mindset.
You might believe there’s something to be gained from talking and learning about death. If so, reading essays about death, grief, and even near-death experiences can potentially help you begin addressing your own death anxiety. This list of essays and articles is a good place to start. The essays here cover losing a loved one, dealing with grief, near-death experiences, and even what someone goes through when they know they’re dying.
Losing a close loved one is never an easy experience. However, these essays on the topic can help someone find some meaning or peace in their grief.
1. ‘I’m Sorry I Didn’t Respond to Your Email, My Husband Coughed to Death Two Years Ago’ by Rachel Ward
Rachel Ward’s essay about coping with the death of her husband isn’t like many essays about death. It’s very informal, packed with sarcastic humor, and uses an FAQ format. However, it earns a spot on this list due to the powerful way it describes the process of slowly finding joy in life again after losing a close loved one.
Ward’s experience is also interesting because in the years after her husband’s death, many new people came into her life unaware that she was a widow. Thus, she often had to tell these new people a story that’s painful but unavoidable. This is a common aspect of losing a loved one that not many discussions address.
2. ‘Everything I know about a good death I learned from my cat’ by Elizabeth Lopatto
Not all great essays about death need to be about human deaths! In this essay, author Elizabeth Lopatto explains how watching her beloved cat slowly die of leukemia and coordinating with her vet throughout the process helped her better understand what a “good death” looks like.
For instance, she explains how her vet provided a degree of treatment but never gave her false hope (for instance, by claiming her cat was going to beat her illness). They also worked together to make sure her cat was as comfortable as possible during the last stages of her life instead of prolonging her suffering with unnecessary treatments.
Lopatto compares this to the experiences of many people near death. Sometimes they struggle with knowing how to accept death because well-meaning doctors have given them the impression that more treatments may prolong or even save their lives, when the likelihood of them being effective is slimmer than patients may realize.
Instead, Lopatto argues that it’s important for loved ones and doctors to have honest and open conversations about death when someone’s passing is likely near. This can make it easier to prioritize their final wishes instead of filling their last days with hospital visits, uncomfortable treatments, and limited opportunities to enjoy themselves.
3. ‘The terrorist inside my husband’s brain’ by Susan Schneider Williams
This article, which Susan Schneider Williams wrote after the death of her husband Robin Willians, covers many of the topics that numerous essays about the death of a loved one cover, such as coping with life when you no longer have support from someone who offered so much of it.
However, it discusses living with someone coping with a difficult illness that you don’t fully understand, as well. The article also explains that the best way to honor loved ones who pass away after a long struggle is to work towards better understanding the illnesses that affected them.
4. ‘Before I Go’ by Paul Kalanithi
“Before I Go” is a unique essay in that it’s about the death of a loved one, written by the dying loved one. Its author, Paul Kalanithi, writes about how a terminal cancer diagnosis has changed the meaning of time for him.
Kalanithi describes believing he will die when his daughter is so young that she will likely never have any memories of him. As such, each new day brings mixed feelings. On the one hand, each day gives him a new opportunity to see his daughter grow, which brings him joy. On the other hand, he must struggle with knowing that every new day brings him closer to the day when he’ll have to leave her life.
Coping with grief can be immensely challenging. That said, as the stories in these essays illustrate, it is possible to manage grief in a positive and optimistic way.
5. Untitled by Sheryl Sandberg
This piece by Sheryl Sandberg, Facebook’s current CEO, isn’t a traditional essay or article. It’s actually a long Facebook post. However, many find it’s one of the best essays about death and grief anyone has published in recent years.
She posted it on the last day of sheloshim for her husband, a period of 30 days involving intense mourning in Judaism. In the post, Sandberg describes in very honest terms how much she learned from those 30 days of mourning, admitting that she sometimes still experiences hopelessness, but has resolved to move forward in life productively and with dignity.
She explains how she wanted her life to be “Option A,” the one she had planned with her husband. However, because that’s no longer an option, she’s decided the best way to honor her husband’s memory is to do her absolute best with “Option B.”
This metaphor actually became the title of her next book. Option B , which Sandberg co-authored with Adam Grant, a psychologist at the Wharton School of the University of Pennsylvania, is already one of the most beloved books about death , grief, and being resilient in the face of major life changes. It may strongly appeal to anyone who also appreciates essays about death as well.
6. ‘My Own Life’ by Oliver Sacks
Grief doesn’t merely involve grieving those we’ve lost. It can take the form of the grief someone feels when they know they’re going to die.
Renowned physician and author Oliver Sacks learned he had terminal cancer in 2015. In this essay, he openly admits that he fears his death. However, he also describes how knowing he is going to die soon provides a sense of clarity about what matters most. Instead of wallowing in his grief and fear, he writes about planning to make the very most of the limited time he still has.
Belief in (or at least hope for) an afterlife has been common throughout humanity for decades. Additionally, some people who have been clinically dead report actually having gone to the afterlife and experiencing it themselves.
Whether you want the comfort that comes from learning that the afterlife may indeed exist, or you simply find the topic of near-death experiences interesting, these are a couple of short articles worth checking out.
7. ‘My Experience in a Coma’ by Eben Alexander
“My Experience in a Coma” is a shortened version of the narrative Dr. Eben Alexander shared in his book, Proof of Heaven . Alexander’s near-death experience is unique, as he’s a medical doctor who believes that his experience is (as the name of his book suggests) proof that an afterlife exists. He explains how at the time he had this experience, he was clinically braindead, and therefore should not have been able to consciously experience anything.
Alexander describes the afterlife in much the same way many others who’ve had near-death experiences describe it. He describes starting out in an “unresponsive realm” before a spinning white light that brought with it a musical melody transported him to a valley of abundant plant life, crystal pools, and angelic choirs. He states he continued to move from one realm to another, each realm higher than the last, before reaching the realm where the infinite love of God (which he says is not the “god” of any particular religion) overwhelmed him.
8. “One Man's Tale of Dying—And Then Waking Up” by Paul Perry
The author of this essay recounts what he considers to be one of the strongest near-death experience stories he’s heard out of the many he’s researched and written about over the years. The story involves Dr. Rajiv Parti, who claims his near-death experience changed his views on life dramatically.
Parti was highly materialistic before his near-death experience. During it, he claims to have been given a new perspective, realizing that life is about more than what his wealth can purchase. He returned from the experience with a permanently changed outlook.
This is common among those who claim to have had near-death experiences. Often, these experiences leave them kinder, more understanding, more spiritual, and less materialistic.
This short article is a basic introduction to Parti’s story. He describes it himself in greater detail in the book Dying to Wake Up , which he co-wrote with Paul Perry, the author of the article.
Essays About Death: Discussing a Difficult Topic
It’s completely natural and understandable to have reservations about discussing death. However, because death is unavoidable, talking about it and reading essays and books about death instead of avoiding the topic altogether is something that benefits many people. Sometimes, the only way to cope with something frightening is to address it.
Categories:
- Coping With Grief
You may also like

What is a 'Good Death' in End-of-Life Care?

11 Popular Websites About Death and End of Life

18 Questions About Death to Get You Thinking About Mortality

15 Best Children’s Books About the Death of a Parent
Essays About Death: Top 5 Examples and 9 Essay Prompts
Death includes mixed emotions and endless possibilities. If you are writing essays about death, see our examples and prompts in this article.
Over 50 million people die yearly from different causes worldwide. It’s a fact we must face when the time comes. Although the subject has plenty of dire connotations, many are still fascinated by death, enough so that literary pieces about it never cease. Every author has a reason why they want to talk about death. Most use it to put their grievances on paper to help them heal from losing a loved one. Some find writing and reading about death moving, transformative, or cathartic.
To help you write a compelling essay about death, we prepared five examples to spark your imagination:
| IMAGE | PRODUCT | |
|---|---|---|
| Grammarly | ||
| ProWritingAid |
1. Essay on Death Penalty by Aliva Manjari
2. coping with death essay by writer cameron, 3. long essay on death by prasanna, 4. because i could not stop for death argumentative essay by writer annie, 5. an unforgettable experience in my life by anonymous on gradesfixer.com, 1. life after death, 2. death rituals and ceremonies, 3. smoking: just for fun or a shortcut to the grave, 4. the end is near, 5. how do people grieve, 6. mental disorders and death, 7. are you afraid of death, 8. death and incurable diseases, 9. if i can pick how i die.
“The death penalty is no doubt unconstitutional if imposed arbitrarily, capriciously, unreasonably, discriminatorily, freakishly or wantonly, but if it is administered rationally, objectively and judiciously, it will enhance people’s confidence in criminal justice system.”
Manjari’s essay considers the death penalty as against the modern process of treating lawbreakers, where offenders have the chance to reform or defend themselves. Although the author is against the death penalty, she explains it’s not the right time to abolish it. Doing so will jeopardize social security. The essay also incorporates other relevant information, such as the countries that still have the death penalty and how they are gradually revising and looking for alternatives.
You might also be interested in our list of the best war books .
“How a person copes with grief is affected by the person’s cultural and religious background, coping skills, mental history, support systems, and the person’s social and financial status.”
Cameron defines coping and grief through sharing his personal experience. He remembers how their family and close friends went through various stages of coping when his Aunt Ann died during heart surgery. Later in his story, he mentions Ann’s last note, which she wrote before her surgery, in case something terrible happens. This note brought their family together again through shared tears and laughter. You can also check out these articles about cancer .
“Luckily or tragically, we are completely sentenced to death. But there is an interesting thing; we don’t have the knowledge of how the inevitable will strike to have a conversation.”
Prasanna states the obvious – all people die, but no one knows when. She also discusses the five stages of grief: denial, anger, bargaining, depression, and acceptance. Research also shows that when people die, the brain either shows a flashback of life or sees a ray of light.
Even if someone can predict the day of their death, it won’t change how the people who love them will react. Some will cry or be numb, but in the end, everyone will have to accept the inevitable. The essay ends with the philosophical belief that the soul never dies and is reborn in a new identity and body. You can also check out these elegy examples .
“People have busy lives, and don’t think of their own death, however, the speaker admits that she was willing to put aside her distractions and go with death. She seemed to find it pretty charming.”
The author focuses on how Emily Dickinson ’s “ Because I Could Not Stop for Death ” describes death. In the poem, the author portrays death as a gentle, handsome, and neat man who picks up a woman with a carriage to take her to the grave. The essay expounds on how Dickinson uses personification and imagery to illustrate death.
“The death of a loved one is one of the hardest things an individual can bring themselves to talk about; however, I will never forget that day in the chapter of my life, as while one story continued another’s ended.”
The essay delve’s into the author’s recollection of their grandmother’s passing. They recount the things engrained in their mind from that day – their sister’s loud cries, the pounding and sinking of their heart, and the first time they saw their father cry.
Looking for more? Check out these essays about losing a loved one .
9 Easy Writing Prompts on Essays About Death
Are you still struggling to choose a topic for your essay? Here are prompts you can use for your paper:
Your imagination is the limit when you pick this prompt for your essay. Because no one can confirm what happens to people after death, you can create an essay describing what kind of world exists after death. For instance, you can imagine yourself as a ghost that lingers on the Earth for a bit. Then, you can go to whichever place you desire and visit anyone you wish to say proper goodbyes to first before crossing to the afterlife.

Every country, religion, and culture has ways of honoring the dead. Choose a tribe, religion, or place, and discuss their death rituals and traditions regarding wakes and funerals. Include the reasons behind these activities. Conclude your essay with an opinion on these rituals and ceremonies but don’t forget to be respectful of everyone’s beliefs.
Smoking is still one of the most prevalent bad habits since tobacco’s creation in 1531 . Discuss your thoughts on individuals who believe there’s nothing wrong with this habit and inadvertently pass secondhand smoke to others. Include how to avoid chain-smokers and if we should let people kill themselves through excessive smoking. Add statistics and research to support your claims.
Collate people’s comments when they find out their death is near. Do this through interviews, and let your respondents list down what they’ll do first after hearing the simulated news. Then, add their reactions to your essay.
There is no proper way of grieving. People grieve in their way. Briefly discuss death and grieving at the start of your essay. Then, narrate a personal experience you’ve had with grieving to make your essay more relatable. Or you can compare how different people grieve. To give you an idea, you can mention that your father’s way of grieving is drowning himself in work while your mom openly cries and talk about her memories of the loved one who just passed away.
Explain how people suffering from mental illnesses view death. Then, measure it against how ordinary people see the end. Include research showing death rates caused by mental illnesses to prove your point. To make organizing information about the topic more manageable, you can also focus on one mental illness and relate it to death.
Check out our guide on how to write essays about depression .
Sometimes, seriously ill people say they are no longer afraid of death. For others, losing a loved one is even more terrifying than death itself. Share what you think of death and include factors that affected your perception of it.
People with incurable diseases are often ready to face death. For this prompt, write about individuals who faced their terminal illnesses head-on and didn’t let it define how they lived their lives. You can also review literary pieces that show these brave souls’ struggle and triumph. A great series to watch is “ My Last Days .”
You might also be interested in these epitaph examples .
No one knows how they’ll leave this world, but if you have the chance to choose how you part with your loved ones, what will it be? Probe into this imagined situation. For example, you can write: “I want to die at an old age, surrounded by family and friends who love me. I hope it’ll be a peaceful death after I’ve done everything I wanted in life.”
To make your essay more intriguing, put unexpected events in it. Check out these plot twist ideas .
May 3, 2023
Contemplating Mortality: Powerful Essays on Death and Inspiring Perspectives
The prospect of death may be unsettling, but it also holds a deep fascination for many of us. If you're curious to explore the many facets of mortality, from the scientific to the spiritual, our article is the perfect place to start. With expert guidance and a wealth of inspiration, we'll help you write an essay that engages and enlightens readers on one of life's most enduring mysteries!
Death is a universal human experience that we all must face at some point in our lives. While it can be difficult to contemplate mortality, reflecting on death and loss can offer inspiring perspectives on the nature of life and the importance of living in the present moment. In this collection of powerful essays about death, we explore profound writings that delve into the human experience of coping with death, grief, acceptance, and philosophical reflections on mortality.
Through these essays, readers can gain insight into different perspectives on death and how we can cope with it. From personal accounts of loss to philosophical reflections on the meaning of life, these essays offer a diverse range of perspectives that will inspire and challenge readers to contemplate their mortality.
The Inevitable: Coping with Mortality and Grief
Mortality is a reality that we all have to face, and it is something that we cannot avoid. While we may all wish to live forever, the truth is that we will all eventually pass away. In this article, we will explore different aspects of coping with mortality and grief, including understanding the grieving process, dealing with the fear of death, finding meaning in life, and seeking support.
Understanding the Grieving Process
Grief is a natural and normal response to loss. It is a process that we all go through when we lose someone or something important to us. The grieving process can be different for each person and can take different amounts of time. Some common stages of grief include denial, anger, bargaining, depression, and acceptance. It is important to remember that there is no right or wrong way to grieve and that it is a personal process.
Denial is often the first stage of grief. It is a natural response to shock and disbelief. During this stage, we may refuse to believe that our loved one has passed away or that we are facing our mortality.
Anger is a common stage of grief. It can manifest as feelings of frustration, resentment, and even rage. It is important to allow yourself to feel angry and to express your emotions healthily.
Bargaining is often the stage of grief where we try to make deals with a higher power or the universe in an attempt to avoid our grief or loss. We may make promises or ask for help in exchange for something else.
Depression is a natural response to loss. It is important to allow yourself to feel sad and to seek support from others.
Acceptance is often the final stage of grief. It is when we come to terms with our loss and begin to move forward with our lives.
Dealing with the Fear of Death
The fear of death is a natural response to the realization of our mortality. It is important to acknowledge and accept our fear of death but also to not let it control our lives. Here are some ways to deal with the fear of death:
Accepting Mortality
Accepting our mortality is an important step in dealing with the fear of death. We must understand that death is a natural part of life and that it is something that we cannot avoid.
Finding Meaning in Life
Finding meaning in life can help us cope with the fear of death. It is important to pursue activities and goals that are meaningful and fulfilling to us.
Seeking Support
Seeking support from friends, family, or a therapist can help us cope with the fear of death. Talking about our fears and feelings can help us process them and move forward.
Finding meaning in life is important in coping with mortality and grief. It can help us find purpose and fulfillment, even in difficult times. Here are some ways to find meaning in life:
Pursuing Passions
Pursuing our passions and interests can help us find meaning and purpose in life. It is important to do things that we enjoy and that give us a sense of accomplishment.
Helping Others
Helping others can give us a sense of purpose and fulfillment. It can also help us feel connected to others and make a positive impact on the world.
Making Connections
Making connections with others is important in finding meaning in life. It is important to build relationships and connections with people who share our values and interests.
Seeking support is crucial when coping with mortality and grief. Here are some ways to seek support:
Talking to Friends and Family
Talking to friends and family members can provide us with a sense of comfort and support. It is important to express our feelings and emotions to those we trust.
Joining a Support Group
Joining a support group can help us connect with others who are going through similar experiences. It can provide us with a safe space to share our feelings and find support.
Seeking Professional Help
Seeking help from a therapist or counselor can help cope with grief and mortality. A mental health professional can provide us with the tools and support we need to process our emotions and move forward.
Coping with mortality and grief is a natural part of life. It is important to understand that grief is a personal process that may take time to work through. Finding meaning in life, dealing with the fear of death, and seeking support are all important ways to cope with mortality and grief. Remember to take care of yourself, allow yourself to feel your emotions, and seek support when needed.
The Ethics of Death: A Philosophical Exploration
Death is an inevitable part of life, and it is something that we will all experience at some point. It is a topic that has fascinated philosophers for centuries, and it continues to be debated to this day. In this article, we will explore the ethics of death from a philosophical perspective, considering questions such as what it means to die, the morality of assisted suicide, and the meaning of life in the face of death.
Death is a topic that elicits a wide range of emotions, from fear and sadness to acceptance and peace. Philosophers have long been interested in exploring the ethical implications of death, and in this article, we will delve into some of the most pressing questions in this field.
What does it mean to die?
The concept of death is a complex one, and there are many different ways to approach it from a philosophical perspective. One question that arises is what it means to die. Is death simply the cessation of bodily functions, or is there something more to it than that? Many philosophers argue that death represents the end of consciousness and the self, which raises questions about the nature of the soul and the afterlife.
The morality of assisted suicide
Assisted suicide is a controversial topic, and it raises several ethical concerns. On the one hand, some argue that individuals have the right to end their own lives if they are suffering from a terminal illness or unbearable pain. On the other hand, others argue that assisting someone in taking their own life is morally wrong and violates the sanctity of life. We will explore these arguments and consider the ethical implications of assisted suicide.
The meaning of life in the face of death
The inevitability of death raises important questions about the meaning of life. If our time on earth is finite, what is the purpose of our existence? Is there a higher meaning to life, or is it simply a product of biological processes? Many philosophers have grappled with these questions, and we will explore some of the most influential theories in this field.
The role of death in shaping our lives
While death is often seen as a negative force, it can also have a positive impact on our lives. The knowledge that our time on earth is limited can motivate us to live life to the fullest and to prioritize the things that truly matter. We will explore the role of death in shaping our values, goals, and priorities, and consider how we can use this knowledge to live more fulfilling lives.
The ethics of mourning
The process of mourning is an important part of the human experience, and it raises several ethical questions. How should we respond to the death of others, and what is our ethical responsibility to those who are grieving? We will explore these questions and consider how we can support those who are mourning while also respecting their autonomy and individual experiences.
The ethics of immortality
The idea of immortality has long been a fascination for humanity, but it raises important ethical questions. If we were able to live forever, what would be the implications for our sense of self, our relationships with others, and our moral responsibilities? We will explore the ethical implications of immortality and consider how it might challenge our understanding of what it means to be human.
The ethics of death in different cultural contexts
Death is a universal human experience, but how it is understood and experienced varies across different cultures. We will explore how different cultures approach death, mourning, and the afterlife, and consider the ethical implications of these differences.
Death is a complex and multifaceted topic, and it raises important questions about the nature of life, morality, and human experience. By exploring the ethics of death from a philosophical perspective, we can gain a deeper understanding of these questions and how they shape our lives.
The Ripple Effect of Loss: How Death Impacts Relationships
Losing a loved one is one of the most challenging experiences one can go through in life. It is a universal experience that touches people of all ages, cultures, and backgrounds. The grief that follows the death of someone close can be overwhelming and can take a significant toll on an individual's mental and physical health. However, it is not only the individual who experiences the grief but also the people around them. In this article, we will discuss the ripple effect of loss and how death impacts relationships.
Understanding Grief and Loss
Grief is the natural response to loss, and it can manifest in many different ways. The process of grieving is unique to each individual and can be affected by many factors, such as culture, religion, and personal beliefs. Grief can be intense and can impact all areas of life, including relationships, work, and physical health.
The Impact of Loss on Relationships
Death can impact relationships in many ways, and the effects can be long-lasting. Below are some of how loss can affect relationships:
1. Changes in Roles and Responsibilities
When someone dies, the roles and responsibilities within a family or social circle can shift dramatically. For example, a spouse who has lost their partner may have to take on responsibilities they never had before, such as managing finances or taking care of children. This can be a difficult adjustment, and it can put a strain on the relationship.
2. Changes in Communication
Grief can make it challenging to communicate with others effectively. Some people may withdraw and isolate themselves, while others may become angry and lash out. It is essential to understand that everyone grieves differently, and there is no right or wrong way to do it. However, these changes in communication can impact relationships, and it may take time to adjust to new ways of interacting with others.
3. Changes in Emotional Connection
When someone dies, the emotional connection between individuals can change. For example, a parent who has lost a child may find it challenging to connect with other parents who still have their children. This can lead to feelings of isolation and disconnection, and it can strain relationships.
4. Changes in Social Support
Social support is critical when dealing with grief and loss. However, it is not uncommon for people to feel unsupported during this time. Friends and family may not know what to say or do, or they may simply be too overwhelmed with their grief to offer support. This lack of social support can impact relationships and make it challenging to cope with grief.
Coping with Loss and Its Impact on Relationships
Coping with grief and loss is a long and difficult process, but it is possible to find ways to manage the impact on relationships. Below are some strategies that can help:
1. Communication
Effective communication is essential when dealing with grief and loss. It is essential to talk about how you feel and what you need from others. This can help to reduce misunderstandings and make it easier to navigate changes in relationships.
2. Seek Support
It is important to seek support from friends, family, or a professional if you are struggling to cope with grief and loss. Having someone to talk to can help to alleviate feelings of isolation and provide a safe space to process emotions.
3. Self-Care
Self-care is critical when dealing with grief and loss. It is essential to take care of your physical and emotional well-being. This can include things like exercise, eating well, and engaging in activities that you enjoy.
4. Allow for Flexibility
It is essential to allow for flexibility in relationships when dealing with grief and loss. People may not be able to provide the same level of support they once did or may need more support than they did before. Being open to changes in roles and responsibilities can help to reduce strain on relationships.
5. Find Meaning
Finding meaning in the loss can be a powerful way to cope with grief and loss. This can involve creating a memorial, participating in a support group, or volunteering for a cause that is meaningful to you.
The impact of loss is not limited to the individual who experiences it but extends to those around them as well. Relationships can be greatly impacted by the death of a loved one, and it is important to be aware of the changes that may occur. Coping with loss and its impact on relationships involves effective communication, seeking support, self-care, flexibility, and finding meaning.
What Lies Beyond Reflections on the Mystery of Death
Death is an inevitable part of life, and yet it remains one of the greatest mysteries that we face as humans. What happens when we die? Is there an afterlife? These are questions that have puzzled us for centuries, and they continue to do so today. In this article, we will explore the various perspectives on death and what lies beyond.
Understanding Death
Before we can delve into what lies beyond, we must first understand what death is. Death is defined as the permanent cessation of all biological functions that sustain a living organism. This can occur as a result of illness, injury, or simply old age. Death is a natural process that occurs to all living things, but it is also a process that is often accompanied by fear and uncertainty.
The Physical Process of Death
When a person dies, their body undergoes several physical changes. The heart stops beating, and the body begins to cool and stiffen. This is known as rigor mortis, and it typically sets in within 2-6 hours after death. The body also begins to break down, and this can lead to a release of gases that cause bloating and discoloration.
The Psychological Experience of Death
In addition to the physical changes that occur during and after death, there is also a psychological experience that accompanies it. Many people report feeling a sense of detachment from their physical body, as well as a sense of peace and calm. Others report seeing bright lights or visions of loved ones who have already passed on.
Perspectives on What Lies Beyond
There are many different perspectives on what lies beyond death. Some people believe in an afterlife, while others believe in reincarnation or simply that death is the end of consciousness. Let's explore some of these perspectives in more detail.
One of the most common beliefs about what lies beyond death is the idea of an afterlife. This can take many forms, depending on one's religious or spiritual beliefs. For example, many Christians believe in heaven and hell, where people go after they die depending on their actions during life. Muslims believe in paradise and hellfire, while Hindus believe in reincarnation.
Reincarnation
Reincarnation is the belief that after we die, our consciousness is reborn into a new body. This can be based on karma, meaning that the quality of one's past actions will determine the quality of their next life. Some people believe that we can choose the circumstances of our next life based on our desires and attachments in this life.
End of Consciousness
The idea that death is simply the end of consciousness is a common belief among atheists and materialists. This view holds that the brain is responsible for creating consciousness, and when the brain dies, consciousness ceases to exist. While this view may be comforting to some, others find it unsettling.
Death is a complex and mysterious phenomenon that continues to fascinate us. While we may never fully understand what lies beyond death, it's important to remember that everyone has their own beliefs and perspectives on the matter. Whether you believe in an afterlife, reincarnation, or simply the end of consciousness, it's important to find ways to cope with the loss of a loved one and to find peace with your mortality.
Final Words
In conclusion, these powerful essays on death offer inspiring perspectives and deep insights into the human experience of coping with mortality, grief, and loss. From personal accounts to philosophical reflections, these essays provide a diverse range of perspectives that encourage readers to contemplate their mortality and the meaning of life.
By reading and reflecting on these essays, readers can gain a better understanding of how death shapes our lives and relationships, and how we can learn to accept and cope with this inevitable part of the human experience.
If you're looking for a tool to help you write articles, essays, product descriptions, and more, Jenni.ai could be just what you need. With its AI-powered features, Jenni can help you write faster and more efficiently, saving you time and effort. Whether you're a student writing an essay or a professional writer crafting a blog post, Jenni's autocomplete feature, customized styles, and in-text citations can help you produce high-quality content in no time. Don't miss out on the opportunity to supercharge your next research paper or writing project – sign up for Jenni.ai today and start writing with confidence!
Try Jenni for free today
Create your first piece of content with Jenni today and never look back
Home — Essay Samples — Literature — The Fault in Our Stars — The Theme of Death, Loss, and Grief
The Theme of Death, Loss, and Grief
- Categories: The Fault in Our Stars
About this sample

Words: 512 |
Published: Jan 29, 2024
Words: 512 | Page: 1 | 3 min read
Table of contents
Interpretation of death as a theme, exploration of loss as a theme, discussion of grief as a theme, analysis of the relationship between death, loss, and grief, comparison of different perspectives and cultural interpretations.
- Shakespeare, William. "Hamlet."
- Green, John. "The Fault in Our Stars."
- Morrison, Ton"Beloved."
- Garcia Marquez, Gabriel. "One Hundred Years of Solitude."

Cite this Essay
Let us write you an essay from scratch
- 450+ experts on 30 subjects ready to help
- Custom essay delivered in as few as 3 hours
Get high-quality help

Prof. Kifaru
Verified writer
- Expert in: Literature

+ 120 experts online
By clicking “Check Writers’ Offers”, you agree to our terms of service and privacy policy . We’ll occasionally send you promo and account related email
No need to pay just yet!
Related Essays
3 pages / 1249 words
6 pages / 2729 words
3.5 pages / 1498 words
4 pages / 1725 words
Remember! This is just a sample.
You can get your custom paper by one of our expert writers.
121 writers online
Still can’t find what you need?
Browse our vast selection of original essay samples, each expertly formatted and styled
Related Essays on The Fault in Our Stars
John Green’s novel “Looking for Alaska” tells the story of Miles “Pudge” Halter, a young man who is seeking a deeper understanding of life and its meaning. Throughout the novel, Pudge is preoccupied with the idea of the “Great [...]
The Fault in Our Stars, written by John Green, is a novel that tackles the difficult topic of terminal illness and the impact it has on the lives of the main characters, Hazel Grace Lancaster and Augustus Waters. The novel [...]
In the book The Fault In Our Stars by John Green, the main character, Hazel Grace, is introduced as a teen. However, she’s not your average teen, she is suffering from thyroid (lung) cancer. She’s described as a sixteen-year-old [...]
John Green's novel, "The Fault in Our Stars," tells the poignant tale of two teenagers who fall in love amidst the looming shadow of cancer. Unlike typical teenage romance narratives, this story is marked by an unresolvable [...]
In psychology, conflict refers to anytime when people have opposing or incompatible actions, objectives, or ideas. The psychologists define conflict to be a state of opposition and disagreement between two or more people, which [...]
In John Green's novel "The Fault in Our Stars," Hazel Grace Lancaster emerges as the central character and protagonist, grappling with the challenges of a terminal cancer diagnosis. The story unfolds as Hazel navigates her [...]
Related Topics
By clicking “Send”, you agree to our Terms of service and Privacy statement . We will occasionally send you account related emails.
Where do you want us to send this sample?
By clicking “Continue”, you agree to our terms of service and privacy policy.
Be careful. This essay is not unique
This essay was donated by a student and is likely to have been used and submitted before
Download this Sample
Free samples may contain mistakes and not unique parts
Sorry, we could not paraphrase this essay. Our professional writers can rewrite it and get you a unique paper.
Please check your inbox.
We can write you a custom essay that will follow your exact instructions and meet the deadlines. Let's fix your grades together!
Get Your Personalized Essay in 3 Hours or Less!
We use cookies to personalyze your web-site experience. By continuing we’ll assume you board with our cookie policy .
- Instructions Followed To The Letter
- Deadlines Met At Every Stage
- Unique And Plagiarism Free

- Table of Contents
- Random Entry
- Chronological
- Editorial Information
- About the SEP
- Editorial Board
- How to Cite the SEP
- Special Characters
- Advanced Tools
- Support the SEP
- PDFs for SEP Friends
- Make a Donation
- SEPIA for Libraries
- Entry Contents
Bibliography
Academic tools.
- Friends PDF Preview
- Author and Citation Info
- Back to Top
This article considers several questions concerning the philosophy of death.
First , it discusses what it is to be alive. This topic arises because to die is roughly to lose one’s life.
The second topic is the nature of death, and how it bears on the persistence of organisms and persons.
The third topic is the harm thesis , the claim that death can harm the individual who dies. Perhaps the most influential case against the harm thesis was made by Epicurus. His argument is discussed, as is a contemporary response, the deprivationist defense of the harm thesis.
The fourth topic is a question that seems to confront proponents of the harm thesis, especially those who offer some version of the deprivationist defense: if a person is harmed by her death, at what time does her death make her worse off than she otherwise would be? Some answers are considered.
Fifth is further issues that may lead us to doubt the harm thesis. One is a further question about deprivationism: we are not always harmed by what deprives us of things; what makes some of these worrisome and not others? Next is a question concerning the fact that there are two different directions in which our lives could be extended: into the past (our lives could have been longer if they began earlier), or into the future (they could have been longer if they ended later). Assuming the former does not matter to us, why should the latter?
The sixth topic concerns events that occur after a person has died: is it possible for these events to harm her?
Seventh is a controversy concerning whether extreme long life, even immortality, would be good for us. Of particular interest here is a dispute between Thomas Nagel, who says that death is an evil whenever it comes, and Bernard Williams, who argues that, while premature death is a misfortune, it is a good thing that we are not immortal, since we cannot continue to have our current characters and remain meaningfully attached to life forever.
A final controversy concerns whether or not the harmfulness of death can be reduced. It may be that, by adjusting our conception of our well-being, and by altering our attitudes, we can reduce or eliminate the threat death poses us. But there is a case to be made that such efforts backfire if taken to extremes.
1.1 Life as a Substance
1.2 life as an event, 1.3 life as a property, 2.1 life and death, 2.2 death and suspended vitality, 2.3 being dead, 2.4 resurrection, 2.5 death and what we are, 2.6 death and existence, 2.7 criteria for death, 3.1 the epicurean case, 3.2 the deprivationist defense, 4.1 concurrentism, 4.2 priorism, 4.3 subsequentism, 4.4 indefinitism, 4.5 atemporalism, 5.1 harmless preclusion.
- 5.2 Lucretius and the Symmetry Argument
6.1 Doubts About Posthumous Harm
6.2 retroactive harm, 7.1 never dying would be good, 7.2 never dying would be a misfortune, 8. can death’s harmfulness be reduced, other internet resources, related entries.
To die is to cease to be alive. To clarify death further, then, we will need to say a bit about the nature of life.
Some theorists have said that life is a substance of some sort. A more plausible view is that life is a property of some sort, but we should also consider the possibility that lives are events. If we say that lives are events, we will want to know something about how to distinguish them from other events, and how they are related to the individuals that are alive. It would also be useful to know the persistence conditions for a life. If instead we conclude that life (or alive ) is a property, we will want to clarify it, and identify what sorts of things bear it. Let us briefly discuss each of these views—that life is a substance, a property, or an event.
We can deal quickly with the view called ‘vitalism’ (defended by Hans Driesch, 1908 and 1914, among others), which holds that being alive consists in containing some special substance called ‘life.’ Vitalism is a nonstarter since it is unclear what sort of stuff vitalists take life to be, and because no likely candidates—no special stuff found in all and only in living things—have been detected. Moreover, vitalism faces a further difficulty, which Fred Feldman calls ‘the Jonah Problem’: a dead thing, such as a whale, may have a living thing, say Jonah, inside it; if Jonah has ‘life’ inside him, then so does the whale, but by hypothesis the whale is not alive. Of course, in this example Jonah is in the whale’s stomach, not in its cells, but the difficulty cannot be solved by saying that an object is alive if and only if it has ‘life’ in its cells, as an infectious agent (organisms with ‘life’ in them) could survive, for a time, within the dead cells of a dead whale.
As Jay Rosenberg noted (1983, p. 22, 103), sometimes when we speak of a life we mean to refer to the events that make up something’s history—the things that it did and the things that happened to it. (For example, the publication of The Problems of Philosophy was one of the events that made up one life, namely Bertrand Russell’s.) Yet a rock and a corpse have histories, and neither has a life. Presumably, then, ‘a life,’ in the sense we are discussing, refers to the history of something that is alive. In that case what we are really looking for is clarification of a property, not an event. We want clarification of what it is to be alive.
According to a second theorist, Peter van Inwagen, while a life is indeed an event, it is not the history of something. “‘Russell’s life,’” van Inwagen writes (1990, p. 83), “denotes a purely biological event, an event which took place entirely inside Russell’s skin and which went on for ninety-seven years.” Russell’s life included the oxygenation of his hemoglobin molecules but not the publication of his books.
If lives are biological events, it would be useful to know more about what they are, how they are individuated, and what their persistence conditions are. Van Inwagen declines to provide these details (1990, p. 145). He assumes that (the events he calls) lives are familiar enough to us that we can pick them out. But he does make the useful comment that each such event is constituted by certain self-organizing activities in which some molecules engage, and that it is analogous to a parade, which is an event constituted by certain marching-related activities of some people. Having taken the notion of a life for granted, he draws upon it in his account of organisms. On his view (1990, p. 90), some things compose an organism if and only if their activity constitutes a life.
Many theorists have defended the view that life, or (being) alive, is a property, but there is considerable disagreement among them about what precisely that property is. The main views on offer are life-functionalist accounts and accounts that analyze life in terms of DNA or genetic information or evolution by natural selection.
Life-functionalism, a view introduced by Aristotle, analyzes the property alive in terms of one or more salient functions that living things typically are able to perform. The salient functions Aristotle listed were nutrition, reproduction, sensation, autonomous motion, and thought. However, life-functionists disagree about how to formulate their account and about which functions are salient. Take Aristotle’s list. Obviously, it would be a mistake to say that something is alive if and only if it can perform all of the functions on the list. Might we say that, for something to be alive, it suffices that it be capable of one or more of the listed functions? Is being capable of one of these functions in particular necessary for something to be alive? As Fred Feldman points out, neither of the suggestions just mentioned is acceptable. Devices such as Roomba cleaning robots can do one of Aristotle’s functions, namely move themselves, but are not alive, so being able to do at least one listed function does not suffice for being alive. Nor is it plausible to say that any one on the list is necessary for being alive. Which on the list would this necessary function be? Perhaps nutrition? Adult silk moths are alive but lack a digestive system, so are incapable of nutrition. And, as many theorists have noticed, many living things cannot reproduce; examples include organisms whose reproductive organs are damaged and hybrid animals such as mules.
What, now, about accounts that analyze life in terms of genetic information? Feldman thinks that something like the Jonah problem arises for any account according which being alive consists in containing DNA or other genetic information, as dead organisms contain DNA. A further problem for such views is that it is conceivable there are or could be life forms (say on other planets) that are not based on genetic information. This latter difficulty can be avoided if we say that being alive consists in having the ability to evolve, to engage in Darwinian evolution, assuming that evolution by natural selection is possible for living things that lack nucleic acid. We might adopt NASA’s definition, according to which life is “a self-sustaining chemical system capable of Darwinian evolution.” However, accounts like NASA’s are implausible for a further reason: while the ability to evolve by natural selection is something that collections of organisms—species—may or may not have, it is not a feature an individual organism may have. Later members of a species come to have features earlier members lacked; some of these new features may make survival more or less likely, and the less ‘fit’ are weeded out of existence. An individual organism, such as a particular dog, cannot undergo this process. Yet individuals may be alive.
Because he has encountered no successful account of life, no account exempt from counterexamples, Feldman concludes that “life is a mystery” (p. 55). Despite his skepticism, however, there is a good case to be made for saying that what distinguishes objects that are alive from objects that are not is that the latter have a distinctive sort of control over what composes them, which the former lack. Let us see if we can make this claim clearer.
Consider ordinary composite material objects that are not alive. We can assume that, at a given time, these are made up of, or composed of, more simple things, such as molecules, by virtue of the fact that the latter meet various conditions. Among the conditions is the requirement that (in some sense in need of clarification) they be bonded together . Take the boulder near my front porch. Among the things that compose it now will be a few molecules, say four molecules near the center of the boulder, that are bonded together, in that each is bonded to the others, directly or indirectly (a molecule, A, is in directly bonded to another molecule, B, if A is directly bonded to a molecule C that is directly bonded to B, or if A is bonded to a molecule that is indirectly bonded to B). The things that make up the boulder are not limited to these four molecules, but they are limited to molecules that are bonded to them. Nor is the boulder unique in this way; something similar seems true of any composite material object. A composite material object is composed of some things at a time only if those things are bonded together at that time.
What sort of bonding relationship holds among the things that compose material objects? Any answer to this question will be controversial. Let us set it aside, and move on to some further assumptions about the composition of nonliving composite material objects, namely that a great many of them persist for a while (some persist for a very long time) and that what composes them at one time normally differs from what composes them at other times. Exactly how this works is a complicated matter, but among the conditions that such objects must meet if they are to persist is that any change in their composition be incremental. (Even this condition is controversial. For more on material objects, see the article Material Constitution and Ordinary objects.) Consider the boulder again. Suppose that at one time, t 0 , it is composed of some molecules, and that all or most of these molecules remain bonded to each other until a later time t 1 . Suppose, too, that no or few (few as compared to the number of molecules that composed the boulder at t 0 ) molecules come to be newly bonded to these by the time that t 1 rolls around. Under these conditions the boulder undergoes an incremental change in composition, and it seems plausible to say that the boulder remains in existence over the interval t 0 – t 1 , and, at t 1 , is composed of the molecules that remain bonded together with the molecules that are newly attached to them. Presumably, it will also survive a series of such incremental changes in composition. But it will not survive drastic and sudden changes. It would stop existing, for example, if the molecules that compose it were suddenly dispersed.
Enough said about composite material objects that are not alive. Now let us see if we can shed some light on what makes living objects special. What is it that distinguishes an object that is alive from an object that is not?
The answer seems to be that, normally, a live object has a distinctive sort of control over whether things come to be, or cease to be, part of it. The control in question is made possible by activities its constituents themselves are capable of. Contrast objects that are not alive, say automobiles. What an ordinary car is composed of is settled for the car by the mechanics who repair it (detaching some parts and affixing others), by whether it is involved in an accident and loses some parts, and so forth. Imagine a car that is not passive in this way. Imagine that its parts were somehow capable of replacing some of themselves with fresh parts, without assistance from outside, so that the activities of the parts that compose the car today were responsible for its being composed of certain parts tomorrow. That would make it quite lifelike.
Let us describe, in a bit more detail, what the molecules that compose living objects can do:
- Working together, these molecules can engage in activities that are integrated in conformity with (under the control of) the information that some of them carry (information that is comparable to blueprints and instructions), much as soldiers that make up an army can engage in activities that are integrated in conformity with battle plans and instructions issued by the commanding officers that are among them.
- Deploying these activities, the molecules can self-modify, in the sense that they can bond new (perhaps recently ingested) molecules to themselves, or prune (and excrete) some away, combining themselves in various ways (e.g., constructing cells), thereby giving way to a slightly different assembly of molecules at a later time, and fueling their activities by drawing upon external energy sources or stored reserves.
- The molecules can also pass along their ability to self-modify, enabling the molecules to which they give way to continue these activities, thus allowing the object they compose to sustain a given form (or forms) over time (say that of a dog) despite the fact that what composes that object at one time differs from what composes it at another time.
The view on offer—we might call it the compositional account of life—is that an object is composed of things that are capable of the activities just described if and only if it is alive.
This account of life needs refinement, but it avoids at least most of the worries mentioned earlier. It implies that an object may be alive even though it is sterile (as in the case of mules), even though it survives on stored energy (as in the case of a silk moth), and conceivably even if it lacks nucleic acid (yet is still composed of things that engage in activities integrated in conformity with information they carry). In fact, it implies that being capable of none of the items on Aristotle’s list is necessary nor sufficient for being alive. What is more, the compositional account just sketched implies that being alive is a property an individual, say the last remaining dodo, may bear on its own, which suggests that it may be alive without being capable of Darwinian evolution. At the same time, it explains how collections of live individuals may evolve. Individual objects are alive only if their composition is under the control of some of their parts (e.g., nucleic acid molecules) that carry information. The mechanisms by which such information is carried tend to be modified over time, altering the information they carry, and thus the features of the organisms they help shape, introducing mutations that may or may not facilitate survival. (For more on the nature of life, see Bedau 2014 and the entry on Life.)
The previous section discussed the nature of life, thereby clarifying what it is that death ends. This section discusses the nature of death and how death is related to the persistence of organisms and persons. (For an excellent discussion of views of death outside of the analytic tradition, see Schumacher 2010.)
According to the compositional account of life discussed in the previous section, objects that are alive have a distinctive capacity to control what they are composed of, fixing these constituents together in various ways, by virtue of the fact that their constituents can engage in various self-modifying activities that are integrated in conformity with information they carry. Let us call these vital activities .
It is one thing to have the capacity to engage in vital activities and another actually to engage in them, just as there is a difference between having the ability to run and actually running. Being alive seems to involve the former. It consists in having the relevant capacity. To die is to lose this capacity. We can call this the loss of life account of death .
The event by which the capacity to engage in vital activities is lost is one thing, and the state of affairs of its having been lost it is another. ‘Death’ can refer to either. However, the capacity to engage in vital activities may be lost gradually, rather than all at once, so it is reasonable to speak of a process of dying. In some cases that process is especially complicated, because the self-modifying activities of some organisms result in the construction of complex physiological systems that must remain largely intact for the self-modifying activities of these organisms to remain integrated. In defining death, some theorists focus on these systems, and claim that an organism’s life ends when that organism’s physiological systems can no longer function as an integrated whole, or when this loss becomes irreversible (Christopher Belshaw 2009; David DeGrazia 2014).
The loss of life account of death has been challenged by theorists who claim that things whose vital activities are suspended are not alive (Feldman 1992, Christopher Belsaw 2009, Cody Gilmore 2013, and David DeGrazia 2014). When zygotes and embryos are frozen for later use in the in vitro fertilization procedure, their vital activities are brought to a stop, or very nearly so. The same goes for water bears that are dehydrated, and for seeds and spores. It seems clear that the zygotes and water bears are not dead, since their vital activities can easily be restarted—by warming the zygote or by wetting the water bear. They are not dead, but are they alive? If we deny that they are alive, presumably we would do so on the grounds that their vital activities are halted. If something’s life can be ended by suspending its vital activities without its dying, then we must reject the loss of life account of death.
However, the loss of life account is thoroughly established in ordinary usage, and is easily reconciled with the possibility of suspended vitality. In denying that frozen embryos are dead, it is clear that we mean to emphasize that they have not lost the capacity to deploy their vital activities. When we say that something is dead, we mean to emphasize that this capacity has been lost. Having used ‘dead’ to signal this loss, why would we want to use the word ‘alive’ to signal the fact that something is making active use of its vital activities? Our best option is to use a pair of contrasting terms. We can use ‘viable’ to indicate that something has the capacity to deploy vital activities and ‘unviable’ to indicate that it has lost this capacity. When instead we are concerned about whether or not something is engaging its vital activities, we can use different contrasting terms, say ‘vital’ and ‘nonvital’, the former to characterize something that is employing its capacity for vital activities and the latter to characterize something that is not making use of its capacity for vital activities. What seems relatively uncontroversial is that being dead consists in unviability. To retain the loss of life account, we have only to add that being alive consists in viability. We can then say that a frozen embryo is viable and hence alive despite its lack of vitality, and it will die if its life ends (it will die if it ceases to be viable). Of course, if we are willing to abandon the loss of life account, we could instead use ‘alive’ to characterize something that is both viable and vital. We would then say that a frozen embryo is not alive (since it lacks vitality) but also that it is not dead (since it remains viable).
People often speak of being dead as a ‘state’ or ‘condition’ as opposed to an event or process. They say an organism comes to be in this state once it dies. This way of speaking can be puzzling on the assumption that what dies ceases to exist. (This assumption is discussed below.) If the assumption is true, then an organism that dies stops existing but simultaneously comes to be in the state of death. Mustn’t something exist at a time if it is (literally) in some state at that time? But of course it would be absurd to deny that something can truly be dead on the grounds that death is a state and what does not exist at a time cannot be in any state at that time.
Why not solve the problem by saying that upon dying an organism leaves a corpse, and it is the corpse that is in the state of being dead? There are several problems with this suggestion. Some organisms do not leave corpses. What corpses are left eventually disintegrate. Whether an organism leaves a corpse or not, and whether its corpse exists or not, if that organism dies at time t and does not regain life then it is dead after t .
The difficulty can be avoided if we say, with Jay Rosenberg 1983, p. 42), that dead is a relation between an organism, the time it died, and a subsequent time, and that when someone asserts, at some given time t , ‘Socrates is dead,’ what is asserted (ignoring the possibility of restored life, discussed in the next section) is roughly that Socrates died before t .
As is mentioned below, some theorists deny that an object that is at one time an organism may continue its existence as a corpse. Such theorists will say that organisms and their corpses are two different objects. They may conclude that ‘dead’ is ambiguous—that it means one thing as applied to organisms, and another thing as attributed to the corpses organisms leave. In any case, they will need to deny that, as concerns corpses, being dead implies having died, as corpses are never alive, according to them. If, on the other hand, an object that is an organism may continue its existence as a corpse, then, at any time t after that object dies, ‘dead’ applies univocally to it at time t , and means roughly died before t .
It will be useful to sharpen the loss of life account if, as seems conceivable, it is possible to restore life to something that has died.
Restoration in this sense is quite different from the revival of something, such as a frozen embryo, whose vital activities have been halted. Something can be revived only if it is alive—only if it has the capacity to deploy vital activities, as in the case of a frozen zygote. It is revived when it regains vitality. Something’s life can be restored only if it has lost its capacity for vital activities. Life is restored when this capacity is regained.
To bring the possibility of restoration into view, imagine a futuristic device, the Disassembler-Reassembler , that chops me into small cubes, or individual cells, or disconnected atoms, which it stores and later reassembles just as they were before. It is far from obvious that I would survive—and that my life would continue—after Reassembly. (Assuming that I am a material object, the account of objects sketched in Section 1.3 implies that chopping me into bits ends my existence forever.) But even if my existence would pick up again after Reassembly occurs, it is quite clear that I would not live during intervals when my atoms are stacked in storage. I would not even exist during such intervals. If I can be Reassembled, my life would be restored, not revived. Restoration, not revival, is a way of bringing a creature back from the dead.
Now imagine a Corpse Reanimator , a device that moves molecules back to where they were prior to the death of the creature that left the corpse, and restarts its vital activities. Some theorists say that I continue my existence as a corpse if it remains in good shape; they will assume that I remain in existence after losing my life, and continue my existence after the Corpse Reanimator does its work. On their view the Corpse Reanimator restores my life--it gives me back the capacity to engage in vital activities.
Given the possibilities of restoration and revivification, it seems best to refine the loss of life account, as follows:
Dying is the loss of an object’s life—the loss of its capacity to perpetuate itself using vital activities. An object dies at the time it loses this capacity. It is dead at all times afterwards, except while that capacity is regained.
Death for you and me is constituted by the loss of our capacity to sustain ourselves using vital activities. This characterization of death could be sharpened if we had a clearer idea of what we are , and its implications concerning our persistence. After all, we cannot retain any capacities if we fail to persist, so if we fail to persist we stop being capable of vital activities. We die. However, what we are, and what is involved in our persistence, is a matter of controversy.
There are three main views: animalism , which says that we are human animals (Snowdon 1990, Olson 1997, 2007); personism , which says that we are creatures with the capacity for self-awareness; and mindism , which says that we are minds (which may or may not have the capacity for self-awareness) (McMahan 2002). Animalists typically say that we persist over time just in case we remain the same animal; mindist typically suggest that our persistence requires our remaining the same mind. Personism is usually paired with the view that our persistence is determined by our psychological features and the relations among them (Locke 1689, Parfit 1984). (For more on what we are, see the entry on Personal Identity.)
If we are animals, with the persistence conditions of animals, we die when we cease to be the same animal. If we are minds, with the persistence conditions for minds, we die when we cease to meet these conditions. And if persistence is determined by our retaining certain psychological features, then the loss of those features will constitute death.
These three ways of understanding death have very different implications. Severe dementia can destroy a great many psychological features without destroying the mind, which suggests that death as understood by personists can occur even though death as understood by mindists has not. Moreover, human animals sometimes survive the destruction of the mind, as when the cerebrum dies but the brainstem does not, leaving an individual in a persistent vegetative state. Many theorists also think that the mind could survive the extinction of the human animal, say when the brain is removed from the body, kept alive artificially, and the remainder of the body is destroyed (assuming that a bare brain is not a human animal). These possibilities suggest that death as understood by mindists can occur even though death as understood by animalists has not (and also that the latter sort of death need not be accompanied by the former.)
What is the relationship between existence and death? May people and other creatures continue to exist after dying, or cease to exist without dying?
Take the first question: may you and I and other creatures continue to exist for some time after our lives end? Fred Feldman (1992, p. 91) coins the term termination thesis to refer to the view that “when a person dies, he or she … goes out of existence; subsequently, there is no such thing as that person.” (A version of the thesis applies to any living thing.) We can call those who accept the termination thesis terminators , and those who deny it anti-terminators . One point anti-terminators such as Feldman (1992, 2000, 2013) cite is that people who encounter corpses sometimes call them dead animals, or dead people. Such talk may suggest that we believe that animals continue to exist, as animals, while no longer alive. The idea might be that an animal continues to count as the same animal if enough of its original components remain in much the same order, and animals continue to meet this condition for a time following death (Mackie 1997). On this view, if you and I are animals (as animalists say), then we could survive for a time after we are dead, albeit as corpses. In fact, we could survive indefinitely, by arranging to have our corpses preserved.
However, this way of defending the anti-terminators’s view may not be decisive. The terms ‘dead animal’ and ‘dead person’ seem ambiguous. Normally, when we use ‘dead people’ or ‘dead animal’ we mean to speak of persons or animals who lived in the past. One dead person I can name is Socrates; he is now a ‘dead person’ even though his corpse surely has ceased to exist. However, in certain contexts, such as when we are standing inside morgues, we seem to use the terms ‘dead animal’ and ‘dead person’ to mean “remains of something that was an animal” or “remains of something that was a person.” On this interpretation, even in morgues calling something a dead person does not imply that it is a person.
Still, the dispute between terminators and anti-terminators is unlikely to be settled on the basis of how we use terms such as ‘dead animal’ and ‘dead person.’ Metaphysical considerations must weigh in. For example, consider that the remarks made in Section 1.3 about the persistence of objects are consistent with the possibility that objects that are people may continue their existence as corpses, which may be useful to anti-terminators. On the other hand, many theorists think that nothing is a person unless it has various psychological features, which corpses lack, and some think that nothing is an organism unless it is alive. Terminators may be able to exploit these thoughts.
What about the second question: can creatures cease to exist without dying? Certainly things that never were alive, such as bubbles and statues, can be deathlessly annihilated. Arguably, there are also ways that living creatures can be deathlessly annihilated (Rosenberg 1983, Feldman 1992, Gilmore 2013). Perhaps an amoeba’s existence ends when it splits, replacing itself with two amoebas, and the existence of chlamydomonas ends when pairs of them fuse to form a zygote. Yet when amoebas split, and chlamydomonas fuse, vital activities do not cease. If people could divide like amoebas, perhaps they, too could cease to exist without dying. (For a famous discussion of division, fusion, and their implications, see Parfit 1981.) If such ‘deathless exits’ are possible, we would have to modify the loss of life account of death.
However, proponents of the loss of life account can hold their ground. They can say that division, fusion, and other apparent examples of deathless exits are unusual ways of dying, because, in such cases, nonexistence is not brought about via the destruction of vital activities, but they are not ways of escaping death altogether. Proponents of the loss of life account might also turn the tables on its critics, and argue as follows: nothing can be alive unless it exists, so if something ceases to exist it ceases to be alive, but to cease to be alive is to die. So there are no deathless exits.
Defining death is one thing; providing criteria by which it can be readily detected or verified is another. A definition is an account of what death is ; when, and only when its definition is met, death has necessarily occurred. A criterion for death, by contrast, lays out conditions by which all and only actual deaths may be readily identified. In some cases criteria for death are intended to capture conditions by which the actual deaths of human persons may be identified. Such a criterion falls short of a definition, but plays a practical role. For example, criteria for the death of a person would help physicians and jurists determine when death has occurred.
In the United States, the states have adopted criteria for the death of a person modeled on the Uniform Determination of Death Act (developed by the President’s Commission, 1981), which says that “an individual who has sustained either (1) irreversible cessation of circulatory and respiratory functions, or (2) irreversible cessation of all functions of the entire brain, including the brain stem, is dead. A determination of death must be made in accordance with accepted medical standards.” In the United Kingdom, the accepted criterion is brain stem death, or the “permanent functional death of the brain stem” (Pallis 1982).
These current criteria are subject to criticism, even if we put aside reservations concerning the qualifier ‘irreversible’. Animalists might resist the criteria since the vital activities of human beings whose entire brains have ceased to function can be sustained artificially using cardiopulmonary assistance. Mindists and personists might also resist the criteria, on the grounds that minds and all psychological features can be destroyed in human beings whose brain stems are intact. For example, cerebral death can leave its victim with an intact brain stem, yet mindless and devoid of self-awareness. (For more on criteria for death, see the article on the Definition of Death.)
3. Epicurus and the Harm Thesis
Is death bad for some people who die? Is it good for some of them?
According to the harm thesis , death is, at least sometimes, bad for those who die, and in this sense something that ‘harms’ them. It is important to know what to make of this thesis, since our response itself can be harmful. This might happen as follows: suppose that we love life, and reason that since it is good, more would be better. Our thoughts then turn to death, and we decide it is bad: the better life is, we think, the better more life would be, and the worse death is. At this point, we are in danger of condemning the human condition, which embraces life and death, on the grounds that it has a tragic side, namely death. It will help some if we remind ourselves that our situation also has a good side. Indeed, our condemnation of death is here based on the assumption that more life would be good. But such consolations are not for everyone. (They are unavailable if we crave immortality on the basis of demanding standards by which the only worthwhile projects are endless in duration, for then we will condemn the condition of mere mortals as tragic through and through, and may, as Unamuno (1913) points out, end up suicidal, fearing that the only life available is not worth having.) And a favorable assessment of life may be a limited consolation, since it leaves open the possibility that, viewing the human condition as a whole, the bad cancels much of the good. In any case it is grim enough to conclude that, given the harm thesis, the human condition has a tragic side.
It is no wonder that theorists over the millennia have sought to defeat the harm thesis. Let us consider some challenges to the harm thesis, beginning with the case against it developed by the ancient Greek philosopher Epicurus.
Epicurus (341–270) adopted a version of hedonism according to which pleasure (or pleasant experiences) is the only thing that is intrinsically good for us (that is, the only thing that is good for us in itself), while pain (or painful experiences) is the only thing that is intrinsically bad for us, bad in itself. Call this view intrinsic hedonism. (For a discussion of intrinsic value, see the entry on Intrinsic vs. Extrinsic Value.) Epicurus’s commitment to intrinsic hedonism prompted him to say, in his Letter to Menoeceus , that “everything good and bad lies in sensation.” He also claimed, in that same letter, that “when we are, death is not, and when death is present, then we are not.” The death of a person, and that person’s existence, do not overlap in time. On the basis of this assumption about death and existence, he concluded that a person’s death does not cause her to have any experiences (sensations)—indeed, “death is to be deprived of sensation.” In the following passage, he uses these thoughts against the harm thesis:
Make yourself familiar with the belief that death is nothing to us, since everything good and bad lies in sensation, and death is to be deprived of sensation. … So that most fearful of all bad things, death, is nothing to us, since when we are, death is not, and when death is present, then we are not.
Much about Epicurus’s argument is unclear, so let us work through it more carefully and see if we can fill in some details that he did not supply. Some speculation will be necessary, but we can develop a reconstruction that aligns with the things he wrote.
Earlier we mentioned one of the views Epicurus accepted, which we can state as follows:
- Intrinsic hedonism is true: a person’s experiences (sensations) of pleasure (or her pleasant experiences) are the only things that are intrinsically good for her, the only things that are good for her in themselves, while her experiences of pain (or painful experiences) are the only things that are intrinsically bad for her, bad in themselves.
From this view it follows that
- something is intrinsically good or bad for a person only if it is an experience.
Now, regardless of whether a person experiences her death, that death is not itself an experience. (Compare: I may experience jogging down the street, and I may experience the cup that is in front of me, but neither jogging nor the cup is itself an experience. My experiences are, so to speak, in my mind. Cups are not.) Let us add this observation to the argument:
- A person’s death is not an experience.
And if a person’s death is not an experience at all, clearly it is not an experience that is intrinsically good or bad for her. So, from 1–3, it follows that
- a person’s death is not intrinsically good or bad for her.
However, something that is not intrinsically bad for a person might nevertheless make other things happen that are detrimental to her, in which case it may be extrinsically bad for her. Seeing somebody fall and break her arm is not intrinsically bad for a person, but it might well cause her painful sadness, which makes the accident she saw extrinsically bad for her. Similarly, something that is not intrinsically good for a person might be extrinsically good for her.
Epicurus recognized the possibility of extrinsic goodness. It is not entirely clear how he understood it, but he seemed to accept a view we can call extrinsic instrumentalism : something is extrinsically good or bad for a person only if it makes her have things (other than itself) that are intrinsically good or bad for her. Let us add this to the argument:
- extrinsic instrumentalism is true: something is extrinsically good or bad for a person only if it makes her have things that are intrinsically good or bad for her.
Armed with this assumption, Epicurus can reject the possibility that a person’s death is extrinsically bad for her, arguing as follows. Because Epicurus thought that the death of a person and that person’s existence do not overlap in time, he thought that
- a person’s death does not make her have any experiences.
From premises 2, 5 and 6 it follows that
- a person’s death is not extrinsically good or bad for her.
To complete the argument against the harm thesis, Epicurus would need an additional assumption, such as this:
- something is good or bad for a person only if it is either intrinsically or extrinsically good or bad for her.
Premises 4, 7 and 8 entail that the harm thesis is false:
- a person’s death is not good or bad for her.
Is this Epicurean argument convincing? Let us see if we can find weak spots. We can begin with a reservation concerning the term ‘death.’
Earlier we noted that ‘death’ might be used for dying, the event or process of losing life, or being dead, the property of having lost life. The first reservation about the argument is that it is strongest if its uses of ‘death’ refer to being dead, and not to (the event or process of) dying. Here is why.
Being dead is not an experience, and it does not make a person have any experiences. So (on Epicurus’s assumptions) it is neither intrinsically nor extrinsically bad for a person to be dead. However, a person may experience dying , and the experience of dying (the experiences dying causes her to have) might well be intrinsically bad for her, even if only painful experiences are intrinsically bad for her (as premise 1 says). So even if being dead is not extrinsically bad for a person, the question arises as to whether, for some people, it is extrinsically bad to die . If something makes a person have painful experiences, isn’t it extrinsically bad for her, other things being equal? At least this much is true: the Epicurean argument does not show that dying painfully is not extrinsically bad for a person.
Apparently, then, the argument does not demonstrate that neither being dead nor dying is ever bad for those who die. Nevertheless, unless we find further weaknesses in it, it still seems to support powerful conclusions: being dead is neither good nor bad for those who die, and dying is extrinsically good or bad for them only if and insofar as it causes them to have painful (pleasant) experiences. Dying is wholly a matter of indifference for those who do not experience it, say because they sleep through it.
But there are further reservations to consider. Intrinsic hedonism is questionable. So is extrinsic instrumentalism.
Consider the first of these. Which things are intrinsically good or bad for us is a controversial matter , but many theorists deny that the list is limited to pleasure and pain. (For further discussion, see the entry on Intrinsic Goodness, the entry on Preferences, and “What Makes Someone's Life Go Best,” Parfit 1984, pp. 493–502.) Adding more things to the list can undermine the Epicurean argument.
For example, we might adopt some version of preferentialism, or the desire fulfillment account, which is the view that it is intrinsically good for us to fulfill one of our desires (assuming that the desire meets various conditions; exactly what these are is controversial—let us put the matter aside), and it is intrinsically bad for us to have a desire that comes to be thwarted. Now, many of my desires may be fulfilled, and many may be thwarted, without my noticing—desire fulfillment need have not experiential upshot. If I want my child to be happy, and she is, my desire is fulfilled, even if she has travelled away so far from me that I cannot interact with her, now or ever again. So preferentialism blocks the Epicurean’s move from premise 1 to 2.
Preferentialism also blocks the move to 7. Epicureans cannot use extrinsic instrumentalism to deny that a person’s death is extrinsically good or bad for her if the things that are intrinsically good or bad for her are not limited to experiences. Preferentialism implies that things may be extrinsically bad for us by virtue of thwarting our desires, regardless of whether this has any experiential upshot. Suppose, for example, that I desire that my child have a happy upbringing, and, for various reasons, it turns out that I am the only one who can make this happen, but I die suddenly, and as a consequence she has a miserable childhood. Arguably, my untimely death would be bad for me, in that it would thwart my desire, even if I die in my sleep, and am never aware of her fate. (The role a person’s experience plays in her being harmed is discussed by several theorists, including Rosenbaum 1986, Nussbaum 2013, Silverstein 2013, and Fischer 2014.)
Now consider some worries about extrinsic instrumentalism, which says that something is extrinsically good or bad for us only if it causes us to have things that are intrinsically good or bad for us. This view overlooks something that Thomas Nagel (1970) noted in his seminal essay “Death,” namely the fact that things may be extrinsically good or bad for us, other things being equal, by virtue of causing us not to have—by virtue of precluding our having—things that are intrinsically good or bad for us. Consider that being rendered unconscious prior to surgery is extrinsically good for a patient who otherwise would endure great suffering when the physicians apply the knife, in that it keeps him from suffering, and not because it causes him to accrue pleasure or some other good. Of course, after waking, the patient might also accrue pleasure or some other good as an indirect result of having been sedated, but in view of the suffering that it averts, being sedated is extrinsically good for him whether he receives that indirect bonus or not. As well, being made unconscious might be extrinsically bad for a person, say when it precedes, not surgery, but rather some joyous occasion he will miss because he is not conscious while it occurs. It is extrinsically bad for him, in this case, because it prevents him from taking joy in the occasion he misses. This remains true whether or not he also accrues some pain or other intrinsic evil as an indirect result of being sedated.
If it is indeed the case that things may be extrinsically good (bad) for us, other things being equal, by virtue of precluding our having evils (goods), we will want to allow for this fact in settling on an adequate understanding of what makes things good or bad for us. Next let us consider how this might be done, and the implications for the harm thesis.
To argue that death may be bad for those who die (even if they do not experience dying), theorists typically draw upon some version of the comparativist view that we are harmed by what makes our lives as wholes worse than they otherwise would be, and benefitted by what makes our lives as wholes better than they otherwise would be (early proponents of this view include Nagel 1970, Quinn 1984, and Feldman 1991). Applying comparativism, we may claim that, in at least some cases, dying at a time makes our lives as wholes worse than they would have been had we not died when we did, roughly because, by cutting our lives short, it deprives us of good life. This suggestion about death needs further development, but first let us explain the comparativist view more clearly.
Note that how well off you are at one time is likely to differ from how well off you are at another time. Your welfare level rises and falls over time. (For a discussion of welfare, see the article on Well-Being.) What determines how well off you are at a time, or during an interval of time, are the things you then accrue that are intrinsically good for you, goods such as pleasure, together with the things you then accrue that are intrinsically bad for you, evils such as pain (using the term ‘evil’ as a synonym for ‘bad’). Accruing the former at a time boosts your welfare level during that time, other things being equal, while accruing the latter lowers your welfare level during that time. Your welfare level during an interval of time will be positive if the goods you then accrue outweigh the evils. It will be 0—neither positive nor negative—if and only if you are capable of accruing goods or evils (unlike, say, a shoe, which is incapable of faring well or ill) but the goods you accrue are exactly offset by the evils and vice versa. The welfare level resulting from the goods and evils you accrue over the course of your life we may call your lifetime welfare level .
Using the notion of a lifetime welfare level, let us formulate an account of what it is for something to be extrinsically good or bad for us. Let us say that something is extrinsically good (bad) for us if and only if, and to the extent that, it is overall good (bad) for us simpliciter , where:
an event is overall good (bad) for us simpliciter if and only if, and to the extent that, it makes our lifetime welfare level higher (lower) than it otherwise would be.
(Why add the term ‘simpliciter’? Read on.) By way of illustration, consider a typical case in which you receive treatment by a dentist. Let us assume that, on this particular occasion, the dentist fills a cavity in one of your teeth, and that, had you not received this treatment, your tooth would have decayed, painfully, for months, until finally you would have sought out proper treatment. So the salient difference between your lifetime welfare level in the situation in which you are treated right away, on one hand, and the lifetime welfare level you would have in the case that you were not treated until much later, on the other, is that, in the latter situation, that level is significantly lower, due to the pain you would incur. Hence, on these assumptions, receiving treatment was overall good for you: the greater that pain would have been, the better for you it was that you were treated.
Note that things that are overall good for you may be a mixed bag—they may bring some pain or other intrinsic evils in their wakes, as well as some intrinsic goods, and the mix may differ from time to time. In some cases, what is overall good for you simpliciter is overall bad for you in a temporally relative sense—overall bad for you during some period of time . And although it is overall bad for you during one period of time, it might be overall good for you during some other period of time. Let us elaborate upon this point briefly. Comparativists can say that:
an event is overall good (bad) for us at some time t if and only if, and to the extent that, it makes our lifetime welfare level higher (lower) at t than it otherwise would be.
Suppose, for example, that, while your tooth’s cavity is being filled, the dentist’s drill causes you pain, and that this is pain you would not have had if you had not sought treatment, and instead watched TV. In that case, your visit to the dentist is overall bad for you during the time your tooth is being repaired. Yet, as emerged earlier, your visit to the dentist is overall good for you simpliciter , insofar as it enables you to reduce the episodes of toothache you would suffer over the course of your life.
Comparativists can accept intrinsic hedonism, but need not. They could, for example, pair comparativism with some version of the preferentialist view (mentioned earlier) that getting what we want—fulfilling one of our desires—is intrinsically good for us, and having our desires thwarted is intrinsically bad for us. Comparativism is neutral on the issue of what counts as the intrinsic goods and evils. Theorists who conclude that things other than pleasure are intrinsically good for us will want to weigh them in when they assess an individual’s welfare level. For example, preferentialists can say that even if accruing pleasure boosts a person’s welfare level so does desire fulfillment.
According to comparativism, a person’s death, whether painful or not, may well be overall bad for her (and hence extrinsically bad for her). To decide whether a person’s death is overall bad for her simpliciter (usually we can drop ‘simpliciter’ without creating confusion) we compare her actual lifetime welfare level to the lifetime welfare level she would have had if she had not died. Suppose, for example, that Hilda died (painlessly) on December 1, 2008 at age 25 and that, had she not died, she would have gone on to prosper for 25 years—her welfare level during that time would have been high—then suffer during her final five years. Her overall welfare level over her final 30 years would have been high, despite the downturn during the last five. Hence her lifetime welfare level had she not died at age 25 is significantly higher than her lifetime welfare level would be upon dying at 25. The former is boosted by the many goods she accrues during her final 30 years, and these goods are absent from her lifetime welfare level as it would be were her life ended at age 25. Hence dying at 25 is overall bad for her.
Importantly, dying at a time is not overall bad for everyone who dies. In fact, it will be overall good in many cases. Imagine that, had she not died at age 25, Hilda would have fared badly for 25 years—her welfare level during that time would have been low. We might also suppose that, during her last five years her welfare level would have been positive. Despite this last stipulation concerning her final five years, her lifetime welfare level had she not died at 25 is significantly lower than her lifetime welfare level would be if she did die at 25, so, on our new assumptions, dying at 25 is overall good for her.
According to comparativism, when a death is bad for us despite not making us accrue intrinsic evils such as pain, it is bad for us because it precludes our coming to have various intrinsic goods which we would have had if we had not died. We might say that death is bad for us because of the goods it deprives us of, and not, or at least not always, because of any intrinsic evils for which it is responsible. This stance is sometimes called deprivationism , and its proponents deprivationists .
As promising as it is, however, there may be grounds for doubting that comparativists can give the harm thesis a deprivationist defense. Let us discuss one such doubt next.
4. The Timing Puzzle
If we cannot identify a time when something makes us worse off than we otherwise would be, we might well doubt that it really was bad for us. We might go so far as to say that what never makes us worse (better) off than we otherwise would be is not bad (good) for us. Call this the Epicurean presumption . Given this presumption, proponents of the harm thesis need an answer to the timing question , which asks: if death is bad for us, at what time (or times) does it make us worse off than we otherwise would have been? In some cases in which things are bad for us, it seems rather easy to identify times when we are made worse off, but in other cases, especially in some cases involving death, it seems more difficult, which may make us worry about the deprivationist defense of the harm thesis. All this needs elaboration.
If having something is intrinsically bad for us, it is bad for us—because it is intrinsically bad for us—while we have it. Moreover, if something is overall bad for us wholly by virtue of making us have things that are intrinsically bad for us, we can say that it makes us worse off while we have those evils. For example, coming to be infected with a flu virus is overall bad for us, and the time it makes us worse off is not when we come to be infected, but rather while we are sick, while we suffer. (If we came to be infected with a virus, and our immune system dealt with it, preventing our becoming sick, the infection would not be bad for us.) This line of thought suggests that a painful death makes us worse off while we die, or rather while dying is painful for us. What about a painless death? Might it also be bad for us? (If so, when are we made worse off?) Perhaps; more on that in a bit.
We can use the term concurrentism for the view that a bad death makes us worse off while we die.
If we reject intrinsic hedonism, we might conclude that death can make us worse off not just while we die but at other times as well. If we adopt some form of preferentialism, we can take the view that things may make us worse off at the time one of our desires is thwarted. Suppose that, as George Pitcher (1984) suggested, a desire that you have now may be thwarted by your death, even though you will die several months from now. In that case, it might be now that your death makes you worse off than you would have been had you not died. Pitcher’s assumptions suggest that priorism is true: death may make you worse off before you die. It may harm you retroactively.
Identifying a time something makes us worse off seems rather easy in cases, such as the examples of infection or thwarted desire, in which it brings us have pain or other things that are intrinsically bad for us. But what about cases in which something is bad for us due to the fact that it precludes our having things that are intrinsically good for us? In cases like this, the victim incurs deprivation harm . But at what time are such persons worse off than they otherwise would be? When, in particular, does dying painlessly make a person worse off?
Is it possible to defend a concurrentist answer to this question about death? Julian Lamont (1998) says we incur deprivation harm at the time some event ensures that we will not retain or attain some good that is otherwise available. Call such an event an ensuring event . Death may itself be an ensuring event, he thought, so death and deprivation harm may occur simultaneously.
But this suggestion appears doubtful. Recall the earlier case in which we come to be infected and only later experience any symptoms. The event of coming to be infected is overall bad for us, but it seems implausible to say that this makes us worse off than we otherwise would be at the time we are infected . Instead, it seems, coming to be infected makes us worse off later, while we are sick. We are unlikely to adopt concurrentism as our story concerning catching the flu, which makes it doubtful as our story concerning deprivation harm.
In cases like catching the flu, it makes sense to say that the offending event is bad for its victim after it occurs—while she is incurring intrinsic evils she otherwise would lack. Perhaps the same is true of deprivation harm. Recall the example, discussed earlier, in which being sedated at time t is bad for a person due to the fact that it deprives her of good things: in this example, it seems, being sedated makes her worse off than she otherwise would be at a time after t —at the time when she would have been enjoying those goods had she not been sedated. Can we extend this story to the deprivation harm for which a victim’s death is responsible? Does a person’s death makes her worse off than she otherwise would be after she dies—during the time when she would have been enjoying the goods of which her death has deprived her, had she not died? Call this stance subsequentism . Proponents of subsequentism include Neil Feit (2002) and Ben Bradley (2004, 2009).
Subsequentism is plausible only if we can make good sense of the welfare level someone occupies while dead, but this may not be possible. There are at least two problems to discuss.
One difficulty is the problem of the subject . Suppose we are terminators rather than anti-terminators (discussed in Section 2.6). Suppose, too, that you die at time t 1 but had you not you would have experienced joy at time t 2 . Time t 2 arrives while you are dead, so that, given the termination thesis, t 2 arrives while you no longer exist. Consider the property, lacks joy . Does it make sense to attribute this (or any other) property to you at t 2 ? Does it make sense to say that some subject has a property at a time when that subject does not exist? If not, it seems difficult to make sense of your having a welfare level then. Epicurus seemed to be thinking along these lines when he wrote that “death is nothing to us, since when we are, death is not, and when death is present, then we are not.” (Echoing Epicurus, Nagel 1970 wrote “So long as a person exists, he has not yet died, and once he has died, he no longer exists; so there seems to be no time when death, if it is a misfortune, can be ascribed to its unfortunate subject.” But if this is the reason we cannot ascribe misfortune to a victim of death then we cannot even ascribe death to any victim.)
It might seem possible to solve the problem of the subject by simply switching sides and becoming anti-terminators, but this will not work. Anti-terminators can say that it is a straightforward matter to attribute the property lacks joy to you at t 2 , since you still exist at t 2 . You are your (joyless) corpse at t 2 . This won’t work because you might die and go out of existence without leaving a corpse, and even if you leave a corpse it might rot away, taking you out of existence, well before time t 2 arrives. Both possibilities are consistent with the fact that, had you not died when you did, at t 1 , you would have experienced joy at t 2 .
Still, there are more promising strategies for solving the problem of the subject. Subsequentists might adopt a view that is sometimes called metaphysical eternalism (defended by Nagel 1970 and Silverstein 1980, among others). On this view, past and future objects are ontologically on a par with present objects. Existing things are spread out in both space and time. Suppose it is possible to refer to anything that is ontologically on a par with present objects. Then, given metaphysical eternalism, we can still refer to Socrates, even though ‘Socrates’ refers to something whose existence is temporally located wholly in the past, and say of him that he is not alive. For similar reasons, perhaps, we can also attribute the property lacks joy to a person, such as Socrates, whose existence is over.
However, even if they can solve the problem of the subject, and make sense of attributing properties to subjects who are dead, subsequentists face another difficulty: it seems confused to speak of how well off a subject is during times when she is dead. Now, it does make sense to attribute the property lacks joy to a corpse, and to a person who has stopped existing. Anti-terminators will add that a person will have this property— lacks joy —while she is a corpse. But it makes no sense to ask how well off a person is while she is a corpse or during some time after she has stopped existing altogether. The concept of faring well or ill does not apply to things like concrete blocks and corpses or to persons while they are corpses. Things that do fare well or ill may pass through periods of time when they have a level of welfare that is equal to 0—during those times they are capable of accruing goods or evils but do neither—but unlike them, bags of concrete are not capable of having any welfare level, not even a level of 0. The same seems true of a corpse. And the same seems true of us during such times as we are no longer alive—times when we have become corpses or when those corpses have turned to dust.
Many theorists who reject subsequentism assume that because death takes a person out of actual existence, the dead are not “there” to be harmed. Palle Yourgrau (2019) rejects this assumption. He combines modal realism (the view that, like the actual world, other possible worlds are concrete objects) with the thesis of transworld identity (one and the same object exists in more than one possible world), and says that although a dead person no longer exists in the actual world, one and the same person is still alive, and exists, in other possible worlds. We may deny that, after a person has died, she is no longer real at all—not “there” to be harmed—because she still exists in other worlds, according to Yourgrau.
Some (Nagel 1970; Silverstein 1980) suggest that death harms us but at no determinate time. This view is criticized by Julian Lamont (1998) on the grounds that it implies that some events take place but at no particular time. But William Grey (1999) counters that Lamont has misunderstood Nagel’s (and Grey’s) indefinitist position, which is that the harm death causes is incurred during a stretch of time that has blurry boundaries (compare: the time of the onset of baldness).
As Grey understands it, indefinitism is correct only if subsequentism, priorism or concurrentism is true (Grey opts for subsequentism), for even a period of time with blurry edges must occur before, after or at the same time as a mortem event (eternalism is an exception since an infinite period has no boundaries to blur).
Suppose we conclude that there just is no (stretch of) time, whether with blurry edges or not, at which we are made worse off than we otherwise would be by a death that precludes our having goods we otherwise would have. Given the Epicurean presumption, we would have to conclude that it is not bad for us to be deprived of such goods by death. But of course we need not accept this conclusion. We can instead reject the Epicurean presumption. Being deprived of goods by death is bad for us, we can say, if, and insofar as, it is overall bad for us simpliciter , and to be overall bad for us simpliciter , there need not be a time at which death makes us worse off than we otherwise would be. There need be no time at which death makes our welfare level lower than it otherwise would be. Death can preclude our enjoying years of pleasant activities, making our lives worse than they would have been had we not died, even if at no time we are worse off than we would be had our lives not been cut short.
Isn’t it still possible to raise a question about timing, namely: if death is overall bad simpliciter for those who are deprived of happy years, at what time is it bad for them? This question does indeed arise, but it is not the timing question we have been asking, and an answer to the one is not an answer to the other. The answer to the new question is this: if true at all, the proposition that death is overall bad for us simpliciter is an eternal, a timeless, truth (Feldman 1991). A timeless truth is a proposition that is true at all times if true at all. That 6 is less than 7 is an example. That the welfare level Harry accrued today is lower than the welfare level Mary accrued today is another example. And so is the proposition that Sam’s death is overall bad for him simpliciter . It amounts to the claim that Sam’s actual lifetime welfare level is lower than the lifetime welfare level Sam would have accrued had he not died. Jens Johansson (2013) coined the term atemporalism for the view that “death is bad for the deceased but not at any time.” (For further discussion of atemporalism see Lamont 1998, Silverstein 2000 and Feit 2002.)
5. Further Reservations Concerning the Harm Theses
Before we move on, let us consider some further objections to the harm thesis and the deprivationist defense of it.
Another worry about the deprivationist defense is that deprivationism appeals to comparativism, and comparativism says that an event or state of affairs harms me, in that it is bad for me, when my life would have been better for me, my lifetime welfare higher, had that that event not occurred. However, there seem to be exceptions.
I am not harmed, it seems, by failing to be brilliant, or rich and beautiful. But compare my life as it is, with my unimpressive IQ, income and looks, to my life as it would be were I brilliant or rich or beautiful: the former is considerably worse than the latter. My not being a genius (or rich and so forth) precludes my coming to have many goods. It makes my life worse than it otherwise would be, so comparativism seems to imply that not being a genius is bad for me. Suppose you have the winning Mega Millions jacpot ticket, and you decide to give it to me. Before you hand it over, you have a stroke and die. Has your death harmed me?
Epicureans might renew their attack on the harm thesis by exploiting examples like these. The examples appear to show that things can have enormous negative value for me without harming me. Similarly, Epicureans might insist, the preclusion of goods by death is harmless: cut short, my life is worse than it would be were I not to die, but this comparative difference does not show that I am harmed.
It seems that the comparative criteria work well when we evaluate losses, such as the loss of my arms, and also when we evaluate some lacks, such as the inability to see or to feel pleasure. But, arguably, the criteria have worrisome implications when we evaluate certain other lacks, such as my lack of genius. It is relatively clear that a person is harmed by the inability to see but less clear that he is harmed by the lack of genius. Why is that?
Nagel seems inclined to think that the solution is to “set some limits on how possible a possibility must be for its nonrealization to be a misfortune,” but also mentions that we might not regard, as a misfortune, “any limitation, like mortality, that is normal to the species.” Draper suggests that harmless preclusion involves cases in which the events or states of affairs that would be good for us if they held are highly improbable (Draper 1999). Another explanation might focus on the relative importance of having some goods rather than others. In some moods, we may consider it harmful to be deprived of a good just when it is important for us to have it. The troublesome lacks we have been discussing might be lacks of goods it is unimportant to have; such lacks would not be harmful even though we would be better off without them. (But if, against all odds, a person is a genius, or rich, or beautiful, would taking these away be harmless to her?)
5.2 The Symmetry Argument
Lucretius, a follower of Epicurus, extended Epicurus’s case against the harm thesis. The argument he developed involved a thought experiment:
Look back at time … before our birth. In this way Nature holds before our eyes the mirror of our future after death. Is this so grim, so gloomy? (Lucretius 1951)
According to his symmetry argument, it is irrational to object to death, assuming it ends our existence, since we do not find it objectionable that we failed to exist prior to being alive, and the way things were for us while not existing then is just like the way things will be for us after death ends our existence; our pre-vital nonexistence and our posthumous nonexistence are symmetrical, alike in all relevant respects, so that any objection to the one would apply to the other.
Lucretius’s argument admits of more than one interpretation, depending on whether it is supposed to address death understood as dying or as being dead (or both).
On one interpretation, the argument is this: the ending of life is not bad, since the only thing we could hold against it is the fact that it is followed by our nonexistence, yet the latter is not objectionable, as is shown by the fact that we do not object to our nonexistence before birth. So understood, the symmetry argument is weak. It would have some force for someone who thought initially that death puts us into a state or condition that is ghastly, perhaps painful, but that need not be our complaint. Instead, our complaint might be that death precludes our having more good life. Notice that the mirror image of death is birth (or, more precisely, becoming alive), and the two affect us in very different ways: birth makes life possible; if a life ends up being good for us, birth starts a good thing going. Death makes further life impossible; it brings a good thing to a close.
Perhaps Lucretius only meant to argue that being dead is not bad, since the only thing we could hold against it is our nonexistence, which is not really objectionable, as witness our attitude about pre-vital nonexistence. So interpreted, there is a kernel of truth in Lucretius’s argument. Truly, our pre-vital nonexistence does not concern us much. But perhaps that is because our pre-vital nonexistence is followed by our existence. Perhaps we would not worry overly about our post-vital nonexistence if it, too, were followed by our existence. If we could move in and out of existence, say with the help of futuristic machines that could dismantle us, then rebuild us, molecule by molecule, after a period of nonexistence, we would not be overly upset about the intervening gaps, and, rather like hibernating bears, we might enjoy taking occasional breaks from life while the world gets more interesting. But undergoing temporary nonexistence is not the same as undergoing permanent nonexistence. What is upsetting might be the permanence of post-vital nonexistence—not nonexistence per se.
There is another way to use considerations of symmetry against the harm thesis: we want to die later, or not at all, because it is a way of extending life, but this attitude is irrational, Lucretius might say, since we do not want to be born earlier (we do not want to have always existed), which is also a way to extend life. As this argument suggests, we are more concerned about the indefinite continuation of our lives than about their indefinite extension . (Be careful when you rub the magic lamp: if you wish that your life be extended, the genie might make you older!) A life can be extended by adding to its future \(or\) to its past. Some of us might welcome the prospect of having lived a life stretching indefinitely into the past, given fortuitous circumstances. But we would prefer a life stretching indefinitely into the future.
Is it irrational to want future life more than past life? No; it is not surprising to find ourselves with no desire to extend life into the past, since the structure of the world permits life extension only into the future, and that is good enough. But what if life extension were possible in either direction? Would we still be indifferent about a lengthier past? And should our attitude about future life match our attitude about past life?
Our attitude about future life should match our attitude about past life if our interests and attitudes are limited in certain ways. If quantity of life is the only concern, a preference for future life is irrational. Similarly, the preference is irrational if our only concern is to maximize how much pleasure we experience over the course of our lives without regard to its temporal distribution. But our attitude is not that of the life- or pleasure-gourmand.
According to Parfit, we have a far-reaching bias extending to goods in general: we prefer that any good things, not just pleasures, be in our future, and that bad things, if they happen at all, be in our past. He argues that if we take this extensive bias for granted, and assume that, because of it, it is better for us to have goods in the future than in the past, we can explain why it is rational to deplore death more than we do our not having always existed: the former, not the latter, deprives us of good things in the future (he need not say that it is because it is in the past that we worry about the life-limiting event at the beginning of our lives less than the life-limiting event at the end). This preference for future goods is unfortunate, however, according to Parfit. If cultivated, the temporal insensitivity of the life- or pleasure-gourmand could lower our sensitivity to death: towards the end of life, we would find it unsettling that our supply of pleasures cannot be increased in the future, but we would be comforted by the pleasures we have accumulated.
Whether or not we have the extensive bias described by Parfit, it is true that the accumulation of life and pleasure, and the passive contemplation thereof, are not our only interests. We also have active, forward–looking goals and concerns. Engaging in such pursuits has its own value; for many of us, these pursuits, and not passive interests, are central to our ‘identities’, our fundamental values and commitments. However, we cannot make and pursue plans for our past. We must project our plans (our self–realization) into the future, which explains our forward bias. (We could have been devising and pursuing plans in the past, but these plans will not be extensions of our present concerns.) It is not irrational to prefer that our lives be extended into the future rather than the past, if for no other reason than this: only the former makes our existing forward-looking pursuits possible. It is not irrational to prefer not to be at the end of our lives, unable to shape them further, and limited to reminiscing about days gone by. As Frances Kamm (1998, 2021) emphasizes, we do not want our lives to be all over with.
Nevertheless, it does not follow that we should be indifferent about the extent of our pasts. Being in the grip of forward-looking pursuits is important, but we have passive interests as well, which make a more extensive past preferable. Moreover, having been devising and pursuing plans in the past is worthwhile. If fated to die tomorrow, most of us would prefer to have a thousand years of glory behind us rather than fifty. We want to have lived well.
In “Death” Thomas Nagel offered a response to Lucretius that has been widely discussed. It is entirely reasonable not to want to come into existence earlier even though we want to live longer, Nagel said, because it is metaphysically impossible for a person to have come into existence significantly earlier than she did, even though it is possible for a person to have existed longer than she actually did. However, his response hinges on questionable assumptions about the essential features of people’s origins, as Nagel acknowledges (in footnote 3 of the reprint of “Death” in his collection Mortal Questions .) Imagine someone who originated from a zygote that had been frozen for a very long time. Mightn't that zygote have been frozen for a brief time instead? Wouldn’t that be a way for this person to have come into existence far earlier than she did?
According to Frederik Kaufman (2016, p. 63), this thought experiment (perhaps tweaked a bit) might provide a way in which a human organism could have come into existence far earlier than she did, but it does not provide a way in which a person could have come into existence far earlier. “Persons (properly understood) cannot exist earlier than they do.” He bases this view on the assumption—challenged by animalists but defended by Parfit—that persons are objects (distinct from organisms) with psychological persistence conditions, chief among which is psychological continuity, together with the assumption that “if mental continuity is constitutive of personal identity, then when a particular consciousness emerges is essential to that person.”
6. Posthumous Harm
According to Aristotle,
a dead man is popularly believed to be capable of having both good and ill fortune—honour and dishonour and prosperity and the loss of it among his children and descendants generally—in exactly the same way as if he were alive but unaware or unobservant of what was happening ( Nicomachean Ethics 1.10)
The belief Aristotle reported in this passage is that a person may be benefitted or harmed by things that happen while she is dead. Nagel (1970, p. 66) agrees; drawing upon his indefinitist approach he says that “a man's life includes much that does not take place within the boundaries … of his life” and that “there is a simple account of what is wrong with breaking a deathbed promise. It is an injury to the dead man.” If something that occurs while a person is dead is bad for her, let us say that it is responsible for posthumous harm . (But this way of speaking is potentially misleading, as theorists who argue that posthumous events may harm us need not assume that the victims are worse off while they are dead.) Is there such a thing as posthumous harm?
The main reason to doubt the possibility of posthumous harm is the assumption that it presupposes the (dubious) possibility of backwards causation. As Ernest Partridge wrote, “after death no events can alter a moment of a person's life” (1981, p. 248). The dead may be wronged, Partridge thought, but being wronged is not a kind of harm. (The claim that a person may be wronged by actions others take after she is dead is itself quite controversial. Like Partridge, some theorists think that people may be wronged but not harmed posthumously. Priorists typically argue that both are possible, while other, theorists, such as J.S. Taylor 2012, argue that neither is possible.)
We might also question the possibility of posthumous harm by drawing on the assumption (made by Mark Bernstein 1998, p. 19, and Walter Glannon 2001, p. 138, among others) that something is intrinsically good or bad for a person only if it reduces to her intrinsic, non-relational properties. For simplicity, we can focus on one version of this view, namely intrinsic hedonism. Suppose we assume that a person is harmed only by what is intrinsically or extrinsically bad for her, that intrinsic hedonism is the correct account of intrinsic harm and comparativism is the correct account of extrinsic harm, and also that the termination thesis (people do not exist while dead) is true. On these assumptions, it is impossible for an event that occurs after a person dies to be bad for her. It cannot be bad for her in itself and it cannot be overall bad for her either. To be overall bad for a person, a posthumous event would have to make her have fewer goods or more evils or both than she would have had if that event had not occurred. But nothing that happens after a person dies and ceases to exist has any bearing on the amounts of pleasure or pain in her life. Nothing that occurs after she ceases to exist modifies any of her intrinsic properties.
Although the above assumptions rule out the possibility of posthumous harm, they are entirely consistent, we have seen, with the possibility of mortal harm, the possibility that people are harmed by dying. (We might think otherwise if, as some theorists do, we assume that a person no longer exists at the time she dies. Joel Feinberg 1984, following Barbara Levenbook 1984, defined death as “the first moment of the subject’s nonexistence,” which makes death something that occurs after a person has ceased to exist, and suggests that by ruling out the possibility that a person is harmed by things that occur after she ceases to exist we rule out the possibility of mortal harm.)
Those who defend the possibility of posthumous harm deny that it involves backwards causation. But how could posthumous events affect people if not via backwards causation?
Some theorists say that posthumous harm occurs when posthumous events change the value of a person’s life for the worse. Dorothy Grover (1989) suggests that posthumous events may affect the “quality” of a person's life, say by changing the value of her accomplishments. David Velleman (1991) argues along similar lines, claiming that later events may affect the meaning of earlier events, and the latter bears on the value of a person’s life.
Some theorists (for example, Pitcher 1984, Feinberg 1984, Luper 2004 and 2012, and Scarre 2013) appeal to preferentialism to explain the possibility of posthumous harm. We noted earlier that preferentialists can defend the idea that some events harm their victims retroactively, and that death is such an event. Preferentialists can take a similar stance on posthumous events, assuming that things that happen after we die may determine whether desires we have while alive are fulfilled or thwarted.
According to Pitcher, posthumous events harm us by being responsible for truths that thwart our desires. For example, being slandered while I am dead makes it true that my reputation is to be damaged, and this harms me at all and only those times when I desire that my reputation be untarnished. It is while I am alive that I care about my reputation’s always being intact, and it is while I am alive that my well-being is brought lower by posthumous slander. Similarly, my desire that my child have a happy upbringing even if I am not there to provide it will be thwarted if, after I die, she catches some devastating illness. The event that makes it true that my child will be miserable occurs after I am gone, but this truth thwarts my desire about my child now, so it is now that I am worse off. The posthumous events themselves harm me only indirectly; directly I am harmed by their making things true that bear on my interests.
However, the desire-based case for the possibility of posthumous harm remains controversial. It will be rejected by theorists who doubt that people are harmed by events that do not modify their intrinsic features, and by theorists who think that it hinges on the possibility of backwards causation, of course. Velleman (1991, p. 339) rejects the desire-based case on the grounds that “we think of a person's current well-being as a fact intrinsic to the present, not as a relation that he currently bears to his future.” Some theorists echo a criticism that was offered by Partridge (1981, p. 246). Consider an event that thwarts one of a person's desires. To harm her by virtue of thwarting that desire, Partridge claims, the event must occur while she still has that desire , while she still cares about whether it is fulfilled, but she and her desire are gone by the time a posthumous event occurs. For some theorists (Vorobej, 1998, Suits 2001), the point is that we have no reason to care whether our desires are fulfilled by events that occur once we no longer have those desires, and we no longer have desires after we die. Parfit resisted this charge by noting that while some of our desires are conditional on their own persistence (we want them fulfilled at a time only on condition that we will still have them at that time), others are not.
7. Never Dying
Is it always a misfortune for us to die? Would never dying instead be bad for us? In a pair of influential essays, Thomas Nagel defends an affirmative answer to the first question, while Bernard Williams defends an affirmative answer to the second.
In “Death” (and in The View From Nowhere , p. 224) Nagel argues that no matter when it happens, dying is bad for those who die. He bases this view on the claim that “life is worth living even when the bad elements of experience are plentiful and the good ones too meager to outweigh the bad ones on their own. The additional positive weight is supplied by experience itself, rather than by any of its contents.” (1970, p. 60) Nagel’s view appears to be that it is intrinsically good for us to experience things, and that this good is great enough to outweigh any evils that accompany it. Hence a person’s welfare level is positive at any time when she is experiencing things, and no matter how much misery continued existence will bring her, it is overall good for her to live longer, assuming that she continues to experience things. (Nagel does not argue that being deprived of continued life would be a misfortune if that life were entirely devoid of experience.)
Nagel considers objections to his view towards the end of his essay. One might argue, Nagel points out (as noted earlier), that mortality is not a misfortune on the grounds that the nonrealization of remote possibilities (like being immortal) is not harmful, or on the grounds that limitations that are normal to the species (like mortality) are not harmful. He responds that the normality and inevitableness of death “do not imply that it would not be good to live longer.” Whenever death comes, it would have been good to live longer, so it is bad for us that we will not: “if there is no limit to the amount of life that it would be good to have, then it may be that a bad end is in store for us all.” (1970, p. 69)
Nagel’s case for saying that death is always bad for those who die rests on his claim that the goodness of experiencing outweighs any accompanying evils. However, the latter is implausible, as is evident to anyone who would rather be sedated into unconsciousness than undergo the suffering she would otherwise experience during surgery. Under such circumstances, sedation is overall good for us, despite the fact that (indeed: because) it stops us from experiencing things for a time. And once this is acknowledged, it seems reasonable to add that, under certain circumstances, dying would be overall good for us, and hence not bad for us after all. It would be overall good for us if the further life we otherwise would have would bring us great evils, such as suffering, that are not offset by goods.
Bernard Williams (and others, such as Shelly Kagan 2012) takes the view that it would be bad to live forever, even under the best of circumstances. In his influential essay “The Makropulos Case: Reflections on the Tedium of Immortality,” Williams argues that although the deaths of some persons is a misfortune for them, never dying would be intolerable. In arguing for these views, Williams draws upon the notion of a categorical desire, which we can clarify as follows.
Consider a woman who wants to die. She might still take the view that if she is to live on, then she should be well fed and clothed. She wants food and clothing on condition she remain alive. In this sense her desires (for food and clothes) are conditional on her remaining alive, and, in being conditional on her living on, they do not give her reason to live. Contrast a father who desires that his beloved daughter have a good start in life. His desire is not conditional on his remaining alive. In this sense, it is, Williams says, categorical. In fact, his desire gives him reason to live, because he can see to her well-being if he survives. Williams thinks that our categorical desires are not only what motivate us to live on, they give meaning to our lives, and are important elements of our characters. He also thinks that it is by virtue of the fact that we will retain the same character until a later time that it is clear to us that we will be the same person until then.
The bearing on death, according to Williams, is, first, that we have good reason to condemn a death that is premature in the sense that it thwarts our categorical desires. Second, mortality is good, for if we live long enough, eventually we will lose our categorical desires. At that point we will no longer be motivated to live on, and oppressive boredom will set in. When we contemplate this fate from our vantage point in the present, we find it that it is not even clear to us that these bored seniors are us.
If we could find a way to extend our lives indefinitely, yet avoid the ravages of senescence, and remain healthy and mentally competent, couldn’t we avoid becoming jaded with life by gradually varying our interests over time, adding to and perhaps replacing some of our categorical desires, again and again? Several theorists including Nagel (1986, p. 224, n. 3), Glover (1977, p. 57), and Fischer (1994), have argued that the lives of superseniors need not become dull and tedious. Williams’s view is that it is not possible to make eternal life desirable (which claim is not identical to the claim that eternal life would inevitably be bad for us). Varying my categorical desires will not work, because, to be desirable, the endless life I design for myself must meet two conditions: (1) “it should clearly be me who lives forever,” and (2) “the state in which I survive should be one that, to me looking forward, will be adequately related, in the life it presents, to those aims I now have in wanting to survive at all.” (1973, p. 83) If I replace my categorical desires, I fall afoul of at least one of these conditions. Life under the future desires is detached from life under my current categorical desires. Moreover, the desires I give myself in the future will be elements of a character that is very different from my current character; replacing my current character with an entirely different one later in life makes it far less clear, Williams appears to think, that the individual living that later life is me. “The degree of identification needed with the later life … is absolutely minimal.” (1973, p. 85)
Williams’s claim that immortality cannot be made desirable remains controversial. It is not obvious that eternal life is undesirable if it involves changing our categorical desires and characters (insofar as our characters are defined by the desires). Nor is it obvious that such changes must violate Williams’s two conditions for the desirability of continued life. Williams seems to think that the individual who is changed in this way will not clearly be the same person as before, but he stops short of saying that it clearly will not be the same person (indeed, he defends a bodily continuity criterion for identity in “The Self and the Future,” pp. 46–63, so he presumably thinks that a person does survive changes of desires and character). Concerning Williams’s second condition, his view is that if we replace our characters and desires, “there is nothing left by which he can judge” whether future life is desirable (1093, p. 85). Yet it seems reasonable to take the view now that it would be good for me to develop and fulfil desires in the future—desires I now lack. Many of us would welcome the prospect of gradually transforming our interests and projects over time. The gradual, continuous transformation of our desires and projects does not end our lives, or existence. It is distinct from, and preferable to, annihilation. If we could live endlessly, the stages of our lives would display reduced connectedness, yet remain continuous, which is a property that is important in the kind of survival most of us prize. Even after drinking from the fountain of eternal youth, we would tend to focus on relatively short stretches of our indefinitely extensive lives, being animated by the specific projects and relationships we have then. However, sometimes we would turn our attention to long stretches of life, and then, prizing continuity, we might well phase in new and worthwhile undertakings that build upon, and do not wholly replace, the old. (For further discussion of the desirability of eternal life, see Overall 2003, Bortolotti 2009, Smuts 2011, Luper 2012b, Altshuler 2016, Buben 2016, Cholbi 2016, and Fischer 2019.)
Even if death is usually bad for those of us who die, perhaps it need not be bad for us, if we prepare ourselves suitably. This might be possible if some form of preferentialism is true, and if, by altering our desires, we could cease to have any interests that dying would impair. For then we might be able to thanatize our desires, in this sense: we might abandon all desires that death might thwart. Among these are desires we can satisfy only if we live on for a few days, but also desires we cannot possibly satisfy within the span of a normal lifetime, and the desire for immortality itself. Instead of desiring that some project of mine succeed, which is a desire that might be thwarted by my death, I might instead adopt a conditionalized version of this desire, namely: should I live on, let my project succeed. If all goes well, thanatizing would insulate us from harm from death by leaving us with no interests with which dying interferes.
Unfortunately, this strategy will backfire. The main problem is that death can interfere with desire fulfillment not just by falsifying the objects of our desires but also by precluding our having desires (Luper 2013). So even if we resolve, from now on, to limit ourselves to desires whose objects cannot be falsified by death, we are still vulnerable to the harm death will do us if it precludes our having and fulfilling desires. Hence thanatizing would force us to avoid having any desires whose fulfillment would have benefitted us, and to deny ourselves such desires would be as bad for us as the harm we are trying to avoid.
However, the core idea of adapting our desires is useful, if not taken to an extreme. It is prudent to avoid taking on goals we cannot possibly attain, and hence prudent to eschew projects that cannot possibly be completed during the course of a normal lifetime.
- Altshuler, R., 2016. “Immortality, Identity, and Desirability,” in Cholbi 2016.
- Bedau, M., 2014. “The Nature of Life” in S. Luper (ed.), The Cambridge Companion to Life and Death , Cambridge: Cambridge University Press.
- Belshaw, C., 2009. Annihilation: The Sense and Significance of Death , Dublin: Acumen Press.
- Bernstein, M. 1998. On moral considerability: an essay on who morally matters , Oxford: Oxford University Press.
- Bortolotti, L., and Nagasawa, Y., 2009, “Immortality Without Boredom,” Ratio , 22 (3): 261–277.
- Braddock, G., 2000. “Epicureanism, Death, and the Good Life,” Philosophical Inquiry , 22 (1–2): 47–66.
- Bradley, B., 2004. “When Is Death Bad for the One Who Dies?” Noûs , 38: 1–28.
- –––, 2009. Well Being and Death , Oxford: Oxford University Press.
- Bradley, B., Feldman, F., and Johansson, J., eds., 2013. The Oxford Handbook of Philosophy of Death , Oxford: Oxford University Press.
- Cholbi, M. (ed.), 2016. “Immortality and the Philosophy of Death,” New York: Rowman & Littlefield.
- DeGrazia, D., 2014. “The Nature of Human Death” in S. Luper (ed.), The Cambridge Companion to Life and Death , Cambridge: Cambridge University Press.
- Draper, K., 1999. “Disappointment, Sadness, and Death,” Philosophical Review , 108: 387–414.
- Driesch, H., 1908. The Science and Philosophy of the Organism (The Gifford Lectures delivered before the University of Aberdeen in the year 1907), London: Adam and Charles Black.
- –––, 1914. The History and Theory of Vitalism , C. K Ogden (trans.), London: MacMillan and Co.
- Epicurus, Epicurus: The Extant Remains , Cyril Bailey (ed.), Oxford: Clarendon Press, 1926.
- Feit, N., 2002. “The Time of Death’s Misfortune,” Noûs , 36: 359–383.
- Feinberg, J., 1984. The Moral Limits of Criminal Law (Volume 1: Harm to Others), New York: Oxford University Press.
- Feldman, F., 1991. “Some Puzzles About the Evil of Death,” The Philosophical Review , 100: 205–27; reprinted in Fischer 1993, 307–326; [ Reprint available from the author ] (in PDF)].
- –––, 1992. Confrontations with the Reaper , New York: Oxford University Press.
- –––, 2000. “The Termination Thesis,” Midwest Studies in Philosophy , 24: 98–115; [ Preprint available from the author (in PDF)].
- –––, 2013. “Death and the Disintegration of Personality,” in B. Bradley, F. Feldman and J. Johansson, (eds.), The Oxford Handbook of Philosophy of Death , Oxford: Oxford University Press.
- Fischer, J. M. (ed.), 1993. The Metaphysics of Death , Stanford: Stanford University Press.
- –––, 2014. “Mortal Harm” in S. Luper (ed.), The Cambridge Companion to Life and Death , Cambridge: Cambridge University Press.
- –––, 2020. Death, Immortality, and Meaning in Life , Oxford: Oxford University Press.
- Gilmore, C., 2013. “When Do Things Die?” in B. Bradley, F. Feldman and J. Johansson (eds.), The Oxford Handbook of Philosophy of Death , Oxford: Oxford University Press.
- Glannon, W., 2001. “Persons, lives, and posthumous harms,” Journal of Social Philosophy , 32: 127–142. doi:10.1111/0047-2786.00084
- Glover, J., 1977. Causing Death and Saving Lives , Harmondsworth: Penguin Books.
- Green, M. and Winkler, D., 1980. “Brain Death and Personal Identity,” Philosophy and Public Affairs , 9: 105–133.
- Grover, D., 1989. “Posthumous Harm,” The Philosophical Quarterly , 39: 334–353
- Grey, W., 1999. “Epicurus and the Harm of Death,” Australasian Journal of Philosophy , 77: 358–364. doi:10.1080/00048409912349121
- Johansson, J., 2013. “The Timing Problem,” in B. Bradley, F. Feldman and J. Johansson, (eds.), The Oxford Handbook of Philosophy of Death , Oxford: Oxford University Press.
- Kagan, S., 2012. Death , New Haven: Yale University Press.
- Kamm, F.M., 1988. “Why Is Death Bad and Worse than Pre-Natal Non-Existence?” Pacific Philosophical Quarterly , 69: 161–164.
- –––, 1998. Morality Mortality , Volume 1, Oxford: Oxford University Press.
- –––, 2021. Almost over: aging, dying, dead , New York: Oxford University Press.
- Kaufman, F., 2016. “Lucretius and the Fear of Death,” in Cholby 2016, pp. 53–67.
- Lamont, J., 1998. “A Solution to the Puzzle of When Death Harms its Victims,” Australasian Journal of Philosophy , 76: 198–212.
- Levenbook, B., 1984. “Harming Someone After His Death,” Ethics , 94 (3): 407–419.
- –––, 2013. “Welfare and Harm after Death,” in J.S. Taylor (ed.), The Metaphysics and Ethics of Death , Oxford: Oxford University Press.
- Locke, J., 1689. An Essay Concerning Human Understanding .
- Lucretius. On the Nature of the Universe . Latham, reg. trans., Penguin Classics, 1951.
- Luper(-Foy), S., 1987. “Annihilation,” The Philosophical Quarterly , 37 (148): 233–52; reprinted in Fischer 1993; [ Preprint available from the author (in Word)].
- –––, 1996. Invulnerability: On Securing Happiness , Chicago: Open Court.
- –––, 2004. “Posthumous Harm,” American Philosophical Quarterly , 41: 63–72; [ Preprint available from the author (in Word)].
- –––, 2005. “Past Desires and the Dead,” in Philosophical Studies , 126 (3): 331–345; [ Preprint available from the author (in Word].
- –––, 2009. The Philosophy of Death , Cambridge: Cambridge University Press.
- –––, 2012. “Retroactive Harms and Wrongs,” in Fred Feldman, Ben Bradley, and Jens Johansson (eds.), Oxford Handbook of Philosophy of Death , Oxford: Oxford University Press, 317–336.
- –––, 2012b, “Exhausting Life,” The Journal of Ethics: An International Philosophical Review , 16 (3): 1–21.
- –––, 2013. “Adaptation” in J.S. Taylor (ed.), The Metaphysics and Ethics of Death , Oxford: Oxford University Press.
- ––– (ed.), 2014. The Cambridge Companion to Life and Death , Cambridge: Cambridge University Press.
- McMahan, J., 1988. “Death and the Value of Life,” Ethics , 99 (1): 32–61; reprinted in Fischer 1993, 233–266.
- –––, 2002. The Ethics of Killing: Problems at the Margins of Life , New York: Oxford University Press.
- Mill, J.S., 1863. Utilitarianism , London: Parker, Son, and Bourn.
- Nagel, T., 1970. “Death,” Noûs 4(1):73–80, reprinted in Nagel, T., Mortal Questions , Cambridge: Cambridge University Press, 1979, and in Fischer 1993; page references are to Fischer.
- –––, 1986. The View From Nowhere , Oxford: Oxford University Press.
- Nozick, R., 1971. “On the Randian Argument,” The Personalist , reprinted in J. Paul (ed.), Reading Nozick , Totowa, NJ: Rowman & Littlefield, 1981.
- Nussbaum, M., 2013. “The Damage of Death: Incomplete Arguments and False Consolations,” in J.S. Taylor (ed.), The Metaphysics and Ethics of Death , Oxford: Oxford University Press.
- Olson, E., 1997. The Human Animal , Oxford: Oxford University Press.
- –––, 2007. What Are We? A Study in Personal Ontology , Oxford: Oxford University Press.
- Overall, C., 2003. Aging, Death, and Human Longevity: A Philosophical Inquiry , Berkeley: University of California Press.
- Pallis, C., 1982. “ABC of Brain Stem Death,” British Medical Journal , 285: 1487–1490.
- Parfit, D., 1984. Reasons and Persons , Oxford: Clarendon Press.
- Partridge, E., 1981. “Posthumous Interests and Posthumous Respect,” Ethics , 91: 243–64.
- Pitcher, G., 1984. “The Misfortunes of the Dead,” in American Philosophical Quarterly , 21 (2): 217–225; reprinted in Fischer 1993, 119–134.
- Perry, J. (ed.), 1975. Personal Identity , Berkeley: University of California Press.
- President’s Commission, 1981. Defining Death: Medical, Legal, and Ethical Issues in the Determination of Death , Washington, D.C.
- Quinn, W., 1984. “Abortion: Identity and Loss,” Philosophy and Public Affairs , 13 (1): 24–54.
- Rosenbaum, S., 1986. “How to Be Dead and Not Care: A Defense of Epicurus,” American Philosophical Quarterly , 23 (2): 217–25; reprinted in Fischer 1993, 119–134.
- –––, 1989. “Epicurus and Annihilation,” Philosophical Quarterly , 39 (154): 81–90; reprinted in Fischer 1993, 293–304.
- Rosenberg, J., 1983. Thinking Clearly About Death , Englewood Cliffs, NJ: Prentice-Hall.
- Scarre, G., 2013. “The Vulnerability of the Dead,” in J. Stacey Taylor (ed.), The Metaphysics and Ethics of Death: New Essays , Oxford: Oxford University Press, pp. 171–187.
- Schumacher, B., 2010. Death and Mortality in Contemporary Philosophy , Cambridge: Cambridge University Press.
- Silverstein, H., 1980. “The Evil of Death,” Journal of Philosophy , 77 (7): 401–424; reprinted in Fischer 1993, 95–116.
- –––, 2000. “The Evil of Death Revisited,” Midwest Studies in Philosophy , 24: 116–135.
- –––, 2013. “The Evil of Death One More Time: Parallels between Time and Space,” in J.S. Taylor (ed.), The Metaphysics and Ethics of Death , Oxford: Oxford University Press.
- Smuts, A., 2011. “Immortality and Significance,” Philosophy and Literature , 35 (1): 134–149.
- Snowdon, P.F., 1990. “Persons, Animals, and Ourselves,” in C. Gill (ed.), The Person and the Human Mind: Issues in Ancient and Modern Philosophy , Oxford: Oxford University Press.
- Suits, D., 2001. “Why Death Is Not Bad for the One Who Died,” American Philosophical Quarterly , 38 (1): 269–84.
- Taylor, J.S., 2012. Death, Posthumous Harm, and Bioethics , London: Routledge.
- –––, 2013. The Metaphysics and Ethics of Death: New Essays , Oxford: Oxford University Press.
- Unamuno, M., 1913. The Tragic Sense of Life in Men and Nations , A. Kerrigan (trans.), Princeton: Princeton University Press, 1972.
- Van Inwagen, P., 1990. Material Beings , Ithaca: Cornell University Press.
- Velleman, D., 1991. “Well-Being and Time,” Pacific Philosophical Quarterly , 72: 48–77.
- Vorobej, M., 1998. “Past Desires,” Philosophical Studies , 90: 305–318.
- Warren, J., 2004. Facing Death: Epicurus and His Critics , Oxford: Oxford University Press.
- Williams, B., 1973. Problems of the Self , Cambridge: Cambridge University Press.
- –––, “The Makropulos Case: Reflections on the Tedium of Immortality,” in Williams 1973. Reprinted in Fischer 1993. Page references are to Fischer.
- –––, “The Self and the Future,” in Williams 1973.
- Yourgrau, P., 2019. Death and Nonexistence , Oxford: Oxford University Press.
How to cite this entry . Preview the PDF version of this entry at the Friends of the SEP Society . Look up topics and thinkers related to this entry at the Internet Philosophy Ontology Project (InPhO). Enhanced bibliography for this entry at PhilPapers , with links to its database.
- Partridge, E., 1981. “ Posthumous Interest and Posthumous Respect ,” Ethics 91, no. 2. Reprint made available by the author.
death: definition of | Epicurus | euthanasia: voluntary | identity | life | personal identity | suicide | well-being
Copyright © 2021 by Steven Luper < sluper @ trinity . edu >
- Accessibility
Support SEP
Mirror sites.
View this site from another server:
- Info about mirror sites
The Stanford Encyclopedia of Philosophy is copyright © 2023 by The Metaphysics Research Lab , Department of Philosophy, Stanford University
Library of Congress Catalog Data: ISSN 1095-5054
Have a language expert improve your writing
Run a free plagiarism check in 10 minutes, generate accurate citations for free.
- Knowledge Base
- How to Write a Thesis Statement | 4 Steps & Examples
How to Write a Thesis Statement | 4 Steps & Examples
Published on January 11, 2019 by Shona McCombes . Revised on August 15, 2023 by Eoghan Ryan.
A thesis statement is a sentence that sums up the central point of your paper or essay . It usually comes near the end of your introduction .
Your thesis will look a bit different depending on the type of essay you’re writing. But the thesis statement should always clearly state the main idea you want to get across. Everything else in your essay should relate back to this idea.
You can write your thesis statement by following four simple steps:
- Start with a question
- Write your initial answer
- Develop your answer
- Refine your thesis statement
Instantly correct all language mistakes in your text
Upload your document to correct all your mistakes in minutes
Table of contents
What is a thesis statement, placement of the thesis statement, step 1: start with a question, step 2: write your initial answer, step 3: develop your answer, step 4: refine your thesis statement, types of thesis statements, other interesting articles, frequently asked questions about thesis statements.
A thesis statement summarizes the central points of your essay. It is a signpost telling the reader what the essay will argue and why.
The best thesis statements are:
- Concise: A good thesis statement is short and sweet—don’t use more words than necessary. State your point clearly and directly in one or two sentences.
- Contentious: Your thesis shouldn’t be a simple statement of fact that everyone already knows. A good thesis statement is a claim that requires further evidence or analysis to back it up.
- Coherent: Everything mentioned in your thesis statement must be supported and explained in the rest of your paper.
Here's why students love Scribbr's proofreading services
Discover proofreading & editing
The thesis statement generally appears at the end of your essay introduction or research paper introduction .
The spread of the internet has had a world-changing effect, not least on the world of education. The use of the internet in academic contexts and among young people more generally is hotly debated. For many who did not grow up with this technology, its effects seem alarming and potentially harmful. This concern, while understandable, is misguided. The negatives of internet use are outweighed by its many benefits for education: the internet facilitates easier access to information, exposure to different perspectives, and a flexible learning environment for both students and teachers.
You should come up with an initial thesis, sometimes called a working thesis , early in the writing process . As soon as you’ve decided on your essay topic , you need to work out what you want to say about it—a clear thesis will give your essay direction and structure.
You might already have a question in your assignment, but if not, try to come up with your own. What would you like to find out or decide about your topic?
For example, you might ask:
After some initial research, you can formulate a tentative answer to this question. At this stage it can be simple, and it should guide the research process and writing process .
Receive feedback on language, structure, and formatting
Professional editors proofread and edit your paper by focusing on:
- Academic style
- Vague sentences
- Style consistency
See an example

Now you need to consider why this is your answer and how you will convince your reader to agree with you. As you read more about your topic and begin writing, your answer should get more detailed.
In your essay about the internet and education, the thesis states your position and sketches out the key arguments you’ll use to support it.
The negatives of internet use are outweighed by its many benefits for education because it facilitates easier access to information.
In your essay about braille, the thesis statement summarizes the key historical development that you’ll explain.
The invention of braille in the 19th century transformed the lives of blind people, allowing them to participate more actively in public life.
A strong thesis statement should tell the reader:
- Why you hold this position
- What they’ll learn from your essay
- The key points of your argument or narrative
The final thesis statement doesn’t just state your position, but summarizes your overall argument or the entire topic you’re going to explain. To strengthen a weak thesis statement, it can help to consider the broader context of your topic.
These examples are more specific and show that you’ll explore your topic in depth.
Your thesis statement should match the goals of your essay, which vary depending on the type of essay you’re writing:
- In an argumentative essay , your thesis statement should take a strong position. Your aim in the essay is to convince your reader of this thesis based on evidence and logical reasoning.
- In an expository essay , you’ll aim to explain the facts of a topic or process. Your thesis statement doesn’t have to include a strong opinion in this case, but it should clearly state the central point you want to make, and mention the key elements you’ll explain.
If you want to know more about AI tools , college essays , or fallacies make sure to check out some of our other articles with explanations and examples or go directly to our tools!
- Ad hominem fallacy
- Post hoc fallacy
- Appeal to authority fallacy
- False cause fallacy
- Sunk cost fallacy
College essays
- Choosing Essay Topic
- Write a College Essay
- Write a Diversity Essay
- College Essay Format & Structure
- Comparing and Contrasting in an Essay
(AI) Tools
- Grammar Checker
- Paraphrasing Tool
- Text Summarizer
- AI Detector
- Plagiarism Checker
- Citation Generator
A thesis statement is a sentence that sums up the central point of your paper or essay . Everything else you write should relate to this key idea.
The thesis statement is essential in any academic essay or research paper for two main reasons:
- It gives your writing direction and focus.
- It gives the reader a concise summary of your main point.
Without a clear thesis statement, an essay can end up rambling and unfocused, leaving your reader unsure of exactly what you want to say.
Follow these four steps to come up with a thesis statement :
- Ask a question about your topic .
- Write your initial answer.
- Develop your answer by including reasons.
- Refine your answer, adding more detail and nuance.
The thesis statement should be placed at the end of your essay introduction .
Cite this Scribbr article
If you want to cite this source, you can copy and paste the citation or click the “Cite this Scribbr article” button to automatically add the citation to our free Citation Generator.
McCombes, S. (2023, August 15). How to Write a Thesis Statement | 4 Steps & Examples. Scribbr. Retrieved July 10, 2024, from https://www.scribbr.com/academic-essay/thesis-statement/
Is this article helpful?
Shona McCombes
Other students also liked, how to write an essay introduction | 4 steps & examples, how to write topic sentences | 4 steps, examples & purpose, academic paragraph structure | step-by-step guide & examples, what is your plagiarism score.
Death Penalty - Essay Samples And Topic Ideas For Free
The death penalty, also known as capital punishment, remains a contentious issue in many societies. Essays on this topic could explore the moral, legal, and social arguments surrounding the practice, including discussions on retribution, deterrence, and justice. They might delve into historical trends in the application of the death penalty, the potential for judicial error, and the disparities in its application across different demographic groups. Discussions might also explore the psychological impact on inmates, the families involved, and the society at large. They could also analyze the global trends toward abolition or retention of the death penalty and the factors influencing these trends. A substantial compilation of free essay instances related to Death Penalty you can find at Papersowl. You can use our samples for inspiration to write your own essay, research paper, or just to explore a new topic for yourself.

Death Penalty and Justice
By now, many of us are familiar with the statement, "an eye for an eye," which came from the bible, so it should be followed as holy writ. Then there was Gandhi, who inspired thousands and said, "an eye for an eye will leave us all blind." This begs the question, which option do we pick to be a good moral agent, in the terms of justice that is. Some states in America practice the death penalty, where some states […]
The Controversy of Death Penalty
The death penalty is a very controversial topic in many states. Although the idea of the death penalty does sound terrifying, would you really want a murderer to be given food and shelter for free? Would you want a murderer to get out of jail and still end up killing another innocent person? Imagine if that murder gets out of jail and kills someone in your family; Wouldn’t you want that murderer to be killed as well? Murderers can kill […]
Stephen Nathanson’s “An Eye for an Eye”
According to Stephen Nathanson's "An Eye for an Eye?", he believes that capital punishment should be immediately abolished and that the principle of punishment, "lex talionis" which correlates to the classic saying "an eye for an eye" is not a valid reason for issuing the death penalty in any country, thus, abolishment of Capital Punishment should follow. Throughout the excerpt from his book, Nathanson argues against this principle believing that one, it forces us to "commit highly immoral actions”raping a […]
We will write an essay sample crafted to your needs.
Does the Death Penalty Effectively Deter Crime?
The death penalty in America has been effective since 1608. Throughout the years following the first execution, criminal behaviors have begun to deteriorate. Capital punishment was first formed to deter crime and treason. As a result, it increased the rate of crime, according to researchers. Punishing criminals by death does not effectively deter crime because criminals are not concerned with consequences, apprehension, and judges are not willing to pay the expenses. During the stage of mens rea, thoughts of committing […]
The Death Penalty: Right or Wrong?
The death penalty has been a controversial topic throughout the years and now more than ever, as we argue; Right or Wrong? Moral or Immoral? Constitutional or Unconstitutional? The death penalty also known as capital punishment is a legal process where the state justice sentences an individual to be executed as punishment for a crime committed. The death penalty sentence strongly depends on the severity of the crime, in the US there are 41 crimes that can lead to being […]
About Carlton Franklin
In most other situations, the long-unsolved Westfield Murder would have been a death penalty case. A 57-year-old legal secretary, Lena Triano, was found tied up, raped, beaten, and stabbed in her New Jersey home. A DNA sample from her undergarments connected Carlton Franklin to the scene of the crime. However, fortunately enough for Franklin, he was not convicted until almost four decades after the murder and, in an unusual turn of events, was tried in juvenile court. Franklin was fifteen […]
About the Death Penalty
The death penalty has been a method used as far back as the Eighteenth century B.C. The use of the death penalty was for punishing people for committing relentless crimes. The severity of the punishment were much more inferior in comparison to modern day. These inferior punishments included boiling live bodies, burning at the stake, hanging, and extensive use of the guillotine to decapitate criminals. In the ancient days no laws were established to dictate and regulate the type of […]
The Death Penalty should not be Legal
Imagine you hit your sibling and your mom hits you back to teach that you shouldn't be hitting anyone. Do you really learn not to be violent from that or instead do you learn how it is okay for moms or dads to hit their children in order to teach them something? This is exactly how the death penalty works. The death penalty has been a form of punishment for decades. There are several methods of execution and those are […]
Effectively Solving Society’s Criminality
Has one ever wondered if the person standing or sitting next to them has the potential to be a murderer or a rapist? What do those who are victimized personally or have suffered from a tragic event involving a loved-one or someone near and dear to their heart, expect from the government? Convicted felons of this nature and degree of unlawfulness should be sentenced to death. Psychotic killers and rapists need the ultimate consequences such as the death penalty for […]
Religious Values and Death Penalty
Religious and moral values tell us that killing is wrong. Thou shall not kill. To me, the death penalty is inhumane. Killing people makes us like the murderers that most of us despise. No imperfect system should have the right to decide who lives and who dies. The government is made up of imperfect humans, who make mistakes. The only person that should be able to take life, is god. "An eye for an eye leaves the whole world blind". […]
Abolishment of the Death Penalty
Abstract: The purpose of this paper is to relate many different criminological theories in regard to capital punishment. We relate many criminological theories such as; cognitive theory, deviant place theory, latent trait theory, differential association theory, behavioral theory, attachment theory, lifestyle theory, and biosocial theory. This paper empirically analyzes the idea that capital punishment is inhumane and should be abolished. We analyze this by taking into consideration false convictions, deterrence of crime, attitudes towards capital punishment, mental illness and juvenile […]
Punishment and the Nature of the Crime
When an individual commits a crime then he/she is given punishment depending on the nature of the crime committed. The US's way of giving punishment to an offender has been criticized for many years. There are 2 types of cases; civil and criminal cases. In civil cases, most of the verdict comprises of jail time or fine amount to be paid. These are not as severe except the one related to money laundering and forgery. On the other hand, criminal […]
The Death Penalty and Juveniles
Introduction: In today's society, many juveniles are being sent to trial without having the chance of getting a fair trial as anyone else would. Many citizens would see juveniles as dangerous individuals, but in my opinion how a teenager acts at home starts at home. Punishing a child for something that could have been solved at home is something that should not have to get worse by giving them the death penalty. The death penalty should not be imposed on […]
Is the Death Penalty “Humane”
What’s the first thing that pops up in your mind when you hear the words Capital Punishment? I’m assuming for most people the first thing that pops up is a criminal sitting on a chair, with all limbs tied down, and some type of mechanism connected to their head. Even though this really isn't the way that it is done, I do not blame people for imagining that type of image because that is how movies usually portray capital punishment. […]
Euthanasia and Death Penalty
Euthanasia and death penalty are two controversy topics, that get a lot of attention in today's life. The subject itself has the roots deep in the beginning of the humankind. It is interesting and maybe useful to learn the answer and if there is right or wrong in those actions. The decision if a person should live or die depends on the state laws. There are both opponents and supporters of the subject. However different the opinions are, the state […]
The Death Penalty is not Worth the Cost
The death penalty is a government practice, used as a punishment for capital crimes such as treason, murder, and genocide to name a few. It has been a controversial topic for many years some countries still use it while others don't. In the United States, each state gets to choose whether they consider it to be legal or not. Which is why in this country 30 states allow it while 20 states have gotten rid of it. It is controversial […]
Ineffectiveness of Death Penalty
Death penalty as a means of punishing crime and discouraging wrong behaviour has suffered opposition from various fronts. Religious leaders argue that it is morally wrong to take someone's life while liberal thinkers claim that there are better ways to punish wrong behaviour other than the death penalty. This debate rages on while statistically, Texas executes more individuals than any other state in the United States of America. America itself also has the highest number of death penalty related deaths […]
Is the Death Penalty Morally Right?
There have been several disputes on whether the death penalty is morally right. Considering the ethical issues with this punishment can help distinguish if it should be denied or accepted. For example, it can be argued that a criminal of extreme offenses should be granted the same level of penance as their crime. During the duration of their sentencing they could repent on their actions and desire another opportunity of freedom. The death penalty should be outlawed because of too […]
Why the Death Penalty is Unjust
Capital punishment being either a justifiable law, or a horrendous, unjust act can be determined based on the perspective of different worldviews. In a traditional Christian perspective, the word of God given to the world in The Holy Bible should only be abided by. The Holy Bible states that no man (or woman) should shed the blood of another man (or woman). Christians are taught to teach a greater amount of sacrifice for the sake of the Lord. Social justice […]
The Death Penalty and People’s Opinions
The death penalty is a highly debated topic that often divided opinion amongst people all around the world. Firstly, let's take a look at our capital punishments, with certain crimes, come different serving times. Most crimes include treason, espionage, murder, large-scale drug trafficking, and murder towards a juror, witness, or a court officer in some cases. These are a few examples compared to the forty-one federal capital offenses to date. When it comes to the death penalty, there are certain […]
The Debate of the Death Penalty
Capital punishment is a moral issue that is often scrutinized due to the taking of someone’s life. This is in large part because of the views many have toward the rule of law or an acceptance to the status quo. In order to get a true scope of the death penalty, it is best to address potential biases from a particular ethical viewpoint. By looking at it from several theories of punishment, selecting the most viable theory makes it a […]
The History of the Death Penalty
The History of the death penalty goes as far back as ancient China and Babylon. However, the first recorded death sentence took place in 16th Century BC Egypt, where executions were carried out with an ax. Since the very beginning, people were treated according to their social status; those wealthy were rarely facing brutal executions; on the contrary, most of the population was facing cruel executions. For instance, in the 5th Century BC, the Roman Law of the Twelve Tablets […]
Death Penalty is Immoral
Let's say your child grabs a plate purposely. You see them grab the plate, smash it on the ground and look you straight in the eyes. Are they deserving of a punishment? Now what if I say your child is three years old. A three year old typically doesn't know they have done something wrong. But since your child broke that one plate, your kid is being put on death row. You may be thinking, that is too harsh of […]
The Death Penalty in the United States
The United States is the "land of the free, home of the brave" and the death penalty (American National Anthem). Globally, America stands number five in carrying executions (Lockie). Since its resurrection in 1976, the year in which the Supreme Court reestablished the constitutionality of the death penalty, more than 1,264 people have been executed, predominantly by the medium of lethal injection (The Guardian). Almost all death penalty cases entangle the execution of assassins; although, they may also be applied […]

Cost of the Death Penalty
The death penalty costs more than life in prison. According to Fox News correspondent Dan Springer, the State of California spent 4 billion dollars to execute 13 individuals, in addition to the net spend of an estimated $64,000 per prisoner every year. Springer (2011) documents how the death penalty convictions declined due to economic reasons. The state spends up to 3 times more when seeking a death penalty than when pursuing a life in prison without the possibility of parole. […]
The Solution to the Death Penalty
There has never been a time when the United States of America was free from criminals indulging in killing, stealing, exploiting people, and even selling illegal items. Naturally, America refuses to tolerate the crimes committed by those who view themselves as above the law. Once these convicts are apprehended, they are brought to justice. In the past, these criminals often faced an ultimate punishment: the death penalty. Mercy was a foreign concept due to their underdeveloped understanding of the value […]
Costs: Death Penalty Versus Prison Costs
The Conservatives Concerned Organization challenges the notion that the death penalty is more cost effective compared to prison housing and feeding costs. The organization argues that the death penalty is an expensive lengthy and complicated process concluding that it is not only a bloated program that delays justice and bogs down the enforcement of the law, it is also an inefficient justice process that diverts financial resources from law enforcement programs that could protect individuals and save lives. According to […]
Death Penalty as a Source of Constant Controversy
The death penalty has been a source of almost constant controversy for hundreds of years, splitting the population down the middle with people supporting the death penalty and people that think it is unnecessary. The amount of people that are been against the death penalty has grown in recent years, causing the amount of executions to dwindle down to where there is less than one hundred every year. This number will continue to lessen as more and more people decide […]
Death Penalty is Politically Just?
Being wrongfully accused is unimaginable, but think if you were wrongfully accused and the ultimate punishment was death. Death penalty is one of the most controversial issues in today's society, but what is politically just? When a crime is committed most assume that the only acceptable consequence is to be put to death rather than thinking of another form of punishment. Religiously the death penalty is unfair because the, "USCCB concludes prisoners can change and find redemption through ministry outreach, […]
George Walker Bush and Death Penalty
George Walker Bush, a former U.S. president, and governor of Texas, once spoke, "I don't think you should support the death penalty to seek revenge. I don't think that's right. I think the reason to support the death penalty is because it saves other people's lives." The death penalty, or capital punishment, refers to the execution of a criminal convicted of a capital offense. With many criminals awaiting execution on death row, the death penalty has been a debated topic […]
Additional Example Essays
- Death Penalty Should be Abolished
- Main Reasons of Seperation from Great Britain
- Leadership and the Army Profession
- Letter From Birmingham Jail Rhetorical Analysis
- Why Abortion Should be Illegal
- Logical Fallacies in Letter From Birmingham Jail
- How the Roles of Women and Men Were Portrayed in "A Doll's House"
- Ethical or Unethical Behavior in Business
- Does Arrest Reduce Domestic Violence
- Recycling Should be Mandatory
- Why I Want to Be an US Army Officer
How To Write an Essay About Death Penalty
Understanding the topic.
When writing an essay about the death penalty, the first step is to understand the depth and complexities of the topic. The death penalty, also known as capital punishment, is a legal process where a person is put to death by the state as a punishment for a crime. This topic is highly controversial and evokes strong emotions on both sides of the debate. It's crucial to approach this subject with sensitivity and a balanced perspective, acknowledging the moral, legal, and ethical considerations involved. Research is key in this initial phase, as it's important to gather facts, statistics, and viewpoints from various sources to have a well-rounded understanding of the topic. This foundation will set the tone for your essay, guiding your argument and supporting your thesis.
Structuring the Argument
The next step is structuring your argument. In an essay about the death penalty, it's vital to present a clear thesis statement that outlines your stance on the issue. Are you for or against it? What are the reasons behind your position? The body of your essay should then systematically support your thesis through well-structured arguments. Each paragraph should focus on a specific aspect of the death penalty, such as its ethical implications, its effectiveness as a deterrent to crime, or the risk of wrongful convictions. Ensure that each point is backed up by evidence and examples, and remember to address counterarguments. This not only shows that you have considered multiple viewpoints but also strengthens your position by demonstrating why these opposing arguments may be less valid.
Exploring Ethical and Moral Dimensions
An essential aspect of writing an essay on the death penalty is exploring its ethical and moral dimensions. This involves delving into philosophical debates about the value of human life, justice, and retribution. It's important to discuss the moral justifications that are often used to defend the death penalty, such as the idea of 'an eye for an eye,' and to critically evaluate these arguments. Equally important is exploring the ethical arguments against the death penalty, including the potential for innocent people to be executed and the question of whether the state should have the power to take a life. This section of the essay should challenge readers to think deeply about their values and the principles of a just society.
Concluding Thoughts
In conclusion, revisit your thesis and summarize the key points made in your essay. This is your final opportunity to reinforce your argument and leave a lasting impression on your readers. Discuss the broader implications of the death penalty in society and consider potential future developments in this area. You might also want to offer recommendations or pose questions that encourage further reflection on the topic. Remember, a strong conclusion doesn't just restate what has been said; it provides closure and offers new insights, prompting readers to continue thinking about the subject long after they have finished reading your essay.
1. Tell Us Your Requirements
2. Pick your perfect writer
3. Get Your Paper and Pay
Hi! I'm Amy, your personal assistant!
Don't know where to start? Give me your paper requirements and I connect you to an academic expert.
short deadlines
100% Plagiarism-Free
Certified writers
Purdue Online Writing Lab Purdue OWL® College of Liberal Arts
Developing Strong Thesis Statements

Welcome to the Purdue OWL
This page is brought to you by the OWL at Purdue University. When printing this page, you must include the entire legal notice.
Copyright ©1995-2018 by The Writing Lab & The OWL at Purdue and Purdue University. All rights reserved. This material may not be published, reproduced, broadcast, rewritten, or redistributed without permission. Use of this site constitutes acceptance of our terms and conditions of fair use.
The thesis statement or main claim must be debatable
An argumentative or persuasive piece of writing must begin with a debatable thesis or claim. In other words, the thesis must be something that people could reasonably have differing opinions on. If your thesis is something that is generally agreed upon or accepted as fact then there is no reason to try to persuade people.
Example of a non-debatable thesis statement:
This thesis statement is not debatable. First, the word pollution implies that something is bad or negative in some way. Furthermore, all studies agree that pollution is a problem; they simply disagree on the impact it will have or the scope of the problem. No one could reasonably argue that pollution is unambiguously good.
Example of a debatable thesis statement:
This is an example of a debatable thesis because reasonable people could disagree with it. Some people might think that this is how we should spend the nation's money. Others might feel that we should be spending more money on education. Still others could argue that corporations, not the government, should be paying to limit pollution.
Another example of a debatable thesis statement:
In this example there is also room for disagreement between rational individuals. Some citizens might think focusing on recycling programs rather than private automobiles is the most effective strategy.
The thesis needs to be narrow
Although the scope of your paper might seem overwhelming at the start, generally the narrower the thesis the more effective your argument will be. Your thesis or claim must be supported by evidence. The broader your claim is, the more evidence you will need to convince readers that your position is right.
Example of a thesis that is too broad:
There are several reasons this statement is too broad to argue. First, what is included in the category "drugs"? Is the author talking about illegal drug use, recreational drug use (which might include alcohol and cigarettes), or all uses of medication in general? Second, in what ways are drugs detrimental? Is drug use causing deaths (and is the author equating deaths from overdoses and deaths from drug related violence)? Is drug use changing the moral climate or causing the economy to decline? Finally, what does the author mean by "society"? Is the author referring only to America or to the global population? Does the author make any distinction between the effects on children and adults? There are just too many questions that the claim leaves open. The author could not cover all of the topics listed above, yet the generality of the claim leaves all of these possibilities open to debate.
Example of a narrow or focused thesis:
In this example the topic of drugs has been narrowed down to illegal drugs and the detriment has been narrowed down to gang violence. This is a much more manageable topic.
We could narrow each debatable thesis from the previous examples in the following way:
Narrowed debatable thesis 1:
This thesis narrows the scope of the argument by specifying not just the amount of money used but also how the money could actually help to control pollution.
Narrowed debatable thesis 2:
This thesis narrows the scope of the argument by specifying not just what the focus of a national anti-pollution campaign should be but also why this is the appropriate focus.
Qualifiers such as " typically ," " generally ," " usually ," or " on average " also help to limit the scope of your claim by allowing for the almost inevitable exception to the rule.
Types of claims
Claims typically fall into one of four categories. Thinking about how you want to approach your topic, or, in other words, what type of claim you want to make, is one way to focus your thesis on one particular aspect of your broader topic.
Claims of fact or definition: These claims argue about what the definition of something is or whether something is a settled fact. Example:
Claims of cause and effect: These claims argue that one person, thing, or event caused another thing or event to occur. Example:
Claims about value: These are claims made of what something is worth, whether we value it or not, how we would rate or categorize something. Example:
Claims about solutions or policies: These are claims that argue for or against a certain solution or policy approach to a problem. Example:
Which type of claim is right for your argument? Which type of thesis or claim you use for your argument will depend on your position and knowledge of the topic, your audience, and the context of your paper. You might want to think about where you imagine your audience to be on this topic and pinpoint where you think the biggest difference in viewpoints might be. Even if you start with one type of claim you probably will be using several within the paper. Regardless of the type of claim you choose to utilize it is key to identify the controversy or debate you are addressing and to define your position early on in the paper.
An official website of the United States government
The .gov means it’s official. Federal government websites often end in .gov or .mil. Before sharing sensitive information, make sure you’re on a federal government site.
The site is secure. The https:// ensures that you are connecting to the official website and that any information you provide is encrypted and transmitted securely.
- Publications
- Account settings
Preview improvements coming to the PMC website in October 2024. Learn More or Try it out now .
- Advanced Search
- Journal List
- HHS Author Manuscripts

Defining a Good Death (Successful Dying): Literature Review and a Call for Research and Public Dialogue
Associated data.
There is little agreement about what constitutes good death or successful dying. The authors conducted a literature search for published, English-language, peer-reviewed reports of qualitative and quantitative studies that provided a definition of a good death. Stakeholders in these articles included patients, prebereaved and bereaved family members, and healthcare providers (HCPs). Definitions found were categorized into core themes and subthemes, and the frequency of each theme was determined by stakeholder (patients, family, HCPs) perspectives. Thirty-six studies met eligibility criteria, with 50% of patient perspective articles including individuals over age 60 years. We identified 11 core themes of good death: preferences for a specific dying process, pain-free status, religiosity/spiritualty, emotional well-being, life completion, treatment preferences, dignity, family, quality of life, relationship with HCP, and other. The top three themes across all stakeholder groups were preferences for dying process (94% of reports), pain-free status (81%), and emotional well-being (64%). However, some discrepancies among the respondent groups were noted in the core themes: Family perspectives included life completion (80%), quality of life (70%), dignity (70%), and presence of family (70%) more frequently than did patient perspectives regarding those items (35%–55% each). In contrast, religiosity/spirituality was reported somewhat more often in patient perspectives (65%) than in family perspectives (50%). Taking into account the limitations of the literature, further research is needed on the impact of divergent perspectives on end-of-life care. Dialogues among the stakeholders for each individual must occur to ensure a good death from the most critical viewpoint—the patient’s.
INTRODUCTION
“The truth is, once you learn how to die, you learn how to live.” —Mitch Albom, Tuesdays with Morrie 1
Considerable lay literature describes positive approaches to dying. For example, in “Tuesdays with Morrie” 1 Mitch Albom visits with his former Sociology professor, Morrie Schwartz, who provides lessons on acceptance, communication, and love in the midst of his own dying process. Similarly, Viktor Frankl’s “Man’s Search for Meaning” 2 describes experiences in a Nazi concentration camp that led to finding meaning during times of suffering and death. Also, in “The Last Lecture,” 3 Randy Pausch discusses, after being diagnosed with advanced pancreatic cancer, how to truly live and embrace every moment because “time is all you have…and you may find one day that you have less than you think.” Finally, in his commencement speech at Stanford University, Steve Jobs, 4 after a recent diagnosis of cancer, called death “very likely the single best invention of life” and described focusing on what was most important and meaningful to him as he confronted death. These literary examples illustrate various constructs of a good death or “dying well.” 5
Within the healthcare community and, more specifically, in hospice and palliative care, there has been some discussion of the concept of a good death. 6 , 7 This concept arose from the hospice movement and has been described as a multifaceted and individualized experience. 8 According to an Institute of Medicine report published 19 years ago, a good death is one that is “free from avoidable distress and suffering for patient, family, and caregivers, in general accord with the patient’s and family’s wishes, and reasonably consistent with clinical, cultural, and ethical standards.” 9 This concept has received some critique in several disciplines, including medicine, psychology, theology, sociology, and anthropology. 6 In particular, concern has been raised that there is no such thing as an external criterion of a good death and that it is more dependent on the perspectives of the dying individual. 10
In this article we use the terms “good death” or “successful dying.” Is successful dying an extension of successful aging? Research on successful aging has grown considerably in recent years; 11 however, there is little agreement as to what specifically constitutes a good death or successful dying despite many reviews examining the concept of a good death from sociological and philosophical viewpoints 12 – 18 as well as research examining the quality of death and dying, which is defined as “the degree to which a person’s preferences for dying and the moment of death agree with observations of how the person actually died, as reported by others.” 19 – 23 However, far fewer studies have specifically defined, rather than conceptualized, what a good death is according to patients, family members, and healthcare providers (HCPs). The goal of this article is to review the literature that examined the definitions of a good death from the perspectives of such patients, their family members, and HCPs.
By examining the perspectives regarding a good death contrasted across different stakeholders, our aim is to identify potential unmet needs of patients and to suggest an approach to achieve a multifaceted and individualized experience for patients approaching death. Because a dearth of literature examines this important topic, our review is limited by the quantity and quality of studies available to evaluate. To our knowledge, no review to date has examined and compiled definitions of good death as defined explicitly by patients, family members, and HCPs or examined the differences among these stakeholders’ viewpoints. This is an area of considerable public health significance and impact on the patients, their families, and the overall healthcare system. The present article is also intended to serve as a call to action to highlight the need for more patient-focused research and open public dialogues on successful dying.
Data Sources
We searched PubMed and PsycINFO databases from inception through November 2015 using the following terms: (definition of) AND (good OR successful OR peaceful) AND (Death OR Dying); (good) OR (successful OR peaceful) AND (“Death and Dying”); (“Terminal Care”[Mesh] AND “Quality of Life”[Mesh] AND “Attitude to Death”[Mesh]); (“Terminal Care”[Mesh]) AND “Attitude to Death”[Mesh] AND (define OR definition); good death and dignity; good death and end of life preferences; good death and quality of death and dying.
Selection of Articles
We restricted our search to include articles that met the following criteria: published in English in peer-reviewed journals and provided quantitative or qualitative data that specifically defined or used a measure of good death as the main aim or outcome of the study. We eliminated all duplicate articles from these searches. Additionally, we reviewed the reference lists of all articles that were relevant as well as recent review papers that examined a good death. 15 , 24 , 25 There were no instances of overlapping samples.
Two authors (EAM and JVG) independently searched PubMed and PsycINFO databases for appropriate articles according to the key words mentioned above. Individual articles were independently coded for themes and subthemes by the two authors. If there was a disagreement between the two, a third author (DVJ) was consulted to help reach a consensus. Specific information about each article was stored in an Excel database.
Most initial search results (3,434) were excluded because of irrelevance to the subject matter in the title or abstract (e.g., “good cell death,” “good bone death,” “animal death,” etc.), which resulted in 392 articles for further review. After a more detailed examination, we narrowed these articles down to 36 relevant to the present review ( Fig. 1 ). Articles were excluded if they were focused solely on euthanasia or assisted suicide or on specific methods of enhancing quality of care at the end of life, unless one of the specific aims of the study was to define good death or successful dying.

Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) flow diagram of the review process.
References from review papers of a good death were examined in detail to see if they met our inclusion criteria. Twenty-seven articles contained qualitative methods, 5 articles used quantitative methods, and 4 articles contained mixed methods (qualitative and quantitative). Of the quantitative and mixed-methods studies (N = 9), 3 articles used standardized measures of a good death, including the Preferences about Death and Dying questionnaire, 26 The Concept of a Good Death scale, 27 and The Good Death Inventory. 28 The other six studies had developed their own quantitative measures (e.g., attitudinal measures of a good death); 29 a 12-item questionnaire based on 12 principles of a good death according to the Future of Health Care of Older People report; 30 , 31 a 57-item questionnaire based on a previous qualitative study; 32 44 items of attributes important at the end of life developed from focus groups and in-depth interviews with patients, family members, and HCPs; 33 and a 72-item survey on perceptions of end-of-life care. 34
Coding of Articles
Two authors (EAM and JVG) independently read all 36 articles. We used the method of coding consensus, co-occurrence, and comparison outlined by Williams et al. 35 and rooted in grounded theory to generate common themes of a good death. Four consensus meetings were held between two coders (EAM and JVG) to create the final coding scheme after resolving any disagreements. We began with 38 themes, which were narrowed to 11 themes in a consensus meeting involving three authors (EAM, JVG, and DVJ). Two authors (EAM and JVG) then independently coded each definition supplied in the 36 articles, which were then mapped onto the 11 core themes. If an item did not fit, it was placed in the “Other” core theme. Inter-rater reliability was calculated for the independent raters by use of the kappa statistic. The inter-rater reliability for the coders was kappa = 0.896 (p < 0.0.000; standard error: 0.023), which was a satisfactory level of agreement. 36 Discrepancies were further discussed by two authors (EAM and JVG), with a third author (DVJ) consulted, when needed, to reach a final consensus on each definition.
The sources of each definition were separated into three groups: (1) patients’ perspectives (N = 20), (2) prebereaved and bereaved family members’ perspectives (N = 10), and (3) HCPs’ perspectives (N = 18). Patient populations consisted of those with advanced cancer, chronic illnesses, HIV/AIDS, as well as the general population. Family members’ perspectives were prebereavement (N = 1) or postbereavement (N = 9). HCPs included physicians, nurses, social workers, and spiritual counselors. HCP perspectives could not be further broken down into specific subgroups (e.g., physicians versus nurses) because these subgroups were usually combined in the studies reviewed. Of the 36 reviewed articles, 29 were coded into one category and 7 were coded into more than one group, 2 articles coded into two groups, and 5 articles were coded into all three.
We did not conduct a formal meta-analysis in light of differences among the studies in terms of depth of information and methods used to assess stakeholders’ (especially patients’) demographics, medical diagnoses, treatment status, cognitive assessment, and so on. By definition, meta-analysis comprises statistical methods for contrasting and combining results from different studies in the hope of identifying patterns among study results, sources of disagreement among those results, or other interesting relationships that may come to light in the context of multiple studies (p. 652). 37 This type of analysis was not possible for our data for the reasons mentioned above. Additionally, weighting was not done because qualitative and quantitative studies were combined. However, because all studies provided stakeholder frequency of responses that endorsed specific themes of a good death, we were able to aggregate frequencies across studies to calculate the mean percentages for different domains of what is perceived to be part of a good death. As such, we calculated the means and standard deviations or percentages, as appropriate, and reported the rate of endorsement of each of the 11 codes within each of the sources (e.g., patients, family members, and HCPs).
In total, 36 articles met our search criteria. These studies were published between 1996 and 2015. Total sample sizes across all studies reviewed ranged from 3 to 2,548 (mean: 184.4; standard deviation: 440.8). As one may expect, qualitative studies had much smaller sample sizes than quantitative investigations. Table 1 summarizes demographics of the patients included in individual studies. The age range of patients spanned 14–93 years (mean: 89.7; standard deviation: 16.6), with 50% of patient perspective articles including individuals over age 60 years. Age was somewhat skewed because several articles only reported a range rather than the mean age. There was a relatively even distribution between men and women across all studies. The studies reviewed had been conducted in the United States (N = 13), United Kingdom (7), Japan (3), Netherlands (3), Thailand (2), Iran (1), Israel (1), Canada (1), Nova Scotia (1), Saudi Arabia (1), South Korea (1), and Sweden (1), Turkey (1).
Demographic Characteristics of Patients in the 36 Articles Reviewed for Successful Dying
| Study Authors and Year | Country | Design/ Methods | Measure of a Good Death | Diagnosis/ Population | Age (y) | Gender | Ethnicity/Race | No. of Patients | No. Family Members | No. of HCPs |
|---|---|---|---|---|---|---|---|---|---|---|
| Payne (1996) | UK | Qualitative | Elicit (patient and palliative care professionals perception of death) | Advanced cancer | Range: 30–81 | 50% Male | — | 18 | — | 20 |
| Payne and Hillier (1996) | UK | Qualitative/quantitative | Narratives from participants used to define a “good death” | Cancer/hospice | Mean: 66 | 50% Male | — | 67 | — | — |
| Leichtentritt (2000) | Israel | Qualitative | Interviewing discussing good death | General population and medical patients | Range: 60–86 | 57% Female | Israelis | 26 | — | — |
| Steinhauser (2000) | USA | Quantitative | Survey (rank 44 attributes important at end of life) | Veterans with advanced chronic illness | Mean: 68 | 78% Male | 69% Non-Hispanic, White | 340 | 332 | 361 |
| Steinhauser (2000) | USA | Qualitative | Discuss (experiences with deaths of family members, friends, or patients and reflect on what made those deaths good) | Oncology and HIV | Range: 26–77 | 36% Male | 70% Non-Hispanic, White | 14 | 4 | 57 |
| Pierson (2002) | USA | Qualitative | Describe a (good death) | AIDS | Mean: 41 | 91% Male | 69% Non-Hispanic, White | 35 | — | — |
| Vig (2002) | USA | Qualitative | Open-ended questions assessing patients views of end of life | Cancer and heart disease | Range: 60–84 | 87% Female | — | 16 | — | — |
| Tong (2003) | USA | Qualitative | Focus groups to elicit views about death and dying | General population | Range: 14–68 | 67% Female | 53% Non-Hispanic, White 23% Black 14% Hispanic | 95 | — | — |
| Vig (2004) | USA | Qualitative | Open-ended questions assessing patients views of end of life | Cancer and heart disease | Mean: 71 | 100% Male | — | 26 | — | — |
| Goldstein (2006) | Amsterdam | Qualitative | Open-ended question interview to explore a “good death” | Cancer patients | Range: 39–83 | 70% Male | Non-Hispanic, White | 13 | — | — |
| Hirai (2006) | Japan | Qualitative | Asked participants for components of a “good death” | Cancer patients | Mean: 62 | 54% Male | — | 13 | 10 | 40 |
| Rietjens (2006) | Netherlands | Qualitative | Respondents were asked to indicate how important they considered 11 attributes of the dying process | General population | Range: 20–93 | 61% Female | — | 1,388 | — | — |
| Lloyd-Williams 2007) | UK | Qualitative | Semistructured interview based on concepts of independence, health, and well-being, societal support; theme of end of life reported in article | Community-dwelling adults | Range: 80–89 | 40% Male | 85% English | 40 | — | — |
| Miyashita (2007) | Japan | Quantitative | Asked subjects about the relative importance of 57 components of a good death | General population | Range: 49–70 | 48% Male | — | 2,548 | 513 | — |
| Gott (2008) | UK | Qualitative | Interviews to explore extent that older adult views are consistent with palliative care “good death” model | Advanced heart failure and poor prognosis | Mean: 77 | 53% Male | 40 | — | — | |
| Hughes (2008) | USA | Qualitative | Definition of good death | Lung cancer | Range: 24–85 | 50% Male | — | 100 | — | — |
| De Jong (2009) | Nova Scotia | Qualitative | Hear stories of good and bad deaths from those directly involved in palliative care | Palliative patients | — | — | — | 3 | 3 | 9 |
| Tayeb (2010) | Saudi Arabia | Qualitative/Quantitative | Principles of good death; agree or disagree with Western principles of good death | Hematology/oncology patients | — | 58% Male | Non-Saudi Arabian | 26 | 77 | 181 |
| Hattori (2012) | USA | Qualitative | Interviews asking “What does a good death mean to you? | Japanese older adults living in Hawaii | Mean: 78 | 77% Female | Japanese | 18 | — | — |
| Reinke (2013) | USA | Qualitative/Quantitative | In-person interview and questionnaire to rate what is most important in last 7 days of life | Veterans with chronic obstructive pulmonary disease | Mean: 69 | 97% Male | 291 White | 376 | — | — |
Themes and Subthemes of Successful Death Definitions
Eleven themes were identified, and each consisted of 2 to 4 subthemes, which are presented in Table 2 . The most frequently appearing theme for a good death across all groups was “preferences for the dying process,” which was reported in 94% of the articles in the sample. These preferences for the dying process included the following subthemes: the death scene (how, who, where, and when), dying during sleep, and preparation for death (e.g., advanced directives, funeral arrangements). “Pain-free status” was the second most frequent core theme of good death in the sample (81%) followed by “emotional well-being” (64%). Examples from patients included the following statements: “Painless. I mean pain is my biggest fear, you know. I don’t want to die in pain,” “a good death would be having the things that you wanted to have taken care of before you die done so you can be at peace with it.” 42 Additionally, some statements included that thinking about death and dying made individuals feel “afraid and depressed.” 50
Core Themes and Subthemes of a Good Death and/or Successful Dying
| Core Theme | Subtheme |
|---|---|
| Preferences for dying process | Death scene (how, who, where, and when) |
| Dying during sleep | |
| Preparation for death (e.g., advanced directives, funeral arrangements) | |
| Pain-free status | Not suffering |
| Pain and symptom management | |
| Emotional well-being | Emotional support |
| Psychological comfort | |
| Chance to discuss meaning of death | |
| Family | Family support |
| Family acceptance of death | |
| Family is prepared for death | |
| Not be a burden to family | |
| Dignity | Respect as an individual |
| Independence | |
| Life completion | Saying goodbye |
| Life well lived | |
| Acceptance of death | |
| Religiosity/spirituality | Religious/spiritual comfort |
| Faith | |
| Meet with clergy | |
| Treatment preferences | Not prolonging life |
| Belief that all available treatments were used | |
| Control over treatment | |
| Euthanasia/physician-assisted suicide | |
| Quality of life | Living as usual |
| Maintaining hope, pleasure, gratitude | |
| Life is worth living | |
| Relationship with HCP | Trust/support/comfort from physician/nurse |
| Physician comfortable with death/dying | |
| Discuss spiritual beliefs/fears with physician | |
| Other | Recognition of culture |
| Physical touch | |
| Being with pets | |
| Healthcare costs |
Four themes—life completion, treatment preferences, dignity, and family—were endorsed by more than 50% of all three stakeholder groups ( Table 3 ). The theme of life completion contained subthemes of saying goodbye, feeling that life was well lived, and acceptance of impending death. Treatment preferences included subthemes related to not prolonging life, a belief that all available treatments were used, a sense of control over treatment choices, and euthanasia/physician-assisted suicide. The theme of dignity consisted of being respected as an individual and maintaining independence, whereas the theme of family included family support, family accepting of death, the family is prepared for the death, and not being a burden to family.
Number of Articles (N = 36) that Included Specific Core Themes
| No. of Articles on Patients (N = 20) | No. of Articles on Prebereaved/Bereaved Family (N = 10) | No. of Articles on HCPs (N = 18) | |
|---|---|---|---|
| Preferences for dying process | 20 (100) | 10 (100) | 17 (94) |
| Pain-free status | 17 (85) | 9 (90) | 15 (83) |
| Religiosity/spirituality | 13 (65) | 5 (50) | 9 (59) |
| Emotional well-being | 12 (60) | 7 (70) | 12 (67) |
| Life completion | 11 (55) | 8 (80) | 10 (56) |
| Treatment preferences | 11 (55) | 7 (70) | 11 (61) |
| Dignity | 11 (55) | 7 (70) | 12 (67) |
| Family | 11 (55) | 7 (70) | 11 (61) |
| Quality of life | 7 (35) | 7 (70) | 4 (22) |
| Relationship with HCP | 4 (20) | 4 (40) | 7 (39) |
| Other | 8 (40) | 4 (40) | 5 (28) |
Note: Values in parentheses are percent of the stakeholders endorsing themes.
Prebereaved and bereaved family members rated eight of the core themes at 70% and higher, the most frequent themes being preferences for dying process (100%), pain-free status (90%), and life completion (80%). Relationship with HCPs was found to be the least important specific theme among all three stakeholders.
Among HCPs, preference for dying process (94%) was the most frequently endorsed core theme of a good death, followed by pain-free status (83%), dignity (67%), and emotional well-being (67%). HCPs had the lowest endorsement for three core themes: life completion (56%), relationship with HCPs (39%), and quality of life (22%). Examples from HCPs included statements such as “having a patient pass quietly so not to disturb other patients,” “having the death occur at a time when there was adequate staff,” and “not having used excessive or futile treatments.” 53 , 54 Some statements included regret for administered treatment or a concern that the medical staff was unable to provide appropriate care.
Differences in frequencies of themes among the stakeholder groups were greatest for quality of life, which was rated more frequently in family perspective articles (70%) than in patient and HCP perspective articles (35% and 22%, respectively) ( Table 3 ). Similarly, prebereaved and bereaved family members identified the importance of family and maintaining dignity at a rate (70%) somewhat higher than that in the patient perspective articles (55% each). In contrast, religiosity/spirituality was endorsed somewhat more in patient perspective articles (65%) than in family perspective articles (50%). Supplementary Table S1 lists core themes endorsed by each stakeholder group in individual articles.
In this review we identified a number of themes important to a good death that both converge and diverge across stakeholders. To our knowledge, this review is the first systematic attempt to review the empirical literature on both the definition of a good death or successful dying according to patients, family members, and HCPs and differences across these stakeholder perspectives. Our review identified a general consensus among patients, family members, and HCPs in regard to pain-free status and specific preferences for the dying process; however, there were some notable discrepancies, for example, family members rated quality of life as more important than patient and HCP articles.
This review has several limitations. The first challenge is the variability among the articles reviewed in reporting data such as respondent characteristics. There were no common measures of a “good death” used in different investigations, which limited our capacity to aggregate results for conducting a meta-analysis or meta-regression. There was also an imbalance in sample sizes across qualitative and quantitative studies. We restricted our search to English-language and peer-reviewed articles, which might have limited the scope of our review. Also, some differences in perspectives of different stakeholders discussed below are rather small in magnitude, compounded by the limited amount of published literature in this emerging area of empirical research; consequently, we were underpowered to make statistical comparisons across study groups.
Empirical research on what comprises a good death began only a couple of decades ago, and several aspects of the methodology used in previously published studies were suboptimal. Most articles reviewed did not report information regarding specific demographics of patients, including age, culture/ethnicity, diagnoses, study inclusion/exclusion criteria, and recruitment procedures. Additionally, there was no mention of the length of time between the interview or survey and the patients’ death, which might have an important impact on specific wishes, desires, and needs as one nears the end of life as well as perceptions of what constitutes a good death, which could change over time and as the process is experienced. In regards to the investigations of family members, most studies included postbereavement family members, and therefore perspectives of prebereavement family members were not well represented. Finally, HCPs were often grouped together in the reports, and it is not known what percentage of HCPs were physicians, nurses, social workers, spiritual counselors, and so on. Furthermore, there was little information on how many, if any, of these HCPs had directly cared for dying patients or received training in such care.
Despite these limitations, we were able to identify some consistency among the three stakeholder groups in their perceptions of what constituted a good death. In more than 85% of the articles reviewed, having patient-focused preferences for the dying process and being pain-free were key components of achieving a good death according to patients, prebereaved and bereaved family members, and HCPs. Physicians, nurses, and other HCPs viewed optimal pain control and keeping the patient comfortable as a requirement for a good death. 17 , 29 , 33 , 51 This is also consistent with the overall philosophy of hospice and palliative care, which focuses on decreasing pain and suffering while improving quality of life for both patients and family members. 55
Although family members’ perspectives seemed to be more in tune with the patients’ needs and desires for end-of-life care than HCPs’, there were also some differences between family members and patients in what themes they believed to be important for a good death. For example, quality of life was rated as an important component of a good death twice as often by family members (70%) as by patients (35%). Most family perspective articles were conducted with bereaved family members who were often asked to recall the death of a loved one. Although we cannot make assumptions regarding the inferences of these findings, it could be argued that family members and patients define quality of life differently. The quality of life literature is large and beyond the scope of this review; however, it is worth further investigating how patients, family members, and HCPs define quality of life near the end of life to help understand and define this construct more precisely.
Additionally, “dignity” was reported to be an important component of a good death in 70% of family articles compared with 55% of the articles that included patient perspectives. Although the difference is not large, the finding is counterintuitive to previous research, which has argued that patients greatly value maintaining dignity during the late phase of their life. 56 , 57 However, definitions of dignity vary, and the concept of dignity may have been absorbed into other themes from the stakeholders’ perspectives. Over the last 17 years, The Oregon Death with Dignity Act has consistently publicized that the three most important concerns reported among patients near the end of their lives include a loss of autonomy (91%), a decrease in the ability to participate in activities that made life enjoyable (86%), and a loss of dignity (71%). 58 Furthermore, in a study conducted in 2002 by Chochinov et al., 56 palliative care patients reported that “not being treated with respect or understanding” (87%) and “feeling a burden to others” (87%) significantly impacted their sense of dignity. Therefore, our findings do not necessarily mean that dignity is less important for dying patients but that perhaps patients have a difficult time expressing the need for or concept of dignity to others.
The role of religiosity/spirituality was also somewhat discrepant between patients and other groups. Nearly two-thirds of patients (65%) in the articles reviewed expressed a desire to have religious or spiritual practices fulfilled as a theme of a good death; in contrast, only 50% of family members rated this theme as important. It should be added that hospice care teams are typically supposed to be composed of physicians, nurses, home health aides, social workers, as well as clergy or spiritual counselors. 59 However, in our current sample not all the patients were receiving hospice services, which might have contributed to a lack of recognition of the importance of religiosity/spirituality, because many organizations and hospitals do not have clergy members or spiritual counselors available on site, especially for diverse groups of patients.
Finally, although some literature exists on pain and physical symptoms, there is a dearth of research examining the psychological aspects of a good death, particularly from a patient perspective. 12 Our review indicates that patients view emotional well-being as a critical component of a successful death, as do family members and HCPs. Although it is important that we attend to the patient’s physical symptoms and pain control, it is crucial that the healthcare system expand the care beyond treating these symptoms and more closely address psychological, social, and religiosity/spirituality themes in end-of-life care for both patients and families. Patients view the end of life as encompassing not only the physical components of death but also psychosocial and spiritual concerns. 33 Both the American Psychological Association and the European Association for Palliative Care have identified a need for mental health professionals to address and measure psychological concerns at the end of life. 60 , 61 Further research regarding the psychological components of a good death is needed, especially in developing effective screening measures and appropriate interventions for dying patients. 12
Future Directions
This review suggests an obvious need for more research to examine the concept of a good death from patients’ perspectives to deliver quality care that is individualized to meet each patient’s needs 8 , 62 as well as the needs of their families. The discrepancies among patient, family member, and HCP perspectives on successful dying in this review indicate a critical need for a dialogue about death among all stakeholders involved in the care of each individual patient. It is important that we not only understand but also further investigate how addressing the themes identified in this review, both convergent and discrepant among stakeholders, may influence patient-related outcomes.
Well-designed studies are also necessary to qualitatively and quantitatively examine the concept of successful dying according to patients themselves, because this would have the potential to influence HCP care practices and to help family members meet the needs of their dying loved ones. Qualitative research could lead to the development of measurement tools for successful dying that allow for real-time modifications in care and examine how specific diseases and interventions intersect values and beliefs that are most important to patients nearing the end of their lives. Future studies would also benefit from mixed qualitative–quantitative method designs that compare people at the end of life with others who have chronic but earlier stage diseases (e.g., heart or lung disease). Additionally, it would be important to include different age cohorts (young, middle-aged, and older adults) to determine whether age impacts the themes that constitute a good death. Investigations of large numbers of demographically, medically, and psychosocially well-characterized patients from diverse ethnic and cultural groups, using standardized and validated instruments for successful dying, and seeking perspectives of these patients along with their prebereaved and bereaved family members and HCPs are recommended to inform the best practices in caring for dying patients and their families. Finally, future studies should use a clearly delineated sampling strategy that would then allow generalization to a larger population of patients, family members, and HCPs.
Finally, an important goal of this review is to issue a call for action to the professional and lay community to accelerate its open dialogue regarding death and dying, as the United States has a largely “death-phobic” culture. 63 Although individuals in many states in the country are formally asked and encouraged to consider advanced directives and organ donations, should we, as clinicians, also not ask our older patients to stipulate their preferences for the dying process? If, as a society, we begin to address the question of how people want to die and what they actually need and want at the end of their lives, perhaps we can enable more people to obtain a good death, reaching their full potential, with dignity and whole-person well-being. As stated eloquently by Gawande, 7 “…our most cruel failure in how we treat the sick and the aged is the failure to recognize that they have priorities beyond merely being safe and living longer; that the chance to shape one’s story is essential to sustaining meaning in life; that we have the opportunity to refashion our institutions, our culture, and our conversations in ways that transform the possibilities for the last chapters of everyone’s lives.”
Supplementary Material
Acknowledgments.
Funding for this research came, in part, from the Sam and Rose Stein Institute for Research on Aging at UC San Diego, American Cancer Society: MRSG-13-233-01 PCSM, and UC San Diego Moores Cancer Center.
APPENDIX: SUPPLEMENTARY MATERIAL
Supplementary data to this article can be found online at doi:10.1016/j.jagp.2016.01.135.
Writing Ideas
- Beginning a compare&contrast paper
- Strong persuasive paper topics
- Response to literature essay samples
- Finding an essay topic on Israel
A List Of Original Argumentative Essay Topics On The Death Penalty
Few issues in the United States are more contentious than the use of the death penalty as a punishment for severe crimes. Capital punishment has been recorded almost since the dawn of written history, but in today’s world, many people have come to see it as unnecessary and inhumane. Although some people are opposed to taking the lives of criminals, other people argue that it’s the best way to deal with serious crimes. They feel that these people have committed such terrible atrocities that they can never realistically be rehabilitated and reintroduced into society. The debate has been ongoing for a long time, with both sides expressing strong opinions.
Because the death penalty is so contentious, it’s a great subject for an argumentative essay. This type of essay revolves around the presentation of a particular stance on an issue, which you need to defend with logic, facts, and sound reasoning. You’ll need to do some research to gather relevant facts that support your point of view, then tie them together in a cohesive paper that presents a lucid argument based on the evidence. Because argumentative essays are such a useful tool for developing and evaluating critical thinking skills, you’ll have to write several of them during high school and college.
There are many arguments that you can make for, or against, the death penalty. Here are a few potential topics regarding capital punishment, which you can consider if you’re writing an argumentative essay.
- The death penalty is a deterrent that prevents potential criminals from committing serious crimes like murder.
- The death penalty is not effective at preventing crime.
- Capital punishment is more cost-effective than lifetime incarceration, which requires the State to pay for a person’s food, lodging, healthcare, and other things for the rest of their lives.
- The death penalty, “a life for a life,” is a just response to murder.
- The justice system does not have the intrinsic moral right to take a life, even that of a murderer.
- The death penalty is more humane than lifetime imprisonment.
- The death penalty is cruel and inhumane.
- Lethal injection is a painless and humane method of execution.
- Lethal injection is ethically questionable, can cause pain, and is often administered by people who are not trained medical professionals.
- People deserving of the death penalty can never be rehabilitated or reintroduced to society.
- Capital punishment deprives the individual of the chance for redemption and rehabilitation.
- The death penalty creates the risk of the execution of someone who is actually innocent.
- The death penalty can be abused or applied unfairly, making it dangerous to allow capital punishment.
“ Every writer, no matter how good he is with his first attempt should proofread his paper. ” – Donna Brians
This resource changes all old-fashioned cliches and boring techniques into new and original ways of writing. Like to come here for fresh ideas!
Never thought writing can be so captivating! Thank you for helping me every time I need!
Writing Partners

Popular Tips
- Creating a perfect paper
- Essay on capital punishment
- Finding an essay writing company
- Where to buy an essay without troubles

Assisted dying: The motivations, benefits and pitfalls of hastening death
As physician-assisted dying becomes more available, psychologists are finding opportunities to study people’s motivations and the potential benefits and harms of aid in dying
By Kirsten Weir
December 2017, Vol 48, No. 11
Print version: page 26
13 min read

- Older Adults and Aging
"CE Corner" is a continuing education article offered by the APA Office of CE in Psychology.
To earn CE credit, after you read this article, purchase the online exam at www.apa.org/ed/ce/resources/ce-corner .
Upon successful completion of the test — a score of 75 percent or higher — you can immediately print your CE certificate.
The test fee is $25 for members and $35 for nonmembers. The APA Office of CE in Psychology retains responsibility for the program. For more information, call (800) 374-2721.
CE credits: 1
Learning objectives: After reading this article, CE candidates will be able to:
- Describe APA’s resolution on assisted dying.
- Discuss the ways depression can complicate a patient’s wish for assisted dying.
- Discuss research on how family and friends are affected when a loved one chooses assisted dying.
It's been two decades since Oregon enacted the nation's first Death with Dignity Act, allowing people with terminal illnesses to hasten their deaths by self-administering medications prescribed by a physician. Since then, California, Colorado, Vermont, Washington state and Washington, D.C., have passed similar statutes.

Yet the topic arouses strong feelings—and raises plenty of questions. Can a person with depression rationally choose to hasten death? Would the option be less appealing if people received better care for physical symptoms and emotional distress? Could aid in dying put marginalized groups at risk?
As physician-assisted dying becomes available in more places, research psychologists are finding opportunities to study people's motivations and the potential benefits and harms of aid in dying. On the clinical side, psychologists' skills are helpful as people sort through their feelings and desires at the end of life, says Elizabeth Goy, PhD, a psychologist at the Portland VA Medical Center and associate professor at Oregon Health and Science University, and chair of the APA Working Group on End-of-Life Issues and Care.
"The very best thing we can do as psychologists is to improve communication and make sure that we are attending to the needs and suffering of patients who are at the end of life," Goy says. "Dying is universal, and it behooves all of us to have some foundational knowledge about end-of-life issues."
A new language
Goy and her colleagues on the working group were charged with updating APA's previous resolution on assisted suicide, adopted in 2001. In August, APA's Council of Representatives voted to approve the updated resolution. Like the previous resolution, the 2017 update states that APA neither endorses nor opposes assisted dying at this time.
"It was the consensus of the working group that this is a matter between the psychologist and the person considering aid in dying," says group member and Jonesville, Virginia–based psychologist James L. Werth Jr., PhD. "Psychologists have to be aware of their own biases, and if they can't be a part of the discussion without those biases getting in the way, they should refer the person to someone else. But we determined that APA shouldn't be a limiter of that discussion."
The most notable update to the resolution was linguistic. When the 2001 resolution was passed, the topic was known as "assisted suicide." Today, providers prefer the term "assisted dying" to reflect the distinction between suicide and the process of hastening death to alleviate pain and suffering.
Still, the specter of depression and suicide hangs over public opinion of assisted dying. Since Oregon first raised the possibility of legalized dying in the 1990s, researchers have grappled with the question of whether it can ever be considered a rational choice, Rosenfeld says. "Some people felt that almost everyone who seeks this option is doing so out of a rational appraisal of their situation. Others argued this is just a form of suicide and we should protect them from themselves," he says.
But research in the intervening years has suggested the truth lies in the gray area between, he adds. "Of the people who pursue this option, a sizable portion are rationally appraising their situation. And a sizable proportion are appraising it through a lens of depression."
In a study of terminally ill patients, for instance, Rosenfeld and his colleagues found that desire for death was associated with depression, and that desire decreased in patients who responded to antidepressants ( Psychosomatics , Vol. 51, No. 2, 2010). Other research, however, suggests that depression is not a major driver for most people who request aid in dying. When Oregon's law was passed, Goy teamed up with psychiatrist Linda Ganzini, MD, MPH, at Oregon Health and Science University, to study the moods, values, needs, concerns and symptom burdens of 58 Oregon residents with terminal illnesses who pursued assisted death. They found that most of those people did not have depressive disorders.
However, they also concluded that the Death with Dignity Act, as written, might fail to protect some patients with depression from making the choice to hasten death ( BMJ , Vol. 337, 2008).
Still, some advocates note that depression shouldn't necessarily make a person ineligible for physician-assisted death. "In the normal world of decision-making, we wouldn't say people lose autonomy to make decisions because they're moderately depressed," Rosenfeld says. Indeed, he adds, there's too little research to indicate how a person should feel or act as they approach their final days. "How cheerful should you be when you have a terminal illness?" he asks.
Some proponents of legalized aid in dying suggest that the option may be unfairly singled out because of cultural beliefs about the morality of suicide. "Assisted dying gets a lot of attention because of the values and emotions that get brought into it," says Werth. Yet many more people with serious illness end their lives through some other negotiated means, he says, such as ceasing medications, withholding food or drink, refusing life-sustaining treatment or signing "do not resuscitate" orders. "Most people will die those ways," he says.
Regaining control
After two decades of evidence from Oregon, research is answer-ing many questions about aid in dying. That evidence suggests that the desire to hasten death often comes from wanting to maintain some power over one's own life, Goy says. "In our research, the main reason people voiced for wanting the option was that they really wanted to have control over the circumstances of dying."
The wish for control can be for a variety of reasons, they found, including loss of autonomy and function or worries about future pain ( JAMA Internal Medicine , Vol. 169, No. 5, 2009). But reassuringly, when Goy and her colleagues compared people who expressed a desire for aid in dying with others with terminal illness who did not seek that option, they found no indication that the former group was motivated by financial concerns or being a burden to their loved ones, Goy says.

More research is needed to fully understand why and when some people ultimately make that choice, Shead notes. But it may be that just having the option provides a sense of control over the circumstances of one's death, allowing the person to focus on the quality of life that remains rather than fear of future suffering.
Research also shows that the choice to hasten death doesn't negatively impact surviving family members. Months or years after the death of the patients in their study, Goy and Ganzini interviewed their family caregivers. When they compared family members of those who requested aid in dying with those who did not, the researchers found no differences in depression, grief or use of mental health services. In fact, families of people who chose aid in dying reported that they felt more prepared and accepting of their loved one's death ( Journal of Pain and Symptom Management , Vol. 38, No. 6, 2009).
That could be because family discussions of hastened death often force families to discuss difficult topics they might otherwise not have spoken about, suggests Judith Gordon, PhD, a Seattle-based psychologist and clinical professor of psychology at the University of Washington who has studied end-of-life decision-making since 1996. "In this culture, there's still a lot of resistance to talking about dying, even if someone is diagnosed with a terminal disease," she says. "When people want to use this option, they need the support of their doctors and typically also want the support of their families."
Most people who receive a prescription for lethal medication talk to their families about their decision. "One of the gifts when someone makes this choice is that it brings the discussion to the table. The whole family or support group talks not just about this particular way of dying, but about all the issues related to how they feel about the death and what they will do later. It's an enormous benefit," Gordon says.
End-of-life inequity
Despite those potential benefits, critics express concerns about the possible harms of assisted death.
One worry surrounds access. So far, most of the people who have requested aid in dying are white, middle-class and typically well-educated, notes Carol Gill, PhD, APA working group member and professor of disability and human development at the University of Illinois at Chicago. "This sector of the population generally has access to options and seeks control of their life circumstances up to the end of life," she points out. "In contrast, there are underrepresented communities who have very different views of assisted dying."
The biggest concern to Gill and others is that people from disadvantaged groups might consider hastened death because their health-care needs are not being met. There are well-documented disparities in access to health-care services, with people from lower socioeconomic backgrounds, those with lower health literacy, and members of ethnic or racial minorities being less likely to receive adequate care, including palliative care services.
"There are a number of marginalized populations that are legitimately concerned about whether they are getting all of the best options in care at the end of life," Goy says. "We want to be sure we are attentive to treating pain adequately and addressing emotional experiences such as hopelessness, depression and despair, so that assisted dying does not seem like the only option."
Gill says that many in the disability-rights community have expressed unease with aid in dying because of concerns that people won't receive the resources they need to live meaningful lives despite physical limitations. "There are no assisted-dying laws that guarantee those resources, and that feels discriminatory to a lot of people with disabilities," she says.
Indeed, the very idea of "death with dignity" is an affront to many people who have physical limitations that require daily assistance, Gill says. "Some right-to-die activists have written about assisted dying as an antidote for indignity that occurs at the end of life, such as needing help to dress or use the bathroom. If you're a person with functional limitations, that's a real slap in the face," she says.
For most people, including those with disabilities and those facing functional loss at the end of life, social connection is what makes life worth living, she adds. "Having a meaningful life doesn't necessarily mean that life needs to be pain-free or without physical impairment or functional limitations. What it means is to remain engaged humanly, and get enough support from others or technology to engage in the activities that matter, that make life meaningful."
Unanswered questions
Even advocates of physician-assisted death say it's crucial that researchers continue to explore the process to ensure it's used responsibly. More work is needed to understand how terminally ill people make treatment decisions, Rosenfeld says, including the decision to end one's life. "The fact that assisted-dying laws aren't used that often has made people more confident that the law isn't being misused. But could that number go down a notch further by having more services available? That's where more research could be really informative," he says.
Gill adds that too little is known about how people make the decision to take lethal medication after they request the prescription. "We don't follow these individuals and hear what they're thinking day to day in the period before they ingest the drugs, and we don't know what happens to people who express interest but don't end up going through with it," she says.
Gill also hopes that researchers will further explore how the availability of aid in dying will affect medical practice. "Will it seem more and more reasonable for people to want their death hastened? Will we remember that life, even when it includes suffering, can still be considered meaningful given adequate support and resources? What will happen to the balance of those resources when assisted dying becomes more common?"
There's an open opportunity for psychology researchers to answer such questions, Rosenfeld says. "I think we are uniquely poised to do the kind of research that would inform these issues."
Psychologists can also fill an important role by evaluating and counseling people who have expressed a wish to pursue aid in dying. Though it's not a topic taught in graduate school, some state psychological associations have prepared guidelines for mental health professionals who do such evaluations, Gordon says. (For example, the Washington State Psychological Association issued the Washington Death with Dignity Act WSPA Guidelines for Mental Health Professionals , and the California Psychological Association recently published its guidelines, California's End of Life Option Act: CPA Guidance for Psychologists .)
Although it's not an easy job to work with people facing their final days, it is often a gratifying one, says Goy. "All of psychology comes to bear when you are working with people at the end of life. It calls for skills in every area that psychologists are trained in," she says. "There are a lot of emotions around this topic and it's ethically sensitive. The best we can do is be open to the concerns, continually be looking for data and challenge our own biases as best we can."
Further reading
APA End of Life Issues and Care www.apa.org/pi/aging/programs/eol
Physician-Assisted Dying: A Turning Point? Gostin, L.O., & Roberts, A.E., JAMA , 2016
Mental Disorders and the Desire for Death in Patients Receiving Palliative Care for Cancer Wilson, K.G., et al., BMJ Supportive & Palliative Care , 2016
The Relief of Existential Suffering Kissane, D.W., JAMA Internal Medicine , 2012
The Oregon Death with Dignity Act: A Guidebook for Health Care Professionals The Center for Ethics in Health Care, Oregon Health and Science University, 2008
Letters to the Editor
- Send us a letter
- Dissertation
- PowerPoint Presentation
- Book Report/Review
- Research Proposal
- Math Problems
- Proofreading
- Movie Review
- Cover Letter Writing
- Personal Statement
- Nursing Paper
- Argumentative Essay
- Research Paper
- Discussion Board Post
Choosing Topic For A Research Paper On The Death Penalty

Table of Contents

The death penalty is highly discussed all around the world. The main aspect of the problem is its moral side: is there any crime worth being punished with death?
Writing a death penalty research paper would demand to state your personal position on the question. It is better to define it for yourself before you start.
Still, you’ve got time for that. No need to rush. Think about it while we explain the basic requirements for a research paper on the topic.
Death penalty research paper: a brief how-to
First of all, the structure… An essential part of any written work.
It consists of:
- Outline . A table of contents, basically.
- Introduction . The beginning of your text. Here you present your thesis, your statement, and explain your vision of the issue. You might also provide the reader with a brief history of the problem, definitions, etc. Anything that would grab the reader’s attention.
- Main body . This is to present all your ideas and research work you’ve done. Remember to place the statements in a logical order and divide the text into paragraphs.
- Conclusion . Here you sum up everything you’ve said before. Keep in mind that you don’t have to add any new ideas in this paragraph.
- References . At the very end, you provide a list of resources and bibliography.
While researching the topic, find out about the death penalty procedure, legislation, countries, that practice it, what kinds of crimes are condemned with the death penalty, what are the terms and conditions, etc.
List of credible sources for inspiration
WWhile there’s a need to know much on the topic, it’s obvious that you have to do a lot of college research paper work. That is why you have to choose the best sources. So here are some ideas where you can take useful, reliable and up to date information:
- Wikipedia . Only to get a general understanding, before digging deeper. Here you can find information on history, contemporary use, public opinion, etc. Pay attention to the references mentioned in the articles. They usually contain valuable resources.
- DPIC (Death Penalty Information Center). Loads of data on capital punishment in the U.S.A. Moreover, they post news about condemnations , have execution database and state-by-state map.
- CNN contains a pretty interesting article “Death Penalty Fast Facts”. It is constantly updated and provides curious statistics.
- NCADP (National Coalition to Abolish the Death Penalty). The movement against capital punishment. Of course, you won’t find information in favour of such punishment on their website, but it is still very informative and has a lot of supporters.
How to choose a topic?
Capital punishment research paper writing may cover a vast variety of issues related to capital punishment. The main task here is to choose a narrow, specialized topic so that it would be interesting and won’t make you get lost in the number of facts.
If you face troubles composing a topic for your work , try this:
- Brainstorm . Set an alarm clock for 5-10 minutes and concentrate on noting ideas for your topic.
- Find the aspect of your most genuine interest.
- Make sure that the issue you chose is well covered with decent materials .
- Note keywords of your topic to be.
- Experiment on phrasing.
- Determine your topic as the main research question.
Didn’t help? Well, we’ve got some ideas for you. Check ‘em out below.
Death penalty research questions
As the issue is very multifaceted, it might get quite difficult to decide where to start.
Whichever topic you choose, it’s better to know general information on the case. Here are the most helpful stats!
- 105 (54%) countries abolished capital punishment for all crimes.
- 7 (4%) countries abolished the death penalty de facto and haven’t used it in practice for more than 14 years, but it is reserved for exceptional cases.
- 55 (28%) countries use the death penalty in practice.
- Most popular issues within the topic are death penalty and international human rights ; racial aspect; methods of performing; religious aspect; humanness.
More statistics, visualized for your convenience:
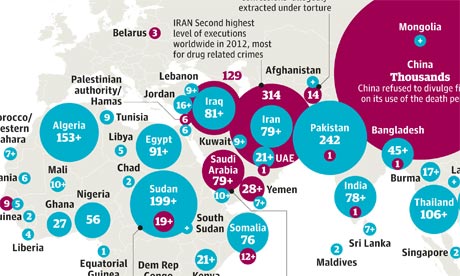
Death penalty essay topics
Since there is a lot to examine within the issue of capital punishment, you would need to come up with a specific topic for your research paper.
Below are some prewritten death penalty research paper topics which may be of great help:
- Can the death penalty be seen as an act of revenge, not as a punishment?
- The death penalty is more human than life imprisonment.
- The negative sides of the death penalty.
- Does the death penalty have a positive effect on crime rates?
- Can capital punishment save the funds that are spent on the imprisoned?
- Is the death penalty equal to murder?
- How should capital punishment be performed?
- There’s always a chance to execute an innocent person. How to solve this problem?
- Death penalty in the religious context.
- Examine the legislation of the countries where capital punishment is practised.
- The moral aspect of the death penalty.
- Pros and cons of the death penalty.
- Lifetime imprisonment is a better punishment for criminals.
- Own attitude towards the death penalty.
- It is better to keep ten criminals alive than to execute one innocent person.
- Methods of performing capital punishment.
- Evolution of the death penalty.
- Analyze all the aspects of capital punishment in a selected country/state.
- People who are considered to deserve capital punishment will never be rehabilitated in society.
- How to deal with the chance of executing an innocent?
- The effectiveness of the death penalty in preventing crimes.
- Can capital punishment be seen as a violation of human rights?
- Families of executed people: psychological context.
- Capital punishment: an efficient means or a relic of history?
- Death penalty as a method of intimidation in third-world countries.
To sum up, we’d say that a capital punishment research paper is indeed a tough but still thought-provoking assignment.
However, knowing the basics of writing such paper will surely ease your work.
Follow the instructions of your teacher, use hints and ideas from this article and be ready to do your best!
Don’t know how to craft a perfect paper on the death penalty, but strive to have one? If there only was a service to help you out… Wait! There is one. Order your perfect essay here and forget all your troubles.

Pro Tips On How To Write Money Cant Buy Happiness Essay

How to Write Abortion Research Paper Homework?

Essay on Ambition: How to Make it Successful?
Reference.com
What's Your Question?
- History & Geography
- Science & Technology
- Business & Finance
- Pets & Animals
What Is a Good Thesis Statement for “Death of a Salesman” by Arthur Miller?
A valid and provocative thesis statement on Arthur Miller’s Pulitzer-prize-winning play “Death of a Salesman” should focus on one of the major themes of the play. These themes revolve around the ideas of denial, abandonment and the disorder of madness.
Because everyone in the Loman family in “Death of a Salesman” is either living in denial or enabling another family member’s denial, this theme is a strong choice for a thesis. In particular, Willy Loman cannot face the truth about his own mediocrity and must cling to his denial of failure to preserve any emotional stability. Willy also feels abandoned by various members of his family and finally abandons them completely when he commits suicide. Willy’s madness and disorder also provide a strong starting place for a thesis statement, as Willy’s denial of the truth ultimately leads him to living in an alternate reality.
MORE FROM REFERENCE.COM

Advertisement
Americans focus on a good life. But what about a good death?
Copy the code below to embed the wbur audio player on your site.
<iframe width="100%" height="124" scrolling="no" frameborder="no" src="https://player.wbur.org/hereandnow/2024/07/05/end-of-life-practices"></iframe>

Americans spend a lot of time thinking about what it means to live a good life. But what about a good death? In 2022 researchers at the Duke University Global Health Institute ranked countries by the quality of their end-of-life care, and the United States ranked only 43, just below Colombia, Romania, Nigeria and Guatemala.
So what does this country need to do? Recent Middlebury College graduate Samara Gordon Wexler is thinking about that question. The 22-year-old winner of a prestigious Watson Fellowship is about to embark on a five-continent journey. She'll visit, work and train with end-of-life practitioners from Ghanaian coffin artists to Indian trekkers to find out what it means to die a good death and how to make it happen here.
Here & Now host Deepa Fernandes talks to Gordon Wexler about the project and why it matters.

This segment aired on July 5, 2024.
More from Here & Now
- Open access
- Published: 25 June 2024
Qualitative study on the perception of good death in patients with end-stage cancer in oncology nurses
- Wei-dan Wu 1 , 2 , 3 na1 ,
- Yi Wang 1 , 2 , 3 na1 ,
- Xin-yu Fu 4 na1 ,
- Jin-hua Zhang 1 ,
- Chen-yang Zhang 4 ,
- Xin-Li Mao 1 , 2 , 3 &
- Shao-wei Li 1 , 2 , 3
BMC Nursing volume 23 , Article number: 431 ( 2024 ) Cite this article
208 Accesses
Metrics details
To explore the perception of good death of patients with end-stage cancer by nurses in the oncology department.
In the study we used a phenomenological approach and semi-structured interviews. A total of 11 nurses from the oncology department of a Grade A hospital in Taizhou were interviewed on the cognition of good death from July 1 to September 30, 2022. Colaizzi’s analysis method was used to analyse the interview data. This study followed the consolidated criteria for reporting qualitative research (COREQ).
Four themes were identified: a strong sense of responsibility and mission; To sustain hope and faith; The important role of family members; Improve patients’ quality of life.
The nurses in the department of oncology have a low level of knowledge about the “good death”, and the correct understanding and view of the “good death” is the premise of the realization of " good death”. The ability of nursing staff to improve the “good death”, attention, and meet the needs and wishes of individuals and families, is the guarantee of the realization of “good death”.
Peer Review reports
Introduction
The 2020 Global Cancer Statistics, published by the American Cancer Society shows that there were 10 million cancer deaths worldwide in 2020, and the global cancer burden is projected to reach 28.4 million by 2040, a 47% increase over 2020 [ 1 ]. Our country leads the world in cancer incidence and mortality [ 1 ], and the health damage caused by cancer is almost twice the world average [ 2 , 3 ].
Patients with end-stage cancer are defined as those who have no hope of a cure in modern medicine and are expected to survive for 3–6 months [ 4 , 5 ]. The terminal cancer patient’s condition can not be reversed, and has not yet effectively alleviated the pain, and the use of life support measures such as breathing machines to some extent prolonged the pain, resulting in patients can not die in comfort and dignity [ 6 ]. Death represents a significant and inevitable stage in the cycle of life, marking its final chapter for all living beings. It is a profound and crucial period that holds tremendous significance in the grand scheme of existence [ 7 ]. Hospice care is a holistic approach aimed at addressing the physical, psychosocial, and spiritual needs of individuals with a terminal illness and their family members. It provides comprehensive support and services to ensure comfort, dignity, and quality of life during this challenging time [ 8 ]. There is substantial evidence demonstrating the positive impacts of hospice care. It has been shown to enhance the quality of end-of-life (EoL) care, reduce medical costs, align with individuals’ preferences for comfort-focused care, and minimize the use of burdensome therapies. These findings support the value and effectiveness of hospice care in providing appropriate and compassionate support to patients and their families during the terminal stages of illness [ 9 , 10 ].
Hospice care in China is still in its early stages compared to certain Western countries. Efforts are being made to expand access to hospice services, raise awareness about the benefits of palliative care, and improve the quality of care provided to individuals with life-limiting illnesses in China [ 11 ]. As the concept of “eugenics” and “optimal parenting” gains popularity, the idea of a “good death” is gradually being brought to the forefront. It not only reflects the respect for life but also signifies the progress of society and civilization. The hospice concept was introduced in China in the 1980s. The concept and characteristics of a “good death” originated from early end-of-life care, with the ultimate goal of advocating for people’s support in the field of end-of-life care and drawing attention to the well-being of terminally ill patients. In 1998, Emanuel et al. proposed the framework for a good death, providing a comprehensive explanation of the multidimensional personal experience encompassed by death. Researchers divided the process of death into four key components: the inherent characteristics of the patient, the variable factors within the patient’s experience, the interventions by the healthcare system, and the outcomes. A “good death” can be described as one that occurs without the knowledge of the exact time of death, enables the individual to bid farewell to loved ones, avoids unnecessary interventions, allows the person to have some control over the place of death, minimizes distress and suffering, respects the patient’s and their family’s wishes, and aligns reasonably with clinical, cultural, and ethical standards. This comprehensive definition encompasses multiple aspects that contribute to a positive and meaningful end-of-life experience for both the individual and their loved ones [ 12 , 13 ].
Across different cultures, certain attributes of a good death are often emphasized. These include maintaining a pain-free status through effective pain management, providing emotional comfort and support to the person and their loved ones, and ensuring that individuals are prepared for the inevitability of death through open communication and appropriate end-of-life planning. These attributes are recognized as important factors in promoting a more peaceful and dignified transition at the end of life, regardless of cultural backgrounds [ 14 , 15 ]. Nurses who have a good understanding of the concept of a “good death” are better equipped to provide more effective end-of-life care to patients [ 16 ]. When providing care to individuals who are dying, nurses may experience a range of emotions, including anger, despair, distress, and guilt [ 17 , 18 ]. Understanding the concept of a good death and accepting the inevitability of death can aid nurses in coping with these complex emotions. However, it is worth noting that the acceptance of hospice care in Chinese society has been relatively slow, despite its introduction to mainland China as early as 1988 [ 19 ]. With the aging population, there is an increasing demand for end-of-life care. To measure this demand, an index system can be used, taking into account factors such as the burden caused by diseases, the dependency ratio of the elderly population, and the speed of aging [ 20 ]. In China, the objective demand for end-of-life care is indeed increasing. However, traditional cultural influences often make discussions about death taboo, and the concept of a “good death” is not widely accepted by most people [ 19 ].
Good Death (GD) is one of the core objectives of hospice care [ 21 , 22 ]. This study conducted in-depth interviews with nurses in the department of oncology to understand the current implementation of good death technology, the cognitive status of medical staff on good death, and the clinical coping strategies for patients with end-stage cancer, to determine the cognitive deficiencies of medical staff in good death and the aspects of continuous learning. The study mentioned focused on oncology inpatient unit nurses because they are frequently involved in providing end-of-life care. As patients with cancer often face end-of-life issues, it is important to understand the experiences and perspectives of nurses working in this specific setting.
Study design
We used phenomenological qualitative research and face-to-face semi-structured interviews to explore the perception of good death of patients with end-stage cancer by nurses in the oncology department in Taizhou Hospital of Zhejiang Province from July 1 to September 30, 2022. In qualitative research, phenomenological methods focus on describing common experiences shared by the entirepopulation, which also helps researchers to engage with participants from an in-depth perspective and to understand their experiences. Our research team has extensive experience in qualitative research.
Participants and ethical considerations
Purposive sampling was employed to select the participants who were eligible and could provide rich information about the research question.
Inclusion criteria: (1) Nurses with a license to practice nursing; (2) Oncology nurses with a minimum of 6 months of clinical nursing experience; (3) Providing care services to terminally ill cancer patients, and have work experience in hospice; (4) Ability to clearly articulate their views; (5) Providing informed consent and voluntary participation in this study. Exclusion criteria: (1) Nurses who withdrew from the interview process; (2) Nurses who were on leave or engaged in training, resulting in an absence from their position for more than 3 months; (3) Nurses who were unwilling to discuss their experiences in caring for terminally ill cancer patients.
In this study, the report will replace each participant with a code, and the interviewee’s identity, contact information will not be disclosed to others. Sound content is also used only in this study. The study was reviewed and approved by the Ethics Committee of Taizhou Hospital, Zhejiang Province, China (approval number: K20220789).
The qualitative data collection method employed for this study involved semi-structured, face-to-face interviews. Prior to the start of each interview, all nurses were provided with written informed consent to participate in the research. All interviews were digitally recorded, assigned pseudonyms, and transcribed verbatim. We took measures to ensure that the participants understood the purpose and process of the study, and we emphasized the privacy of the interview environment and the confidentiality of the data. The interviews will take place within the confines of the hospital’s designated conversational chambers, ensuring utmost privacy for the participants. Saturation was considered to be reached when no new themes emerged from the inductive content analysis. In total, we conducted interviews with 11 members of the oncology nursing team (See Table 1 ).
Data collection
During the interview, subjects were also given the opportunity to read the consent form, confirm understanding, and ask questions. Verbal consent was obtained to preserve the anonymity of the subjects. During the interviews, participants were offered explanations for any inquiries they had. Additionally, participants had the option to refuse further interviews and withdraw from the study for any reason. In addition, two oncology nurses were selected for a pre-interview prior to data collection to ensure the clarity of the questions and to identify any potential problems. The data from preliminary interviews was not included in this study but was utilized to modify the interview structure based on the preliminary findings. The preinterviews were treated as tests and were excluded from the analysis. The final interview used in this study included the items are listed in Table 2 . Interviews were conducted in a quiet consultation room at the hospital between July 1 and September 30, 2022. Each person was interviewed one time, and each interview lasted approximately 30–50 min. All the interviews were conducted by a nurse with master who was trained in qualitative research. A research assistant played an auxiliary role which included recording the interviews.
The investigator audio recorded with permission, and participants’ responses, including nonverbal cues and body language during the interviews, were noted. The results will be returned to each participant within 24 h of each interview, to verify the interview details, thus ensuring the accuracy and credibility of the analysis. Before this interview, investigators were trained in interview and communication skills, including effective listening and giving positive feedback, establishing good relationships with interviewees, maintaining eye contact, not interrupting interviewees, not judging their views, etc.
Data analysis
Audio recordings were transcribed verbatim and checked for accuracy by repeated listening within 24 h of the interviews. After the interview, the data were analysed separately and immediately by two researchers with skilled analysis experience. Interview data was analysed using Nvivo12.0, a computer-assisted qualitative data management software. Colaizzi’s phenomenological seven-stepmethod was used for data analysis to complete theextraction of themes and sub-themes regarding the perception of good death of patients with end-stage cancer among oncology nurses (see Table 3 ). Any disagreement between researchers was resolved by making decisions through discussion until a consensus was reached. The final transcribed data, as well as the extracted themesand sub-themes, were sent to the participants simultaneously, and all participants agreed to be contacted again. This study met the criteria of Consolidated Criteria for Reporting Qualitative Studies (COREQ).
Rigor and trustworthiness
To ensure the study’s dependability, the methods and analyses used were described in detail. The study interviewer was a master’s degree student in nursing. The interviewer received systematic qualitative training to master qualitative research methods, was experienced in oncology practices, and established a good relationship with the participants before the interviews commenced. This facilitated the acquisition of real information. The researcher maintained a neutral attitude during the interview, did not lead or hint, did not interrupt the interviewee at will, and only asked timely follow-up questions, rhetorical questions, and clarifications until no new information emerged. Therefore, credibility was ensured. The collection, analysis, and interpretation of data were continually reviewed and detailed to ensure its dependability. The data extracted from the survey results were described in detail to achieve confirmability. Regarding transferability, this study described in detail the inclusion criteria, exclusion criteria, and demographic characteristics involved. Simultaneously, the Consolidated Criteria for Reporting Qualitative Research (COREQ) checklist was used to report the findings (See Appendix I for details).
Characteristics of the 11 participants are shown in Table 1 . All eleven participants were female. The shortest term of employment as a Registered Nurse was one and a half years, and the longest was 17 years (Fig. 1 ). Four distinct themes emerged from analysis of the interview data: (1) A strong sense of responsibility and mission; (2) Sustaining hope and faith; (3) The important role of family members; and (4) Improving patients’ quality of life. Each theme included three–four subthemes (see Table 4 ).

A visual analysis of the working years of the 11 participants included
Theme one: a strong sense of responsibility and mission
Most respondents said that when they realized that a patient was dying, their presence was more important than ever, triggering a strong sense of responsibility and mission. “End-stage patients will leave at any time, when in the dying patient evaluation period, I will often ward, observe the patient’s vital signs, keep the comfort of family members, at this time of the patients and family members are in great need of medical personnel to accompany and support, especially families, at this point the heart is very fragile, especially need a psychological support.” (A5, female, 28 y.o) “For the families of the patients whose death is imminent, I will tell them to tell the patients as soon as possible if there is anything they need to tell them. If there is anything that needs the help of our doctors and nurses, they can tell us at any time. We will do our best to help.” (A7, female, 39 y.o).
Theme two: sustaining hope and faith
Patient confidentiality.
Under the influence of traditional Chinese culture, when patients enter the terminal stage of cancer, considering the patients’ physical and psychological conditions and psychological acceptance of the disease, medical staff needs to inform the patients’ families and seek treatment advice, whether to conceal the true condition of patients [ 23 ], whether to continue treatment or give up treatment and so on so that the whole family is faced with a major choice. In this interview, the interviewees discussed their views on the confidentiality of the patient’s condition from the point of view of good death, and the nurses had better cognition of the confidentiality of the patient’s condition. “We have a lot of family members who are concerned about the patient’s ability to cope. They tell us in advance not to discuss the patient’s condition in front of the patient, and they ask us to keep it confidential when the patient asks. We usually comply with their request at this time. “(A9, female, 32 y.o).
“A lot of family members ask for the patient’s condition to be kept confidential. Our doctors and nurses usually communicate on how to settle accounts with patients in a unified way. “(A3, female, 42 y.o).
Moral support
Patients and family members experience a complex range of emotions after being informed of a cancer diagnosis, and how to make patients and family members accept the reality that cancer is incurable is a challenge for healthcare professionals [ 24 , 25 , 26 , 27 ]. In the interview, the interviewees mentioned the importance of spiritual support for cancer families. “Many patients have no faith. I have seen many patients who have been in a period of anger after learning that they have cancer. They think why they are so unlucky. They have this disease and have no interest in doing anything. They think that the world is unfair and cruel to them. If we can help them to seek their faith, such as religion, it may have some spiritual comfort for them. " (A8, female, 37 y.o) “I met a retired civil servant in my work who, after learning that he had cancer, organized his years of Work Records and compiled a memoir by year. I think he would review his experiences and values when he read these memoirs, and his heart would be at peace for a while. I got an idea from him that I could use a similar approach to help other patients and their families find value in their lives and live more peacefully in the final stages of their lives. " (A6, female, 29 y.o).
Theme three: the important role of family members
The accompanying role of family members.
Influenced by our traditional culture, most terminal cancer patients want their closest family members to be with them at the end of their lives. Most of the interviewees indicated that the accompany of family members is a comfort to the patients, which makes them feel that they are loved and meets their psychological needs [ 28 ]. “Patients at this stage are more psychologically vulnerable than those with other diseases. At the end of their lives, the company of their family members is a great psychological comfort to them. Although I can’t have a lot of company during an epidemic, I usually ask one of the family members to stay here to accompany the patient. “(A2, female, 36 y.o) “At this time, the family member will stay by the patient’s side. Even if they don’t do anything or say anything, the patient will feel that they are cared for by someone and feel that they are still loved. “(A10, female, 30 y.o).
The communication role of family members
Under the influence of the Chinese traditional concept of life and death, there are still some difficulties in implementing and promoting euthanasia, especially for cancer patients, whose families often choose to hide the true situation from them, medical staff can only discuss it with their families [ 29 , 30 ]. The nurses mentioned that most of the family members lack the methods of psychological care and the experience of taking care of terminal cancer patients, do not know the psychological needs of the terminal cancer patients, and can not do the psychological work of the patients in time and effectively. “During the work process, some patients’ psychological needs are very high, but the family members accompanying them don’t understand the patients’ psychological needs. The two of them can’t chat together and have nothing to say for a whole day. “(A4, female, 26 y.o).
The caregiving role of family members
Family members accompany patients for a long time, know the daily living habits of patients best, can provide wholehearted care, and can timely detect and feedback on the symptoms of patients and changes in their condition, the care of family members for patients is an important component of the medical staff to evaluate the patient’s good death. “Many patients at this stage due to pain and other effects, the ability to move limited, and many daily activities need family care.” (A11, female, 25 y.o) “Terminally ill patients, ECG monitoring everyday detection of vital signs, we usually also one hour patrol, family members beside can pay attention to the patient’s vital signs changes. " (A1, female, 33 y.o).
Theme four: improving patients’ quality of life
Symptom control.
Most interviewees believed that end-stage patients should focus on symptom control and pain relief. “In the end, the most uncomfortable thing for many patients is the cancer pain, which makes them unable to move when they turn over. Taking painkillers and injecting painkillers can no longer control the pain. If it can reduce their pain, it is very meaningful for good death.” (A8, female, 37 y.o) “When patients enter the terminal stage, some other treatments are meaningless and try not to disturb them, so that patients can quietly go through the final stage of life.” (A7, female, 39 y.o).
Palliative care
During the interview, most interviewees expressed that they should try their best to meet the reasonable requirements of patients, reduce invasive operations on patients, listen to the voice of patients and their families more, improve the comfort level of patients, and give more tolerance and understanding to patients and their families. “During the epidemic, patients and their families are required to reduce going out and order meals in the department. However, patients with advanced stage do have a poor appetite. Some of their families will prepare meals and send them to the first floor of the hospital building. (A9, female, 32 y.o) “When I perform a blood gas analysis or an infusion on this type of patient, if I feel that I cannot successfully puncture the vein on the first try, I will seek assistance from other colleagues to avoid subjecting the patient to the pain of a second puncture.” (A1, female, 33 y.o).
The aim of this study was to explore the perceptions of oncology nurses regarding end-of-life care for patients with advanced-stage cancer in China. The interviews conducted in this study revealed that oncology nurses have generated numerous ideas and understandings about end-of-life care for patients. This demonstrates their strong concern for end-of-life care issues and their utmost efforts to help patients achieve a good death. The cognition of healthcare professionals regarding a good death is influenced by traditional cultural factors, and their ability to assist patients in achieving a good death is also limited by their level of knowledge and skills.
In contemporary times, the majority of individuals pass away within the confines of a hospital setting, necessitating the presence of nurses during their final days. As patients approach the end of their lives, nurses provide companionship and support throughout this significant transition [ 31 ]. The attitudes exhibited by nurses play a pivotal role in shaping the quality of end-of-life care. A positive attitude towards death can signify that nurses possess a more effective adaptation to the practices related to end-of-life care. This also implies that they are better equipped to provide compassionate and supportive care to patients during this sensitive stage [ 32 , 33 ]. By fostering positive attitudes towards the dying, nurses can overcome their own fears of death. This allows them to create a safe and supportive environment where patients can experience a peaceful and dignified process of dying. Such an atmosphere fosters a sense of respect and enables patients to feel valued as individuals during this vulnerable time [ 34 ]. The research conducted by Ceyhan et al. revealed a positive correlation between the perception of a good death and the attitudes of intensive care nurses towards providing care for patients in their final moments. These nurses exhibited favorable attitudes towards end-of-life care and possessed a strong belief in the concept of a good death. The study suggests that nurses in the intensive care setting are more inclined to embrace and prioritize the well-being and comfort of dying patients [ 35 ].
The correct understanding and view of “good death” is the premise to realize “good death”
This is similar to the findings of Hilal Türkben Polat and others [ 34 ]. The concept of death often evokes negative emotions in patients, patient relatives, and nurses. Consequently, it is typically avoided and sometimes even considered a taboo in certain regions. Patients in Eastern countries encounter unique challenges when it comes to preparing for death. This is primarily due to lower frequencies of receiving bad news, such as diagnoses and prognoses, as well as cultural practices that discourage discussions about death. Moreover, stronger taboos surrounding death discussions exist in Eastern countries compared to Western countries [ 36 ]. In western countries, the disclosure of diagnoses is regarded as a fundamental patient right and an essential practice. Within the western ethical tradition, there is significant emphasis on providing patients with truthful information. Medical practitioners have a responsibility to respond to patients’ questions regarding their diagnosis in an honest and forthright manner [ 37 ].
Under the influence of Eastern philosophy, the challenges related to diagnosis disclosure are further magnified in Eastern countries. Traditional Eastern philosophical beliefs, such as the emphasis on harmony, collective well-being, and the idea of protecting patients from distress, can create barriers to open and direct communication about diagnoses. Balancing the values of truthfulness and preserving emotional well-being becomes a particular challenge within the Eastern cultural context [ 38 ]. In China, it is common for family members to withhold cancer diagnoses from the patient, as they believe it may help protect the patient from potential emotional distress and depression. This practice stems from a desire to shield loved ones from the potentially negative impact of such news. However, it is important to note that this approach may differ from the Western emphasis on patient autonomy and the right to access complete information about one’s own health condition [ 26 ]. As highlighted by Jiang Yu et al., the decision to withhold cancer diagnoses in China is often a collective consensus among family members. This collective decision-making process is influenced by cultural norms, where the family plays a central role in matters of health and well-being. In such cases, the family members believe that keeping the diagnosis concealed is in the best interest of the patient, aiming to maintain emotional well-being and alleviate potential distress. It is important to recognize and respect these cultural differences and the role of familial decision-making in the context of healthcare practices [ 39 ].
The concept of “Avoid death” in our traditional culture will affect the expression of the needs of terminal cancer patients. Compared with patients, their families have more difficulty accepting the concept of good death, which they believe means giving up treatment, waiting for death, and being difficult to accept psychologically [ 40 ]. The medical personnel should strengthen the family members’ correct understanding of good death and make them realize the importance of respecting the patient’s right to know and independent decision-making to realize good death, it is suggested that family decision-making should be gradually changed into a way of discussion between patients and their families, to lighten the psychological burden of both sides and let patients realize their wishes. Fully pay attention to the needs of end-stage patients and their families, and take targeted measures to help patients to achieve good death [ 41 ].
The good death ability of nursing staff needs to be improved
The attitude of professional nurses to death greatly influences the treatment decision of terminal cancer patients and affects the quality of patients’ death. The more skilled the nursing skills, the better the communication skills, and the terminal attitude of terminal cancer patients, the better the quality of life of the patients.
Based on the interview results, it is evident that nurses have insufficient competency in implementing end-of-life care. They make efforts to help patients manage clinical symptoms and enhance the caregiving abilities of family members through their own capabilities, aiming to assist patients in a better end-of-life experience. However, the nurses’ level of competence directly affects the patient’s experience of end-of-life care. They have limited opportunities for formal end-of-life care training and education, resulting in a relative lack of knowledge in this area. The end-of-life experience is unique and personal for each individual, with most people desiring to avoid pain during this period, while others may prioritize prolonging life at any cost. End-of-life care may be provided by doctors, physicians, nurses, emergency personnel, or volunteers. However, nurses play a significant role and bear primary responsibilities in this regard [ 14 ]. A study indicated that nurses, as moral agents, possess a profound commitment to upholding the moral integrity of end-of-life care, particularly when it involves assisted death. This suggests that nurses play a crucial role in ensuring that ethical principles and values are upheld throughout the process. Their dedication to promoting the well-being and dignity of patients in these complex situations highlights their ethical and moral responsibility in providing compassionate and supportive end-of-life care [ 15 ]. In addition, another research study highlighted the indispensable role of nurses in providing compassionate care to patients in their final stages of life [ 16 ]. Nurses are entrusted with the responsibility to deliver exceptional care to terminally ill patients and their families. Insufficient knowledge has been identified as a major obstacle in providing optimal care for individuals nearing the end of their lives [ 18 ]. A lack of education and training in end-of-life care has been recognized as a significant contributing factor to insufficient recognition and management of symptoms, as well as challenges in effective communication with patients and their families [ 17 ].
At present, the level of knowledge and skills of our palliative care is not high, and they lack the skills of psychological, social, and spiritual support and are difficult to implement skillfully [ 42 ]. The limited awareness of hospice care in Mainland China can be attributed to various factors, such as the absence of systematic policy support, limited public educational campaigns, and the lack of comprehensive academic and practical curricula and training programs on hospice care. These factors have collectively contributed to the insufficient understanding and recognition of hospice care among the general public and healthcare professionals in Mainland China [ 43 ].
Healthcare professionals need professional knowledge and skills should use a variety of ways to educate professionals, and guide them not only care about patient survival rate, and quality of life, at the same time, we should also pay attention to the physical and psychological needs of incurable patients [ 44 ], educate patients with end-stage cancer and their families, provide a suitable environment and the necessary help, improve the quality of patient’s death, and meeting the needs of patients who are nearing the end of life. By enhancing the medical curriculum to include comprehensive education on hospice care and establishing hospice care programs within hospitals, opportunities can be increased for physicians, nurses, patients, and their family members to enhance their awareness and utilization of hospice care services. This would ultimately contribute to improving end-of-life care and ensuring that individuals receive the support and comfort they need during this crucial time [ 45 ]. In addition, the whole society should widely carry out life education and Death Education, guide people to look at life and death correctly, a planned, leisurely life with, a good start, and a good finish.
Paying attention to and meeting the needs and wishes of individuals and families is the guarantee of achieving “good death”
In the Chinese cultural context, there is a strong emphasis on the centrality of the family and social relationships [ 12 ]. Family dynamics are considered crucial for a good death, and Asian populations, influenced by Confucian teachings, place great importance on the cohesion of the family and the significance of familial relationships [ 46 ]. Nurses take care of terminal cancer patients for a long time, and they are familiar with the patients and their families. Clinical nurses should play an active role as a good communication bridge, which can help them communicate their needs or promote communication among themselves, at the same time, teach family members to play a better role in family support to meet the needs of patients with end-stage cancer to receive family warmth and care [ 47 , 48 , 49 ].
This study still has some limitations. Primarily, the participants were confined exclusively to a solitary tertiary hospital, thereby potentially limiting the generalizability of the findings. To augment representativeness, future investigations could contemplate sampling participants from nontertiary hospitals. Furthermore, the inclusion of solely female nurses in the analysis neglects male nurses, thus introducing a predisposed bias into the results. Within the targeted population of this inquiry, the dearth of male nurses serving escalates the complexity of ameliorating this bias. Secondly, the study lacked the amalgamation of quantitative research, impeding the determination of specific domains and the magnitude of improvement required in nurses’ competencies. To rectify this, future research endeavors should endeavor to broaden the sample size and scope, employing quantitative research methods to scrutinize the precise cognitive facets and knowledge modules necessitating enhancement in nurses. Additionally, there exists a demand for further exploration of culturally tailored competency models in the Chinese context. This would assist in confronting and resolving the challenges impeding the current competency development process. Furthermore, interviews were conducted in Chinese and subsequently analyzed and translated into English. Despite efforts by professional English editors to guarantee accurate translation, there remains a small risk that the translation process may have influenced the study outcomes. Lastly, further exploration is still required to ascertain the appropriate cultural backdrop of our model, and to refine and address the prevailing complications encountered in the euthanasia procedure.
This study explored the general cognition of nurses in the oncology department about good death from the perspective of Chinese nurses. The results showed that nurses in the oncology department had a low level of knowledge about good death, and had a correct understanding and view of “good death”. Indeed, strengthening hospice education is crucial to improve public awareness and acceptance of hospice care, leading to better quality end-of-life care. To enhance public education on hospice care, it is essential to develop and implement culturally appropriate educational programs systematically. By tailoring these programs to the specific cultural context, we can effectively address the barriers and taboos surrounding discussions about death and promote understanding and acceptance of hospice care [ 50 ]. It is the premise of realizing “good death”, and the ability of nurses should be improved. It is the guarantee of realizing “good death” to pay attention to and satisfy the needs and wishes of individuals and families.
Data availability
The datasets generated during the current study are available from the corresponding author on reasonable request.
Sung H, Ferlay J, Siegel RL, Laversanne M, Soerjomataram I, Jemal A, Bray F. Global Cancer statistics 2020: GLOBOCAN estimates of incidence and Mortality Worldwide for 36 cancers in 185 countries. CA Cancer J Clin. 2021;71:209–49.
Article PubMed Google Scholar
Wei W, Zeng H, Zheng R, Zhang S, An L, Chen R, Wang S, Sun K, Matsuda T, Bray F, He J. Cancer registration in China and its role in cancer prevention and control. Lancet Oncol. 2020;21:e342–9.
Feng RM, Zong YN, Cao SM, Xu RH. Current cancer situation in China: good or bad news from the 2018 Global Cancer statistics? Cancer Commun (Lond). 2019;39:22.
PubMed Google Scholar
Roger C, Morel J, Molinari N, Orban JC, Jung B, Futier E, Desebbe O, Friggeri A, Silva S, Bouzat P, Ragonnet B, Allaouchiche B, Constantin JM, Ichai C, Jaber S, Leone M, Lefrant JY, Rimmelé T. Practices of end-of-life decisions in 66 southern French ICUs 4 years after an official legal framework: a 1-day audit. Anaesth Crit Care Pain Med. 2015;34:73–7.
Kawasaki Y. Consultation techniques using shared decision making for patients with cancer and their families. Clin J Oncol Nurs. 2014;18:701–6.
Ho AH, Leung PP, Tse DM, Pang SM, Chochinov HM, Neimeyer RA, Chan CL. Dignity amidst liminality: healing within suffering among Chinese terminal cancer patients. Death Stud. 2013;37:953–70.
Joarder T, Cooper A, Zaman S. Meaning of death: an exploration of perception of elderly in a Bangladeshi village. J Cross Cult Gerontol. 2014;29:299–314.
Kumar P, Wright AA, Hatfield LA, Temel JS, Keating NL. Family perspectives on Hospice Care experiences of patients with Cancer. J Clin Oncol. 2017;35:432–9.
Huang YT, Wang YW, Chi CW, Hu WY, Lin R Jr., Shiao CC, Tang WR. Differences in medical costs for end-of-life patients receiving traditional care and those receiving hospice care: a retrospective study. PLoS ONE. 2020;15:e0229176.
Article CAS PubMed PubMed Central Google Scholar
Shen VW, Yang C, Lai LL, Chen YJ, Huang HH, Tsai SH, Hsu TF, Yen DH. (2021) Emergency Department Referral for Hospice and Palliative Care Differs among patients with different end-of-life trajectories: a retrospective cohort study. Int J Environ Res Public Health 18.
Cheng Q, Duan Y, Zheng H, Xu X, Khan K, Xie J, Chen Y. Knowledge, attitudes and preferences of palliative and end-of-life care among patients with cancer in mainland China: a cross-sectional study. BMJ Open. 2021;11:e051735.
Article PubMed PubMed Central Google Scholar
Krikorian A, Maldonado C, Pastrana T. Patient’s perspectives on the notion of a good death: a systematic review of the literature. J Pain Symptom Manage. 2020;59:152–64.
Üzen Cura Ş. Nursing students’ spiritual orientations and their attitudes toward the principles of dying with dignity: a sample from Turkey. J Relig Health. 2021;60:221–31.
Noome M, Dijkstra BM, van Leeuwen E, Vloet LCM. Effectiveness of supporting intensive care units on implementing the guideline ‘End-of-life care in the intensive care unit, nursing care’: a cluster randomized controlled trial. J Adv Nurs. 2017;73:1339–54.
Ghezelsefli Z, Ahmadi F, Mohammadi E. End-of-Life Care provided for Cancer patients: a Metasynthesis Study. Holist Nurs Pract. 2020;34:210–20.
Mahan P, Taggart H, Knofczynski G, Warnock S. Transforming nursing students’ attitudes toward End-of-Life Care. J Hosp Palliat Nurs. 2019;21:496–501.
McIlfatrick S, Connolly M, Collins R, Murphy T, Johnston B, Larkin P. Evaluating a dignity care intervention for palliative care in the community setting: community nurses’ perspectives. J Clin Nurs. 2017;26:4300–12.
Aslakson RA, Wyskiel R, Thornton I, Copley C, Shaffer D, Zyra M, Nelson J, Pronovost PJ. Nurse-perceived barriers to effective communication regarding prognosis and optimal end-of-life care for surgical ICU patients: a qualitative exploration. J Palliat Med. 2012;15:910–5.
Colaizzi PF. Psychological research as the phenomenologist views it. In: Valle RS, King M, editors. Existential-phenomenological Alternatives for psychology. Oxford University Press; 1978. p. 6.
Tong A, Sainsbury P, Craig J. Consolidated criteria for reporting qualitative research (COREQ): a 32-item checklist for interviews and focus groups. Int J Qual Health Care. 2007;19:349–57.
Gurdogan EP, Aksoy B, Kinici E. The Concept of a good death from the perspectives of Family caregivers of Advanced Cancer patients. Omega (Westport). 2022;85:303–16.
Lyerly HK, Fawzy MR, Aziz Z, Nair R, Pramesh CS, Parmar V, Parikh PM, Jamal R, Irumnaz A, Ren J, Stockler MR, Abernethy AP. Regional variation in identified cancer care needs of early-career oncologists in China, India, and Pakistan. Oncologist. 2015;20:532–8.
Billings JA, Block S. Palliative care in undergraduate medical education. Status report and future directions. JAMA. 1997;278:733–8.
Article CAS PubMed Google Scholar
Hahne J, Liang T, Khoshnood K, Wang X, Li X. Breaking bad news about cancer in China: concerns and conflicts faced by doctors deciding whether to inform patients. Patient Educ Couns. 2020;103:286–91.
Ling DL, Yu HJ, Guo HL. Truth-telling, decision-making, and ethics among cancer patients in nursing practice in China. Nurs Ethics. 2019;26:1000–8.
Liu Y, Yang J, Huo D, Fan H, Gao Y. Disclosure of cancer diagnosis in China: the incidence, patients’ situation, and different preferences between patients and their family members and related influence factors. Cancer Manag Res. 2018;10:2173–81.
Rao A, Ekstrand M, Heylen E, Raju G, Shet A. Breaking Bad News: patient preferences and the role of Family members when delivering a Cancer diagnosis. Asian Pac J Cancer Prev. 2016;17:1779–84.
Griggs C. Community nurses’ perceptions of a good death: a qualitative exploratory study. Int J Palliat Nurs. 2010;16:140–9.
Yamagishi A, Morita T, Miyashita M, Igarashi A, Akiyama M, Akizuki N, Shirahige Y, Eguchi K. Pain intensity, quality of life, quality of palliative care, and satisfaction in outpatients with metastatic or recurrent cancer: a Japanese, nationwide, region-based, multicenter survey. J Pain Symptom Manage. 2012;43:503–14.
Miyashita M, Morita T, Sato K, Hirai K, Shima Y, Uchitomi Y. Factors contributing to evaluation of a good death from the bereaved family member’s perspective. Psychooncology. 2008;17:612–20.
Loerzel VW, Conner N. Advances and challenges: student reflections from an online death and dying course. Am J Hosp Palliat Care. 2016;33:8–15.
Gillan PC, van der Riet PJ, Jeong S. End of life care education, past and present: a review of the literature. Nurse Educ Today. 2014;34:331–42.
Henoch I, Browall M, Melin-Johansson C, Danielson E, Udo C, Johansson Sundler A, Björk M, Ek K, Hammarlund K, Bergh I, Strang S. The Swedish version of the Frommelt attitude toward care of the dying scale: aspects of validity and factors influencing nurses’ and nursing students’ attitudes. Cancer Nurs. 2014;37:E1–11.
Türkben Polat H. Nurses’ Perceptions on Good Death and Their Attitudes Towards the Care of Dying Individuals. Omega (Westport; 2022. p. 302228221100638.
Ceyhan Ö, Özen B, Zincir H, Şimşek N, Başaran M. How intensive care nurses perceive good death. Death Stud. 2018;42:667–72.
Xiao J, Ding J, Huang C. Notion of a good death for patients with cancer: a qualitative systematic review protocol. BMJ Open. 2022;12:e056104.
Zolkefli Y. The Ethics of Truth-Telling in Health-Care settings. Malays J Med Sci. 2018;25:135–9.
PubMed PubMed Central Google Scholar
Beyraghi N, Mottaghipour Y, Mehraban A, Eslamian E, Esfahani F. Disclosure of Cancer Information in Iran: a perspective of patients, Family Members, and Health professionals. Iran J Cancer Prev. 2011;4:130–4.
CAS PubMed PubMed Central Google Scholar
Jiang Y, Liu C, Li JY, Huang MJ, Yao WX, Zhang R, Yao B, Du XB, Chen J, Xie K, Zhao X, Wei YQ. Different attitudes of Chinese patients and their families toward truth telling of different stages of cancer. Psychooncology. 2007;16:928–36.
Emanuel EJ, Emanuel LL. The promise of a good death. Lancet. 1998;351(Suppl 2):Sii21–29.
Cipolletta S, Oprandi N. What is a good death? Health care professionals’ narrations on end-of-life care. Death Stud. 2014;38:20–7.
van Laarhoven HW, Schilderman J, Verhagen CA, Vissers KC, Prins J. Perspectives on death and an afterlife in relation to quality of life, depression, and hopelessness in cancer patients without evidence of disease and advanced cancer patients. J Pain Symptom Manage. 2011;41:1048–59.
Ni K, Gong Y, Li F, Cao X, Zhang H, Chu H, Li T, Mairipaiti A, Zhao Y, Li N. Knowledge and attitudes regarding hospice care among outpatients and family members in two hospitals in China. Med (Baltim). 2019;98:e15230.
Article Google Scholar
Brumley R, Enguidanos S, Jamison P, Seitz R, Morgenstern N, Saito S, McIlwane J, Hillary K, Gonzalez J. Increased satisfaction with care and lower costs: results of a randomized trial of in-home palliative care. J Am Geriatr Soc. 2007;55:993–1000.
Yin Z, Li J, Ma K, Ning X, Chen H, Fu H, Zhang H, Wang C, Bruera E, Hui D. Development of Palliative Care in China: a tale of Three cities. Oncologist. 2017;22:1362–7.
Li J. Chinese conceptualization of learning. Ethos. 2001;29:111–37.
Article CAS Google Scholar
Walczak A, Butow PN, Tattersall MH, Davidson PM, Young J, Epstein RM, Costa DS, Clayton JM. Encouraging early discussion of life expectancy and end-of-life care: a randomised controlled trial of a nurse-led communication support program for patients and caregivers. Int J Nurs Stud. 2017;67:31–40.
Hattori K, McCubbin MA, Ishida DN. Concept analysis of good death in the Japanese community. J Nurs Scholarsh. 2006;38:165–70.
Becker CL, Arnold RM, Park SY, Rosenzweig M, Smith TJ, White DB, Smith KJ, Schenker Y. A cluster randomized trial of a primary palliative care intervention (CONNECT) for patients with advanced cancer: protocol and key design considerations. Contemp Clin Trials. 2017;54:98–104.
Lin H, Ko E, Wu B, Ni P. (2022) Hospice Care preferences and its Associated factors among Community-Dwelling residents in China. Int J Environ Res Public Health 19.
Download references
This work was supported in part by Medical Science and Technology Project of Zhejiang Province (2024KY1788), Major Research Program of Taizhou Enze Medical Center Grant (19EZZDA2), Program of Taizhou Enze Medical Center Grant (22EZD06), Open Project Program of Key Laboratory of Minimally Invasive Techniques & Rapid Rehabilitation of Digestive System Tumor of Zhejiang Province (21SZDSYS01), Program of Taizhou Science and Technology Grant (23ywa33).
Author information
Wei-dan Wu, Yi Wang and Xin-yu Fu contributed equally to this work.
Authors and Affiliations
Department of Gastroenterology, Taizhou Hospital of Zhejiang Province affiliated to Wenzhou Medical University, Linhai, Zhejiang Province, China
Wei-dan Wu, Yi Wang, Jin-hua Zhang, Xin-Li Mao & Shao-wei Li
Key Laboratory of Minimally Invasive Techniques & Rapid Rehabilitation of Digestive System Tumor of Zhejiang Province, Taizhou Hospital of Zhejiang Province affiliated to Wenzhou Medical University, Linhai, Zhejiang Province, China
Wei-dan Wu, Yi Wang, Xin-Li Mao & Shao-wei Li
Institute of Digestive Disease, Taizhou Hospital of Zhejiang Province Affiliated to Wenzhou Medical University, Linhai, Zhejiang Province, China
Taizhou Hospital of Zhejiang Province affiliated to Wenzhou Medical University, Linhai, Zhejiang Province, China
Xin-yu Fu & Chen-yang Zhang
You can also search for this author in PubMed Google Scholar
Contributions
W-D W, W Y, X-L M and S-W L identified the research topic and designed the research process; W-D W, W Y, X-Y F were involved in writing the article; W-D W, J-H Z, X-Y F, W Y and C-Y Z were involved in interviewing and summarizing; W-D W, X-Y F, X-L M and S-W L were involved in correcting and revising the article.
Corresponding authors
Correspondence to Xin-Li Mao or Shao-wei Li .
Ethics declarations
Ethics approval and consent to participate.
All methods were carried out in accordance with the Declaration of Helsinki. The study was reviewed and approved by the Ethics Committee of Taizhou Hospital of Zhejiang Province affiliated to Wenzhou Medical University Institutional Review Board (approval No. K20220789). Researchers contacted and explained the research procedures and recruitment criteria to the participants and emphasised that participants’ responses would remain anonymous and confidential. Informed consent was obtained from all study participants.
Consent to publish
Not applicable.
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note.
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Supplementary Material 1
Rights and permissions.
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/ . The Creative Commons Public Domain Dedication waiver ( http://creativecommons.org/publicdomain/zero/1.0/ ) applies to the data made available in this article, unless otherwise stated in a credit line to the data.
Reprints and permissions
About this article
Cite this article.
Wu, Wd., Wang, Y., Fu, Xy. et al. Qualitative study on the perception of good death in patients with end-stage cancer in oncology nurses. BMC Nurs 23 , 431 (2024). https://doi.org/10.1186/s12912-024-02081-x
Download citation
Received : 28 July 2023
Accepted : 06 June 2024
Published : 25 June 2024
DOI : https://doi.org/10.1186/s12912-024-02081-x
Share this article
Anyone you share the following link with will be able to read this content:
Sorry, a shareable link is not currently available for this article.
Provided by the Springer Nature SharedIt content-sharing initiative
- Oncology department
- Qualitative research
BMC Nursing
ISSN: 1472-6955
- General enquiries: [email protected]
Jon Bon Jovi mourns the death of his mother: 'She will be greatly missed'
Carol Bongiovi died on Tuesday, July 9, at 83.
Jon Bon Jovi is mourning the loss of his mother Carol Bongiovi who died on Tuesday, July 9, at 83, according to an obituary provided by the rock star's representative.
1st look at upcoming Jon Bon Jovi interview special
"Our mother was a force to be reckoned with, her spirit and can-do attitude shaped this family. She will be greatly missed," wrote Jon Bon Jovi in a statement on behalf of his family.
Editor’s Picks

Bon Jovi’s story to be told in docuseries, 'Thank You, Goodnight: The Bon Jovi Story'

Jon Bon Jovi reflects on life as a rock and roll star: ‘It was pretty good’
Born Carol Sharkey, Carol Bongiovi was born in Erie, Pennsylvania, and joined the U.S. Marine Corps in 1959, where she met her husband, John Biongiovi, Sr. The couple moved to New Jersey, where their sons John Bongiovi Jr. -- later known as Jon Bon Jovi -- Anthony and Matthew were born.
Described as an entrepreneur who operated several businesses, Carol Bongiovi also worked as a Playboy Bunny and founded the Bon Jovi fan club.

Bon Jovi's story will be explored in docuseries, 'Thank You, Goodnight: The Bon Jovi Story'
According to the obituary, she's survived by her husband, John Bongiovi Sr., her three sons and daughters-in-law and eight grandchildren.
Related Topics
Trending reader picks.

Serena Williams on life after tennis and more
- Jul 10, 10:37 AM

'Horizon 2' pulled from August release date
- Jul 10, 7:01 PM

Alaska considers cruise ship ban on Saturdays
- Jul 10, 10:10 AM

1st look at rarely-seen rooms of Buckingham Palace
- Jul 9, 7:01 PM

Priyanka Chopra Jonas shares family photos
- Jul 10, 12:08 PM
ABC News Live
24/7 coverage of breaking news and live events
105 Death of a Salesman Essay Topics & Examples
Death of a Salesman is Arthur Miller’s multiple award-winning stage play that explores such ideas as American Dream and family. Our writers have prepared a list of topics and tips on writing the Death of a Salesman thesis statement, essay, or literary analysis.
trending now in US News

Obama knew in advance of Clooney’s bombshell call for Biden to...

Eerie details emerge after husband kills wife, daughter in...

Nursing student, 22, found beaten to death, days after judge...

ABC News exec was ‘furious’ after George Stephanopoulos said...

Biden-backing gov — and rumored replacement — caught on hot...

Ex-Kanye West muse Amber Rose says she'll speak at Republican...

Mystery deepens in case of 3 Chiefs fans found frozen to death...

Embattled Biden set to hold 'big-boy' press conference in bid to...
Breaking news, gov. gretchen whitmer says it ‘wouldn’t hurt’ for biden to take cognitive assessment as prez denies need.
- View Author Archive
- Get author RSS feed
Thanks for contacting us. We've received your submission.
Michigan Gov. Gretchen Whitmer said Wednesday that it “wouldn’t hurt” for President Biden to take a cognitive test.
Whitmer acknowledged that the assessment would be a good idea in an interview Wednesday, despite the octogenarian president denying that there’s a need for him to undergo such testing.
“I don’t think that it’d hurt, to be honest,” Whitmer told CNN in response to a question about Biden taking a mental acuity test.

The White House has been plagued with questions about Biden’s mental abilities since the June 27 debate, when he appeared to be confused and stumbled over his responses at times.
Polls show a majority of Americans are concerned about his mental fitness — and an increasing number of congressional Democrats and close allies are calling for him to drop out of the 2024 race.
The president tried to alleviate concerns about his age by sitting down for an interview with ABC’s George Stephanopoulos, but his performance there spurred even more allies to call on him to drop out.
Whitmer, a Democrat who has been a fierce supporter of Biden and is rumored to be a potential replacement if the president were to choose to suspend his campaign, also admitted that “the first presidential debate was not a success for President Biden.”
But, Whitmer said, Democrats need to continue to rally behind Biden while he’s in the race if they want to defeat former President Donald Trump.

“We can’t lose sight of how high these stakes are. We have a field. And unless one person, Joe Biden, makes an alternative decision, this is the field, and we’ve gotta go.”
Whitmer’s remarks echo a similar comment made by former House Speaker Nancy Pelosi (D-Calif.), who said Biden needs to “make that decision” on whether he’s going to stay in the race.
The president has been firm that he’s going to continue his bid. He wrote a letter to congressional Democrats on Monday stressing that he’s not dropping out, and later went on “Morning Joe” to say he is the Democratic nominee.

Biden has also laid out several excuses for his bad performance against Trump in the first debate. In his interview with Stephanopoulos , Biden argued that he was “exhausted” and “sick” with a “bad cold,” before pivoting to saying Trump’s points “distract me.”
He has never publicly released the results of a mental acuity test and has argued over the years that his time in the Oval Office is proof that he doesn’t need one.
“Look, I have a cognitive test every single day,” Biden told Stephanopolous. “Every day, I’ve had tests. Everything I do. You know, not only am I campaigning, I’m running the world. And that’s not — it sounds like hyperbole, but we are the central nation of the world.”

Advertisement

IMAGES
VIDEO
COMMENTS
Dorothy Parker was Lopatto's cat, a stray adopted from a local vet. And Dorothy Parker, known mostly as Dottie, died peacefullywhen she passed away earlier this month. Lopatto's essay is, in part ...
Writing an essay about death can be a profound and thought-provoking experience, allowing individuals to reflect on their own mortality and explore existential questions. To inspire your writing, here are 115 death essay topic ideas and examples. The concept of death in different cultures. The role of death in religious beliefs.
If so, reading essays about death, grief, and even near-death experiences can potentially help you begin addressing your own death anxiety. This list of essays and articles is a good place to start. The essays here cover losing a loved one, dealing with grief, near-death experiences, and even what someone goes through when they know they're ...
1. Life After Death. Your imagination is the limit when you pick this prompt for your essay. Because no one can confirm what happens to people after death, you can create an essay describing what kind of world exists after death. For instance, you can imagine yourself as a ghost that lingers on the Earth for a bit.
Death is defined as the permanent cessation of all biological functions that sustain a living organism. This can occur as a result of illness, injury, or simply old age. Death is a natural process that occurs to all living things, but it is also a process that is often accompanied by fear and uncertainty.
All Are Equal in Death. Death refers to the lasting termination of all life's tasks in a human being. Death chances on its prey in the middle of their actions and strikes equally to all. Socrates: His Life, Philosophy, & Death. The Philosopher, Socrates was a Greek and he was born in the proximities of 470 B.
She died before her 60th birthday - her terminal illness was discovered very late, and she passed away less than a year after receiving the diagnosis. Such a rapid change in my life left a mark on my memory and reshaped my view of life and death. Get a custom essay on Death, Dying, and Bereavement: Reflection. 187 writers online.
Death, loss, and grief are universal experiences that have been explored and portrayed in literature for centuries. These themes often serve as a reflection of the human condition, providing insights into the emotional, psychological, and cultural dimensions of these experiences. This essay will delve into the interpretations of death, loss ...
This article considers several questions concerning the philosophy of death. First, it discusses what it is to be alive. This topic arises because to die is roughly to lose one's life. The second topic is the nature of death, and how it bears on the persistence of organisms and persons. The third topic is the harm thesis, the claim that death ...
Step 2: Write your initial answer. After some initial research, you can formulate a tentative answer to this question. At this stage it can be simple, and it should guide the research process and writing process. The internet has had more of a positive than a negative effect on education.
Any thesis statement should be determined by what the author really believes. This question about the death penalty is one that really tries to force the author to take a position for or against.
Defining death helps refine the central question of the essay. There are good reasons to believe that dying can harm the person who dies. For example, dying can harm someone because it is frightening or painful. This essay, however, is an attempt to determine whether death, as opposed to dying, can harm the person who dies.
82 essay samples found. The death penalty, also known as capital punishment, remains a contentious issue in many societies. Essays on this topic could explore the moral, legal, and social arguments surrounding the practice, including discussions on retribution, deterrence, and justice. They might delve into historical trends in the application ...
Capital punishment has been a debatable issue for decades. Some people believe that the death penalty plays a crucial role in the criminal justice system, while others think that this procedure is highly unethical. We will write. a custom essay specifically for you by our professional experts. 192 writers online.
This thesis statement is not debatable. First, the word pollution implies that something is bad or negative in some way. Furthermore, all studies agree that pollution is a problem; they simply disagree on the impact it will have or the scope of the problem. No one could reasonably argue that pollution is unambiguously good.
Of the quantitative and mixed-methods studies (N = 9), 3 articles used standardized measures of a good death, including the Preferences about Death and Dying questionnaire, 26 The Concept of a Good Death scale, 27 and The Good Death Inventory. 28 The other six studies had developed their own quantitative measures (e.g., attitudinal measures of ...
Share Cite. Possible thesis statements: While Hamlet suffers a tragedy in death, he died as a hero, finally avenging his father's death. Hamlet is a tragic hero because he dies while avenging his ...
3. Methods. This review synthesised concept analyses on a good death to create a shared understanding of a good death within nursing. One researcher found the concept analyses by searching PubMed, CINAHL Complete, and Medline (Ebsco). The search terms used were "concept analysis" and "good death "or "peaceful death."
Here are a few potential topics regarding capital punishment, which you can consider if you're writing an argumentative essay. The death penalty is a deterrent that prevents potential criminals from committing serious crimes like murder. The death penalty is not effective at preventing crime. Capital punishment is more cost-effective than ...
That evidence suggests that the desire to hasten death often comes from wanting to maintain some power over one's own life, Goy says. "In our research, the main reason people voiced for wanting the option was that they really wanted to have control over the circumstances of dying."
Set an alarm clock for 5-10 minutes and concentrate on noting ideas for your topic. Find the aspect of your most genuine interest. Make sure that the issue you chose is well covered with decent materials. Note keywords of your topic to be. Experiment on phrasing. Determine your topic as the main research question.
A valid and provocative thesis statement on Arthur Miller's Pulitzer-prize-winning play "Death of a Salesman" should focus on one of the major themes of the play. These themes revolve around the ideas of denial, abandonment and the disorder of madness. Because everyone in the Loman family in "Death of a Salesman" is either living in ...
In 2022 researchers at the Duke University Global Health Institute ranked countries by the quality of their end-of-life care, and the United States ranked only 43.
Death is the only allowable reason for a candidate to drop out according to Wisconsin law, impeding potential replacement of Biden on the 2024 ballot. Getty Images
Letexier's average of 3.33 yellow cards per game is also among the lowest at Euro 2024, which could be good news for a Spain side who have been among the most prolific foulers in Germany.
News. Calls for justice grow in death of Black man outside Milwaukee hotel as GOP convention approaches. D'Vontaye Mitchell's death on June 30 has become the most recent flashpoint in how the ...
Objective To explore the perception of good death of patients with end-stage cancer by nurses in the oncology department. Method In the study we used a phenomenological approach and semi-structured interviews. A total of 11 nurses from the oncology department of a Grade A hospital in Taizhou were interviewed on the cognition of good death from July 1 to September 30, 2022. Colaizzi's ...
Carol Bongiovi died on Tuesday, July 9, at 83. Jon Bon Jovi is mourning the loss of his mother Carol Bongiovi who died on Tuesday, July 9, at 83, according to an obituary provided by the rock star ...
12 min. Death of a Salesman is Arthur Miller's multiple award-winning stage play that explores such ideas as American Dream and family. Our writers have prepared a list of topics and tips on writing the Death of a Salesman thesis statement, essay, or literary analysis. Table of Contents.
Michigan Gov. Gretchen Whitmer said Wednesday that it "wouldn't hurt" for President Biden to take a cognitive test. Whitmer acknowledged that the assessment would be a good idea in an ...